Hierarchical condition categories are key for improving health outcomes and getting accurate reimbursements.

At the heart of value-based care programs are the dual goals of lowering health care costs and improving outcomes. One powerful way to reach those goals is to identify patients at high risk of serious health events such as emergency department visits or inpatient hospitalizations and prevent them. Regulatory agencies and payers use hierarchical condition categories (HCCs) to calculate patient risk; the higher the risk score for a population, the higher the benchmark will be for expenditures, which can affect shared savings in value-based payment arrangements.1
HCC codes are determined by corresponding diagnosis codes reported on claims. Not all diagnosis codes “ladder up” to HCC codes for risk adjustment, but those that do carry more weight in your patient panel.2 Failing to use accurate diagnosis codes can underreport your patients' severity of illness, which can affect reimbursement in value-based care arrangements.
It's not just a financial concern, though. Accurate diagnosis coding can help your team identify high-risk patients and give them the right care at the right time.
KEY POINTS
- Payers use hierarchical condition category (HCC) codes to capture patient risk for value-based care programs.
- HCC codes are based on ICD-10 codes on claims, which makes accurate diagnosis coding critical to success in value-based care.
- There are a number of ways to ensure that HCC codes accurately represent your patient panel's risk, including avoiding unspecified and symptom codes when a more accurate diagnosis code is available.
KEYS TO CAPTURING RISK
Here are 10 things to remember about risk-adjustment coding.
Duration: HCC codes reset annually, so diagnoses that remain active need to be reported every calendar year (starting Jan. 1) for each patient. They only need to be reported once but must be reported each year, regardless of how long the patient has had the condition. So, if you're doing an annual wellness visit for a patient who has moderate, recurrent major depressive disorder (ICD-10 code F33.1), which has a corresponding HCC code (59), and you discuss the patient's depression (e.g., medications and current management), you can report that diagnosis code for the encounter. In this way, you will not only capture the patient's risk level, which can ensure accurate value-based care payments, but also make sure the patient's condition is being managed proactively.
Specificity: Avoid unspecified diagnosis codes. Most unspecified codes do not risk adjust, so use the most specific code possible for each diagnosis. For example, if you're coding all of your patients with type 2 diabetes using ICD-10 code E11, you're not capturing the true risk for those who have type 2 diabetes with diabetic chronic kidney disease (E11.22) or type 2 diabetes with hyperglycemia (E11.65). Those extra digits make a big difference in HCC codes. Even E11.9 (type 2 diabetes without complications) carries some weight in HCC coding. Being as specific as you can with your diagnosis codes will also help you track which patients have their chronic conditions under control and which need more management.
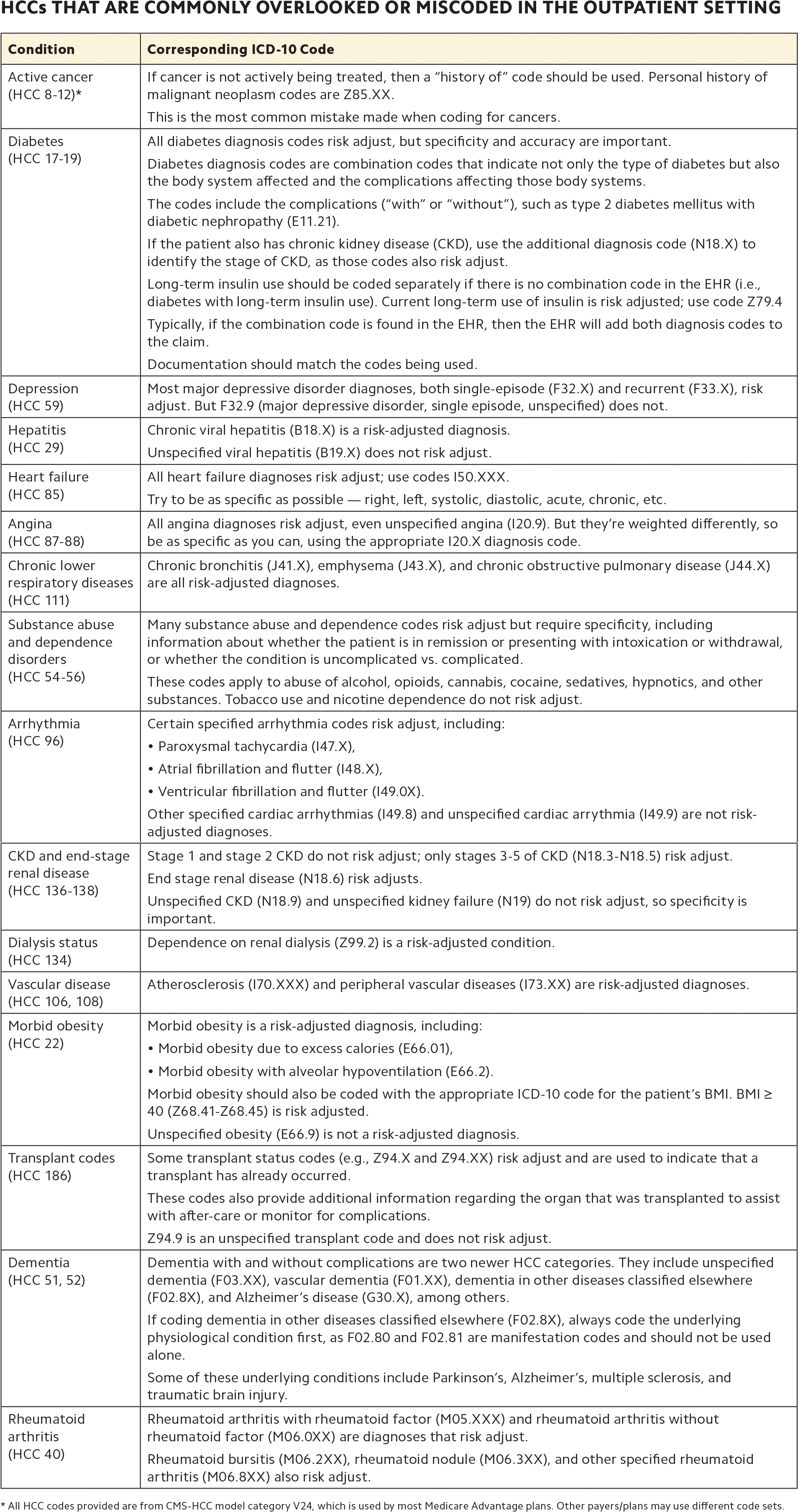
Chronic conditions: When seeing your patients with chronic diseases, keep in mind that many chronic conditions are HCCs (see “HCCs that are commonly overlooked or miscoded in the outpatient setting”). Not all chronic diseases are addressed at every visit, so make sure you are addressing each chronic disease at least annually. That will get them counted toward the patient's HCC risk-adjustment score for the year and help you proactively manage those conditions.
HCCs THAT ARE COMMONLY OVERLOOKED OR MISCODED IN THE OUTPATIENT SETTING
| Condition | Corresponding ICD-10 Code |
|---|---|
| Active cancer (HCC 8–12)* | If cancer is not actively being treated, then a “history of” code should be used. Personal history of malignant neoplasm codes are Z85.XX. |
| This is the most common mistake made when coding for cancers. | |
| Diabetes (HCC 17-19) | All diabetes diagnosis codes risk adjust, but specificity and accuracy are important. |
| Diabetes diagnosis codes are combination codes that indicate not only the type of diabetes but also the body system affected and the complications affecting those body systems. | |
| The codes include the complications (“with” or “without”), such as type 2 diabetes mellitus with diabetic nephropathy (E11.21). | |
| If the patient also has chronic kidney disease (CKD), use the additional diagnosis code (N18.X) to identify the stage of CKD, as those codes also risk adjust. | |
| Long-term insulin use should be coded separately if there is no combination code in the EHR (i.e., diabetes with long-term insulin use). Current long-term use of insulin is risk adjusted; use code Z79.4 | |
| Typically, if the combination code is found in the EHR, then the EHR will add both diagnosis codes to the claim. | |
| Documentation should match the codes being used. | |
| Depression (HCC 59) | Most major depressive disorder diagnoses, both single-episode (F32.X) and recurrent (F33.X), risk adjust. But F32.9 (major depressive disorder, single episode, unspecified) does not. |
| Hepatitis (HCC 29) | Chronic viral hepatitis (B18.X) is a risk-adjusted diagnosis. |
| Unspecified viral hepatitis (B19.X) does not risk adjust. | |
| Heart failure (HCC 85) | All heart failure diagnoses risk adjust; use codes I50.XXX. |
| Try to be as specific as possible — right, left, systolic, diastolic, acute, chronic, etc. | |
| Angina (HCC 87-88) | All angina diagnoses risk adjust, even unspecified angina (I20.9). But they're weighted differently, so be as specific as you can, using the appropriate I20.X diagnosis code. |
| Chronic lower respiratory diseases (HCC 111) | Chronic bronchitis (J41.X), emphysema (J43.X), and chronic obstructive pulmonary disease (J44.X) are all risk-adjusted diagnoses. |
| Substance abuse and dependence disorders (HCC 54-56) | Many substance abuse and dependence codes risk adjust but require specificity, including information about whether the patient is in remission or presenting with intoxication or withdrawal, or whether the condition is uncomplicated vs. complicated. |
| These codes apply to abuse of alcohol, opioids, cannabis, cocaine, sedatives, hypnotics, and other substances. Tobacco use and nicotine dependence do not risk adjust. | |
| Arrhythmia (HCC 96) | Certain specified arrhythmia codes risk adjust, including:
Other specified cardiac arrhythmias (I49.8) and unspecified cardiac arrythmia (I49.9) are not risk-adjusted diagnoses. |
| CKD and end-stage renal disease (HCC 136–138) | Stage 1 and stage 2 CKD do not risk adjust; only stages 3–5 of CKD (N18.3-N18.5) risk adjust. |
| End stage renal disease (N18.6) risk adjusts. | |
| Unspecified CKD (N18.9) and unspecified kidney failure (N19) do not risk adjust, so specificity is important. | |
| Dialysis status (HCC 134) | Dependence on renal dialysis (Z99.2) is a risk-adjusted condition. |
| Vascular disease (HCC 106, 108) | Atherosclerosis (I70.XXX) and peripheral vascular diseases (I73.XX) are risk-adjusted diagnoses. |
| Morbid obesity (HCC 22) | Morbid obesity is a risk-adjusted diagnosis, including:
Morbid obesity should also be coded with the appropriate ICD-10 code for the patient's BMI. BMI ≥ 40 (Z68.41-Z68.45) is risk adjusted. Unspecified obesity (E66.9) is not a risk-adjusted diagnosis. |
| Transplant codes (HCC 186) | Some transplant status codes (e.g., Z94.X and Z94.XX) risk adjust and are used to indicate that a transplant has already occurred. |
| These codes also provide additional information regarding the organ that was transplanted to assist with after-care or monitor for complications. | |
| Z94.9 is an unspecified transplant code and does not risk adjust. | |
| Dementia (HCC 51, 52) | Dementia with and without complications are two newer HCC categories. They include unspecified dementia (F03.XX), vascular dementia (F01.XX), dementia in other diseases classified elsewhere (F02.8X), and Alzheimer's disease (G30.X), among others. |
| If coding dementia in other diseases classified elsewhere (F02.8X), always code the underlying physiological condition first, as F02.80 and F02.81 are manifestation codes and should not be used alone. | |
| Some of these underlying conditions include Parkinson's, Alzheimer's, multiple sclerosis, and traumatic brain injury. | |
| Rheumatoid arthritis (HCC 40) | Rheumatoid arthritis with rheumatoid factor (M05.XXX) and rheumatoid arthritis without rheumatoid factor (M06.0XX) are diagnoses that risk adjust. |
| Rheumatoid bursitis (M06.2XX), rheumatoid nodule (M06.3XX), and other specified rheumatoid arthritis (M06.8XX) also risk adjust. | |
* All HCC codes provided are from CMS-HCC model category V24, which is used by most Medicare Advantage plans. Other payers/plans may use different code sets.
Symptoms: Physicians should avoid using symptom codes if a specific diagnosis code can be used instead. For example, don't simply report “other chest pain” (R07.89) if the patient has unspecified angina (I20.9). Symptom codes do not risk adjust, but many diagnosis codes do, including all angina codes (unspecified angina is one of the few unspecified codes that risk adjust).
Secondary diagnoses: Physicians often address a risk-adjusted diagnosis (or diagnoses) during a visit even if it is not the primary reason for the visit. Don't forget to code for the risk-adjusted diagnosis if you addressed it or if it played a role in managing the patient's other condition (e.g., considering a patient's diabetes when treating an allergic reaction).
Documentation is key in these instances. Remember the acronym MEAT to document that you monitored, evaluated, assessed/addressed, or treated the condition in order to code for the diagnosis during that visit. Ask yourself if the diagnosis affected the care of the patient during that visit. If the diagnosis played a role in your medical decision making, you can code it, but make sure your documentation supports the code.
Complications: If a condition has a complication, don't forget to code for the complication as well as the condition. The most often-missed risk-adjusted complications are those related to diabetes.
Medicare wellness visits: A diagnosis code that risk adjusts can be used for a Medicare wellness visit if the condition is addressed during the visit, but it should not be the primary diagnosis for the visit. As mentioned, annual visits are a good opportunity to confirm that past conditions are still present, because HCC codes reset each year.
Undocumented codes: If a patient has a diagnosis that you are not documenting, it not only affects reimbursement in value-based care but also affects patient outcomes. Health care professionals often rely on documentation to provide the best care. If a diagnosis is not documented, the patient's care team may not be aware of the diagnosis and may fail to consider it in their treatment plans.
Diagnosis code specificity tool: Electronic health record (EHR) vendors often use many different descriptions for the same diagnosis code to make it easier for users to search for diagnoses. Don't let different descriptions for the same ICD-10 code fool you. If your EHR has a diagnosis code calculator, make sure you use it to help you code to the highest level of specificity supported by documentation.
“History of” codes: If a patient's condition is currently being treated, do not use “history of” codes for that condition. This includes chronic conditions such as diabetes and heart failure, along with cancers. For example, if a patient with breast cancer has had a tumor removed through mastectomy but is still receiving adjuvant therapy to prevent recurrence, the condition should be coded as an active cancer case.
Keeping these 10 items in mind will help ensure that your patients are risk adjusted accurately so that you can get appropriate reimbursement from value-based care programs. It should also help you and the rest of the care team track your patients' conditions more thoroughly, which leads to better health outcomes.

