The biggest changes in evaluation and management coding since 1997 will take effect Jan. 1, 2021. It is time to prepare for them now.
Editor's note: In its 2021 Medicare Physician Fee Schedule, CMS released new guidance regarding coding for prolonged E/M services. This article has been updated accordingly.

Say goodbye to counting exam bullet points and making sure you have correctly separated your history of present illness from your review of systems: Changes are coming that should streamline your coding and help you zip through your documentation faster.
The shift in required documentation for CPT codes 99202-99215 takes effect Jan. 1, 2021. Coding for office visits will be based solely on medical decision making (MDM) or total time, and the history and exam components will no longer be used.1 It's the biggest change in evaluation and management (E/M) office coding since 1997.
The reforms will apply only to regular office visits (levels 2–5 for new and established patients) — not other visit types (e.g., nursing home or hospital visits) — and should help simplify many aspects of coding. They will allow family physicians to produce shorter, more readable notes that will enhance patient care and save time. They will also lead to more accurate coding and allow us to be reimbursed more fairly for the work we do.
This article outlines what you need to know about the new rules, and it includes some templates to help you prepare your mind and your EHR.
KEY POINTS
- The biggest changes in evaluation and management coding in more than two decades take effect Jan. 1, 2021. They will allow physicians to code office visits based only on total time or medical decision making.
- The medical decision making coding method relies on three categories: problems (the severity of the conditions for which you're seeing the patient), data (what you had to review for the visit), and risk (the patient's morbidity or mortality odds).
- You can start creating coding tables and templates now, so your EHR will be optimized for faster documentation once the new rules go into effect.
OPTION 1: TOTAL TIME
Total time will be measured as the time the physician or other qualified health professional spent on that patient on the day of the encounter. It will include time spent before, during, and after the visit, including time spent documenting the visit. Yes, that means after Jan. 1, “pajama time” (the time you spend finishing your charts after your kids are asleep) can be reimbursed. But get your charts done before midnight, because time spent the following day cannot be counted.
Hospital coding can already use time spent on the patients' unit/floor before and after the visit to determine the level of service, while office coding currently counts only face-to-face time. Allowing coding by total time will correct this double standard.
On the day of the patient encounter, total time will include time spent before the visit reviewing the patient's medical record (e.g., recent visits, labs, and studies); seeing the patient in the office (face-to-face time); discussing the patient's care with other health professionals or family members; ordering medications, studies, procedures, or referrals; calling the patient or family later in the day with results and further recommendations; and documenting the visit in the medical record. Total time will not include time spent by your nurse or other clinical staff caring for the patient and will not include time you spend performing a procedure during the same office visit (the assumption is that you will bill that procedure separately, in addition to the office visit).
While it's not required under the new rules, you may want to develop a table for documentation that shows the actual minutes spent in each category of total time (before, during, and after the visit). This will provide backup verification in case of an audit that challenges coding levels.
In another welcome change, total time thresholds will be clearly spelled out under the new regimen (e.g., 30–39 minutes total time for a level 4 established patient visit). Currently, time thresholds are listed without ranges (e.g., 25 minutes face-to-face for a level 4 visit). As a result, some clinicians, coders, and insurance companies have interpreted the times listed to be minimum requirements, while others have interpreted them to be averages. The new, more specific time thresholds should decrease confusion, improve coding accuracy, and decrease insurance company denials.
An easy way to remember the new time thresholds is the “30-, 40-, 55-Minute Rule.” For established patients, total time between 30 and 39 minutes is a level 4 visit, between 40 and 54 minutes is a level 5, and prolonged services start at 55 minutes of total time, per CPT. (Note that the prolonged services code and rules differ for Medicare; see below.) Total time requirements for each visit level will remain longer for new patients than for established patients under the new rules.
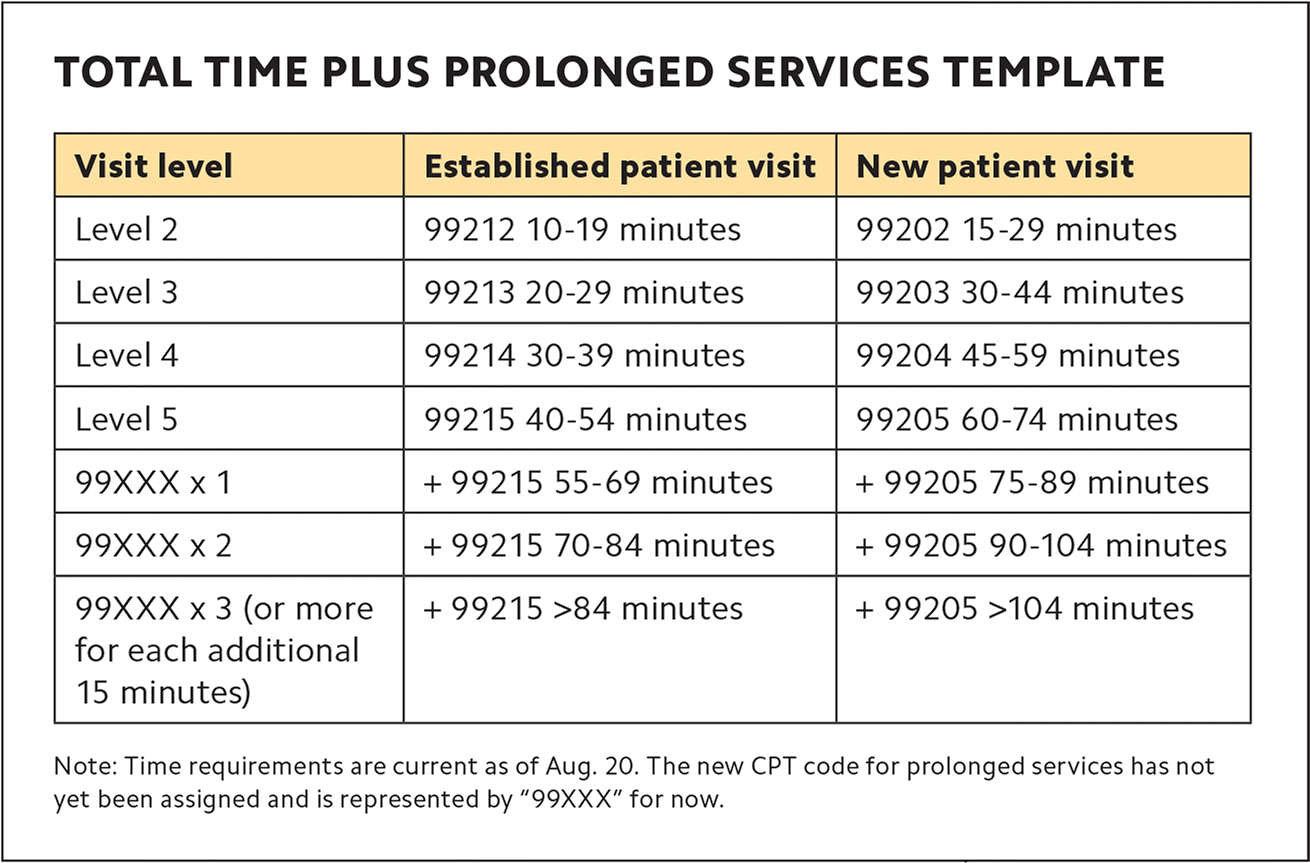
Currently, when extra time is spent caring for complex or very sick patients, prolonged service codes (99354 and 99355 for office or other outpatient visits and 99356 and 99357 for inpatient visits) are often not billed because of confusion about the requirements. When they are billed, they're often incorrectly denied by insurance companies. After Jan. 1, coding for prolonged services will also be greatly simplified, leading to more of your long and complex visits being properly reimbursed. The current prolonged service codes will become a single new code that can be billed in 15-minute increments when total time exceeds a level 5 visit. (See “Total time plus prolonged services template.”) When coding for prolonged services, make sure you don't forget to submit the level 5 code (99215 or 99205) in addition to the prolonged services code (99417).
When using total time to code visits, remember to document it at the end of the note (i.e., “My total time spent caring for the patient on the day of the encounter was XX minutes”).
TOTAL TIME PLUS PROLONGED SERVICES TEMPLATE
| Visit level | Established patient office visit | New patient office visit |
|---|---|---|
| Level 2 | 99212 10-19 minutes | 99202 15-29 minutes |
| Level 3 | 99213 20-29 minutes | 99203 30-44 minutes |
| Level 4 | 99214 30-39 minutes | 99204 45-59 minutes |
| Level 5 | 99215 40-54 minutes | 99205 60-74 minutes |
| 99417 x 1 | + 99215 55-69 minutes | + 99205 75-89 minutes |
| 99417 x 2 | + 99215 70-84 minutes | + 99205 90-104 minutes |
| 99417 x 3 (or more for each additional 15 minutes) | + 99215 >84 minutes | + 99205 >104 minutes |
| For Medicare patients | ||
| G2212 x 1 | + 99215 69-83 minutes | + 99205 89-103 minutes |
| G2212 x 2 | + 99215 84-98 minutes | + 99205 104-118 minutes |
| G2212 x 3 (or more for each additional 15 minutes) | + 99215 >98 minutes | + 99205 > 118 minutes |
Update: The CPT prolonged services code is 99417.
These thresholds are based on CPT guidelines. Some payers may differ. In the 2021 Medicare Physician Fee Schedule, CMS introduced prolonged services code G2212. In order to bill this code, clinicians must have exceeded the maximum time for a level 5 visit by 15 minutes or more (i.e., 69 minutes for an established patient and 89 minutes for a new patient) rather than the minimum as required by CPT for code 99417.
OPTION 2: MEDICAL DECISION MAKING
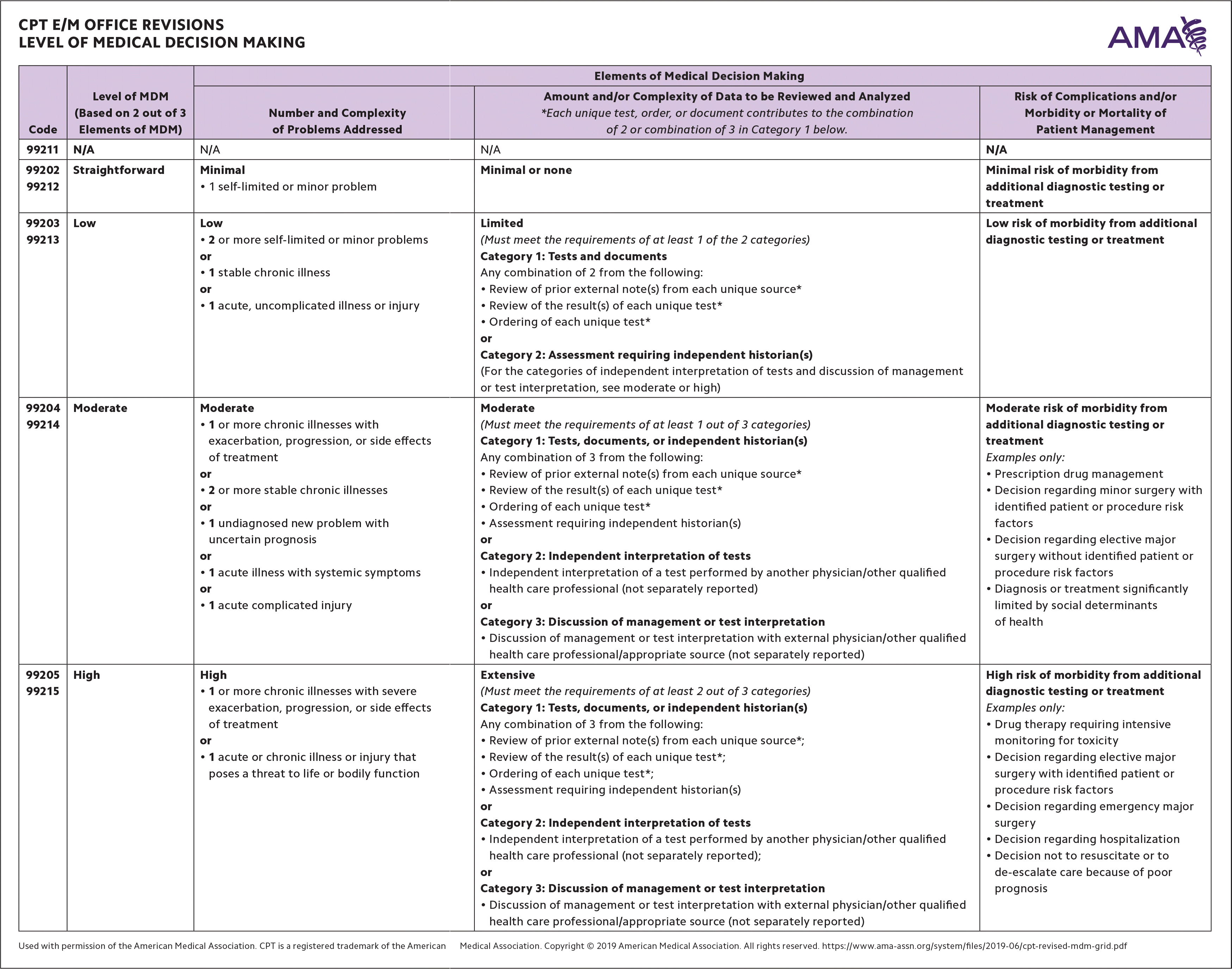
To understand the new MDM requirements, let's look closely at the new American Medical Association (AMA) MDM chart approved by the Centers for Medicare & Medicaid Services. (See “CPT E/M office revisions level of medical decision making.”) It shows that MDM is made up of three elements: problems, data, and risk. The level of service is based on the highest level met by at least two of the three elements, whether the patient is new or established. New patient codes are assigned higher values to recognize the work of establishing care.
Problems. These are the patient problems you are evaluating during the office visit. This element does not include other problems the patient may have that you are not addressing during the encounter, or problems managed solely by another provider.
Each visit will be designated as “minimal,” “low,” “moderate,” or “high” in this category, depending on how many problems are addressed, whether they are chronic or acute, and how stable the chronic problems are. Stable chronic illnesses could include hypertension, diabetes mellitus, or benign prostatic hyperplasia. But for coding purposes, patients with poorly controlled hypertension whose blood pressure is not at goal, or patients with diabetes whose A1C is not at goal, are considered to have chronic illnesses that are not stable.
Data. This category includes each unique test, order, or document that you had to review for the visit. Each visit will be designated as “minimal or none,” “limited,” “moderate,” or “extensive” in this category, depending on the amount of data reviewed, the complexity of the data, and where it came from.
Note a few important definitions for this category:
- An “external” physician or qualified health professional is a provider from a different specialty or a totally different group practice.
- An “external” note includes records, notes, and tests from external providers.
- A single “unique test” for coding purposes includes panels (e.g., a basic metabolic panel is considered a single unique test).
- “Independent interpretation of tests” includes looking at or interpreting a chest X-ray (CXR) or electrocardiogram (ECG) tracing (i.e., “I ordered and personally reviewed the CXR and it shows …”). You are not credited with interpretation in this category if you are also billing for your interpretation separately.
Risk. This is the patient's risk of complications, morbidity, or mortality. This category will be designated as “minimal,” “low,” “moderate,” or “high,” depending on whether the patient's problems call for discussions about things like prescription drug management, surgery, or hospitalization.
CPT E/M OFFICE REVISIONS LEVEL OF MEDICAL DECISION MAKING
| Code | Level of MDM (Based on 2 out of 3 Elements of MDM) | Elements of Medical Decision Making | ||
|---|---|---|---|---|
| Number and Complexity of Problems Addressed | Amount and/or Complexity of Data to be Reviewed and Analyzed *Each unique test, order, or document contributes to the combination of 2 or combination of 3 in Category 1 below. | Risk of Complications and/or Morbidity or Mortality of Patient Management | ||
| 99211 | N/A | N/A | N/A | N/A |
| 99202 99212 | Straightforward | Minimal
| Minimal or none | Minimal risk of morbidity from additional diagnostic testing or treatment |
| 99203 99213 | Low | Low
| Limited (Must meet the requirements of at least 1 of the 2 categories) Category 1: Tests and documents Any combination of 2 from the following:
or Category 2: Assessment requiring independent historian(s) (For the categories of independent interpretation of tests and discussion of management or test interpretation, see moderate or high) | Low risk of morbidity from additional diagnostic testing or treatment |
| 99204 99214 | Moderate | Moderate
| Moderate (Must meet the requirements of at least 1 out of 3 categories) Category 1: Tests, documents, or independent historian(s) Any combination of 3 from the following:
or Category 2: Independent interpretation of tests
Category 3: Discussion of management or test interpretation
| Moderate risk of morbidity from additional diagnostic testing or treatment Examples only:
|
| 99205 99215 | High | High
| Extensive (Must meet the requirements of at least 2 out of 3 categories) Category 1: Tests, documents, or independent historian(s) Any combination of 3 from the following:
or Category 2: Independent interpretation of tests
or Category 3: Discussion of management or test interpretation
| High risk of morbidity from additional diagnostic testing or treatment Examples only:
|
Used with permission of the American Medical Association. CPT is a registered trademark of the American Medical Association. Copyright © 2019 American Medical Association. All rights reserved. https://www.ama-assn.org/system/files/2019-06/cpt-revised-mdm-grid.pdf
SOME EXAMPLES
Here are some examples of what the documentation for various levels of visits might look like under the new rules.
Level 2 office visit. This is a visit for a simple problem such as a viral upper respiratory infection or a simple recheck of a stable problem, during which you neither prescribe a new medication nor adjust an existing prescription. Or this could be a visit in which your total time is 10–19 minutes (for an established patient).
Example:
Subjective: 58 yo male returns for a recheck of R arm cellulitis. Doing well. Redness gone. No fever. Finished cephalexin yesterday.
Objective: T 98.2, R 84, BP 130/70. R arm: cellulitis is gone, no erythema, no axillary adenopathy.
Assessment/plan: Cellulitis of right upper extremity L03.113: Cellulitis is resolved. Discussed skin infections. RTC prn.
Total time spent caring for the patient on the day of the encounter was 15 minutes.
Level 3 office visit. This could be a visit in which a patient comes in with a problem and you prescribe a medication. Or it could be a visit in which your total time is 20–29 minutes.
Example:
Subjective: 43 yo female presents with a 10 d hx of frontal maxillary sinus pain, drainage, and fatigue. No fever, ST, ear pain, or cough.
Objective: T 99.2, R 16, P 72, BP 135/84. NAD. Frontal sinus tender w/ palpation, TMs nl, pharynx nl, no cervical adenopathy, CV RRR, lungs CTA.
Assessment/plan: Acute non-recurrent frontal sinusitis J01.10: Discussed sinus infections, fluids, amoxicillin 500mg TID x 7 days, RTC or call if symptoms persist or worsen.
Total time spent caring for the patient on the day of the encounter was 25 minutes.
Level 4 office visit. This could be a visit in which you address a patient's moderately complex problem, and you prescribe a medication or order and interpret/review an X-ray, an ECG, or three separate lab tests (or panels). Or this could be a visit in which your total time is 30-39 minutes.
Example:
Subjective: 68 yo male presents for recheck of DM, HTN, hyperlipidemia. He is exercising and watching his diet and weight. Vision is stable. BP is good. FBS avg 180.
Current medications: Atorvastatin 40 mg 1 po q h, Losartan 100 mg 1 po q am, Metformin 500 mg po bid.
Objective: P 64, R 18, BP 120/70, 162 lbs. Fundii benign, PERRLA, TMs nl, throat nl, neck no adenopathy, heart S1 S2 s murmur regular, lungs clear. Extr no edema or lesions, pulses intact, can feel 3/3 touches w LEEP filament.
Labs:
A1C 4/20 7.1, 8/20 8.2, Creatinine 8/20 0.9, LDL chole 8/20 55.
Assessment/plan:
- Dyslipidemia E78.5: LDL within goal, continue atorvastatin.
- Essential hypertension I10: BP is well controlled, continue losartan.
- Type II diabetes without complication, without long-term use of insulin E11.9: A1C not to goal, metformin increased to 1000 mg bid. RTC 4 months with fasting lab.
Total time spent caring for the patient on the day of the encounter was 35 minutes.
Level 5 visit. This could be a visit in which you see a very acutely sick patient who requires admission to the hospital (assuming you are not admitting the patient yourself, because then you would bill for the admission only). Another example of a level 5 office visit is caring for a very sick patient with high-complexity problems, for which you order and interpret an X-ray or ECG, plus order and review three lab tests or panels. Or this could be a visit in which your total time is 40–54 minutes.
Example (using total time):
Subjective: 22 yo male presents with a 2 wk hx of depressed mood, crying spells, poor appetite assoc w/ 10 lb wt loss, problems getting and staying asleep, poor concentration, anxiety, and loss of pleasure (no longer fishing). He denies irritability or suicidal ideation. Nonsmoker, nondrinker. No access to guns. Denies prior hx of depression or fm hx of depression/mental illness. Job is going well, no financial concerns, no family concerns, and no addiction concerns. Symptoms started after his girlfriend broke up with him.
Objective: P 92, R 18, BP 138/88, 195 lbs. Alert, cooperative, good eye contact but appears slightly tearful/sad. Normal reasoning. Good insight.
Current medications: none
Assessment/plan: Current moderate episode of major depressive without prior episode F32.1. Discussed depression at length (depression handout given and discussed). Start to walk/exercise. Download and use recommended depression phone apps. Begin sertraline 50 mg 1 po q am. Risks and benefits of medication discussed. Recheck 2 wks. Call, email, text, or RTC sooner if symptoms should worsen or suicidal ideation should develop.
Total time spent caring for the patient on the day of the encounter was 45 minutes.
TEMPLATES AND FURTHER SIMPLIFICATIONS
Is it possible to make the new coding changes even more doctor-friendly and still come up with the correct code most of the time? I believe so. I looked closely at the new regulations and compiled three new templates.
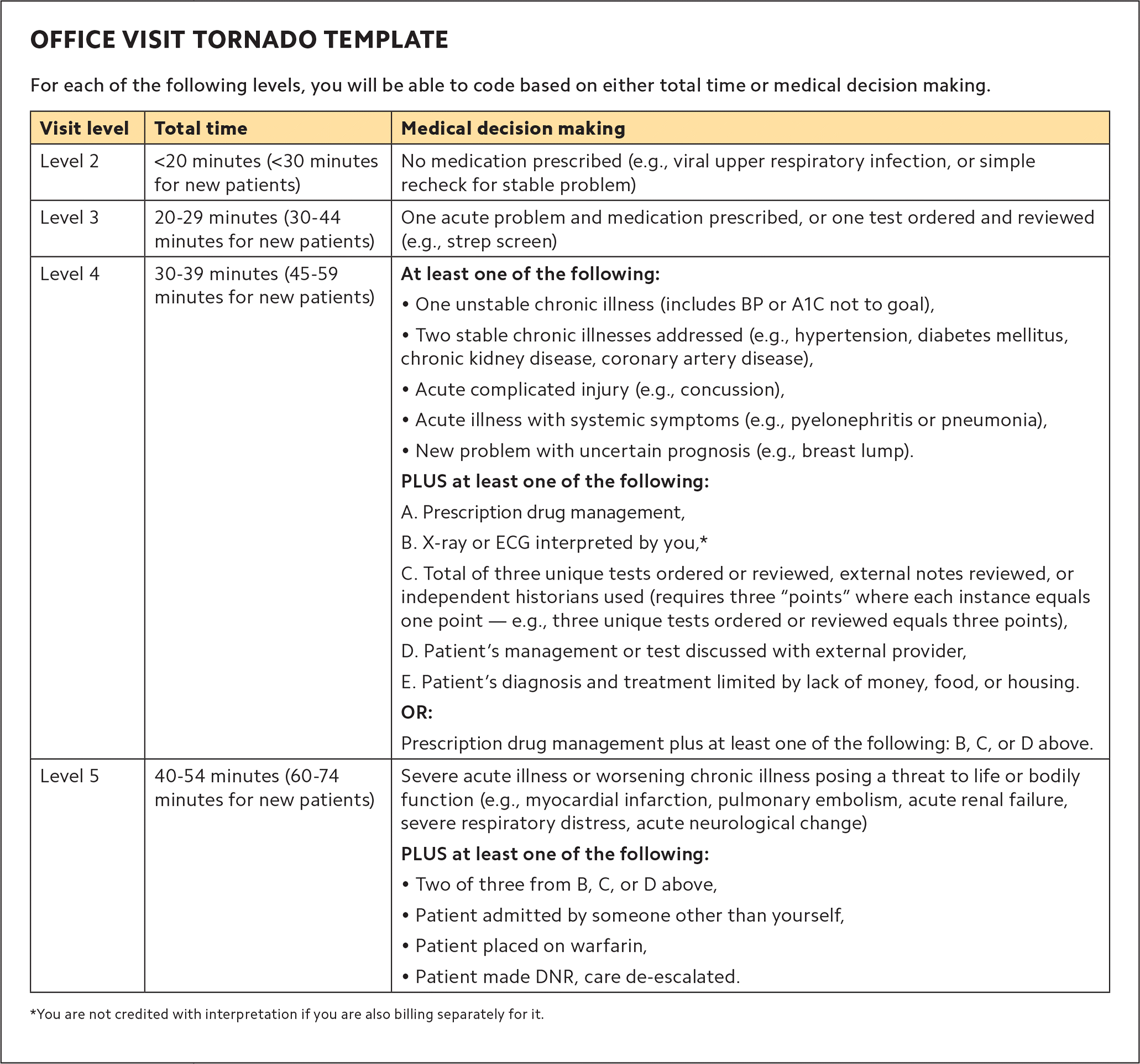
The first is the “Office visit tornado template,” which combines MDM with total time in a way that allows you to quickly determine the level of the visit, and therefore the code. I call it the “tornado template,” because I hope it proves to be a concise and powerful tool to cut through the confusion of coding office visits. The template provides total time thresholds for both new and established patients, combines MDM data with risk, and adds examples of problems (diagnoses) and other helpful information.
I've also created a template for coding pre-operative visits. (See “Coding pre-ops template.”)
OFFICE VISIT TORNADO TEMPLATE
| Visit level | Total time | Medical decision making |
|---|---|---|
| Level 2 | <20 minutes (<30 minutes for new patients) | No medication prescribed (e.g., viral upper respiratory infection, or simple recheck for stable problem) |
| Level 3 | 20–29 minutes (30–44 minutes for new patients) | One acute problem and medication prescribed, or one test ordered and reviewed (e.g., strep screen) |
| Level 4 | 30–39 minutes (45–59 minutes for new patients) | At least one of the following:
OR: Prescription drug management plus at least one of the following: B, C, or D above. |
| Level 5 | 40–54 minutes (60–74 minutes for new patients) | Severe acute illness or worsening chronic illness posing a threat to life or bodily function (e.g., myocardial infarction, pulmonary embolism, acute renal failure, severe respiratory distress, acute neurological change) PLUS at least one of the following:
|
*You are not credited with interpretation if you are also billing separately for it.
CODING PRE-OPS TEMPLATE

| Visit level | Type of operation |
|---|---|
| Level 3 | Minor surgery (e.g., pressure equalizer tube insertion, cataract repair) without risk factors. |
| Level 4 | Minor surgery with risk factors* or major surgery with or without risk factors, Plus: Evaluating/reviewing the status of one unstable or two stable chronic illnesses OR ordering/reviewing three lab tests OR interpreting a CXR or ECG.† |
| Level 5 | Major surgery with risk factors, plus ordering/reviewing three tests, AND ordering and interpreting a CXR or ECG.† |
*Risk factors include hypertension, chronic kidney disease, diabetes mellitus, etc. Include risk factors in your opening statement: Mrs. Jones is seen today for preoperative consultation requested by Dr. Smith for patient’s R TKA scheduled on 4/8/21 at Mercy Hospital because of her diabetes and hypertension.
† You are not credited with interpretation if you are also billing separately for it.
As you become more familiar with the new rules, you may want to create your own documentation templates. There are other things you can do to ease your documentation burden as well. Consider combining the patient's chief complaint (CC), history of present illness (HPI), and pertinent review of systems (ROS). It should be clear in your first or second sentence what problems you are addressing at that visit (e.g., “the patient presents for a physical,” “the patient presents for evaluation of his DM, HTN, and CKD,” or “the patient presents with a new onset rash and follow-up for worsening depression”). When auditing a chart, I find it frustrating to review a long narrative that doesn't make it immediately clear what problems are being addressed at that patient encounter.
The problems addressed in the CC/HPI/pertinent ROS section should also mirror the problems in your assessment and plan.
To further shorten and improve your documentation, consider combining your assessment with your plan.
Example:
- Essential hypertension I10: BP is well controlled, continue losartan,
- Dyslipidemia E78.5: LDL within goal, continue rosuvastatin,
- Type II diabetes mellitus with hyper-glycemia, E11.65: A1C not to goal, metformin increased to 1000 mg bid. RTC 3 months with fasting lab.
With the new coding changes, most of us will choose to leave out non-pertinent past medical, family, and social histories from our documentation. But I would recommend including current medications in your level 4 and 5 documentation. It is often helpful from a clinical management standpoint to know what medications the patient was on at that past visit.
In the future, perhaps the AMA will consider including more specific clinical examples for level 2 (minimal), level 3 (low), and level 4 (moderate) problems. For instance, are new-onset migraine, new-onset hypertension, pelvic inflammatory disease, sexually transmitted infections, influenza, respiratory syncytial virus bronchiolitis, and mononucleosis all considered level 4 problems? A list of several clinical examples of what constitutes minor and major surgery from a pre-op coding perspective would also be helpful.
But for now these changes provide long-awaited relief for some of our documentation frustrations. They are a game-changer, and will be a big plus for primary care.
E/M CODING REFORMS SERIES
This is the first in a series of articles about the changes to E/M coding and documentation requirements coming in 2021.
Upcoming articles:
November/December 2020 — Test your knowledge of specific coding scenarios.
January/February 2021 — Coding level 4 visits.
Editor’s Note
For more information on the coding and documentation changes, including the AAFP's new E/M reference card, visit aafp.org/emcoding.

