Taking a cue from industries like aviation, physicians and care teams can use proven tools to keep patients from harm.

Next time you fly, pay attention to the flight crew's language. You might hear something like “Flight attendants, set doors to arrival, cross-check, and all call,” or “Ladies and gentlemen, we will be arriving at gate B-nine. That's Bravo-nine.” This is more than just industry jargon. It's a way to communicate quickly and clearly, in order to reduce errors.
According to the World Health Organization, people have about a one-in-300 chance of being harmed during health care (versus one-in-a-million traveling by plane).1 Examples of patient harm include dispensing the wrong medication, failing to recognize symptoms, or amputating the wrong limb. While the risks in outpatient medicine do not usually rise to the level of hospital care, there is still the potential for bad outcomes (e.g., prescribing an antibiotic that your patient is allergic to). In fact, it's been estimated that 6% of hospital stays are the direct result of an error in the ambulatory setting.2
KEY POINTS
- While errors are often more serious in hospital care, they can compromise patient safety in outpatient settings as well (e.g., prescribing an antibiotic your patient is allergic to).
- Clear communication between members of the health care team is critical to avoiding errors, and tools such as SBAR and BLUF can help.
- Situation awareness, cross-checking, and clinical huddles can help members of the care team work synergistically to prevent harmful errors.
Highly reliable organizations, in health care or other industries, have systems in place to prevent errors and often obsessively focus on error reduction (see “The five principles of high-reliability organizations”). The first step in implementing such systems in your practice is to develop a culture of safety and accountability in which physicians and teams talk openly about mistakes and identify ways to prevent them, a concept that has been addressed before in this journal.3 Once you've established that culture, this article can help you expand on it with specific team-based tools to improve safety.
THE FIVE PRINCIPLES OF HIGH-RELIABILITY ORGANIZATIONS
1. Preoccupation with failure.
2. Reluctance to simplify interpretations.
3. Sensitivity to operations.
4. Commitment to resilience.
5. Deference to expertise.
Source: Weick KE, Sutcliffe KM. Managing the Unexpected – Assuring High Performance in an Age of Complexity. Jossey-Bass; 2007.
Some errors can be prevented through technology and automation (e.g., an EHR that notifies physicians if they've prescribed something on the patient's allergy list). But preventing other errors requires the health care team to work together. Think of the following strategies like Swiss cheese: If we layer in enough safety interventions (i.e., cheese slices), then the holes in the cheese will be less likely to line up and allow errors to slip through (see “Swiss cheese safety model”).
For example, if I ask my medical assistant (MA), “Can you give the patient in Room 5 a tetanus vaccine?” there are several potential “holes.” It's a verbal order, so the MA may not have heard me clearly and understood what I meant. When I said “tetanus,” did I mean Tdap, Td, or DTaP? What if I really meant that I wanted Mrs. Jones in Room 4 to have a pneumonia vaccine, but I misspoke because I was thinking about Mr. Smith in Room 5 who asked me when his last tetanus shot was. Any one of these holes could cause an error, but if we “Swiss cheese” the visit by layering in enough of the following tools, we can greatly reduce the odds.
SWISS CHEESE SAFETY MODEL
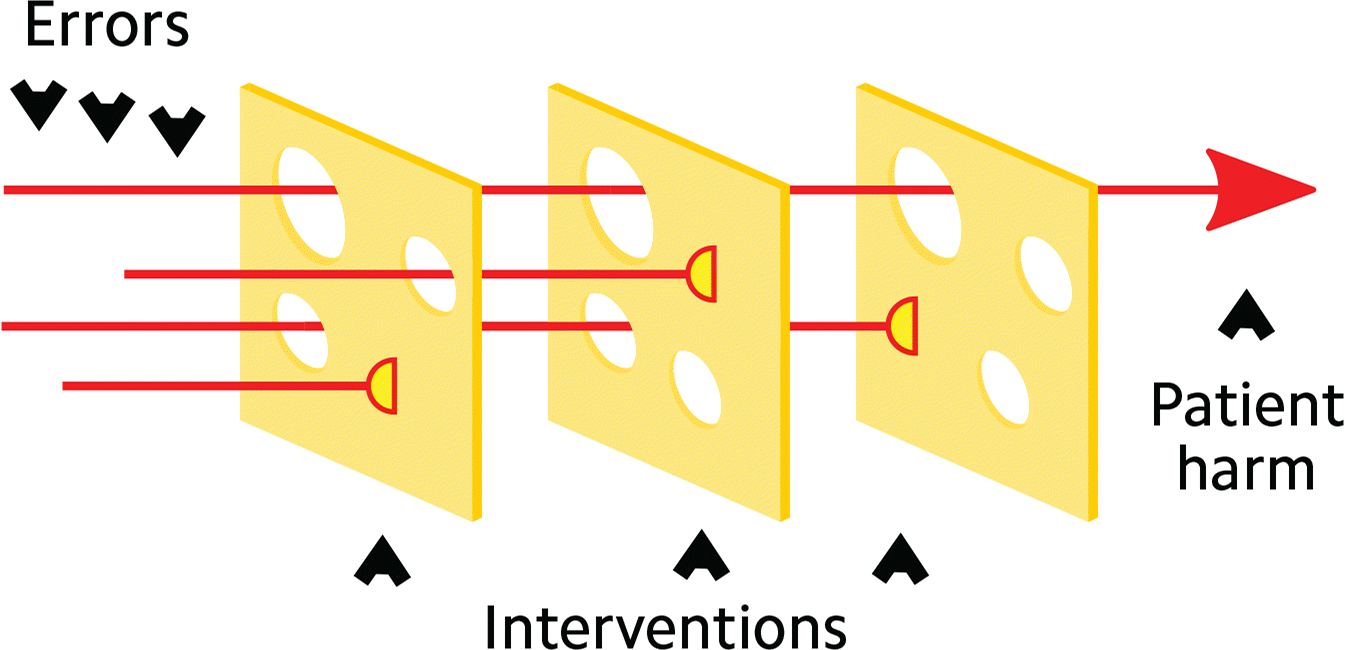
Each layer of intervention (or cheese slice) has its limitations (or holes). If the holes line up, an error can get through and reach the patient. But the more “slices” you add, the lesser the odds of harm.
Source: The “Swiss Cheese Model” of loss prevention. BenAveling. Used under CC-BY-SA-4.0. Text changed from original. https://commons.wikimedia.org/wiki/File:Swiss_cheese_model.svg
WRITTEN COMMUNICATION TOOLS
Since the early days of medical school, we've been trained in how to communicate with each other using a written medical record, usually in the form of a “SOAP” note (subjective, objective, assessment, and plan). But that structure might not be feasible for brief communications, non-discrete interactions, or phone messages that are often typed as the patient talks and read like a stream of consciousness.
Here's an example: Patient (Mrs. Jones) calling with some dizziness and headaches. Started sertraline last week. Wants to know if this is normal. Also has some fatigue and is sleeping all day. Has an appointment in three weeks and isn't sure if she needs to be seen sooner or if you can talk to her. Was seen last week and hasn't had a chance to see counselor yet.
It's hard to tell from the message what the patient really wants. Reassurance about the medication's side effects? An appointment to discuss them? Both?
Two tools can be useful in these situations.
SBAR (situation, background, assessment, recommendation/request). Using SBAR,4 the message becomes separated into an actionable component and a background component. The “situation” field summarizes the call, prompting the recipient for the “background” to come. This is followed by an “assessment” that prompts the recipient for the “recommendation/request,” which is the action item. This format allows recipients to focus on the most important part of the message (the request or recommendation) and track back to read more about what's going on (the background) if necessary.
Let's look at how SBAR transforms the message above:
S: Patient having side effects.
B: Mrs. Jones called today. She saw you in the office last week and was started on sertraline. She's having dizziness, headaches, and fatigue. She is unsure if this is normal and is concerned. She has an appointment in three weeks but doesn't know if she should be seen sooner or if you could call her. She hasn't yet gone to her counselor.
A: Mrs. Jones is having side effects to her new medication and wants to discuss them with you.
R: Do you want to schedule an appointment with Mrs. Jones to talk about her side effects? If not, what message can I give her about her symptoms?
BLUF (bottom line up front). This technique, designed for speed and clarity, is a preferred communication tool in the military. It is especially useful for patient hand-offs, when a concise “executive summary” conveys critical information, followed by supporting background information.5 Here's an example of a BLUF message I might send to a colleague who's on call:
Bottom line: Mr. Smith is on the way to the emergency department for dyspnea and weight gain, and he will likely need to be admitted for a heart failure exacerbation.
Background: I got a phone call earlier today from Mr. Smith. He has a history of heart failure with reduced ejection fraction and has been having increased shortness of breath this week. He has been taking extra doses of furosemide per our treatment plan, but it's not helping. Today he reported another three pounds of weight gain overnight, for a total of seven pounds this week. I instructed him to go to the hospital, and his wife is going to drive him there. His cardiologist is Dr. Hart, but the patient hasn't seen her in months. Aside from furosemide, the patient is on sacubitril/valsartan, dapagliflozin, and carvedilol. His echocardiogram from nine months ago showed an ejection fraction of 30%.
Using the SBAR and BLUF techniques can help you make your written communication as clear and concise as possible. Additionally, it's best to keep medical abbreviations to a minimum, and eliminate them altogether when it comes to medications.6,7
VERBAL COMMUNICATION TOOLS
While verbal orders are generally discouraged because of the risk of error,8 not all communication in an office can be written. For example, if a patient needs an urgent electrocardiogram (ECG), it would be appropriate to say that directly to your MA, rather than enter it in the EHR and wait for the MA to see it.
Here are two tools for safer verbal communication.
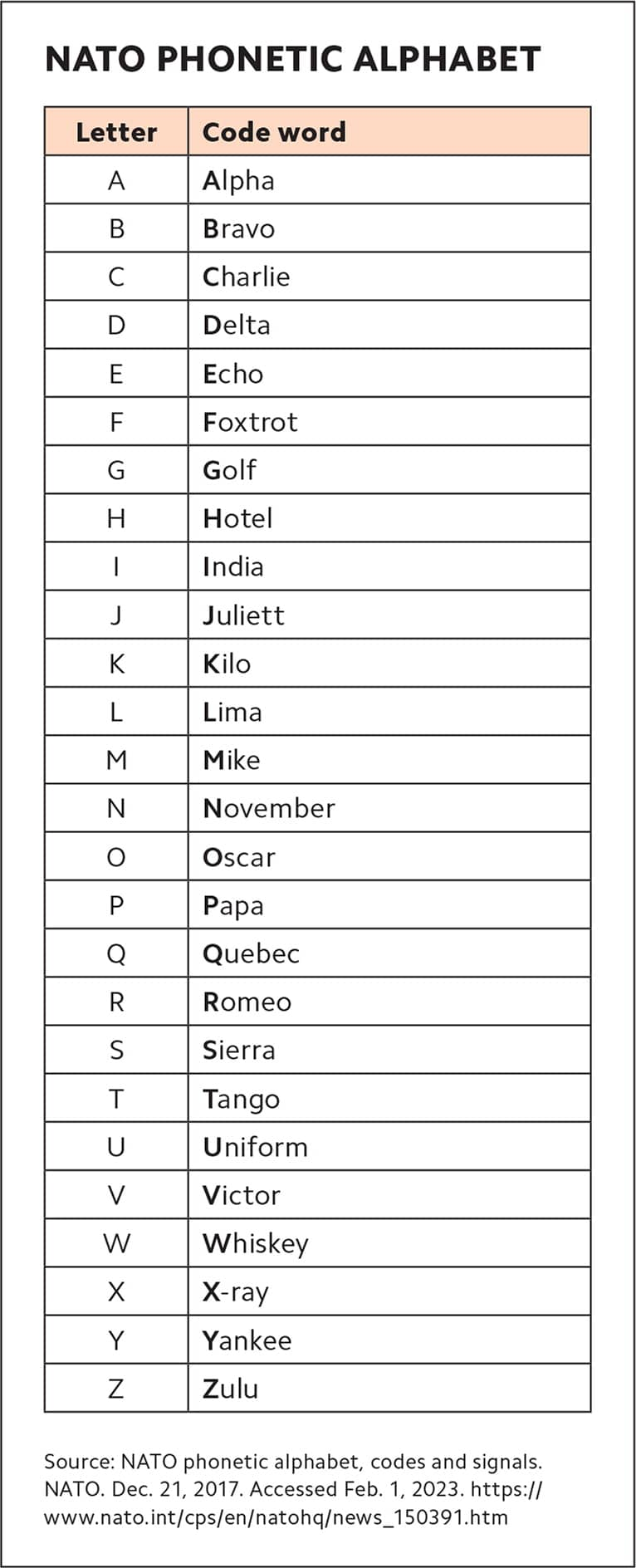
Phonetic alphabet. The phonetic alphabet allows clear communication of letters using a series of standardized code words for which the first letter is easily recognizable (see “NATO phonetic alphabet”). For example, the other day I was discussing a patient with one of my advanced practice providers (APP) and suggested she order a BNP (B-type natriuretic peptide). Because that sounds very similar to BMP (basic metabolic panel), and I wanted to make sure there was no confusion, I told the APP, “I think you should order a BNP. That's Bravo-November-Papa.”
| Letter | Code word |
|---|---|
| A | Alpha |
| B | Bravo |
| C | Charlie |
| D | Delta |
| E | Echo |
| F | Foxtrot |
| G | Golf |
| H | Hotel |
| I | India |
| J | Juliett |
| K | Kilo |
| L | Lima |
| M | Mike |
| N | November |
| O | Oscar |
| P | Papa |
| Q | Quebec |
| R | Romeo |
| S | Sierra |
| T | Tango |
| U | Uniform |
| V | Victor |
| W | Whiskey |
| X | X-ray |
| Y | Yankee |
| Z | Zulu |
Check-back. Check-back is a technique to quickly verify that information has been communicated accurately. It involves repeating back a verbal order in a “sender-receiver-sender” pattern. The sender gives a verbal order, the receiver repeats back the order, and the sender verifies the repeat-back. Here's an example:
Physician: “The patient in Room 6, Ms. Jones, needs a vision screening. Can you do that please?”
Medical assistant: “Ms. Jones, who is in Room 6, needs a vision screen. Correct?”
Physician: “Yes, that's correct. Thank you.”
TEAM-BASED COMMUNICATION TOOLS
For optimal patient safety, the whole health care team must be on the same page. Here are three tools to ensure that happens.
Situation awareness. Situation awareness (SA) is the overlap of your perception of reality and what that means for the immediate future.9 It's the ability to “read the room” and understand what next steps are needed. Team-based SA is a synergistic application of that. Examples would be a receptionist noticing a patient having difficulty getting out of his car and going to assist him, an MA observing an irregular pulse and getting the ECG ready, or a physician noticing a patient is visibly short of breath walking down the hall and immediately going to the exam room to check on the patient. By emphasizing SA, highly reliable organizations foster teams that are sensitive to potential hazards throughout the operation.
Cross-check. A cross-check is when a colleague verifies and supports a team member's actions or suggests a change based on the information presented. It might be spontaneous, spurred by SA (“I noticed you are getting ready to do an ECG, but you left the box of electrodes in the other room”) or collaborative (“Can you take a look at this set of labs Dr. Smith ordered? The patient says she is supposed to get a thyroid test, but I don't see it listed.”) The CHARMED study showed that emergency department physicians who cross-checked each other's patients significantly reduced adverse events.10 In primary care, cross-checking could be two physicians discussing a patient's condition and care plan, an APP collaborating with a physician, or a resident presenting a case.
Clinical huddles. A clinical huddle is essentially a brief work stoppage where all team members come together to discuss a topic. It could be a daily clinical huddle in which everyone stops and focuses on the day's upcoming patients. Or it could be an impromptu huddle to discuss a particular patient during the workday. In either case, it's an opportunity for a team to focus on a topic in a structured manner. Communication during the huddle should be clear, concise, and limited to the matter at hand. Side topics or conversations should be saved for other times. Safety-related items to discuss in a huddle include the following:
- Sound-alike patient names (“We have two patients this afternoon with the same last name, so be careful calling them back from the lobby”),
- Equipment issues (“The ECG stopped working this morning, but we have a replacement coming this afternoon”),
- Patient-specific topics (“Remember, Mr. Jones has difficulty walking, so let's be sure to give him some help”),
- Staffing issues (“Dr. Smith will be leaving at 3 p.m. today”).
TAKING SMALL STEPS FORWARD
Many of the tools discussed here can be found on the Agency for Healthcare Research and Quality's TeamSTEPPS website, free of charge.11 There are also proprietary tools available from other organizations for a fee, and many health systems have safety training available to members of the medical staff. Like all primary care transformation, the key is to establish a culture of change and then make small, iterative reforms. I recommend the Plan-Do-Study-Act cycle for doing this.12 Using safety tools in primary care will not only help ensure safer patient outcomes but also can help drive quality improvement.

