A single screening question and an arsenal of cost-reducing strategies can help you help your patients afford their medications.

Patients are increasingly concerned about growing out-of-pocket prescription costs.1 In 2017, the United States spent $1,025 per capita on prescription drugs.2 High prescription costs are a leading reason why patients do not take their prescribed medications, resulting in avoidable emergency department visits and hospitalizations.3–5 High prescription costs can further affect patients' ability to pay rent and other bills, and to purchase food.6–8
Despite the impact of prescription costs on adherence, most patients will not mention their cost concerns unless specifically asked.9–11 Instead, patients tend to engage in a range of cost-saving strategies such as not picking up a prescription or skipping doses to conserve quantities.6 The clinical ramifications of these behaviors are significant, and identifying these patterns is essential to successfully managing chronic diseases. Fortunately, feasible office-based strategies exist to assist patients in reducing their medication costs.12–13
Herein, we present a practical approach to screening and management of patients' cost-related medication concerns. We piloted this approach in seven primary care practices and found that it doubled discussions of patients' out-of-pocket prescription costs and was viewed as useful by patients, clinicians, and staff.14
KEY POINTS
- High prescription costs are a common reason for medication non-adherence, but most patients will not mention their cost concerns unless specifically asked.
- Screening patients for prescription cost concerns can be accomplished with a single question.
- All staff members can play a meaningful role in addressing cost-related medication nonadherence, and each role should be clearly identified in your practice's workflow.
STEP ONE: HAVE YOUR STAFF CONDUCT A ONE-QUESTION SCREENING
Screening patients and then addressing their prescription cost concerns should be a team effort, analogous to depression screening and treatment. Having staff handle the first step, the screening, reduces the burden on the physician and engages key team members in the office. Practice staff are frequently more involved with patients' prescription cost concerns than physicians realize. Patients often share information with reception and nursing staff through phone messages and refill requests. Moreover, some patients may be more apt to share information about their nonadherent behaviors with nursing or other office staff than with their physician. We learned from our pilot that staff often want to help, and there is a meaningful role for all staff members in addressing cost-related medication nonadherence.
Identifying patients who have prescription cost concerns requires systematic screening. In some cases, patients might have indicators of cost concerns such as poor control of chronic diseases or exhibit some indirect evidence of sporadic medication adherence. However, screening based solely on poor adherence or even presumed patient income will miss many patients who have prescription cost concerns.
Although little empirical evidence exists to guide the wording of a screening question, we found it effective in our pilot to simply ask patients, “Is the cost of any of your medications a burden for you?”14 We encouraged practices to adapt this question as necessary, using straightforward wording and matter-of-fact body language to normalize conversations about prescription costs.
A SINGLE SCREENING QUESTION
“Is the cost of any of your medications a burden for you?”
Screening for prescription cost burdens should be conducted in a way that preserves patients' privacy and is compatible with the practice workflow. Screening at the point of medication reconciliation offers a natural time for many practices. Some of the practices in our pilot asked patients to complete a self-administered questionnaire before visits that included medication reconciliation along with a question to help identify any medications that pose a cost burden. In other practices, staff began the screening process in the exam room. All practices developed ways for relaying this information to the prescribing physician. For example, staff who reviewed the questionnaire or conducted the medication reconciliation recorded the findings in a standardized place in the medical record. Physicians then had to adopt the critical habit of reviewing what staff had entered to avoid missing valuable information obtained during the screening. (See “A sample workflow for screening and addressing cost concerns.”)
To aid screening efforts, practices can post information in the reception area and exam rooms to signal that physicians and staff are interested in assisting patients in addressing their prescription cost concerns. A simple sign stating, “Having trouble affording your medications? Tell your doctor or nurse today!” may suffice.
A SAMPLE WORKFLOW FOR SCREENING AND ADDRESSING COST CONCERNS
Front-desk receptionist:
- Asks the patient to review his or her medication list, which involves crossing out inactive medications, writing down new medications, and circling any that are a cost burden.
Rooming nurse:
- Reviews the list with the patient in the exam room and confirms that the circled prescriptions are a cost burden.
- Adds concerns about the cost of the circled prescriptions to the patient's chief complaint in the medical record.
Clinician:
- Reviews prescription concerns with the patient to identify causes.
- Considers whether the medication is still necessary and, if not, whether a deprescribing trial is feasible.
- Considers extended prescriptions.
- Considers lower-cost alternatives, discount programs, and cost-saving websites and apps.
- Refers the patient as needed to office staff or community-based organizations to assist with insurance concerns, including eligibility for low-income subsidies.
STEP TWO: USE BRIEF COST-REDUCING STRATEGIES DURING VISITS
During the office visit, clinicians in our pilot confirmed with the patient any concerns identified from the screening and then briefly explored the circumstances. Cost burdens can result from a variety of causes, such as unmet deductibles or the use of brand name drugs (see “Common reasons for medication-related cost burdens”). Identifying the contributing factors is important because they can inform mitigation strategies.
COMMON REASONS FOR MEDICATION-RELATED COST BURDENS
- Lack of insurance coverage
- Unmet deductibles
- Dispensing pharmacy does not have correct insurance information on file
- Use of high-tiered or brand name drugs
- Paying cash for medications denied by the insurance
- Entering the Medicare Part D coverage gap (“donut hole”)
Clinicians in our pilot employed various strategies to help patients address prescription cost concerns (see “Cost-saving strategies”):
- Review the necessity of the patient's medications, and offer a deprescribing trial when appropriate.15
- Use extended (e.g., 90-day) prescriptions to reduce copayments, improve medication adherence, and reduce practice time devoted to processing refills.13,16
- Substitute a less costly medication,17 or use discount programs such as the “$4 lists” offered by most large chain pharmacies.18 Even patients with adequate insurance coverage may benefit from using these drug lists. For example, a patient on lisinopril 10 mg, once daily could go from paying a tier-one copay of $10 for a 30-day supply to paying $4 for a 30-day supply, an annual savings of $72. The cost savings can be even greater if 90-day supplies are prescribed. If this patient also begins filling other tier-one medications through the $4 plan, such as glipizide, metformin, and atorvastatin, the annual savings become quite substantial.
- Use websites and apps such as https://www.goodrx.com that provide comparative costs between pharmacies and coupons for prescription medications. One study found that in nearly a quarter of filled prescriptions, patient copayments exceed the reimbursement pharmacies receive from insurance,19 so shopping around can help. Both GoodRx coupons and the $4 programs can be used by patients with Medicare coverage.
COST-SAVING STRATEGIES
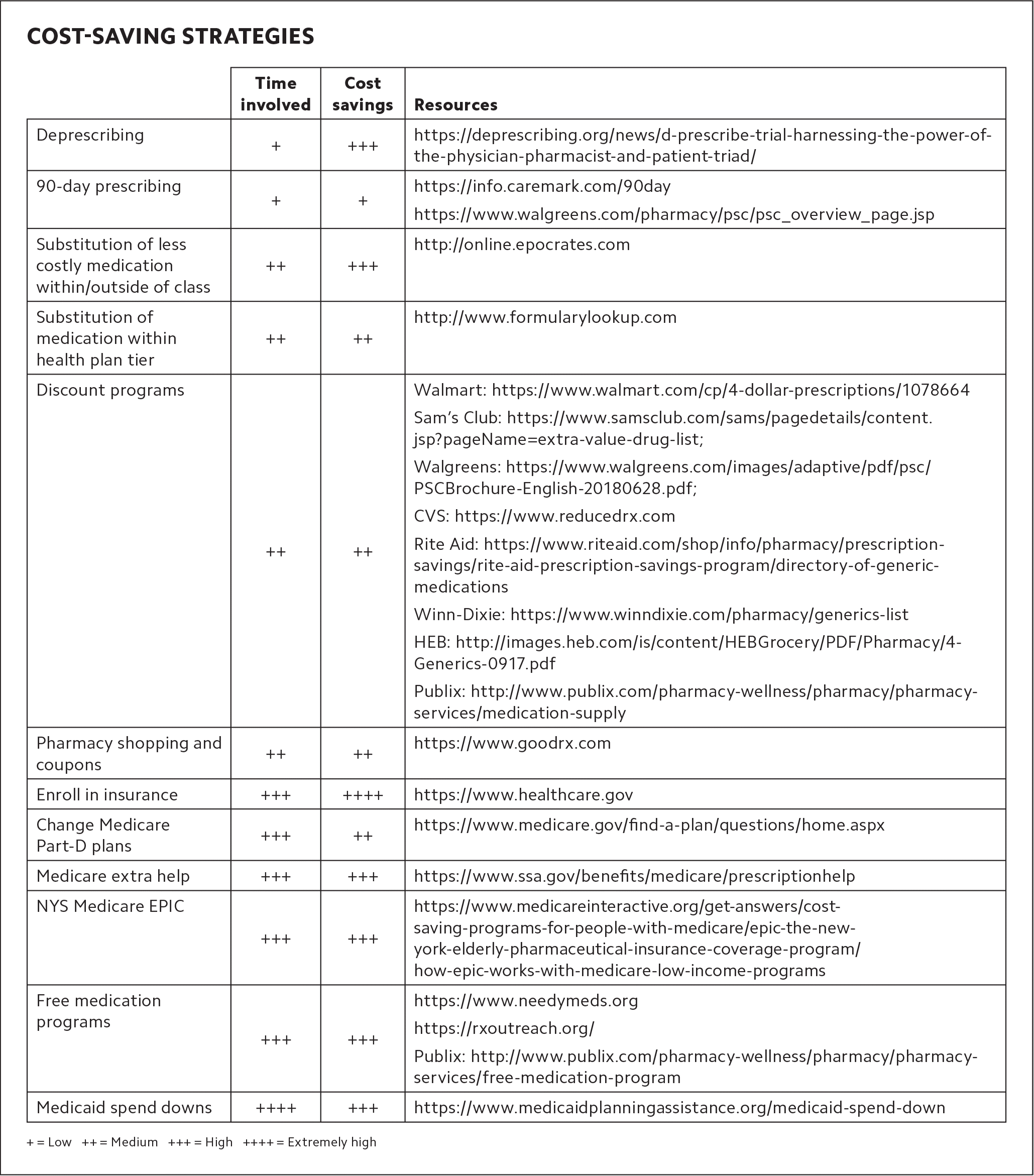
+ = Low ++ = Medium +++ = High ++++ = Extremely high
STEP 3: REFER PATIENTS WHO NEED MORE ASSISTANCE
At times, patients may require more intensive support to address complex prescription cost issues. For example, patients may need additional help navigating insurance plans, determining eligibility for additional insurance coverage (such as low-income subsidies), and applying for pharmaceutical medication assistance programs, all of which require a high degree of health/insurance literacy. When available, care managers or social workers can provide valuable expertise in these areas. In practices without these resources, another member of the clinical staff can be identified to serve as a champion and provide assistance. In addition, local health systems may have resources available to assist patients.
Even when patients or their families have the resources and literacy to research these issues themselves, they may still need some guidance from the medical office. In other cases, particularly those involving life-saving medications or patients with limited health/insurance literacy, practices should always offer this additional support.
The resources listed in “Cost-saving strategies” can be given to patients as well. Additionally, practices could create flyers that include tips for reducing prescription costs and make them available in the reception area or include general cost-saving tips in after-visit summaries to provide valuable education to patients.
KEEPING THE BENEFITS IN MIND
Adding another screening to primary care may sound overwhelming, but with a team effort and a clear workflow, addressing patients' prescription cost concerns is doable. Keeping the benefits in mind can help practices sustain their efforts. Patients in our pilot appreciated that clinicians and staff asked about their cost burdens and tried to help them. Identifying and addressing concerns about medication costs are important steps toward partnering with patients to reduce barriers, improve medication adherence, and ultimately improve their health.

