
When done well, precepting is a win-win-win for physicians, medical students, and patients.
Fam Pract Manag. 2021;28(5):5A-5C
Author disclosures: no relevant financial affiliations.
Have you ever caught yourself saying “When I was a medical student …” and then describing a formative experience you had during those years? Perhaps you helped a medical practice by writing orders, performing procedures, changing dressings, following up on labs or other studies, writing notes, or discussing patient care with consultants. In other words, you helped take care of “your” patients. Those experiences likely molded you into the physician you are today.
Over the past few decades, a variety of factors — including regulatory constraints and documentation burdens — limited students' opportunities to meaningfully contribute to clinical care and pushed students to peripheral roles.1 But recent regulatory changes, better preclerkship training, and a broadening educational focus that includes population health are creating new opportunities for students to again be meaningful members of care teams. This can result in better patient care and enhanced learning for students: a win-win-win for the patient, learner, and preceptor.
SEVEN WAYS TO INVOLVE STUDENTS IN YOUR PRACTICE
Many physicians think they're too busy for precepting, but here are seven ways to make it a worthwhile experience for all involved.
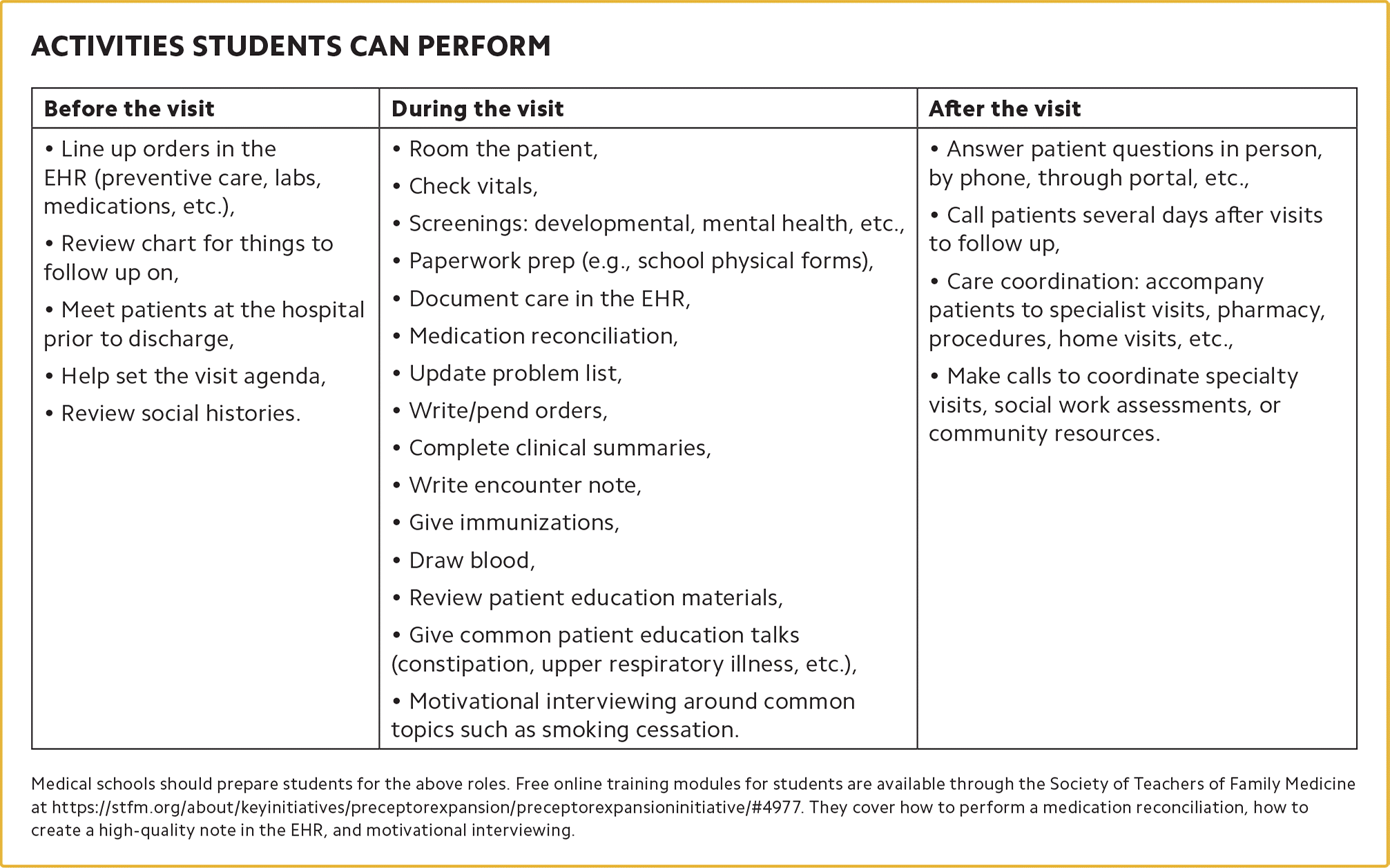
1. Look for opportunities for students to care for patients, clinically or otherwise. Avoid assigning “scutwork” or “nonclinical yet essential tasks that don't require a doctor's degree or expertise.”2 But understand that tasks that aid patient care (e.g., calling to request outside records) or build patient rapport (e.g., getting a patient a cup of water) are not “scut-work,” even if they're non-clinical. (See “Activities students can perform.”)
2. Share the teaching responsibility. Engage your nurses, social workers, care managers, and patients in the education of students. This demonstrates to students the importance of team-based care and helps them become “collaborative experts.”3
3. Change your workflow to allow students to contribute before, during, and after visits. The classic apprenticeship model of medical education in family medicine typically follows one of two paths:
Students see some patients independently, then “report back” to the teaching physician what they learned through history and physical exam, with time for synthesis and plan formation. The teaching physician then reperforms the visit, verifying the student's findings. This path is less efficient but has more educational benefit for the student because it is active, experiential learning.
Students “shadow” the teaching physician, learning through observation with very little time for active skills training. This path is efficient but has less educational value for the student because it is passive.
While both paths may have their place within medical education, a hybrid model that integrates students in the workflow can result in efficiency, optimal learning, and improved patient care.4 This model is easier to implement thanks to a significant 2018 regulatory change. The Centers for Medicare & Medicaid Services (CMS) now allows teaching physicians to verify student documentation of evaluation and management (E/M) services rather than redocumenting this work.5 This prepares students for future practice and allows the teaching physician to use all elements of the students' notes for CMS billing. Previously, only social history, family history, and review of systems documented by the student could be used this way. These changes are a huge win for students and the physicians they work with. Preceptors should check with their own health systems and states regarding other EHR functions such as updating medication lists and order entry.
4. Engage students in panel management. Students should be given a panel of patients to follow throughout their rotations. This may include being part of visits in the office as well as proactively reaching out to patients who need care.4 It may be reasonable to have a student focus on a particular component of care, such as diabetes management or preventive care services (e.g., influenza vaccinations). The student can document care and quality metrics within registries and the EHR.
5. Involve students in community health. Patient care goes beyond the office. Students can make an impact on the health of your community by participating in health fairs, vaccination events, and other local health and wellness programs.
6. Let students participate in and even lead quality improvement (QI) activities. QI is a mainstay of modern medical practice. It's an expectation of family medicine and a requirement for American Board of Family Medicine (ABFM) and American Osteopathic Board of Family Physicians certification.6,7 QI is also important to reimbursement, which is increasingly tied to quality metrics. However, with so many demands in clinical practice, it can be challenging to dedicate time and resources to QI.8 Getting students involved allows them to gain meaningful experience while adding value to the practice.9 For example, at the University of North Carolina School of Medicine, the faculty introduced a QI curriculum and then sent students to clinical practices where they applied the skills they had learned. It was a success. Students learned, and quality metrics at the clinical sites improved.10,11
7. Advocate for longer teaching relationships. When students spend more than just a few weeks in your office, it helps them more fully integrate and become truly valued and accountable team members.3 Many medical schools have transitioned to longitudinal clerkships in which students get prolonged clinical exposure to primary care.12 Just like building relationships with patients, building relationships with students can allow you to partner with them more meaningfully.
The strategies outlined above are intended to enhance the experience of physicians, students, and patients. But it may be overwhelming for even the most seasoned preceptor to try all these changes at once. Consider a step-by-step approach, choosing strategies that make sense for your setting, practice structure, and students' abilities.
| Before the visit | During the visit | After the visit |
|---|---|---|
|
|
|
COMMUNITY-BASED MEDICAL EDUCATION NEEDS YOU
Community-based medical education is important, but wouldn't be possible without community preceptors volunteering their time.13 Preceptors repeatedly identify several factors that motivate them to start teaching and keep them coming back: relationships with students, giving back to the profession, enjoyment of teaching, and enhanced clinical knowledge.14
While these intrinsic factors are major drivers, educational institutions are increasingly recognizing that precepting is a huge ask of community physicians. Individual medical schools vary in how they say “thank you,” with some offering discounted CME, faculty awards, or payment for hosting students.15 The ABFM is now incentivizing teaching through the Precepting Performance Improvement Program, one of many options family physicians have to meet the performance improvement portion of the ABFM certification. By completing a performance improvement project focused on clinical teaching and hosting students in their office, ABFM diplomates can claim performance improvement credit through a sponsoring institution.
If you're not yet a preceptor, it's easy to start. Contact your local medical school or alma mater or visit https://www.teachingphysician.org and click on “Become a Preceptor” at the top of the page.
