Using nurses and other staff to coordinate the care of patients being discharged from hospitals allows physicians to fulfill TCM requirements at sustainable costs.

Transitional care management (TCM) is a Medicare-billable service designed for health care teams to care for patients during their transition from hospitalization to home. The essence of TCM is that a physician or other clinician takes charge of the patient's care upon discharge to prevent care gaps. Evidence has shown that transitional care is needed to prevent adverse outcomes and improve quality of care.1–3
Our primary care clinic in an academic hospital implemented a team-based workflow to ensure we identified TCM-eligible patients and provided them appropriate care. After two years, our data has shown that the workflow not only improves patient outcomes and decreases emergency department visits but also can be financially sustainable. This article provides a roadmap for other practices to implement their own TCM workflow.
KEY POINTS
- Transitional care management (TCM) is a bundle of services intended to prevent care gaps for patients being discharged from the hospital to their home.
- Requirements to bill Medicare for TCM include attempting to contact the patient within two days of discharge and arranging a face-to-face visit in 14 days or less.
- By using nurses and other staff to identify, contact, and schedule TCM patients, clinics can form TCM programs that are sustainable at Medicare reimbursement rates.
TCM REQUIREMENTS AND CHALLENGES
Medicare beneficiaries are eligible to receive TCM services in the 30-day period following their discharge from an inpatient or partial hospitalization setting. TCM includes several components:
- An interactive contact within two business days of discharge. This can be a phone call, e-mail, or face-to-face communication with the patient or caregiver by the physician or clinical staff. The medical record must include documentation of at least two attempts to contact the patient.
- Certain non-face-to-face services. These include, but are not limited to, reviewing the hospital course and discharge summary, following up on or ordering pertinent tests, ensuring referrals are made, and educating the patient and caregiver.
- A face-to-face visit. This must be completed within 14 days of discharge and requires a minimum of moderate-complexity medical decision making for code 99495 (this is measured similarly to medical decision making in an evaluation and management visit).4 If the face-to-face visit occurs within seven days of discharge and the medical decision making is high-complexity, then the TCM is eligible for higher reimbursement using code 99496.
Primary care physicians face several challenges in providing effective and timely transitional care. Hospitals often function in silos and do not provide a “warm handoff” of the patient to the physician or assign responsibilities at the time of discharge (e.g., who gets notified if the patient develops problems during the transitional period). Clinicians have little time to check for discharges or initiate TCM because of their busy clinic responsibilities and consistent pressure of clinical productivity. And in the past, the payment system provided little financial incentive for collaboration during the transition between inpatient and outpatient care. Medicare introduced TCM codes in 2013 to change the incentives and promote better care coordination.
TCM WORKFLOW
Our family medicine clinic implemented a physician-led, nurse-coordinated TCM program in 2017 as part of an ongoing initiative5 to improve care during transitions in a financially sustainable manner.
We selected eligible patients for TCM services after discharge from our family medicine inpatient service. (The primary reasons for ineligibility were either that the patient didn't have Medicare as primary payer or was being discharged somewhere other than home, e.g., a skilled nursing facility, hospice, or intermediate care facility.) A dedicated registered nurse (RN) and administrative services coordinator reviewed an EHR-generated discharge list on business days. They completed chart review on patients discharging to home from either hospital observation or inpatient admission to ensure a follow-up visit at our outpatient clinic within 14 days of discharge. A nurse called eligible patients within 48 business hours of discharge (making at least two contact attempts) to confirm the patient had discharge instructions and an accurate medication list, and to answer any questions about the discharge care plan. The RN also completed clinic prep work, such as pending labs and outpatient consults recommended by the discharging clinician. Finally, the nurse documented the phone call, sent it through the shared EHR to the patient's primary care clinician, and updated the appointment notes to indicate that the visit qualifies for TCM services.
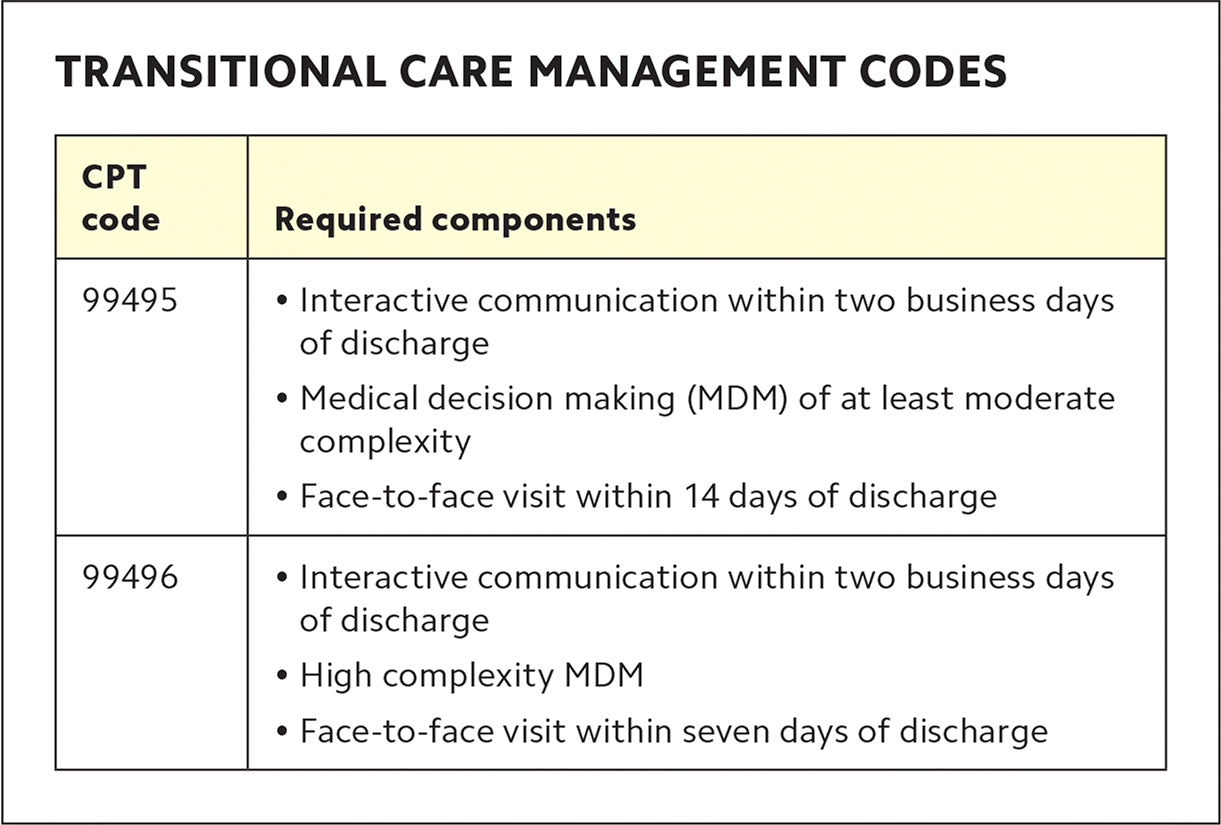
During the face-to-face visit, the primary care clinician reviewed the discharge summary (if an advanced practice provider or resident physician performed the visit, a staff physician was available, as needed). The clinician then coded the visit as either 99495 or 99496, depending on the complexity of the case and how soon the patient was seen (see “Transitional care management codes”). The administrative services coordinator and RN reviewed TCM visits to ensure the appropriate CPT code was used and sent a reminder through the EHR to the billing clinician to update the code, when indicated.
TRANSITIONAL CARE MANAGEMENT CODES
| CPT code | Required components |
|---|---|
| 99495 |
|
| 99496 |
|
Our clinic had the advantage of sharing an EHR with our affiliated hospital, which made it easier to spot patients eligible for TCM. In clinics that do not share an EHR or attending physician with their local hospitals, there are a few alternatives for identifying patients who qualify for TCM services. One would be to designate an RN to connect with a care coordinator at each hospital to obtain a daily discharge patient list. Another is to use the EHR to alert the RN when a patient schedules a visit that is categorized as “inpatient follow-up.” This would allow the RN to evaluate the patient for TCM eligibility.
FEWER ED VISITS
To gauge our workflow's effectiveness, we conducted a TCM study from Dec. 15, 2018, through Dec. 15, 2020. We divided the patient population between a control group without TCM services and an intervention group with TCM, ensuring there were no significant differences between the two groups in age, sex, LACE index (a validated measure of risk of readmission),6 and Charlson Comorbidity Index (a validated measure that predicts 10-year survival in patients based on age and comorbidities).7
During the two-year study period, the intervention group that received TCM had lower rates of emergency department visits, hospital readmissions, and mortality than the control group. The differences in readmissions and mortality were not statistically significant because our sample was small (e.g., one death in the 184-person intervention group and two deaths in the 273-person control group), but other studies have shown TCM reduces readmissions and mortality.8–10 The most significant difference in our study was in emergency department visits: 27.7% of patients in the intervention group had an emergency department visit within 30 days following discharge vs. 32.6% in the control group. This decrease is a boon to our institution, where the emergency department is consistently challenged with high patient volumes and long wait times. The difference in the emergency department visit rate was largest among patients with a Charlson Comorbidity Index score of 6 or greater (18.6% in the TCM group vs. 30.5% in the control group). This suggests that patients with higher rates of comorbidities may be more likely to benefit from TCM services.
FINANCIAL SUSTAINABILITY
In addition to improving patient outcomes and helping patients avoid readmissions and ED visits, TCM programs must be financially sustainable. We examined our program's sustainability by looking at the clinic's cost, relative value units (RVUs) produced, and the reimbursement rate. The cost was largely based on the time commitment of the designated RN (2.5 hours per week at $26 per hour) who coordinated the identification of patients and the other tasks outlined above. We determined that the face-to-face visits included in the TCM code generated an average of 2.5 RVUs per visit, compared with 1.56 RVUs per visit in the control group, for which visits were billed using standard evaluation and management codes (99213-99215). This generated an average reimbursement of $126 per visit for the TCM group versus $108 for the non-TCM group (based on the 2020 Medicare physician fee schedule).
This payment difference, coupled with a workflow that delegates much of the non-face-to-face TCM work to clinic staff, was enough to make TCM financially sustainable and even beneficial for our clinic. Our TCM intervention group received services at a clinic that is facility-based. In a non-facility-based clinic, the financial benefit could be greater because the reimbursement rate for TCM is higher in non-facility settings, to account for overhead expenses.
WORTH THE EFFORT
Many practices haven't embraced TCM because they're uncertain about the amount of effort involved and the clinical and financial benefits. Our clinic decreased emergency department visits with a TCM program, bolstering previous research that shows TCM can prevent adverse outcomes in patients' transitions from hospital to home while reducing health care costs. Using a team-based workflow that can be adapted to most primary care clinic settings, we have also shown a financial benefit to TCM, making our program effective and sustainable.

