These five strategies can help you create positive and compassionate patient interactions without adding significant time to the visit.

It has been a busy day in clinic, and your 10th patient of the morning is roomed 30 minutes late. The reason given for the visit is “preventive health.” When you enter the exam room, you introduce yourself and confirm the patient is there for a preventive check-up. Then you ask about health behaviors and screenings, do an exam, and make a plan for testing and immunizations. As you are finishing up the visit, the patient says, “But we never discussed my concerns. I'm having this wrist pain and hand numbness, which have been bothering me a lot. And I keep getting headaches. I'm having one right now, and it's terrible. And my knees are giving out on me a lot, and I'm wondering what you think I should do.” Feeling exasperated, you explain that you don't have time to address these complaints and the patient should follow up at a later date because you have other patients waiting. The patient agrees and leaves, but later gives you a poor review and switches to another practice because “My concerns weren't listened to.”
WHY COMMUNICATION MATTERS
A positive patient experience is the result of multiple factors before, during, and after the patient encounter, but chief among them is effective doctor-patient communication. When patients and physicians communicate well, outcomes are better,1 in part because patients are more engaged in their health care. Patients who take an active role in their health can confidently bring up concerns and make lifestyle changes.2
Physicians are constantly being evaluated as communicators — through online ratings, post-visit surveys, etc. Although patient satisfaction scores can push us to improve, they may also add performance pressures if we lose sight of the true goal, which is not to improve “scores” but to build trust.3
This article describes how we can improve communication with our patients without pushing ourselves toward more burnout. Because time constraints are the primary concern for most physicians, we have chosen to focus on five strategies that create positive and compassionate interactions without adding significantly to the time with the patient.
KEY POINTS
- When patients and physicians communicate well, outcomes are better, and patients are engaged in their health care.
- Making a non-medical “connection” with the patient at the beginning of the encounter takes 1–2 minutes but can improve the patient's perception of the interaction.
- Agenda-setting, open-ended questions, reflective statements, and visit summaries are strategies that can improve communication without adding much time to the visit.
1. MAKE A POSITIVE CONNECTION WITH THE PATIENT
Making a positive connection is not always easy, especially when our days are rushed and we are stressed and distracted, but each encounter should set the stage for respectful communication.
Before entering the exam room, take a slow, mindful breath to re-center yourself. When entering the room, make eye contact with the patient, warmly introduce yourself, and explain your role. Clarify how the patient would like to be addressed and include others in the room in the introduction. Although it's tempting to start by asking “How are you?” this can be confusing for the patient, who is there seeking care for a concern, and it may jump-start the medical interview before introductions have finished. Making a non-medical “connection” with the patient at the beginning of the encounter takes only 1–2 minutes but can improve the patient's perception of the interaction.4 This can be a simple comment about weather, sports, or other neutral topics. At the end of the encounter, thank the patient for entrusting their care to you.
Here are some examples of language physicians can use to make positive connections:
- “Hi, I am Dr. Smith, one of the family physicians here. How would you like me to call you?”
- “Well, it's nice to meet you, Rhonda. Who do you have with you today?”
- “It's nice to meet you. Is it still snowing outside? It's been so cold today!”
- “Thank you so much for coming to see me today. I really appreciate that you trusted us with this problem.”
2. DEMONSTRATE ACTIVE LISTENING
One common patient complaint is that physicians do not listen carefully to what they have to say. We can demonstrate active listening in several ways:
- Attend to patients without multitasking or distractions,
- Express nonverbally that we are listening through eye contact, sitting down, nodding, responding with facial expressions, and showing concern,
- Provide verbal cues (“Mmhmm”, “Ah-ha,” or “I see”),
- Allow patients to speak uninterrupted at the beginning of the visit.
An often-cited study from 1984 demonstrated that it takes patients two minutes at most to explain their complaint, but physicians often interrupt between 18 to 23 seconds.5 This can make the patient feel unheard and create missed opportunities to gather potentially important data. Interruptions include any statement that stops the patient's flow of thought.
Checking the EHR while the patient is talking can interfere with active listening, so avoid that if possible unless you've explained up front what you are doing (“I am just reviewing your recent labs so I can understand better what is going on”). If the patient drifts off on a tangent, gently redirect the conversation by saying, “That is interesting, but I really want to know more about [health item on agenda].”
After listening to the patient's chief complaint uninterrupted, it is imperative to pause and establish an agenda for the visit before gathering more history. To do this, ask “Is there something else you would like to discuss?” until the patient answers “No.” The term “something else” is preferable to “anything else” because it elicits more concerns without unduly lengthening the visit.6 Eliciting patients' concerns up front will help you avoid “doorknob” moments when you are leaving the room and their hidden agenda emerges after you have already used your allotted time. Once all the patient's concerns are elicited, add your own items as well. Then, negotiate a shared agenda of what you will address at the current visit.
This can be difficult when patients present with multiple concerns that don't match up with the concerns you've identified, or when patients don't have realistic expectations about what you can address given the visit's time constraints. If this is the case, have an open conversation with the patient about the need to prioritize their concerns as well as yours. If less acute concerns cannot be addressed at the current visit, make sure the patient understands that they will be discussed at a follow-up visit, not ignored or put aside. If you have already set the stage for respectful communication, the patient will be more likely to understand and accept the agenda.
4. USE OPEN-ENDED QUESTIONS AND REFLECTIVE STATEMENTS
Open-ended questions and reflective statements demonstrate concern and empathy for the patient.
After introductions and small talk have taken place, starting the patient interview with an open-ended question such as “How can I help you today?” has been shown to have high impact on physician communication scores.7 Use additional open-ended questions or statements throughout the encounter such as “Tell me more about that,” “What else have you noticed?” or “What are your thoughts about what is going on?”
Physicians are rated as more empathetic when they spend more time listening and making reflective statements.8 Reflecting the patient's emotional state, either directly (“You are frustrated”) or indirectly (“It seems like that would be frustrating”), can show that you empathize with their feelings. Ignoring a patient's emotional cues out of a sense of haste can backfire, leading to longer encounters. It is best to acknowledge when a patient seems upset, angry, or anxious. Continue using positive nonverbal communication to demonstrate your compassion and concern, and to assure the patient that you are listening. If complaints about care arise, asking “What can I do to make this better?” can help bring the conflict to a mutually agreeable solution.
5. SOLIDIFY THE RELATIONSHIP WITH CLEAR EXPLANATIONS
Patients often come away from their visits not knowing the actual name of their diagnosis, the reasons for their new medications, possible side effects, or what to expect next. It is important to explain things clearly — your thoughts, diagnoses, treatment recommendations, and plan for follow up — and to write down all new diagnoses and medications to allow full patient engagement. Having printed educational materials you can give to the patient can be helpful, as long as patient literacy and educational levels are considered. Visit summaries filled out by staff and physicians can provide helpful follow-up information and instructions post-visit. Even if you have explained things thoroughly during the visit, patients are often overwhelmed with information and may not hear everything correctly. The teach-back method has been shown to improve patient outcomes.9 You can preface it by saying, “I know we just went over a lot of information, so if you wouldn't mind, can you tell me what the next steps are, so I know I didn't miss anything?” This will ensure patient understanding and prevent further questions, calls, and re-explanations. In addition, at the end of every visit, ask “What questions do you have?” instead of “Do you have any questions?” as this encourages patient involvement.
POCKET GUIDE TO PATIENT COMMUNICATION
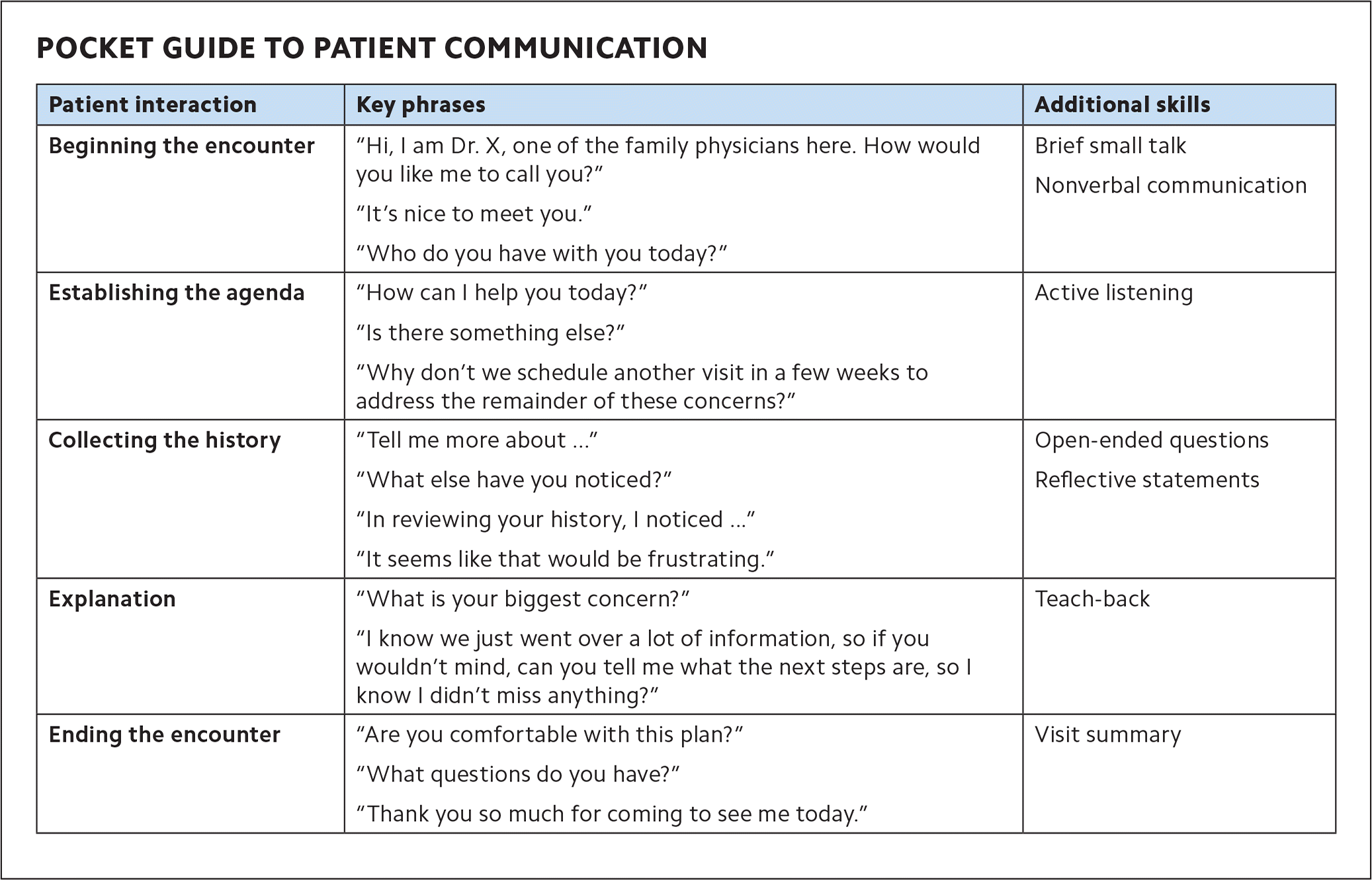
| Patient interaction | Key phrases | Additional skills |
|---|---|---|
| Beginning the encounter | “Hi, I am Dr. X, one of the family physicians here. How would you like me to call you?” “It's nice to meet you.” “Who do you have with you today?” | Brief small talk Nonverbal communication |
| Establishing the agenda | “How can I help you today?” “Is there something else?” “Why don't we schedule another visit in a few weeks to address the remainder of these concerns?” | Active listening |
| Collecting the history | “Tell me more about ...” “What else have you noticed?” “In reviewing your history, I noticed ...” “It seems like that would be frustrating.” | Open-ended questions Reflective statements |
| Explanation | “What is your biggest concern?” “I know we just went over a lot of information, so if you wouldn't mind, can you tell me what the next steps are, so I know I didn't miss anything?” | Teach-back |
| Ending the encounter | “Are you comfortable with this plan?” “What questions do you have?” “Thank you so much for coming to see me today.” | Visit summary |
WHAT ABOUT TIME CONSTRAINTS?
The time constraints of office visits are a concern shared by physicians and patients. Wait time and visit length can certainly affect patient satisfaction, but one study showed that what mattered more was the patient's perception of the amount of time spent with the physician.10 The techniques discussed above will enhance patient satisfaction even if the actual time spent with the patient is short. To address the time constraints of office visits, set expectations early on. Be up-front with patients without dismissing complaints by saying, “I know we have a lot of things that we'd both like to discuss, and I want to be able to give each of them the appropriate time and attention. Why don't we schedule another visit in a few weeks to address the remainder of these concerns?”
AN IMPROVED PATIENT VIGNETTE
Let's take another look at the previous patient vignette, this time applying some of the skills and tips discussed above.
It has been a busy day in clinic, and your 10th patient of the morning is roomed 30 minutes late. The reason given for the visit is “preventive health,” but your rooming staff notifies you that the patient has a lot of other concerns to address as well. Before entering the room, you note that you are feeling pretty stressed from the busy morning and remind yourself that you want to be present for your patient. You take a deep breath before entering the room. When you step inside, you say hello to the patient and introduce yourself. You comment on the weather outside and thank the patient for waiting for you, since you are running behind. You then say, “The nurse mentioned you are here for an annual visit but also have a lot of concerns. How can I help you today?” The patient shares complaints regarding her wrists, hands, and knees. You then say, “Before I ask you more about that, is there something else you'd like to discuss today?” The patient nods and tells you about the constant headaches. You ask again if there's something else, and the patient tells you that is all. You tell the patient that you want to give adequate time to these concerns, so you would like to address the hand pain and headaches today and save the long-term knee issue and annual visit for next time. After finishing your history and physical exam, you come up with a plan and write down instructions for the patient. Before saying goodbye, you tell the patient, “Thank you so much for bringing these concerns to me. I hope we can work together to figure out these issues.”
START WITH SMALL CHANGES
These small changes in communication can have a big impact on the patient experience. Just as we advise our patients who are trying to make major lifestyle changes to focus on small steps, we too should work on incorporating small changes one at a time, using your own style and personality, until it starts to feel natural. Don't worry if you slip back into old ways of doing things; just start again with the next patient. We have included a table of the most pertinent tips and phrases, which can be printed as a pocket card. As you seek to improve your communication skills, we hope that your patients will be happier and have better outcomes and that you will experience higher satisfaction.

