Providing Medicare wellness visits can be challenging but can improve quality and practice revenue.
Editor's note: This is a corrected version of the article previously published.

The Affordable Care Act of 2010 created the Medicare annual wellness visit (AWV) as a way to provide patients with comprehensive preventive care services at no cost. Yet many practices have been slow to provide substantial numbers of these visits. Only 15.6 percent of eligible patients received an AWV through 2014.1 In addition to finding lackluster overall participation, researchers have found AWV rates are lower among practices caring for underserved populations, such as racial minorities, rural residents, or those dually enrolled in Medicaid.2
Physicians and other health care providers do not offer AWVs to their Medicare patients for numerous reasons. Providing and documenting all of the required AWV elements efficiently can be challenging, and some practices may feel their staffing or electronic health record resources are too limited. Many patients and even some physicians may not know what the AWV entails, and patients with complex socioeconomic risk factors may have pressing health conditions that need to take priority over preventive services. These explanations can all be valid, but this article seeks to help physicians reevaluate the AWV, along with the initial preventive physical examination (IPPE) or “Welcome to Medicare” visit, and recognize the value these wellness visits can bring not only to their patients but also to their practices or health care organizations.
KEY POINTS
- The Medicare annual wellness visit (AWV) and the initial preventive physical examination (IPPE) provide a number of benefits to patients and physicians, but many physicians still do not provide them.
- Medicare wellness visits can help physicians address care gaps and report quality measures important in pay-for-performance systems.
- When billed correctly and delivered efficiently along with other covered Medicare preventive services, AWVs can boost practice revenue.
THE VALUE OF MEDICARE WELLNESS VISITS
The main benefit of the AWV to patients is the creation of a personalized prevention plan, a written plan that can help guide their preventive care decisions for the next five to 10 years. This plan includes age-appropriate preventive services, recommendations offered by both the U.S. Preventive Services Task Force and the Advisory Committee on Immunization Practices, and personalized health advice that identifies risk factors and suggests referrals or programs to address them.3
Providing Medicare wellness visits also offers a structure that helps physicians to close many pay-for-performance quality measure gaps, including those recognized by the Core Quality Measures Collaborative, the Integrated Healthcare Association’s California Value Based P4P program, and the National Committee for Quality Assurance’s Healthcare Effectiveness Data and Information Set. In addition, accountable care organizations participating in the Medicare Shared Savings Program can use data collected during wellness visits to satisfy specific quality measures for the 2018 and 2019 quality reporting years.4 (See “Closing quality measure gaps.”)
There also are financial incentives to implementing AWVs. Physicians participating in Medicare’s Merit-based Incentive Payment System (MIPS) can use AWVs to raise their quality scores, which can potentially lead to positive Medicare payment adjustments. Practices that provide AWVs often generate greater revenue than those that do not – a result of billing AWVs with associated preventive services and same-day problem-oriented services.2 AWVs also provide physicians another opportunity to assess and report risk-adjusted diagnoses for Medicare Advantage beneficiaries. Future payment rates for higher risk patients are calculated based on risk-adjusted factor (RAF) scores, so addressing Hierarchical Condition Category-related diagnoses in the same visit can be of additional value. (For more on this subject, see “Is Your Diagnosis Coding Ready for Risk Adjustment?” FPM, March/April 2018, and “Diagnosis Coding for Value-Based Payment: A Quick Reference Tool,” FPM, March/April 2018.)
CLOSING QUALITY MEASURE GAPS
Many pay-for-performance measures can be addressed during Medicare wellness visits, including these, which are associated with the following programs: Core Quality Measures Collaborative (Collaborative), the Integrated Healthcare Association’s California Value Based P4P Program (IHA), and the National Committee for Quality Assurance’s Healthcare Effectiveness Data and Information Set (HEDIS). Measures used by the Medicare Shared Savings Program (MSSP) 2018 and 2019 reporting years are also listed.
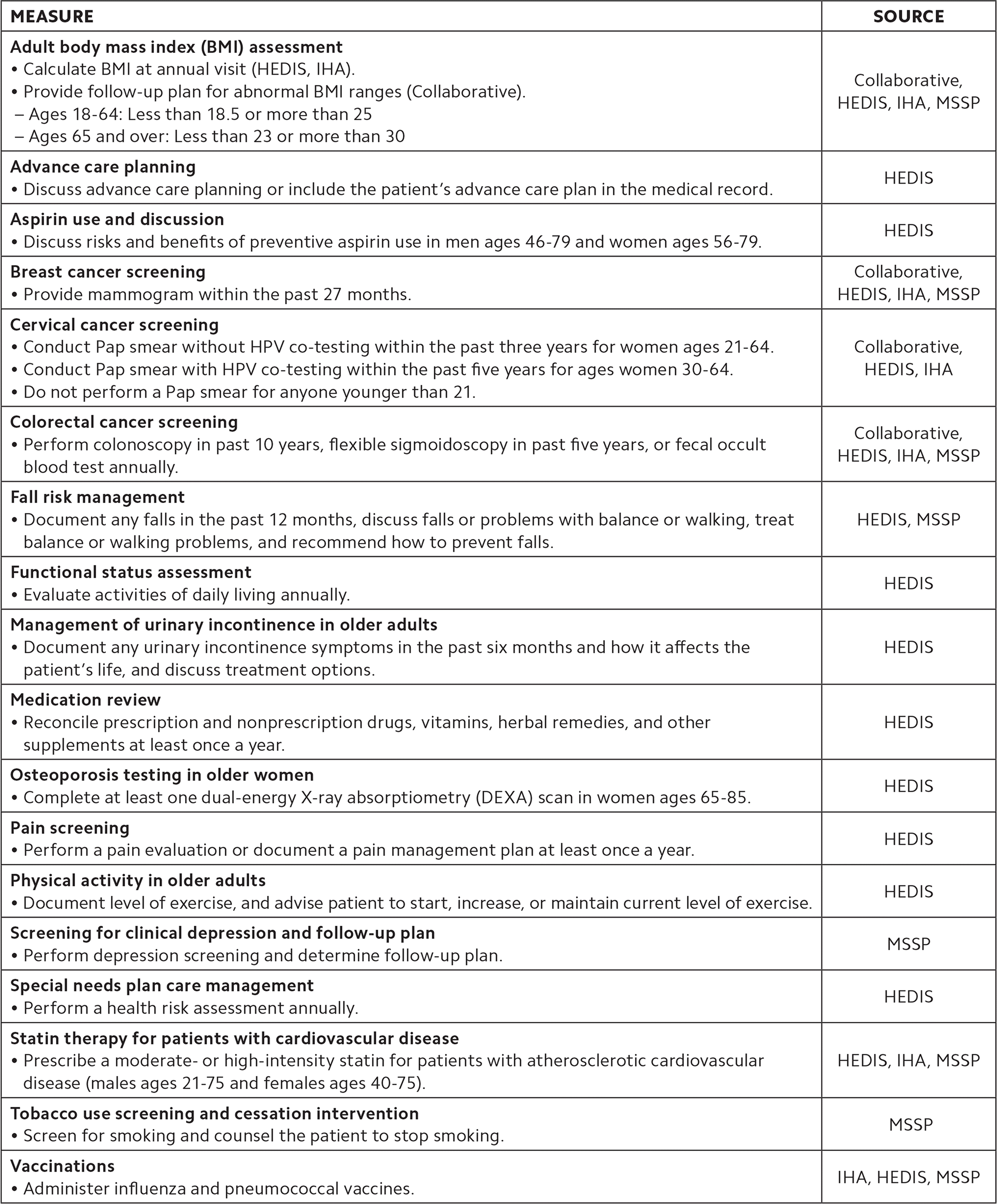
| MEASURE | SOURCE |
|---|---|
Adult body mass index (BMI) assessment
| Collaborative, HEDIS, IHA, MSSP |
Advance care planning
| HEDIS |
Aspirin use and discussion
| HEDIS |
Breast cancer screening
| Collaborative, HEDIS, IHA, MSSP |
Cervical cancer screening
| Collaborative, HEDIS, IHA |
Colorectal cancer screening
| Collaborative, HEDIS, IHA, MSSP |
Fall risk management
| HEDIS, MSSP |
Functional status assessment
| HEDIS |
Management of urinary incontinence in older adults
| HEDIS |
Medication review
| HEDIS |
Osteoporosis testing in older women
| HEDIS |
Pain screening
| HEDIS |
Physical activity in older adults
| HEDIS |
Screening for clinical depression and follow-up plan
| MSSP |
Special needs plan care management
| HEDIS |
Statin therapy for patients with cardiovascular disease
| HEDIS, IHA, MSSP |
Tobacco use screening and cessation intervention
| MSSP |
Vaccinations
| IHA, HEDIS, MSSP |
HOW TO CODE FOR MEDICARE WELLNESS VISITS
The type of wellness visit you report depends on when the patient joined Medicare.
The IPPE is a one-time physical exam performed within the first 12 months of a patient’s enrollment under Part B Medicare. The initial AWV can be provided 12 months after the patient first enrolled or 12 months after he or she received the IPPE. A subsequent AWV can then be provided annually.
Physicians should bill for preventive services provided in addition to the AWV or IPPE, many of which carry work relative value units (wRVUs) that can affect their productivity scores and revenue. Some of these services are payable by Medicare in addition to the AWV or IPPE and can be performed several times during the year. However, patients and physicians should be aware that a few of these services do have a copay or deductible. (See “Medicare-covered preventive services.”)
MEDICARE-COVERED PREVENTIVE SERVICES
This table includes preventive services that generate work relative value units (wRVUs). For a complete list of Medicare preventive services, see https://go.cms.gov/2sK65XA.
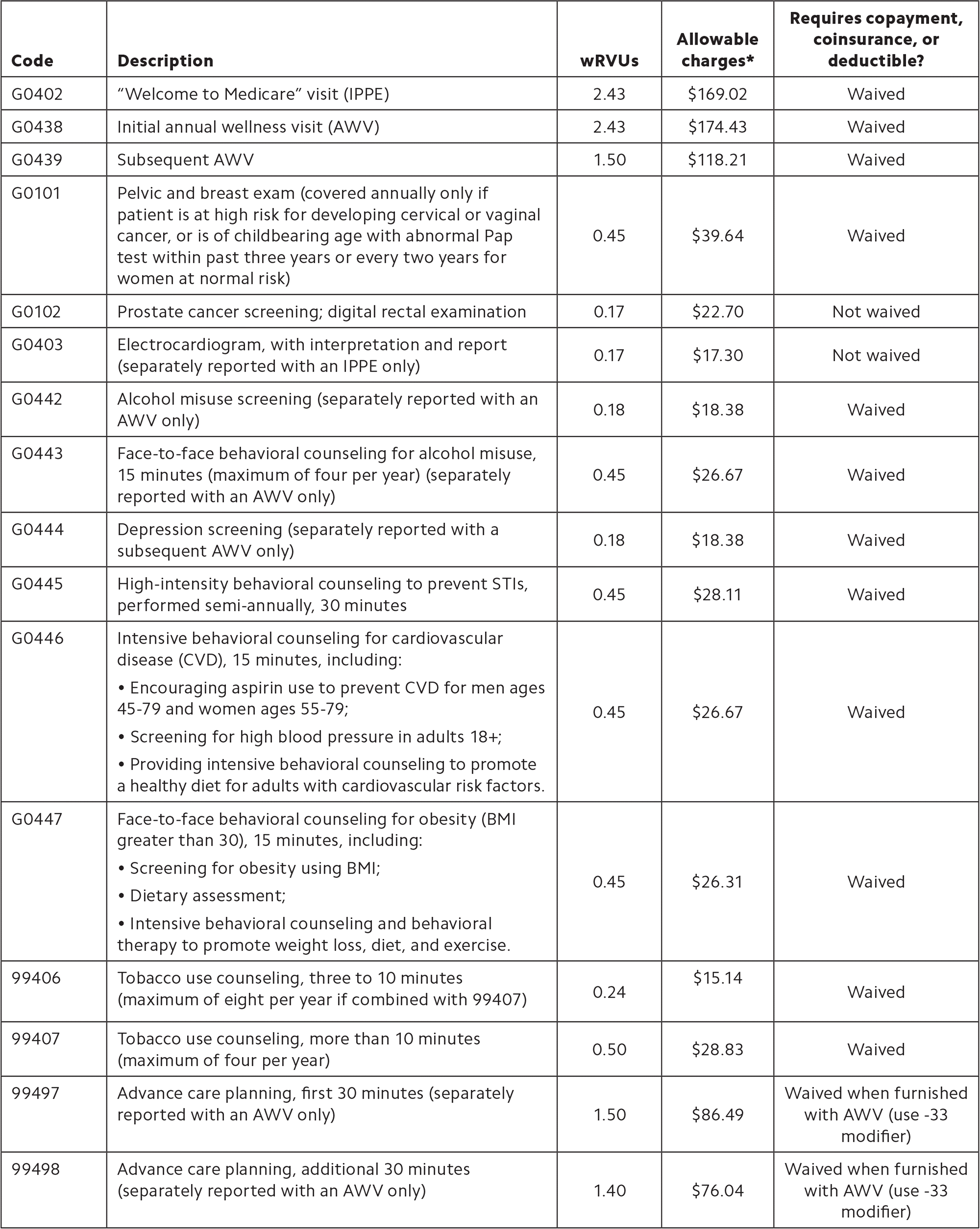
| Code | Description | wRVUs | Allowable charges* | Requires copayment, coinsurance, or deductible? |
|---|---|---|---|---|
| G0402 | “Welcome to Medicare” visit (IPPE) | 2.43 | $169.02 | Waived |
| G0438 | Initial annual wellness visit (AWV) | 2.43 | $174.43 | Waived |
| G0439 | Subsequent AWV | 1.50 | $118.21 | Waived |
| G0101 | Pelvic and breast exam (covered annually only if patient is at high risk for developing cervical or vaginal cancer, or is of childbearing age with abnormal Pap test within past three years or every two years for women at normal risk) | 0.45 | $39.64 | Waived |
| G0102 | Prostate cancer screening; digital rectal examination | 0.17 | $22.70 | Not waived |
| G0403 | Electrocardiogram, with interpretation and report (separately reported with an IPPE only) | 0.17 | $17.30 | Not waived |
| G0442 | Alcohol misuse screening (separately reported with an AWV only) | 0.18 | $18.38 | Waived |
| G0443 | Face-to-face behavioral counseling for alcohol misuse, 15 minutes (maximum of four per year) (separately reported with an AWV only) | 0.45 | $26.67 | Waived |
| G0444 | Depression screening (separately reported with a subsequent AWV only) | 0.18 | $18.38 | Waived |
| G0445 | High-intensity behavioral counseling to prevent STIs, performed semi-annually, 30 minutes | 0.45 | $28.11 | Waived |
| G0446 | Intensive behavioral counseling for cardiovascular disease (CVD), 15 minutes, including:
| 0.45 | $26.67 | Waived |
| G0447 | Face-to-face behavioral counseling for obesity (BMI greater than 30), 15 minutes, including:
| 0.45 | $26.31 | Waived |
| 99406 | Tobacco use counseling, three to 10 minutes (maximum of eight per year if combined with 99407) | 0.24 | $15.14 | Waived |
| 99407 | Tobacco use counseling, more than 10 minutes (maximum of four per year) | 0.50 | $28.83 | Waived |
| 99497 | Advance care planning, first 30 minutes (separately reported with an AWV only) | 1.50 | $86.49 | Waived when furnished with AWV (use -33 modifier) |
| 99498 | Advance care planning, additional 30 minutes (separately reported with an AWV only) | 1.40 | $76.04 | Waived when furnished with AWV (use -33 modifier) |
(*) Based on the 2019 Medicare Physician Fee Schedule, non-facility national payment amount
If you provide advance care planning (ACP), CPT code 99497 or 99498, at the same visit, make sure to append modifier 33, “Preventive service,” so that the usual coinsurance and deductible charged for the ACP is waived.5 You may need to append modifiers to other preventive service codes as well, to avoid bundling. Practices should check with their Medicare contractor for guidance.
To find out how many wRVUs a particular service is worth, see the 2019 Medicare Physician Fee Schedule) or the wRVU calculator provided by the American Academy of Professional Coders.
Below are some examples of wellness visits and the wRVUs resulting from each one.
Patient 1: A 67-year-old male, who is an established patient of your practice, is seeing you for an initial AWV. His chronic problems include hypertension and dyslipidemia. He is taking hydrochlorothiazide 25 mg per day and atorvastatin 20 mg at bedtime. His history and the health risk assessment he completed confirm he has smoked one pack of cigarettes per day for 34 years. He does not have an advance directive. He rarely drinks alcohol, and his PHQ-2 depression screening score is zero. His vital signs are stable with good blood pressure control. His BMI is 33.7. He requests a digital rectal exam (DRE) because his father had prostate cancer. You create the patient’s personalized prevention plan and discuss your clinical recommendations with the patient, who agrees to receive several preventive services, including a lipid panel, diabetes screening, hepatitis C screening, lung cancer screening with a low-dose CT scan, a pneumococcal vaccination, a DRE, and AAA screening with ultrasound. You order the labs and imaging, provide counseling focused on several of the patient’s health risk behaviors, and recommend a follow-up visit in six months or sooner if needed to address test results.
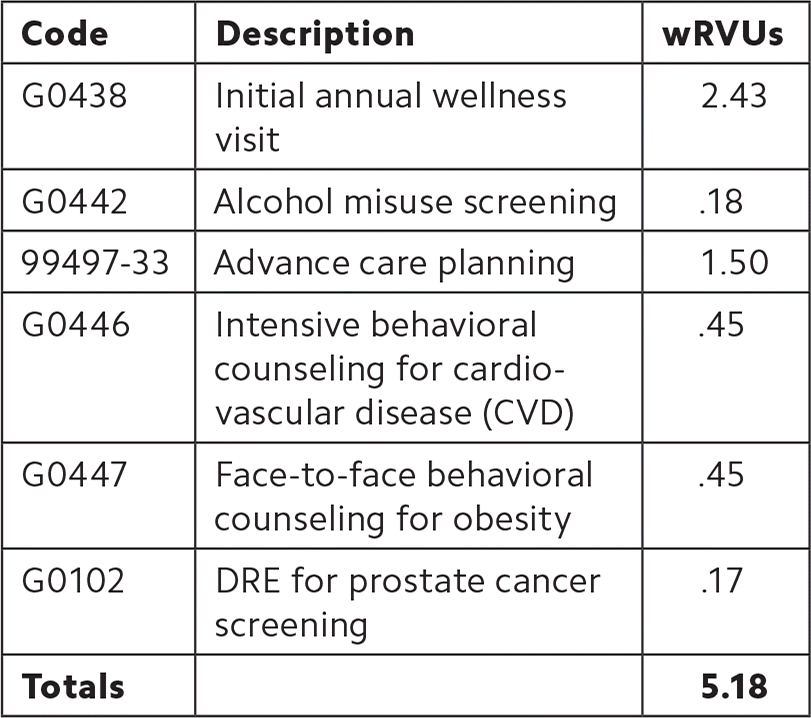
| Code | Description | wRVUs |
|---|---|---|
| G0438 | Initial annual wellness visit | 2.43 |
| G0442 | Alcohol misuse screening | .18 |
| 99497-33 | Advance care planning | 1.50 |
| G0446 | Intensive behavioral counseling for cardiovascular disease (CVD) | .45 |
| G0447 | Face-to-face behavioral counseling for obesity | .45 |
| G0102 | DRE for prostate cancer screening | .17 |
| Totals | 5.18 |
Patient 2: A 77-year-old female, who is an established patient of your practice, is seeing you for her first AWV. She has a Medicare Advantage insurance plan. Her previous office visit was about nine months ago. She has diabetes, hypertension, peripheral neuropathy, glaucoma, mild major depression, anxiety, and COPD. She is due for her routine lab work and is requesting refills of all her medications. She would like a flu shot, but the rest of her immunizations are current. Her list of medications includes metformin 500 mg twice a day, sitagliptin 50 mg daily, lisinopril 10 mg daily, gabapentin 300 mg three times per day, albuterol as needed, tiotropium daily, alprazolam 0.25 mg daily as needed, sertraline 50 mg daily, and dorzolamide ophthalmic twice a day. She has tried in the past to wean herself off the alprazolam but needs it to control her anxiety; she fills her prescription for 30 pills every three or four months, which you confirm via a controlled substance prescription database. Her history, along with her health risk assessment, shows she drinks up to three glasses of wine per day. She does not have an advance directive. Her vital signs are stable with good blood pressure control, and her BMI is 22.4. You address her concerns and order labs appropriate to her chronic medical conditions, refill her medications, order a flu shot, provide counseling related to her health risk behaviors, and discuss your preventive service recommendations as part of her personalized prevention plan, which includes ordering a DEXA scan.
Given the complexity of her health status, you ask her to schedule a follow-up appointment in one week to go over her lab results. Also, because the patient is a Medicare Advantage beneficiary, you remember to assess and report risk-adjusted diagnoses and HCC codes.
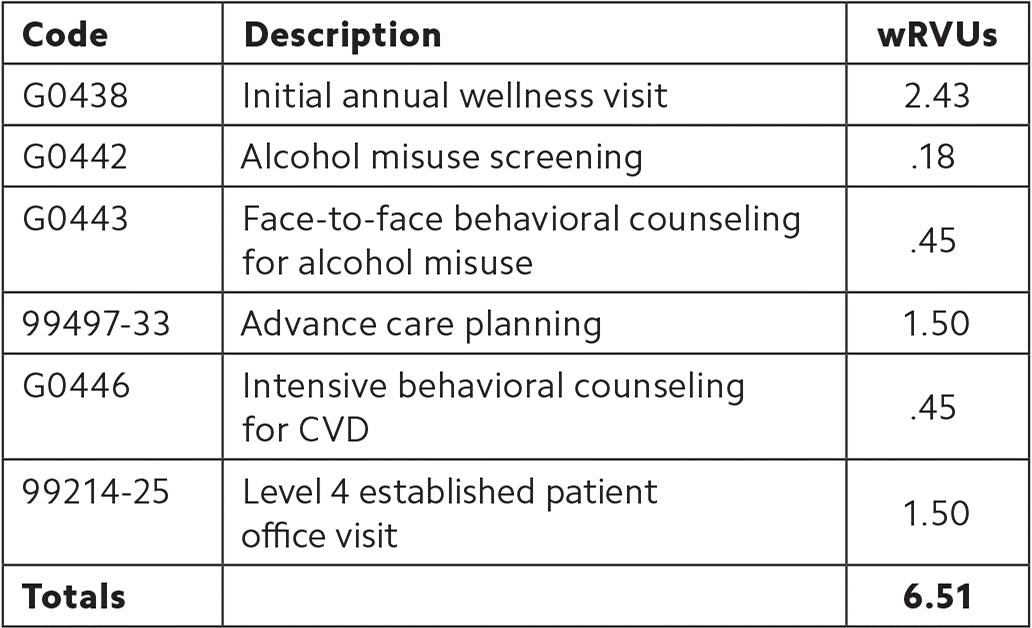
| Code | Description | wRVUs |
|---|---|---|
| G0438 | Initial annual wellness visit | 2.43 |
| G0442 | Alcohol misuse screening | .18 |
| G0443 | Face-to-face behavioral counseling for alcohol misuse | .45 |
| 99497-33 | Advance care planning | 1.50 |
| G0446 | Intensive behavioral counseling for CVD | .45 |
| 99214-25 | Level 4 established patient office visit | 1.50 |
| Totals | 6.51 |
Patient 3: A 57-year-old female, who is an established patient of your practice, recently became disabled. She now has dual insurance coverage with Medicare and Medicaid. She is scheduled for her “Welcome to Medicare” visit. She was seeing a partner of yours who recently retired, and she has transferred to you for care. Her last visit was four weeks ago, and her diabetes lab work at that time showed that her A1C was 6.7 and her LDL was 94. She had her annual eye exam two months ago. She has diabetes, hypertension, and end-stage renal disease (ESRD). Her list of medications includes insulin glargine 10 units at bedtime, insulin aspart on a sliding scale, amlodipine 5 mg daily, and pravastatin 10 mg at bedtime. Her history, along with her health risk assessment, shows that she has multiple sex partners. She does not drink alcohol and does not smoke. Her PHQ-2 depression screening is 0. Her last mammogram was three years ago, and her last Pap smear was six years ago. She has not received her pneumococcal vaccine. She has never had a colonoscopy or fecal occult blood testing. Her vital signs are stable with good blood pressure control and a BMI of 27.1. She has been feeling sick for the last two weeks with sinus infection symptoms. You treat her for a sinus infection, perform a gynecologic exam and Pap smear, and update her pneumococcal vaccination. You discuss and then order screens for hepatitis B, hepatitis C, HIV, and sexually transmitted infections (STIs), in addition to a mammogram. You also agree to make referrals for a colonoscopy and medical nutrition therapy for ESRD. Finally, you ask her to follow up in four to six months or as needed.
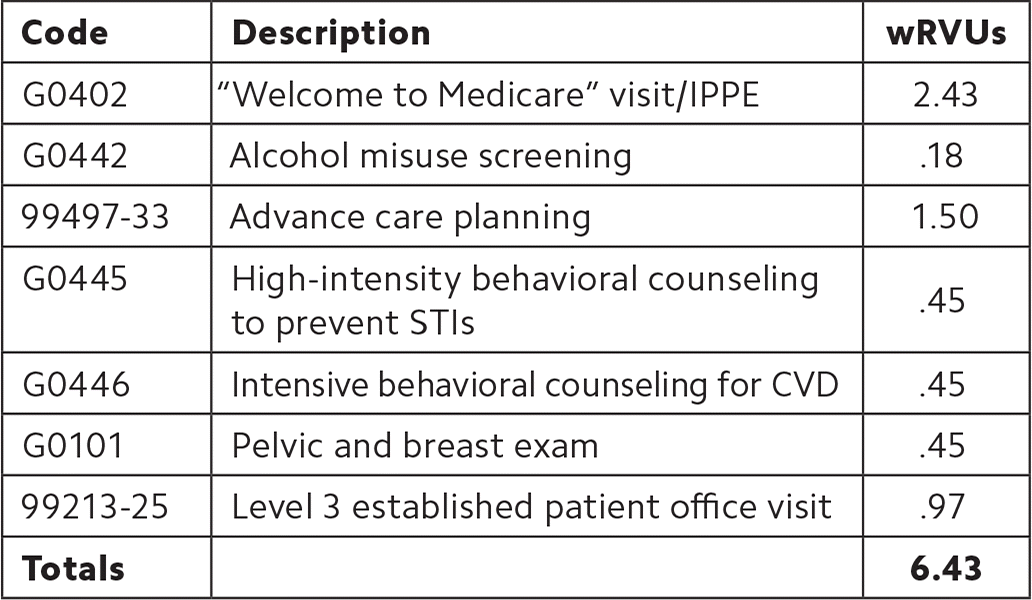
| Code | Description | wRVUs |
|---|---|---|
| G0402 | “Welcome to Medicare” visit/IPPE | 2.43 |
| G0445 | High-intensity behavioral counseling to prevent STIs | .45 |
| G0446 | Intensive behavioral counseling for CVD | .45 |
| G0101 | Pelvic and breast exam | .45 |
| Q0091 | Screening Pap smear | .37 |
| 99213-25 | Level 3 established patient office visit | .97 |
| Totals | 5.12 |
MEETING THE CHALLENGE
Providing wellness visits is not easy, but there are ways to make your practice more prepared. For example, a nurse or medical assistant could handle pre-visit planning to make the physician-led visit more efficient.6 Another variation of the team-based model, which used a dedicated scheduler to contact Medicare patients about AWVs and then clinical pharmacists and licensed practical nurses to provide the visits, significantly increased use of preventive services.7 It may also be worthwhile to set aside more time for these types of visits. While some visits can be completed in 30 to 40 minutes, more complicated encounters may take longer. Your EHR may also have templates and other tools available to make providing Medicare wellness visits more efficient, although the range of EHR capabilities is too wide to discuss here.
Regardless of how you schedule and perform these visits, you should recognize that Medicare wellness visits have great value in not only providing important preventive services to the patient but also closing quality measure gaps and contributing financial stability to a practice or organization.

