In an era of patient-centered medical homes and value-based care, the old approach to physician orientation just doesn't cut it.

Consider the following tale of two orientations. Which one would you want if you were new to a practice?
Orientation 1: A physician arrives at his first job out of residency and is excited to start — until he learns that he will also be serving as clinic director because the other two physicians are leaving. During his first week, he finds out that the clinic needs to transition toward a patient-centered medical home (PCMH) and that patient satisfaction is low and needs to be addressed. The office manager gives the new physician a sheet of paper with a few notes regarding common patient forms and the time of staff meetings but no other information. He struggles for the next six months.
Orientation 2: After moving to be closer to family, a physician starts a new job with a new organization. She arrives feeling uncertain about what to expect but is pleasantly surprised by the clinic's efficient, organized, and well-thought-out orientation plan. The clinic director meets with her on day one and takes time to explain the expectations. The new physician then meets with all members of the team, including extended team members, who explain their roles and the ways they can assist in patient care. The new physician is given a reasonable workload that increases incrementally over the first six months. She stays at the organization for the next 20 years.
KEY POINTS
- A well-organized orientation can help maximize physician performance and retention.
- Physician orientation needs to include not only policies and procedures but also social engagement and training related to the specific practice model.
- Set a reasonable and gradual plan to help the new physician reach performance goals.
THE CASE FOR A NEW APPROACH TO PHYSICIAN ORIENTATION
Getting oriented to a new practice can be daunting, particularly if the new physician is unfamiliar with the practice model, such as a PCMH or value-based care model. These models often require significant changes in practice patterns in addition to all the other changes inherent in a new position.
In 2010, our organization, the Department of Veterans Affairs, became the largest integrated health system in the United States to implement the PCMH model.1 This ambitious and sometimes difficult shift from the traditional provider-centric model led to an increase in the number of primary care patients1 but also an increase in provider turnover.2 It necessitated a new approach to provider orientation.
Practices often dedicate a great deal of planning and time to recruitment but less to orientation. The complexity of health care delivery, the highly competitive job market, and the focus on physician and staff satisfaction as a driver for patient satisfaction all contribute to the need for standardizing orientation. High-quality orientation can maximize a physician's performance and is the first step in a meaningful retention effort. It can be touted during the recruitment process as demonstration of the practice's commitment to physician education and engagement.
The components of physician orientation differ from those a human resources (HR) department or medical center would typically cover under “new employee orientation.” HR often focuses on a broad orientation to the work site, benefits, and policies geared toward all employees, while medical center orientation often covers information about the organization's mission and goals as well as basic clinical information such as privacy and infection control.
In this article, we present a framework for organizing orientation for new physicians. Although practices may already have their own orientation with didactic sessions, web-based modules, handbook reviews, or a hybrid of these modalities, this article suggests other steps that can complement procedures already in place. These six orientation components are purposely broad in nature so they can be modified to align with a practice's current plan. They focus on the PCMH model of care but can be applied to many settings for physicians and other clinical staff.
1. BE DELIBERATE ABOUT SOCIAL ENGAGEMENT OF THE NEW PHYSICIAN AND CURRENT STAFF.
Don't trust that social engagement of the new physician will just happen naturally. Be purposeful about it. This begins prior to the physician's arrival with periodic “check-in” emails or calls to see how the relocation process and preparation paperwork associated with credentialing and privileging are progressing. Another component of social engagement includes email or staff meeting announcements that provide a brief biographical sketch of the new clinician before his or her arrival. Depending on your setting, you may also want to consider a local newspaper or website announcement including the physician's specialty area and biographical information.
Other social components may include the following:
- Personally introduce the physician at his or her first staff meeting.
- Post a welcome sign or other visual acknowledgment on the physician's first day.
- Have a peer or clinical supervisor grab coffee or lunch with the new physician. Because the first day can be overwhelming, providing a few minutes to sit and decompress can be a welcoming gesture.
- Provide a list of local restaurants or cultural attractions if the physician is new to the area.
- Provide a roster of colleagues, including their pictures, interests, educational background, years at current site, or other applicable information.
- Finally, assign a “buddy” to help with daily questions. This helps distribute the orientation work and gets others invested in the process. In a small practice, the buddy may be the new physician's supervisor, but in a larger practice, a new physician could be paired with a colleague. Two benefits of the latter approach are that sometimes new employees may feel more comfortable asking a peer a question, and the direct supervisor may be less accessible than a peer. The buddy can help share pearls he or she has learned, such as who to contact within specific departments, how to access templates in the electronic health record (EHR) system, and other efficiency tips.
2. HELP THE PHYSICIAN GET ACQUAINTED WITH THE WORKSPACE.
Getting oriented to the physical workspace is critical to the new physician feeling welcome, confident, and productive. This includes work-station assignment, a tour of the practice to meet staff and locate key areas (including the bathroom, lunch area, and refrigerator), and distribution of supplies, the white coat, and other items. The tour should also include the exam rooms so the physician can see what standard equipment is available, where additional equipment and supplies are stored, and what to do with used supplies. If your practice is large, consider using a “scavenger hunt” to help the new physician find key items such as the defibrillator, chemical safety data sheets, the lab, and safety exits. Making the orientation more active will increase knowledge retention.
3. MAKE EMERGENCY PREPAREDNESS A PRIORITY.
On day one, introduce the new physician to any emergency plans for the practice so that if an emergency arises after orientation, the new physician will know how to respond effectively and efficiently. Topics should include location of the code cart if applicable, when to call 911, treatment of on-site anaphylaxis, how to respond to violent patients, and what to do in the event of a fire, natural disaster, or power outage. You should also review your state and facility policies on reporting domestic violence, child abuse or neglect, elderly abuse, and unsafe drivers. Ideally, this aspect of training will be repeated annually, so decide how you will track it and who will provide it moving forward.
4. CREATE AN ORIENTATION CHECKLIST.
This checklist should list key topics a supervisor or subject matter expert needs to review verbally with the new physician. For example, a clinical pharmacist could review on-site pharmacy processes, if applicable. The supervisor could review preferred forms of communication between staff and with the supervisory chain, including use of email, staff meetings, huddles, or communication boards, as well as email use with patients, social media policies, and cell phone use while at work. For PCMH practices, the checklist could also include reviewing the philosophy and mechanics of the PCMH model.
There is a time commitment to developing the initial checklist, but it can then be modified as needed over future years. Circulate the checklist to staff for their contributions and ideas. Great checklists incorporate hyperlinks to key documents, policies (such as those for no-shows or opiates), procedures, or other resources to augment training. Tackle the orientation checklist in multiple sessions so you don't overwhelm the new physician.
“A sample orientation checklist” is shown below. This checklist is not comprehensive; content may vary widely based on clinic location and what is covered by HR or medical center orientations. If appropriate for your clinic, consider having the trainer sign that they reviewed the information with the new physician. This can be helpful if a dispute arises in the future over whether the physician was informed of something.
A SAMPLE ORIENTATION CHECKLIST
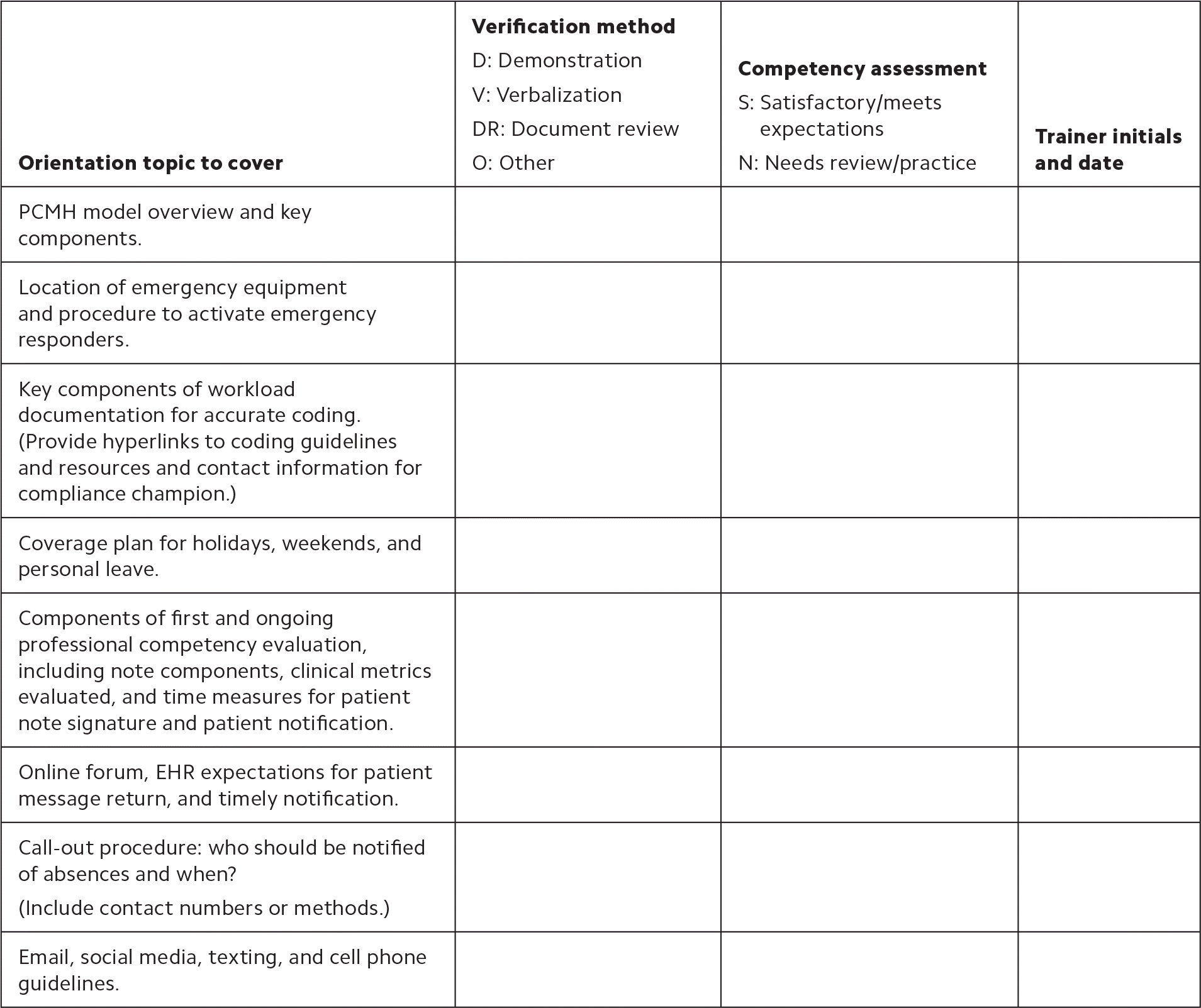
| Orientation topic to cover | Verification method D: Demonstration V: Verbalization DR: Document review O: Other | Competency assessment S: Satisfactory/meets expectations N: Needs review/practice | Trainer initials and date |
|---|---|---|---|
| PCMH model overview and key components. | |||
| Location of emergency equipment and procedure to activate emergency responders. | |||
| Key components of workload documentation for accurate coding. (Provide hyperlinks to coding guidelines and resources and contact information for compliance champion.) | |||
| Coverage plan for holidays, weekends, and personal leave. | |||
| Components of first and ongoing professional competency evaluation, including note components, clinical metrics evaluated, and time measures for patient note signature and patient notification. | |||
| Online forum, EHR expectations for patient message return, and timely notification. | |||
| Call-out procedure: who should be notified of absences and when? (Include contact numbers or methods.) | |||
| Email, social media, texting, and cell phone guidelines. |
5. CREATE AN ORIENTATION SCHEDULE.
Having a schedule will help keep the orientation process on track. Communicate the schedule to the new physician and to all appropriate staff. Numerous delays or unanticipated events can occur during the first few days to weeks of onboarding a new physician, so the schedule should be flexible and allow sufficient time for questions to be answered.
The orientation schedule should include all of the elements previously discussed — work-station assignment, a tour of the practice, distribution of supplies, and emergency preparedness, as well as all items from the orientation checklist. Here are some additional items to include on the schedule:
- Shadowing clinical peers (volunteers can be solicited ahead of time) to help the new physician learn the daily workflow and how to interact with the EHR. This is especially important if the new physician will be using an unfamiliar EHR.
- Meeting with nurses or office staff the new physician will work with daily to discuss work styles, communication preferences, expectations of team members, and the supervisory structure.
- Meeting with any extended team members such as the social worker, nutritionist, psychologist, or other staff who frequently provide care for the patient population.
- Completing required training such as basic life support or computer training.
6. DEVELOP A REASONABLE RAMP-UP PLAN.
You should discuss performance expectations early on, but don't expect the new physician to meet performance goals right away. Instead, allow for a gradual increase in performance. For example, discuss how many patients the physician will be expected to see per day by specific future dates. Having reasonable numbers will keep the physician from feeling discouraged. If possible, consider whether new physicians in the outpatient setting can start with walk-ins or urgent patients instead of inheriting a large patient panel on the first day.
Regular check-ins with a supervisor (weekly to biweekly) for the first six months can help resolve and address issues as they arise. The new physician should also know when the first formal performance evaluation will occur and what the components are.
POST-ORIENTATION STEPS
After orientation is complete, ask the new physician for feedback so you can adjust activities and learning opportunities for the next time. You can always alter the plan based on a physician's familiarity with the practice site, EHR knowledge, prior work roles, and time since formal training.
It's also important to conduct an annual review of the orientation process so you can incorporate changes in the practice's policies and procedures. For example, if the practice has adopted a new protocol for diabetic foot exams or a new screening tool for social determinants of health, having a mechanism to catalog these changes so you can share them with future hires is important. One way to do this is to save updates to a shared electronic folder. If a staff member is interested in taking on a quality improvement project or more responsibility, revamping the orientation process and related documents can be a great starting point.
A well-executed orientation process provides new physicians with the information they need to be successful, which is good for your practice, your patients, and the new physician. It can also help to establish your practice as an employer of choice for health care professionals.

