Identifying your patients, sorting them by risk, and managing their chronic conditions as a team can help you make the most of value-based care programs.

As health care costs spiral higher, more payers are looking to replace the fee-for-service (FFS) system with value-based payment models focused on quality (rather than quantity) of care.
The National Academy of Medicine defines value-based care (VBC) as safe, timely, efficient, equitable, effective, and patient-centered — or STEEEP.1 The University of Utah Health offers a more practical definition, the value equation:2 Value = (Quality × Patient Experience) / Cost.
Value increases when costs go down while quality and patient experience improve. Thus, VBC programs incentivize increased quality (measured through a variety of health metrics) and decreased cost (e.g., keeping patients out of hospitals or emergency departments).
Physicians are often understandably wary of any new payment model. Many of us have been around long enough to hear about the “next great thing” in health care payment reform, only to watch it evaporate while we all keep running on the FFS hamster wheel. But what if we were paid up front to take care of patients and also rewarded for good clinical outcomes? In principle, that's VBC.
KEY POINTS
- Payers are moving away from fee-for-service payments and toward value-based care (VBC) as a way to curb ever-rising health care costs.
- Identifying the patients for whom you're responsible, sorting them by risk, and then managing their chronic conditions as a team are keys to succeeding in VBC.
- There are several pitfalls to avoid in VBC arrangements. If your diagnosis codes are not precise, for example, payers may not adequately credit you for high-risk patients.
VALUE-BASED PAYMENT MODELS
There is not just a single VBC program for your practice to join. Instead, there is a hodgepodge of ever-changing models from Medicare, Medicaid, commercial insurers, and private employers. Unfortunately, sometimes these models come and go (e.g., Medicare's Comprehensive Primary Care Plus program, which is ending this year3), and sometimes their rules and measures are similar, but not quite the same.
It would be simpler and less frustrating if there was a unified, lasting VBC system with consistent metrics. We're not there yet, but a decade of lessons learned is getting us closer.4 However you feel about it, VBC is not going away. In fact, it continues to grow because the goal of improving health outcomes by rewarding clinical quality, prevention of illness, and cost-effective care is appealing to patients, physicians, and payers.
If you're ready to get started in VBC, here are four skills you'll need to succeed and some pitfalls you'll want to avoid.
EMPANELMENT
To take care of your patients, you need to know who they are. Under FFS, we are paid for the patients we see; if a patient doesn't come through the doors of our office or hospital, we are not paid. In VBC, we are paid to care for a set panel of patients, regardless of how many times they visit the clinic.
Empanelment is the “process of identifying and assigning active patients to clinicians or care teams to establish and maintain patient-clinician relationships.”5 Empanelment allows for continuity of care, and continuity of care improves outcomes and patient satisfaction.6
The first step in empanelment is to define “active patient.” For many practices, it's any patient seen within the previous 24 to 36 months. In this digital age, a better definition is probably any patient you interacted with during that time period, including face-to-face visits, telehealth, asynchronous web messaging, etc.
The next step is to check patient attribution lists provided by payers. Patients may have designated you as their primary care physician when they signed up for insurance, even if they've never been in your office (or haven't been for years). If you are assigned patients you have not seen, you can proactively reach out and encourage them to come in for an office visit. Or you can work with the payer to “clean up” the list and remove patients with whom you have no professional relationship.
A patient panel is a living thing. It will change month to month as patients move, die, get new insurance, or find a different primary care doctor. Therefore, the final step in empanelment is to ensure you're updating your panel regularly. There is no formal guideline, but once a year is a reasonable benchmark.
RISK STRATIFICATION
While it varies some from year to year, studies have found that 5% of the U.S. population accounts for almost 50% of health care spending.7 That means you will be more successful in value-based payment programs if you can identify your most high-risk patients and help them avoid “downstream” complications that require expensive care.
Risk stratification is the process of assigning patients to higher- and lower-risk groups. It is critical to achieving good outcomes in VBC. High-risk patients require the most resources, but keeping them healthy yields the greatest rewards.
Methods for sorting your patients into higher- and lower-risk groups have been described in previous FPM articles.8 But one of the quickest ways is to use hierarchical condition category (HCC) codes, which payers combine with patient demographic data (such as age and gender) to assign a risk adjustment factor (RAF) score. A higher score suggests a more complex patient.9 For example, a 69-year-old male with uncomplicated diabetes has a RAF score of 0.40. That same patient with diabetic complications and major depression has a RAF score of 1.01. Sorting your panel by RAF and identifying those with the highest scores is an easy way to do objective risk stratification.
PANEL MANAGEMENT
“Taking care of the patients not in front of you” is one way to think about panel management. It requires proactively managing all the patients assigned to you, which is at the heart of VBC. In my practice, we have 618 patients with diabetes, and on a given morning I might see four of them. What about the other 614? Are we checking in with them to ensure they're managing their chronic condition?
“Panel management” means proactively addressing patient problems, closing care gaps, identifying high-risk patients, and preventing avoidable emergency department visits and inpatient hospitalizations. For example, who are the high-risk patients who should be prioritized for a flu shot? Are you performing breast cancer screenings on all patients who fit the guidelines? What patients should your care manager be working with?
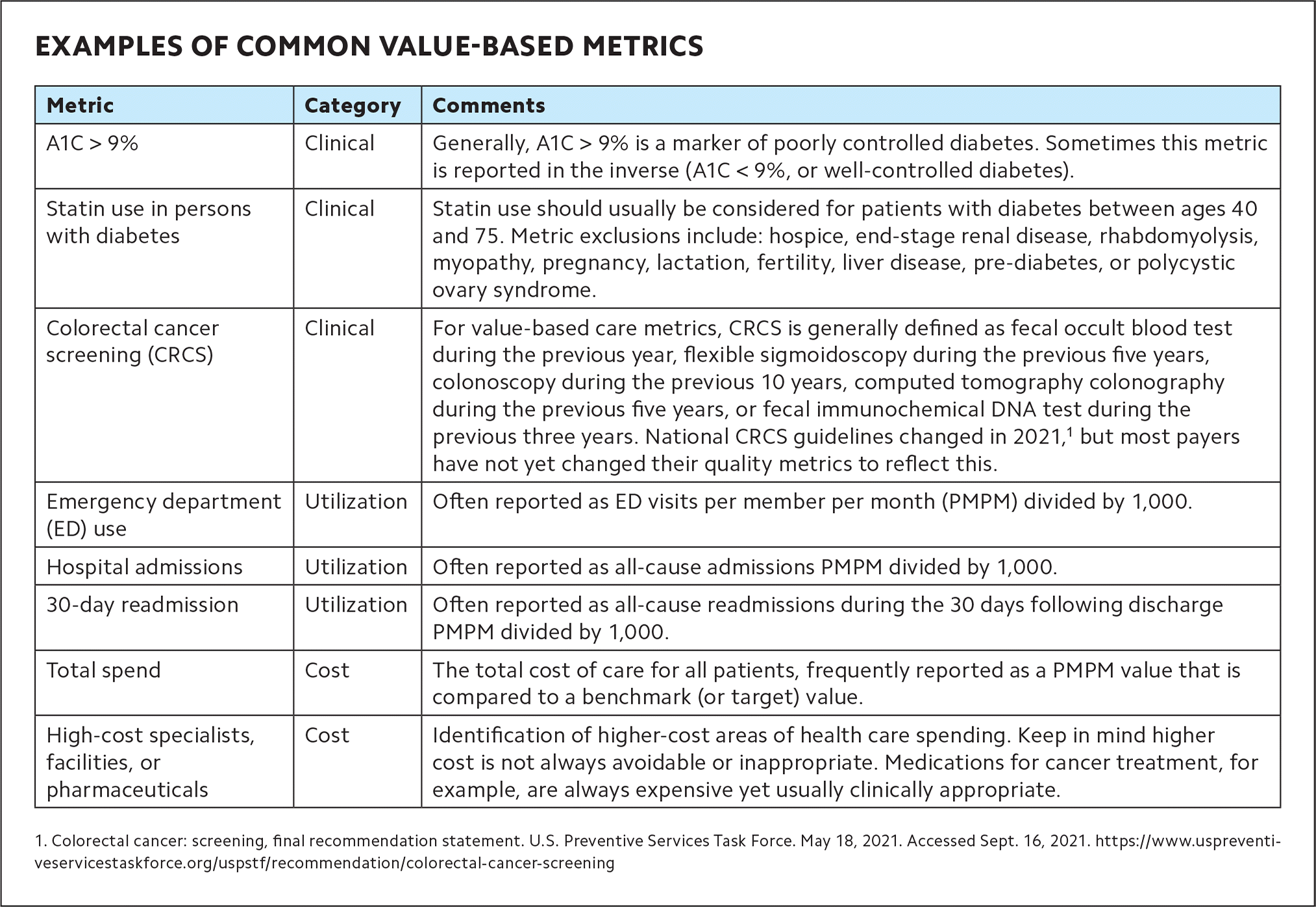
Successful panel management improves patient outcomes. Payers use a variety of metrics to assess your performance, such as the percentage of patients with diabetes who have an A1C > 9% (see “Examples of common value-based metrics”). Some payers give you the data at regular intervals, and some EHRs can produce data reports on demand so you can gauge your performance whenever you want.
EXAMPLES OF COMMON VALUE-BASED METRICS
| Metric | Category | Comments |
|---|---|---|
| A1C > 9% | Clinical | Generally, A1C > 9% is a marker of poorly controlled diabetes. Sometimes this metric is reported in the inverse (A1C < 9%, or well-controlled diabetes). |
| Statin use in persons with diabetes | Clinical | Statin use should usually be considered for patients with diabetes between ages 40 and 75. Metric exclusions include: hospice, end-stage renal disease, rhabdomyolysis, myopathy, pregnancy, lactation, fertility, liver disease, pre-diabetes, or polycystic ovary syndrome. |
| Colorectal cancer screening (CRCS) | Clinical | For value-based care metrics, CRCS is generally defined as fecal occult blood test during the previous year, flexible sigmoidoscopy during the previous five years, colonoscopy during the previous 10 years, computed tomography colonography during the previous five years, or fecal immunochemical DNA test during the previous three years. National CRCS guidelines changed in 2021,1 but most payers have not yet changed their quality metrics to reflect this. |
| Emergency department (ED) use | Utilization | Often reported as ED visits per member per month (PMPM) divided by 1,000. |
| Hospital admissions | Utilization | Often reported as all-cause admissions PMPM divided by 1,000. |
| 30-day readmission | Utilization | Often reported as all-cause readmissions during the 30 days following discharge PMPM divided by 1,000. |
| Total spend | Cost | The total cost of care for all patients, frequently reported as a PMPM value that is compared to a benchmark (or target) value. |
| High-cost specialists, facilities, or pharmaceuticals | Cost | Identification of higher-cost areas of health care spending. Keep in mind higher cost is not always avoidable or inappropriate. Medications for cancer treatment, for example, are always expensive yet usually clinically appropriate. |
1. Colorectal cancer: screening, final recommendation statement. U.S. Preventive Services Task Force. May 18, 2021. Accessed Sept. 16, 2021. https://www.uspreventiveservicestaskforce.org/
TEAM-BASED CARE
Teamwork is key to success in VBC. A care team may consist of only a physician and a medical assistant or advanced practice provider, or it could include any number of ancillary providers such as pharmacists and counselors.
Depending on the size of your office, you may have multiple care teams. These smaller teams, often called “teamlets,”10 are each responsible for managing the care of a panel of patients.
The care team's power comes from two things: 1) allowing team members to work at the top of their licenses and 2) off-loading nonclinical responsibilities from physicians and other clinicians. How much nonphysician team members can do clinically depends on your state laws and institutional policies regarding scope of practice, but encourage staff to do as much as they can within those boundaries.
At least once a day, the care team should huddle. Huddles make the day flow more smoothly by proactively managing the schedule. Huddles can be a quick, informal overview of the day in which you flag any key visits, or they can be a formal step-by-step analysis of the day's patients (see “Huddle checklist”).
Huddles allow a team to sort patient care responsibilities into “tasks for staff and decisions for physicians,” as my colleague, William J. Warning II, MD, has put it. For example, in my office, my medical assistant prepares the electronic chart for me by focusing on the tasks of care. She will identify a patient's last colonoscopy, urine microalbuminuria, or pneumonia vaccine. If the patient is due for another, she'll place the order in the chart for me. She will also gather records from specialists, hospitals, and emergency departments. This allows me, the physician, to focus on decisions: Does the patient need to be on a statin? What can I do to help the patient quit smoking? How many milligrams of furosemide should I prescribe?
Using a combination of standing orders and workflow redesign, clinicians can be freed up to manage patients (“decisions”) while the rest of the team handles other duties (“tasks”).
HUDDLE CHECKLIST
Things to discuss during your daily team huddle:
- High-risk patients,
- Hospital, emergency department, or nursing facility follow-up visits,
- Results or referrals needed for the day,
- Patient-specific issues,
- Scheduling: clinician and staff,
- Scheduling: patients (back-to-back lengthy visits, openings, etc.),
- Potential bottlenecks (work slowdowns),
- Safety issues (sound-alike names, equipment issues, transportation, etc.),
- Patient risk levels.
FIVE PITFALLS
Following the steps outlined above creates a good framework for success in VBC programs. But there are some pitfalls to watch for.
Paltry payments. One of the most common complaints physicians have with VBC is payers not fully committing to a value-based arrangement, which leads to very little change in care or clinical outcomes. Some payers offer only small payments for care coordination or shared savings (see “Getting paid in value-based care”). The result is a “value-based” contract that is nearly indistinguishable from a FFS contract. Sufficient up-front investment from payers is critical to VBC success. Be mindful of this when choosing which VBC programs to join. The Health Care Payment Learning & Action Network has a tool to compare different VBC models.11
GETTING PAID IN VALUE-BASED CARE
In VBC arrangements, payments are typically structured in one of three ways:
- Fee-for-service (FFS): Per-encounter payments at a rate that allows clinicians to capture the value of their daily work and of goods and services used.
- Care coordination: Up-front per-patient payments provided to take care of patients outside traditional face-to-face visits. The payments are often made on a monthly basis.
- Shared savings: Retrospective payments made after cost and quality benchmarks have been achieved.
Clunky data reporting. A colleague recently shared her experience trying to report an accurate record of her colorectal cancer screening (CRCS) performance. In most instances, she ordered the screening, the patient completed the test, and results were available in the chart. Unfortunately, they weren't stored in a data field that could easily be reported. As a result, her reported performance looked worse than her actual clinical performance. Having accurate and precise data reporting capabilities is critical to VBC. An ideal reporting platform combines clinical data from the EHR with patients' insurance claims data.
Poor change management. Not having a change management plan can be a barrier to achieving better outcomes. Without a plan to implement and sustain change, the “old ways” will quickly return. The same colleague who told me of her frustration with her CRCS data was even more upset about her organization's proposed solution: create an order in the EHR for the colonoscopy and enter the results herself. Her organization is failing her by not supporting a transformational, team-based approach that frees her up to focus on clinical decision-making. There are several models of change management, such as Kotter's 8-Step Model and Lewin's 3-Stage Model of Change,12 which practices can follow to effect change.
Lack of incentives. The incentive under FFS is productivity: the more billed charges, the greater potential for financial success. This is not the case in VBC, where things like clinical outcomes and patient utilization are just as important. The goal is to achieve some degree of the triple aim: better patient experience, better clinical outcomes, and reduced costs.13 Practices need to institute appropriate incentives for clinicians and staff to reward performance in VBC. Transparent reporting, in which everyone gets to see how everyone else is doing, can incentivize better performance. Financial incentives for hitting clinical targets are also an option, but external motivators such as bonuses for clinicians and gift cards for staff typically only drive short-term outcomes.14 Long-term success comes from intrinsic motivators, such as the sense of accomplishment and satisfaction we get from doing something well. In this case, the joy of being freed to focus on patient care without the “hamster-wheel” mentality of FFS can be a powerful — and durable — intrinsic motivator.
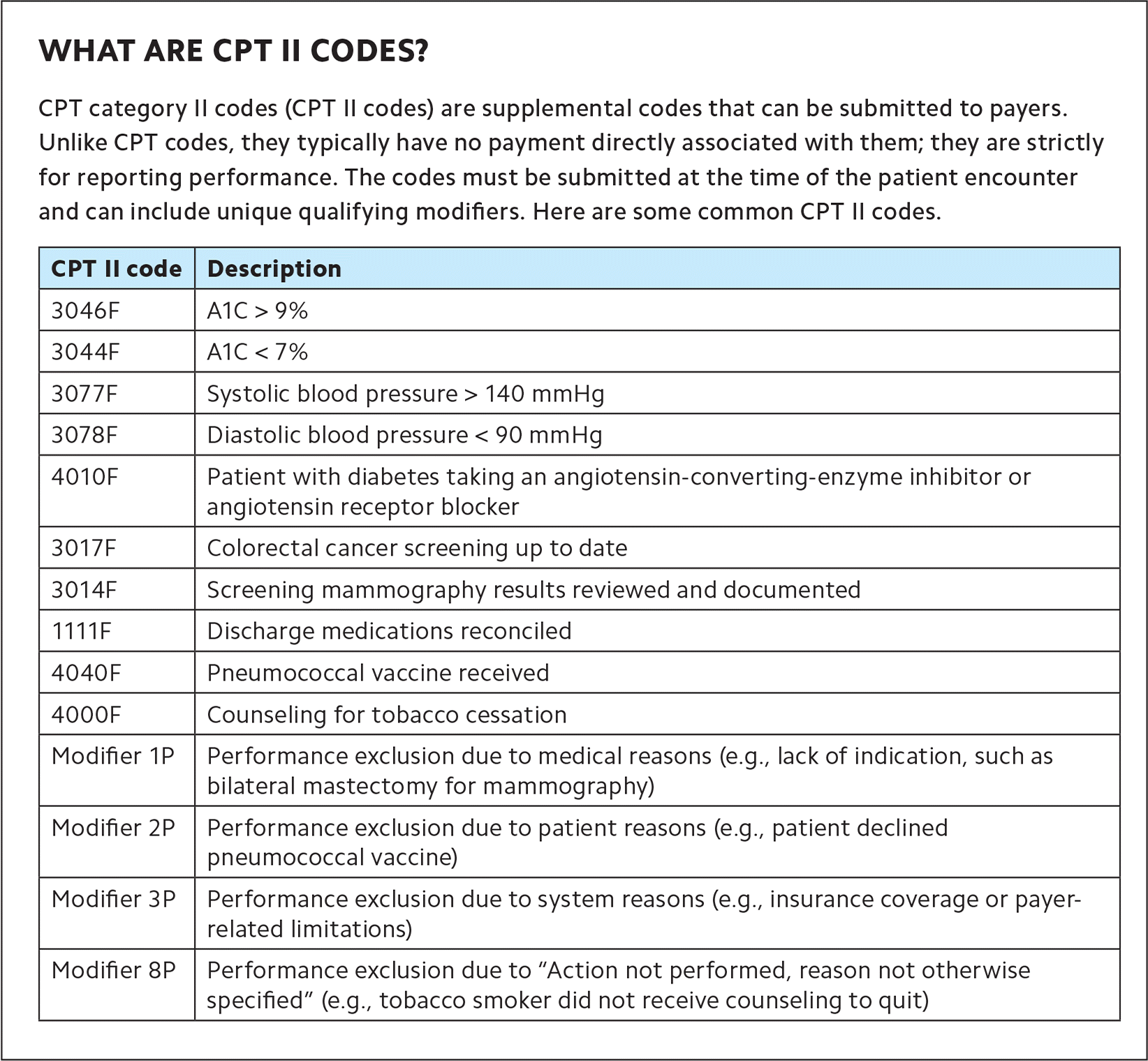
Coding missteps. Inaccurate or imprecise diagnosis coding will hinder long-term success.15 Payment under VBC is directly tied to the disease burden of your patient panel. Sicker patients require more resources; therefore, practices receive more reimbursement for those patients.16 Correctly coding a patient with diabetes complications (e.g., diabetic neuropathy) will support better financial performance. It will also give you a better clinical understanding of your patient panel. For example, let's say I want a list of all my patients with poorly controlled diabetes so I can assign them to my care manager and enroll them in diabetic education. If I've coded all my patients with diabetes using ICD-10 code E11.9, then I have no way of knowing which ones are poorly controlled. But if I've coded only patients with well-controlled diabetes with E11.9, and coded those with out-of-range A1C measurements with E11.65 and so forth, then I will better understand my panel's disease burden. Diagnosis codes map to HCC codes, which factor into the RAF scores payers use to assess patient risk. Under the current HCC model, each patient's RAF score “resets” to zero on Jan. 1. This is one reason to make sure all Medicare or Medicare Advantage patients have their annual wellness visit, as it allows you to capture all the relevant and appropriate diagnosis codes each year.17 Some payers also allow reporting of CPT II codes (see “What are CPT II codes?”) to supplement ICD-10 coding.
WHAT ARE CPT II CODES?
CPT category II codes (CPT II codes) are supplemental codes that can be submitted to payers. Unlike CPT codes, they typically have no payment directly associated with them; they are strictly for reporting performance. The codes must be submitted at the time of the patient encounter and can include unique qualifying modifiers. Here are some common CPT II codes.
| CPT II code | Description |
|---|---|
| 3046F | A1C > 9% |
| 3044F | A1C < 7% |
| 3077F | Systolic blood pressure > 140 mmHg |
| 3078F | Diastolic blood pressure < 90 mmHg |
| 4010F | Patient with diabetes taking an angiotensin-converting-enzyme inhibitor or angiotensin receptor blocker |
| 3017F | Colorectal cancer screening up to date |
| 3014F | Screening mammography results reviewed and documented |
| 1111F | Discharge medications reconciled |
| 4040F | Pneumococcal vaccine received |
| 4000F | Counseling for tobacco cessation |
| Modifier 1P | Performance exclusion due to medical reasons (e.g., lack of indication, such as bilateral mastectomy for mammography) |
| Modifier 2P | Performance exclusion due to patient reasons (e.g., patient declined pneumococcal vaccine) |
| Modifier 3P | Performance exclusion due to system reasons (e.g., insurance coverage or payer-related limitations) |
| Modifier 8P | Performance exclusion due to “Action not performed, reason not otherwise specified” (e.g., tobacco smoker did not receive counseling to quit) |
WHERE TO BEGIN
So how do you get started in a VBC program? It may be as simple as signing up. Many commercial insurance companies have programs that you can opt in to. Primary Care First (PCF) is a nationwide value-based approach for Medicare patients, but it's only available in some parts of the country.18
You could also consider joining an accountable care organization (ACO). An ACO is a group of physicians and other providers who partner to manage the health outcomes of a population of patients. There may be local ACOs sponsored by other providers or health systems near you, and there are also some national ACOs. My practice belongs to a local ACO, which gives us access to resources we otherwise couldn't afford (such as a registered nurse care manager). It also allows us to take advantage of value-based contracts that might have been out of our reach as a small, independent practice.
There are other, less traditional ways for practices to embrace VBC. Some have joined nationwide models funded by payers, large employers, or venture capitalists.19 Examples include Oak Street Health, Agilon, Aledade, One Medical, and Optum, among others. That list is not an endorsement of those organizations or that approach, but rather a starting point for finding the best fit for your practice should you choose to go that route.
Our national shift from FFS to VBC relies heavily on a strong primary care backbone. Primary care has traditionally been underfunded and overworked. Even a small change in that calculus could dramatically improve our health care system. For every $100 spent on health care in the United States, only about $5 is spent on primary care.20 Meanwhile, every $1 invested in primary care saves the health care system up to $13, and it's been estimated that doubling the nation's current spending on primary care would pay for itself in savings.21, 22 Family physicians represent the greatest opportunity for improving health care quality and lowering cost — in other words, increasing value.

