Quality measures and clinical tools can bring focus and clarity to caring for patients with cognitive impairment and supporting their caregivers.

Alzheimer's Disease is the sixth-leading cause of death in the United States, and one in three American seniors dies of some form of dementia.1 Caring for adults with dementia challenges physicians' usual paradigm of establishing a definitive diagnosis and then offering treatments to either alleviate the symptoms or improve the prognosis. Frustrated physicians may feel “there's nothing that can be done” and stick with what they know: focusing on the patients' co-morbid conditions, such as high cholesterol, hypertension, and diabetes. For the patients and their caregivers, however, it is dementia's cognitive, functional, and behavioral losses that most affect their quality of life. Diagnosis and treatment options for dementia may one day improve. In the meantime, focusing on what can be done, using a navigational framework and clinical tools like the ones described in this article, can help us to more effectively help patients and their families.
USING DEMENTIA QUALITY MEASURES AND CARE KITS
The American Academy of Neurology and the American Psychiatric Association convened a work group of 26 members (including Dr. Unwin) from 21 international organizations “to conceptualize the best possible care for patients with dementia and their caregivers and to operationalize optimal processes for delivering such care.”2 The resulting Dementia Management Quality Measurement Set, disseminated in 2016, provides clinicians with a nationally recognized, evidence-based, clearly defined, effective group of metrics with which to evaluate their current level of care and that serves as a basis for quality improvement initiatives. (See “Dementia Management Quality Measurement Set.”) Groups can use established quality improvement processes, such as Plan, Do, Study, Act (PDSA), to systematically target specific areas. For example, clinicians could collect baseline data on how often they diagnose dementia and then develop and initiate a plan to enhance dementia assessment and diagnosis. They could then collect data on their plan's effectiveness and modify it as necessary.
KEY POINTS
- The Dementia Management Quality Measurement Set gives physicians goals to pursue in improving their care of patients and communication with caregivers.
- Physicians can use dementia toolkits to build tailored care plans that focus on the patient's short-term and long-term needs and goals.
- Some elements of dementia care can be performed by nonclinicians, improving clinical workflow.
- Medicare now reimburses physicians for cognitive assessment and care plan services.
DEMENTIA MANAGEMENT QUALITY MEASUREMENT SET
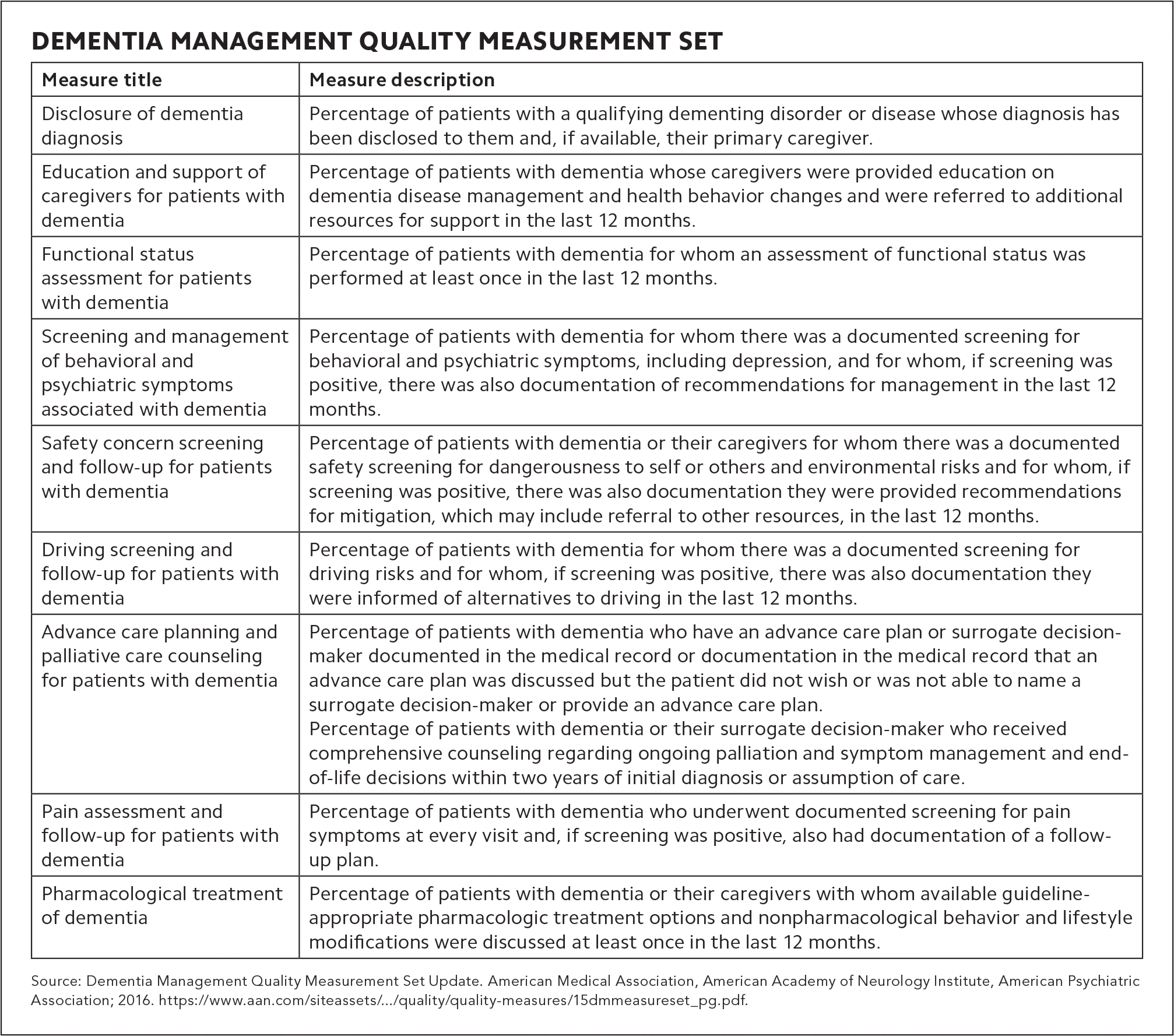
| Measure title | Measure description |
|---|---|
| Disclosure of dementia diagnosis | Percentage of patients with a qualifying dementing disorder or disease whose diagnosis has been disclosed to them and, if available, their primary caregiver. |
| Education and support of caregivers for patients with dementia | Percentage of patients with dementia whose caregivers were provided education on dementia disease management and health behavior changes and were referred to additional resources for support in the last 12 months. |
| Functional status assessment for patients with dementia | Percentage of patients with dementia for whom an assessment of functional status was performed at least once in the last 12 months. |
| Screening and management of behavioral and psychiatric symptoms associated with dementia | Percentage of patients with dementia for whom there was a documented screening for behavioral and psychiatric symptoms, including depression, and for whom, if screening was positive, there was also documentation of recommendations for management in the last 12 months. |
| Safety concern screening and follow-up for patients with dementia | Percentage of patients with dementia or their caregivers for whom there was a documented safety screening for dangerousness to self or others and environmental risks and for whom, if screening was positive, there was also documentation they were provided recommendations for mitigation, which may include referral to other resources, in the last 12 months. |
| Driving screening and follow-up for patients with dementia | Percentage of patients with dementia for whom there was a documented screening for driving risks and for whom, if screening was positive, there was also documentation they were informed of alternatives to driving in the last 12 months. |
| Advance care planning and palliative care counseling for patients with dementia | Percentage of patients with dementia who have an advance care plan or surrogate decision-maker documented in the medical record or documentation in the medical record that an advance care plan was discussed but the patient did not wish or was not able to name a surrogate decision-maker or provide an advance care plan. Percentage of patients with dementia or their surrogate decision-maker who received comprehensive counseling regarding ongoing palliation and symptom management and end-of-life decisions within two years of initial diagnosis or assumption of care. |
| Pain assessment and follow-up for patients with dementia | Percentage of patients with dementia who underwent documented screening for pain symptoms at every visit and, if screening was positive, also had documentation of a follow-up plan. |
| Pharmacological treatment of dementia | Percentage of patients with dementia or their caregivers with whom available guideline-appropriate pharmacologic treatment options and nonpharmacological behavior and lifestyle modifications were discussed at least once in the last 12 months. |
Source: Dementia Management Quality Measurement Set Update. American Medical Association, American Academy of Neurology Institute, American Psychiatric Association; 2016. https://www.aan.com/siteassets/home-page/policy-and-guidelines/quality/quality-measures/15dmmeasureset_pg.pdf.
In addition to the quality measurement set, the American Academy of Family Physicians (AAFP),3 the Alzheimer's Association,4 and others have developed toolkits that are evidence-based, user-friendly, informative, and scorable and can be incorporated into electronic health records (EHRs). They allow clinicians to systematically approach various domains of care, such as assessment and treatment of behavioral and psychiatric problems, and provide caregivers educational materials.
Combined with the measurement set, these tools give physicians quality improvement goals to strive for and the means to achieve them. (See “Dementia practice tools.") For example, measure eight, “Pain assessment and follow-up for patients with dementia,” includes the appropriate tools for clinicians to conduct this assessment and relevant resources for the caregiver. Physicians can use these materials to optimally address dementia care needs.
DEMENTIA PRACTICE TOOLS
| Measure 1: Disclosure of dementia diagnosis |
| Measure 2: Education and support of caregivers for patients with dementia |
| Measure 3: Functional status assessment for patients with dementia |
| Measure 4: Screening and management of behavioral and psychiatric symptoms associated with dementia |
| Measure 5: Safety concern screening and follow-up for patients with dementia |
| Measure 6: Driving screening and follow-up for patients with dementia |
| Measure 7: Advance care planning and palliative care counseling for patients with dementia |
| Measure 8: Pain assessment and follow-up for patients with dementia |
| Measure 9: Pharmacologic treatment of dementia |
Source: Cognitive Care Kit. Leawood, KS: American Academy of Family Physicians; November 2017. https://www.aafp.org/patient-care/public-health/cognitive-care.html.
CREATING DEMENTIA CARE PLANS
Physicians can also use these tools to develop comprehensive and organic care plans to achieve patient-centered goals. A dementia care plan has four core components:
- Defining and acting on the cognitive problems encountered,
- Managing the neurological, mental health, behavioral, and functional problems that result from the disease,
- Addressing relevant co-morbid conditions,
- Providing caregiver assistance.
The “Dementia care plan checklist” allows the clinician to address immediate needs, such as assessing safety to drive, while also encouraging long-range planning and goal setting, such as establishing a power of attorney and advanced directives. You should formally update the care plan every year or when disease progression is evident. An old adage for the care of patients with dementia is to “Provide safety and structure to the patient; sanity and serenity to the caregiver.” Many issues of dementia care are out of anyone's control, so it is important to plan for the known, common problems that develop with this condition.
Some elements of these plans can be delegated to a well-trained care team with adequate resources. For example, clinical staff could administer some of the assessment tools over the telephone before a visit, asking a family member about the patient's function and cognition. Conducting selected tests and surveys either before or after the planned physician visit can optimize clinic workflow. (See the “Cognitive impairment visit template.”) The practice could also develop protocols and provide training to enable clinical staff to help counsel patients and caregivers. Staff can provide patient evaluation and education handouts and connect patients and their caregivers with community resources, such as support groups and legal or financial services based on their priorities. Embedding these links in the practice's EHR can improve efficiency.
COGNITIVE IMPAIRMENT VISIT TEMPLATE
Incidentally, building relationships with community groups and service organizations can also result in referrals. The Carilion Clinic partnered with the Alzheimer's Association to sponsor a dementia care support group for patients and their caregivers.
DEMENTIA CARE PLAN CHECKLIST
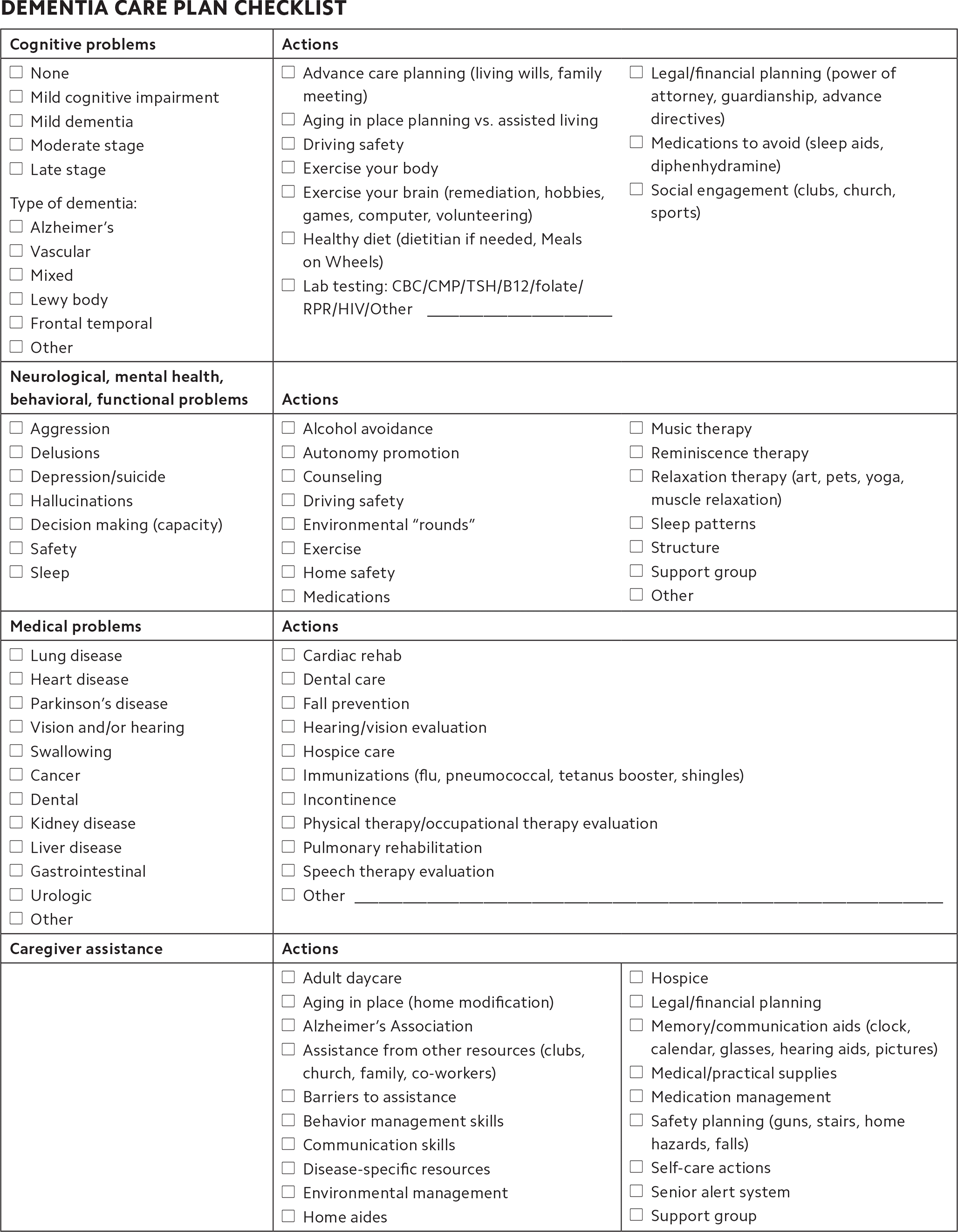
| Cognitive problems | Actions | |
| □ None □ Mild cognitive impairment □ Mild dementia □ Moderate stage □ Late stage Type of dementia: □ Alzheimer's □ Vascular □ Mixed □ Lewy body □ Frontal temporal □ Other | □ Advance care planning (living wills, family meeting) □ Aging in place planning vs. assisted living □ Driving safety □ Exercise your body □ Exercise your brain (remediation, hobbies, games, computer, volunteering) □ Healthy diet (dietitian if needed, Meals on Wheels) □ Lab testing: CBC/CMP/TSH/B12/folate/ RPR/HIV/Other _______________________ □ Legal/financial planning (power of attorney, guardianship, advance directives) □ Medications to avoid (sleep aids, diphenhydramine) □ Social engagement (clubs, church, sports) | |
| Neurological, mental health, behavioral, functional problems | Actions | |
| □ Aggression □ Delusions □ Depression/suicide □ Hallucinations □ Decision making (capacity) □ Safety □ Sleep | □ Alcohol avoidance □ Autonomy promotion □ Counseling □ Driving safety □ Environmental “rounds” □ Exercise □ Home safety □ Medications | □ Music therapy □ Reminiscence therapy □ Relaxation therapy (art, pets, yoga, muscle relaxation) □ Sleep patterns □ Structure □ Support group □ Other |
| Medical problems | Actions | |
| □ Lung disease □ Heart disease □ Parkinson's disease □ Vision and/or hearing □ Swallowing □ Cancer □ Dental □ Kidney disease □ Liver disease □ Gastrointestinal □ Urologic □ Other | □ Cardiac rehab □ Dental care □ Fall prevention □ Hearing/vision evaluation □ Hospice care □ Immunizations (flu, pneumococcal, tetanus booster, shingles) □ Incontinence □ Physical therapy/occupational therapy evaluation □ Pulmonary rehabilitation □ Speech therapy evaluation □ Other ___________________________________ _________________________________________ | |
| Caregiver assistance | Actions | |
| □ Adult daycare □ Aging in place (home modification) □ Alzheimer's Association □ Assistance from other resources (clubs, church, family, co-workers) □ Barriers to assistance □ Behavior management skills □ Communication skills □ Disease-specific resources □ Environmental management □ Home aides | □ Hospice □ Legal/financial planning □ Memory/communication aids (clock, calendar, glasses, hearing aids, pictures) □ Medical/practical supplies □ Medication management □ Safety planning (guns, stairs, home hazards, falls) □ Self-care actions □ Senior alert system □ Support group | |
Developed by Brian K. Unwin, MD, Natalia Loskutova, MD, Patrick Knicely, and Christopher D. Wood, DO. Copyright © 2019 American Academy of Family Physicians. Physicians may duplicate or adapt for use in their own practices; all other rights reserved.
GETTING PAID FOR DEMENTIA CARE
Delivering high-quality care to patients with cognitive impairment takes time, but Medicare only recently began reimbursing for it. CPT code 99483, “Assessment of and care planning for a patient with cognitive impairment,” was introduced in 2018 to facilitate payment for care provided to eligible individuals who are cognitively impaired or may have cognitive impairment. Physicians, physician assistants, nurse practitioners, clinical nurse specialists, and certified nurse midwives can bill under the code, which requires a comprehensive dementia assessment and a dementia care plan. (See “Required elements for CPT code 99483.”) The Medicare national payment allowance (not geographically adjusted) for 99483 is $241 in non-facility settings.5 There are a number of codes that cannot be billed on the same date of service as 99483, including those for routine office visits, care plan oversight, psychiatric diagnostic evaluation, advance care planning, and home health care and hospice supervision. By addressing dementia care comprehensively with dedicated visits, other appointments can address significant co-morbid conditions.
Rethinking what is important in caring for patients with dementia and using readily available clinical tools to address those issues allows physicians to render exceptional care not only to the millions of patients affected by these conditions but also the millions more who care for them.
REQUIRED ELEMENTS FOR CPT CODE 99483
- Record cognition-focused history, physical examination, and evaluation (include informant data).
- Document medical decision making of moderate or high complexity.
- Assess function (and needed level of assistance): – Activities of daily living: bathing, toileting, grooming, feeding, transferring, and continence.
– Instrumental activities of daily living: telephone, shopping, food preparation, housekeeping, laundry, transportation, medication management, and finances.
- Measure stage and severity of cognitive impairment using validated instruments.
- Review and reconcile medication use (including over-the-counter medications).
- Evaluate neuropsychiatric syndromes.
- Evaluate safety factors (e.g., medication, weapons, home hazards, falls, driving, and egress).
- Identify caregiver needs and supports.
- Conduct advance care planning discussion and palliation needs.
- Create care plan and document sharing with patient and/or caregiver.

