Providing options for remote access to care can keep your practice running and your patients healthy when an infectious disease outbreak prevents you from seeing them in person.
Published online ahead of the May/June 2020 issue on March 30, 2020.
Editor’s note: On April 30, the Centers for Medicare & Medicaid Services issued further updates to its telehealth policies, making Medicare payments for audio-only telephone E/M visits (CPT codes 99441-99443) equal to payments for similar office/outpatient visits (CPT codes 99212-99214). This article has been updated.

To reduce the risk of exposure during a public health crisis like the COVID-19 pandemic, providing care through virtual visits is a key part of clinic workflow. Remote access to care is important for patients who are symptomatic and may be contagious, as well as those who are scheduled for preventive care and other visits but do not want the risk of exposure.
As part of its interim guidance for COVID-19, the Centers for Disease Control and Prevention (CDC) encouraged health care facilities to explore alternatives to in-person visits by using patient portals, interacting with patients through telephone or telehealth video appointments, and developing an algorithm to identify which patients can be managed by virtual visits.1 (For a virtual visit algorithm, see "A virtual visit algorithm: how to differentiate and code telehealth visits, e-visits, and virtual check-ins.")
There are two main categories of virtual visits:
- Face-to-face video visits, traditionally identified by Medicare as telehealth,
- Non-face-to-face e-visits and other digital communication, or “non-telehealth,” which don't require real-time audio and video interaction. This category includes online evaluation and management (E/M) visits; brief virtual check-ins (by telephone or other telecommunication device); and telephone E/M visits (which payers have traditionally resisted reimbursing but Medicare and others are now allowing during this public health emergency). For physicians who are treating most patients remotely for the first time, it can be difficult to determine what type of services are being provided, and how to bill for them.
This article describes the coding and billing requirements for virtual visits, including recent changes to expand their use, so that physicians can continue to be paid for their services while providing the best patient care during the COVID-19 public health crisis and beyond. (See “Comparison of virtual visits.”)
KEY POINTS
- Recent legislation has decreased telehealth restrictions in response to the COVID-19 pandemic, allowing more clinics to provide telehealth (video) services that are reimbursed at the same rate as in-person services.
- Alternatives to video visits are also available to clinics, including online digital evaluation and management services, virtual check-ins, and remote evaluation services. Some require only a phone.
- Correct diagnosis coding for suspected or confirmed cases of COVID-19 is important for patient management and data collection on the disease burden.
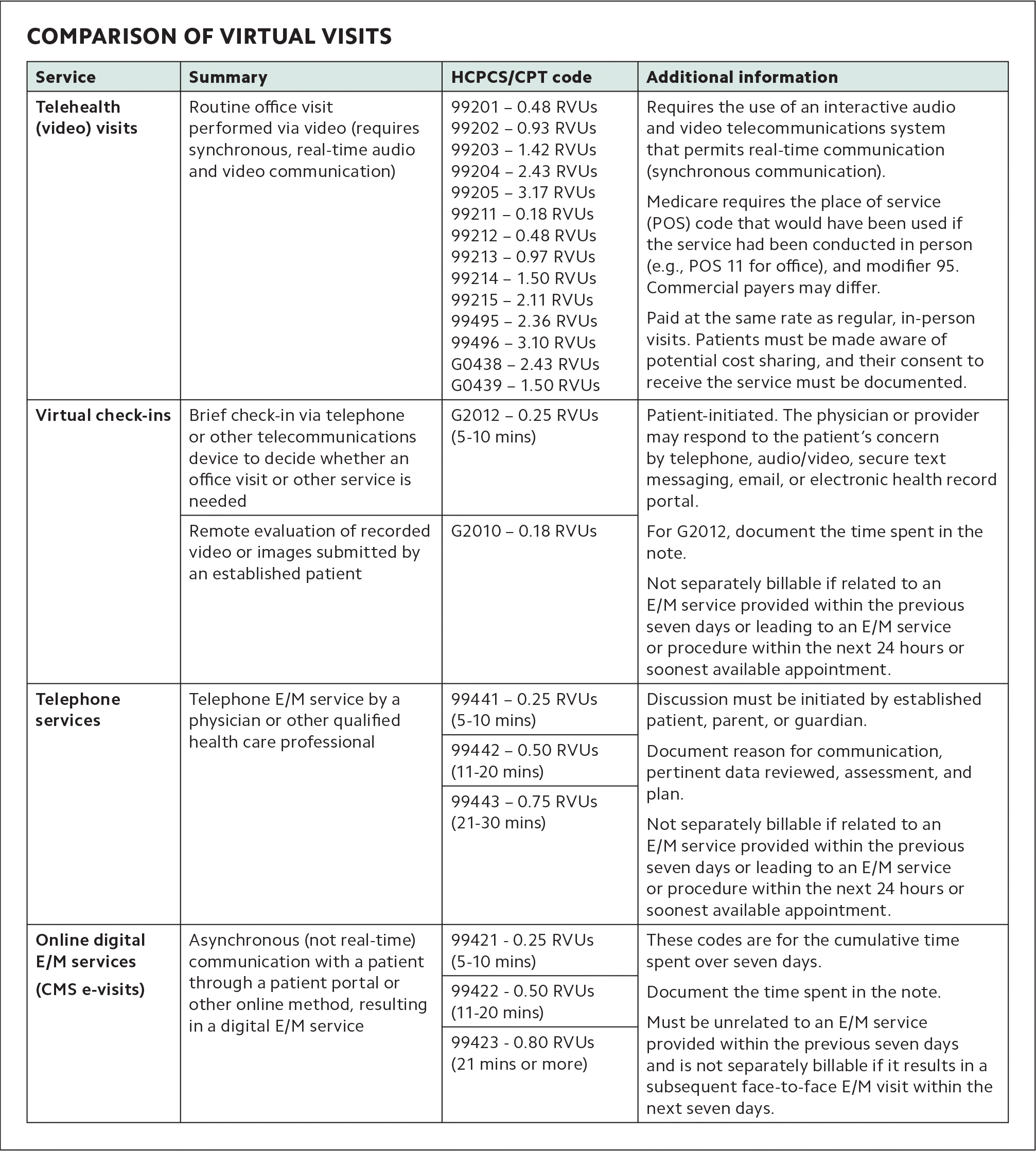
COMPARISON OF VIRTUAL VISITS
| Service | Summary | HCPCS/CPT codes and RVUs | Additional information | ||
|---|---|---|---|---|---|
| Telehealth (video) visits | Routine office visit performed via video (requires synchronous, real-time audio and video communication) | 99201-99205 0.48-3.17 RVUs | Requires the use of an interactive audio and video telecommunications system that permits real-time communication (synchronous communication). Medicare requires the place of service (POS) code that would have been used if the service had been conducted in person (e.g., POS 11 for office), and modifier 95. Commercial payers may differ. Paid at the same rate as regular, in-person visits. Patients must be made aware of potential cost sharing, and their consent to receive the service must be documented. | ||
| 99211-99215 0.18-2.11 RVUs | |||||
| 99495-99496 2.36- 3.10 RVUs | |||||
| G0438-G0439 2.43-1.50 RVUs | |||||
| Virtual check-ins | Brief check-in via telephone or other telecommunications device to decide whether an office visit or other service is needed | G2012 0.25 RVUs (5-10 mins) | Patient-initiated. The physician or provider may respond to the patient's concern by telephone, audio/video, secure text messaging, email, or electronic health record portal. For G2012, document the time spent in the note. Not separately billable if related to an E/M service provided within the previous seven days or leading to an E/M service or procedure within the next 24 hours or soonest available appointment. | ||
| Remote evaluation of recorded video or images submitted by an established patient | G2010 0.18 RVUs | ||||
| Telephone services | Telephone E/M service by a physician or other qualified health care professional | 99441 0.25 RVUs (5-10 mins) | Discussion must be initiated by established patient, parent, or guardian. Document reason for communication, pertinent data reviewed, assessment, and plan. Not separately billable if related to an E/M service provided within the previous seven days or leading to an E/M service or procedure within the next 24 hours or soonest available appointment. | ||
| 99442 0.50 RVUs (11-20 mins) | |||||
| 99443 0.75 RVUs (21-30 mins) | |||||
| Online digital E/M services (CMS e-visits) | Asynchronous (not real-time) communication with a patient through a patient portal or other online method, resulting in a digital E/M service | 99421 0.25 RVUs (5-10 mins) | These codes are for the cumulative time spent over seven days. Document the time spent in the note. Must be unrelated to an E/M service provided within the previous seven days and is not separately billable if it results in a subsequent face-to-face E/M visit within the next seven days. | ||
| 99422 0.50 RVUs (11-20 mins) | |||||
| 99423 0.80 RVUs (21 mins or more) | |||||
TELEHEALTH VISITS
Face-to-face video, or telehealth, visits have historically faced several barriers beyond just the technological challenges inherent in real-time, synchronous audio and video communication. But some of those barriers are now coming down because of COVID-19. For example, until recently, most telehealth visits required that patients go to defined originating sites (which were health care facilities) in designated rural areas. Only patients with end-stage renal disease receiving home dialysis or patients with substance use disorder could receive telehealth services in their home.2 Patients and providers were also restricted in the types of software they could use and had to have an existing relationship before engaging in telehealth. However, these restrictions and others changed with the March 6 passage of The Coronavirus Preparedness and Response Supplemental Appropriations Act.
Under the Act, the U.S. Department of Health and Human Services (HHS) waived certain Medicare telehealth restrictions during the COVID-19 public health emergency, including the originating site requirement.3 As a result, Medicare telehealth services have quickly expanded beyond rural communities, and patients are receiving telehealth services at home. (See “Summary for telehealth video visits.”)4 Some commercial payers have adopted these same guidelines, though physicians should check with their payers to confirm they're on board.
SUMMARY FOR TELEHEALTH VIDEO VISITS
Under the Medicare telehealth expansion for public health emergencies:
- Bill professional claims with modifier 95 for Medicare telehealth visits. This tells the Centers for Medicare & Medicaid Services (CMS) that the service has met the telehealth requirements.
- Some payers may differ from Medicare on telehealth coding. Work with your billing team to determine what modifiers to use for commercial and Medicaid plans.7,8
- The originating site restriction was removed so patients can receive telehealth services in their homes.
- The designated rural area restriction was removed so patients can receive telehealth regardless of location.
- Previously limited to established patients only, telehealth visits are now available to new patients as well.8,9
- Non-public-facing remote communication apps (e.g., Skype or FaceTime) may be used for telehealth services.
- Patient consent to receive telehealth services is required.
- Telehealth visits are paid at the same rate as in-person visits. Patients should be told these visits will be billed the same and out-of-pocket costs may apply. The patient's acknowledgement and consent must be documented.9
- Different visit types are covered under telehealth, including routine office visits and transitional care management. Medicare annual wellness visits and others that require a physical exam may also be covered if patients can self-report their vitals, but there is a lack of clarity from Medicare on this.
- When technical difficulties arise with telehealth visits, on either the patient or physician end, clinics should be prepared with alternative solutions.
The HHS telehealth expansion also relaxes the requirement to use HIPAA-compliant platforms for video visits. Physicians and health care providers will not be subject to penalties for HIPAA violations that occur in the good-faith provision of telehealth during the public health emergency.5 This allows the use of common, non-public-facing remote communication applications (apps) such as Skype, WhatsApp, Google Hangouts, Facebook Messenger, and Apple's FaceTime for telehealth visits. However, use of public-facing remote communication products, such as TikTok, Twitch, Facebook Live, or Slack, remain unacceptable for patient care. State medical privacy laws may still apply to all platforms.
The expectation is that clinicians will perform telehealth visits in private settings, such as their clinics, connecting to patients who are at home or in another clinic setting. However, if telehealth cannot be provided in a private setting, clinicians should implement reasonable HIPAA safeguards, including lowering voices, not using the speakerphone, or moving a reasonable distance from others when personal health information (PHI) is discussed.
Some states are also waiving licensure requirements for physicians to increase access to telehealth across state lines. The Federation of State Medical Boards is compiling a list on its website.
Many types of patient care are covered under telehealth, and telehealth services use the same codes as the corresponding in-person services, such as office visits (CPT codes 99201-99205 and 99211-99215), transitional care management (CPT codes 99495-99496), and some preventive visits.6 Physicians may therefore find telehealth the easiest type of virtual visit to operationalize. For the duration of the public health emergency, Medicare is allowing physicians to select the level of service for telehealth E/M based on medical decision making (as currently defined) or total time spent (defined as all the time associated with the E/M service on the day of the encounter); the current typical times assigned to the E/M codes must be met.
Providing services through telehealth can assist clinics in preventing care gaps during the public health crisis. Keep in mind, though, that the “Welcome to Medicare” physical (G0402) cannot be billed through telehealth and that Medicare annual wellness visits (G0438 and G0439) have a required physical exam component that includes measurement of vitals, such as body mass index and blood pressure. My organization is handling this by getting self-reported vitals from telehealth patients. Your organization will need to outline best practices on how to reliably obtain this information for video visits until Medicare offers clear guidance on this.
Access issues due to technical difficulties are still likely to arise with telehealth visits. Some patients can't access video visit technology because they don't have the necessary device or internet speed. Others may struggle to understand how to use the technology to reach their provider (especially if they need to download a new app). Sometimes the technical difficulties may occur on the physician side. Having a back-up plan to make sure the service can still be delivered, such as rescheduling if there are problems with the connection or converting to an audio-only phone visit if the patient cannot access video, can help prevent frustration. During the public health emergency, Medicare is allowing many types of telehealth services to be provided with audio only.
Telehealth services may require cost-sharing, so patients' consent to this must be documented. Consent may be written or verbal and can be obtained by anyone in the clinic, not just the physician.
BEYOND TELEHEALTH: OTHER VIRTUAL SERVICES
What if your clinic doesn't have the time or resources to provide telehealth video visits? The Centers for Medicare & Medicaid Services (CMS) recently expanded the use of other non-face-to-face virtual visits that historically do not fall under “telehealth.” Virtual check-ins, remote evaluations, and online digital E/M services, or “e-visits,”9 are covered by Medicare and some commercial insurance plans and can help clinics operate effectively in the current environment. (See “Summary for non-telehealth virtual visits.”) Virtual check-ins are brief telephone discussions. Remote evaluations include the review of video or images (not necessarily in real time). Online digital E/M services are performed by exchanging digital messages with patients.
SUMMARY FOR NON-TELEHEALTH VIRTUAL VISITS
Online digital E/M services, or “e-visits” (CPT 99421-99423): Back-and-forth, not real-time (asynchronous) communication. Medicare covers these services and so do some commercial payers. Check with payers in your area.
Virtual check-ins (HCPCS G2012): Synchronous brief communication by phone or other device to determine if in-person care is needed. Medicare covers these services and so do some commercial payers. Check with payers in your area.
Remote evaluation (HCPCS G2010): Evaluation of recorded video or images (store and forward). Medicare covers these services and so do some commercial payers. Check with payers in your area.
Telephone E/M services (CPT 99441-99443): Diagnosis and management of a patient's problem over the phone. Medicare now covers this; check with commercial payers before billing.
Common to all four types of non-telehealth virtual visits:
- Not limited to rural settings; no location restrictions.
- Time-based codes must have time documented in the note.
- Can now be provided to new or established patients during the public health emergency.
- Must be patient-initiated. The patient calls the clinician or sends a message requesting a new appointment, or the patient agrees to change a previously scheduled face-to-face visit to a virtual encounter.
- May result in co-pay or cost-sharing; patient consent must be documented. (Depending on your organization, a general consent can be used and updated annually to cover all of these services. If it's not possible to build these services into a general consent, then consent should be obtained prior to each service rendered.)
- Information that can be stored and shared (for example, text messages, recorded video, or images) must be stored in the patient's electronic health record. Best practice is to include it in the encounter note.
Medicare now covers telephone E/M services, and so do some commercial payers. Physicians should check with their payers to learn their policies. Medicare's temporary coverage was announced March 30 after medical organizations, including the American Academy of Family Physicians, advocated for it during this public health emergency.
Each non-telehealth visit type is examined in detail below and in the "Summary for non-telehealth virtual visits." All require that the patient initiate the service, though clinicians may have to make patients aware of their availability prior to initiation and patients may consent to have previously scheduled office visits converted to virtual visits. These visits have previously been allowed for established patients only. However, CMS has announced that during the public health emergency virtual check-ins and telephone E/M services can be provided to both new and established patients.
Online digital E/M services (e-visits). On Jan. 1, 2020, new codes were added to CPT to allow billing for online E/M services. These are patient-initiated online services provided through sharing digital messages with physicians or other qualified health care professionals (QHPs) who are able to bill Medicare independently. CMS refers to these as e-visits and only allows them on HIPAA-compliant platforms, such as an electronic health record (EHR) portal or secure email.
Billing for online digital E/M services requires a physician or other QHP's evaluation, assessment, and management of the patient.10 Merely responding to portal or secure email messages does not qualify. There must be an E/M service provided through the online communication, including a clinical decision that would otherwise typically be provided in the office.
The codes for these services are time-based. Report the total time spent on each patient over a seven-day period, regardless of whether the communication is for the same problem or multiple different problems. The seven-day period begins with the physician or other QHP's initial, personal review of the patient inquiry. The time spent should be documented in the note. The documented time would include things like reviewing the patient's inquiry, the patient's record, and data relevant to the assessment; interacting with clinical staff about the patient's problem; developing management plans; and ordering tests and prescriptions. Any subsequent communication with the patient (via online portal, email, other digitally supported methods, or phone) can also be included.
Do not include the non-evaluative electronic communication of test results, scheduling of appointments, or other communication that does not include E/M as part of the cumulative time. Do not include clinical staff time.
Online digital E/M services may be billed by a physician or QHP in any specialty. But if the patient's inquiry is related to a surgical procedure and occurs during the post-operative period (global period), do not report an online E/M visit. Also, do not report online digital E/M services on the same day as the following codes: 99201-99205 (new patient office visit), 99212-99215 (established patient office visit), and 99241-99245 (office consultation visit).
The online digital E/M service must be unrelated to any in-person E/M service provided within the previous seven days, and the online E/M service is not separately billable if it results in a subsequent in-person E/M visit within the next seven days.
Here is a sample workflow for documenting online digital E/M services:
- Go to the patient chart and open a type of note that is different than an office visit (for example, case management or telemedicine) so it is clear that a non-face-to-face service was provided.
- Copy and paste digital messages into the note (this will show patient initiation).
- Document information pertinent to the E/M services provided, making sure to include assessment and plan based on communication with the patient.
- Document the total time spent within the seven-day requirement.
- Make sure to associate the appropriate diagnosis code with the service and bill for it after the seven days are up.
Virtual check-ins and remote evaluation. “Virtual check-ins” are brief technology-based services, like phone calls or texts, for patients to communicate with their providers remotely. They may include remote evaluation of images and recorded videos sent by patients. These services cannot be billed separately if they originate from a related in-person E/M service provided within the previous seven days or lead to an in-person E/M service or procedure within the next 24 hours or soonest available appointment. Less than five minutes is not billable. Work with your billing department to determine the proper place of service code. Images and videos must be added to the patient's medical records or encounter note in order to bill for remote evaluation.
Telephone E/M services. These are time-based, non-face-to-face E/M services provided to a patient, parent, or guardian using the phone. Medicare is allowing these services for both new and established patients during the public health emergency. CMS also announced that during the emergency it would make Medicare payments for telephone E/M codes (CPT 99441-99443) equal to office/outpatient visits with established patients on claims retroactive to March 1 (the new payment rates range from $46-$110).
Telephone E/M can be provided by a physician or other QHP who may report E/M services. The difference between telephone E/M services and virtual check-ins is that virtual check-ins are used to evaluate whether an office visit or other service is warranted, while telephone E/M services include the diagnosis and management of a problem over the phone and require medical necessity to be billable.
As with virtual check-ins and remote evaluation, telephone E/M cannot be billed separately if it originates from a related in-person E/M service provided within the previous seven days or leads to an in-person E/M service or procedure within the next 24 hours or soonest available appointment. Create a note to outline the reason for the communication and the outcome (telephone E/M services require an assessment and plan).
DIAGNOSIS CODES FOR COVID-19 ENCOUNTERS
Diagnosis codes are just as important for virtual visits as they are for routine office visits. Accurate diagnosis documentation is not only important to establish medical necessity for services, but also for data collection to understand the disease burden (both financial and medical) and the epidemiologic impact. If the patient is suspected to have COVID-19 or does have COVID-19, use the following guidance for diagnosis coding.
The World Health Organization (WHO) added a new ICD-10 emergency code, U07.1, for COVID-19, and the CDC recently announced an unprecedented, off-cycle update to the U.S. ICD-10 code set, adding U07.1 effective April 1, 2020 (codes are usually added only on Oct. 1 each year).11
Codes for respiratory conditions caused by COVID-19 should be used in conjunction with U07.1. There are also codes for exposure to COVID-19 and suspected exposure ruled out after examination. (See “ICD-10 coding for COVID-19 and potential complications.”)
For patients presenting with symptoms such as fever or dry cough where a definitive diagnosis has not been established, assign the appropriate code for each of the presenting signs and symptoms. Diagnosis code B34.2, “Coronavirus infection, unspecified,” generally would not be appropriate for documenting COVID-19 because the cases have universally been respiratory in nature, so the site would not be “unspecified.”
ICD-10 CODING FOR COVID-19 AND POTENTIAL COMPLICATIONS

| Condition | ICD-10 code |
|---|---|
| COVID-19 (effective April 1) | U07.1, “COVID-19” |
| COVID-19 exposure | Z20.828, “Contact with and (suspected) exposure to other viral communicable diseases” |
| COVID-19 exposure ruled out | Z03.818, “Encounter for observation for suspected exposure to other biological agents ruled out” |
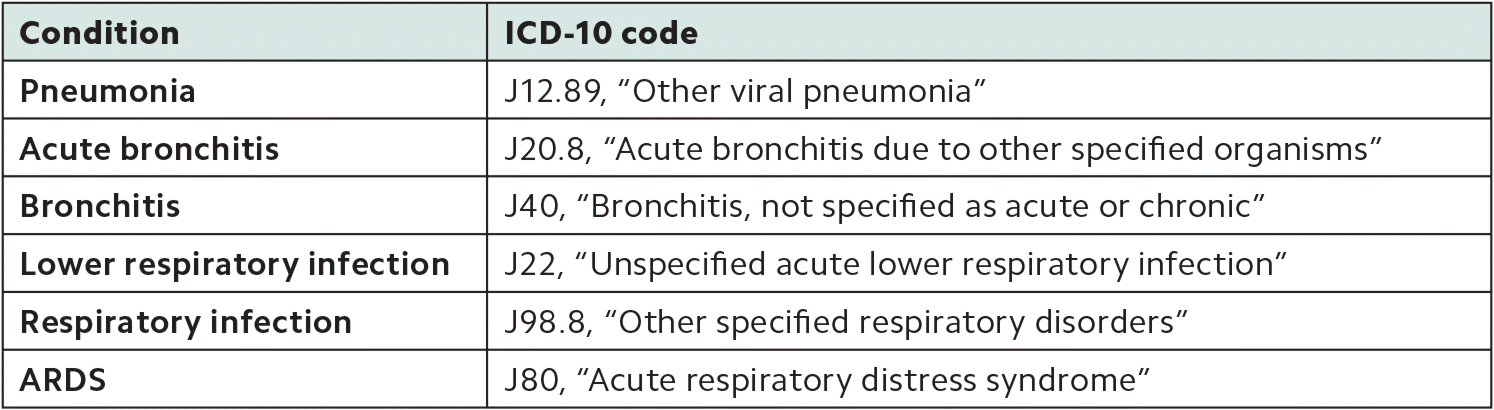
Common respiratory complications
Coded in combination with U07.1 when caused by COVID-19.
| Condition | ICD-10 code |
|---|---|
| Pneumonia | J12.89, “Other viral pneumonia” |
| Acute bronchitis | J20.8, “Acute bronchitis due to other specified organisms” |
| Bronchitis | J40, “Bronchitis, not specified as acute or chronic” |
| Lower respiratory infection | J22, “Unspecified acute lower respiratory infection” |
| Respiratory infection | J98.8, “Other specified respiratory disorders” |
| ARDS | J80, “Acute respiratory distress syndrome” |
FINAL THOUGHTS
Virtual visits are a good way not only to triage sick patients who may expose other patients and clinic staff but also to continue caring for well patients who may be apprehensive about coming to your clinic during the COVID-19 pandemic.
Work with your billing staff to understand commercial insurance coverages and your local Medicare Administrative Contractor (MAC) guidelines for virtual services so you can avoid claims denials, and be sure your practice has a process in place for appealing any denials you do receive. Look for more information from AAFP and other trusted organizations if questions arise. (See “Resources.”)
Public health emergencies will alter the way your clinic operates — be flexible and be prepared.
RESOURCES
- A Toolkit for Building and Growing a Sustainable Telehealth Program in Your Practice. American Academy of Family Physicians.
- AMA Quick Guide to Telemedicine in Practice. American Medical Association.
- Medicare Telemedicine Health Care Provider Fact Sheet. Centers for Medicare & Medicaid Services.

