These principles can help keep your patients' problem lists well-curated and useful.

If you have an electronic health record (EHR), you are familiar with the problem list — the list of conditions that have been associated with each patient at some point in time. At its best, the problem list gives a quick and easy-to-understand summary of the patient. If it's not up to date, however, the problem list can become so unwieldy it's not useful or, worse, it's deceptive.
Keeping problem lists orderly is more complicated if you work for a large organization with multiple specialties that share the lists. It requires the entire team; but as primary care physicians (PCPs) and “captains of the ship,” we often have ultimate control over — and therefore responsibility for — the list.
There is no single way to organize a problem list, and no national consensus about it in the U.S., although there is in some other countries.1 Therefore, in many organizations, the problem list is a catch-all for capturing visit problems, symptoms, past medical history, family history, allergies, etc. In this article, we focus on using the problem list for only chronic conditions and recurrent acute problems considered important for patient care, and we present some principles to help you organize your lists.
KEY POINTS
- The problem list can provide a useful snapshot of a patient's current health needs, but only if it's up-to-date and complete.
- Problems that are no longer active but still affect treatment can be given a “History of” designation and stay on the list. Problems that no longer affect treatment should be removed.
- Because family physicians are responsible for the ongoing care of the patient, curating the problem list often falls to us, but it should be a team effort.
WHAT A PROBLEM LIST SHOULD BE
The problem list is a shortcut to understanding the patient. It should be a quick, useful reference describing who the patient is medically. To remain useful, the problem list must be a “living document” that changes as the patient's condition changes. Problem lists should only include active problems and issues relevant to present and future care. This requires removing problems that are no longer relevant and adding newly diagnosed chronic conditions.
In most EHRs, the problem list is used for clinical decision support. For example, if diabetes and chronic obstructive pulmonary disease are on the problem list, the EHR may remind the clinician to order a microalbumin or a pneumonia vaccination. If some entries on the list are inaccurate or obsolete, it becomes harder to zero in on what the patient really needs.
When a condition is no longer active but affects the future management of a patient, a PCP can keep it on the list but give it a “History of” designation. For example, a patient diagnosed with deep vein thrombosis (DVT) gets “DVT” on their problem list. When DVT is no longer present but the patient is continuing on anticoagulants, the diagnosis changes to “History of DVT” and stays on the problem list because of the importance of anticoagulation management. The same is true for gastrointestinal (GI) bleeding. Once resolved, the problem becomes “History of GI bleed” and remains on the problem list because of its implications for medication selection. If a patient is on a medication for a specific condition, that condition should remain on the problem list as well, but giving it a “History of” designation helps quickly differentiate it from active problems. This is different than “resolving” a problem, which removes it from the problem list entirely.
Significant elements of the patient's family history may appear on the problem list, but only if they inform current treatment or screening. For example, “Family history of Lynch Syndrome” is pertinent until the patient has had a normal colonoscopy, and then it can probably be relegated to the family history list. On the other hand, “Family history of skin cancer” is not needed on the problem list after the patient has been diagnosed with skin cancer, because “Skin cancer” itself will be added to the list. At that point, the family history is not going to change the treatment plan.
The problem list is not the same as the visit problems — though most EHRs allow the visit problems to be selected from the problem list. If the words “acute” or “encounter for” are part of the diagnosis, it rarely goes on the problem list. The problem list is also not the place for past medical history or past surgical history, which have other places in the chart. It is sometimes appropriate to include pieces of those lists if they're needed to shape future diagnosis or treatment, however. For example, some PCPs would allow “History of bilateral mastectomy” to remain on the problem list to explain the lack of need for a mammogram, while others would look on the surgical history if they needed that information. On the other hand, “History of appendectomy” should probably stay on the surgical history list. The best guideline is if it influences current treatment, it should appear somewhere on the problem list.
While there aren't always hard-and-fast rules, the “stoplight” tool provides more examples of what should and shouldn't be on the problem list.
PROBLEM LIST STOPLIGHT
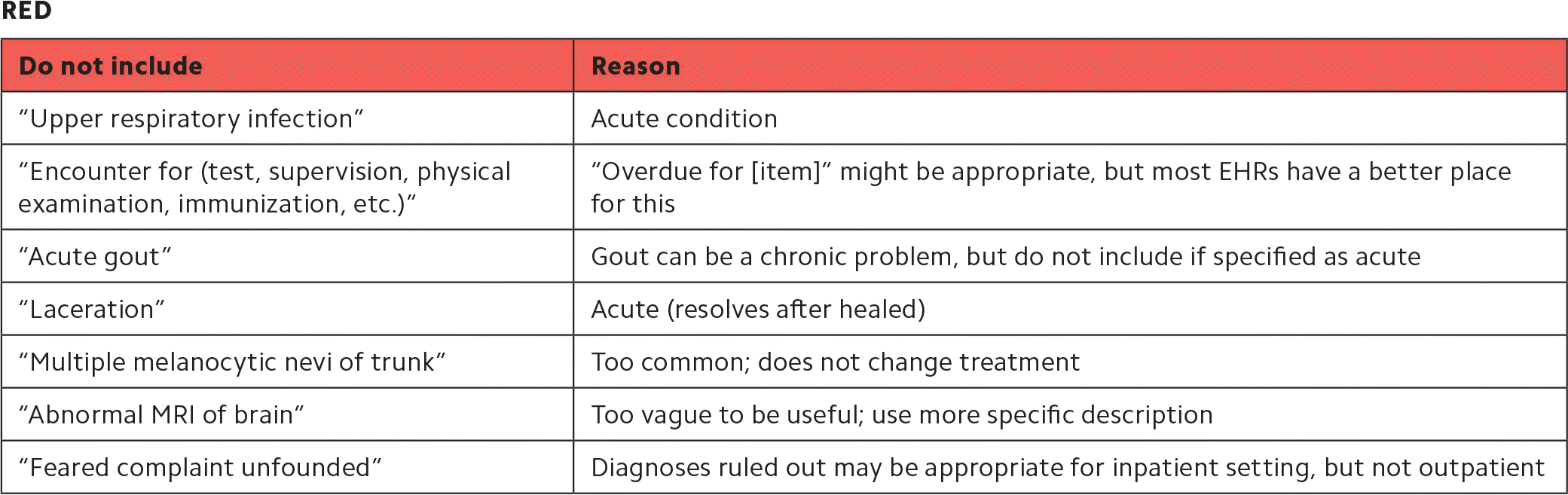
| Do not include | Reason |
| “Upper respiratory infection” | Acute condition |
| “Encounter for (test, supervision, physical examination, immunization, etc.)” | “Overdue for [item]” might be appropriate, but most EHRs have a better place for this |
| “Acute gout” | Gout can be a chronic problem, but do not include if specified as acute |
| “Laceration” | Acute (resolves after healed) |
| “Multiple melanocytic nevi of trunk” | Too common; does not change treatment |
| “Abnormal MRI of brain” | Too vague to be useful; use more specific description |
| “Feared complaint unfounded” | Diagnoses ruled out may be appropriate for inpatient setting, but not outpatient |
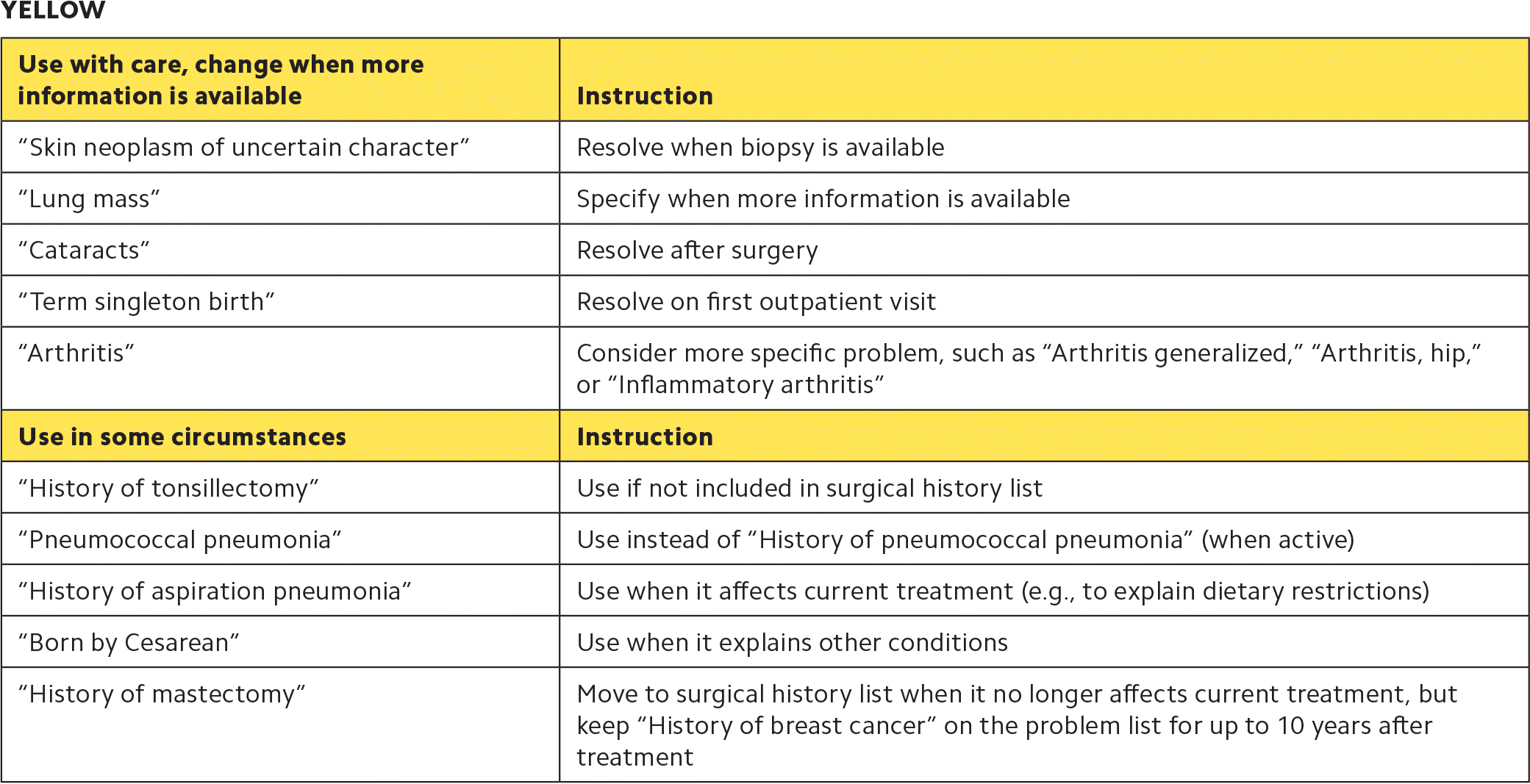
| Use with care, change when more information is available | Instruction |
| “Skin neoplasm of uncertain character” | Resolve when biopsy is available |
| “Lung mass” | Specify when more information is available |
| “Cataracts” | Resolve after surgery |
| “Term singleton birth” | Resolve on first outpatient visit |
| “Arthritis” | Consider more specific problem, such as “Arthritis generalized,” “Arthritis, hip,” or “Inflammatory arthritis” |
| Use in some circumstances | Instruction |
| “History of tonsillectomy” | Use if not included in surgical history list |
| “Pneumococcal pneumonia” | Use instead of “History of pneumococcal pneumonia” (when active) |
| “History of aspiration pneumonia” | Use when it affects current treatment (e.g., to explain dietary restrictions) |
| “Born by Cesarean” | Use when it explains other conditions |
| “History of mastectomy” | Move to surgical history list when it no longer affects current treatment, but keep “History of breast cancer” on the problem list for up to 10 years after treatment |

| Use in most circumstances | Reason |
| “Adenocarcinoma of lung, stage 3” | Use while undergoing treatment, then change to “History of lung cancer” when treatment and surveillance complete |
| “History of gastric bypass” | Requires ongoing surveillance |
| “Blindness” | Important to know for all those caring for patient |
| “Gout” (chronic or recurrent) | Affects treatment choices |
| “Presence of pacemaker / ICD” | Affects treatment choices |
| “Low literacy” | May alter the way information is given |
THE WELL-CURATED PROBLEM LIST
The problem list loses its usefulness if it gets unwieldy. Therefore, best practice is to keep the list current, accurate, precise, clear, and concise.
Current: Leaving old or resolved problems on the list is confusing and can lead to inappropriate care. For example, active breast cancer requires different attention than breast cancer that has been in remission for 10 years.
Accurate: If the A1C is greater than 7%, diabetes should be on the problem list, but it is often omitted.2 If the A1C later falls out of diabetic range (due to lifestyle changes, medications, etc.), the diabetes diagnosis should stay on the list for a while with a “History of” designation so the PCP knows to check for recurrence. (When hyperglycemia is not caused by diabetes but by steroids, then the problem is temporary and can be removed from the list when no longer active.)
Patients with chest pain should not have “Heart disease” placed on their problem list if it has not been confirmed. Instead, the problem list should simply say “Chest pain” until the cause is determined. If heart disease is ruled out, don't add “Suspected heart disease, ruled out,” which can create confusion. (Inpatient charts can have rule-out diagnoses, but outpatient charts generally should focus on the related signs and symptoms until the diagnosis is confirmed.3) Similarly, a visit diagnosis of “Screening tests for hyperlipidemia” should not result in a problem list entry of high cholesterol unless the report indicates it.
Precise: Be as precise as possible when listing the problem. “Heart failure with reduced ejection fraction” and “Systolic heart failure” are more precise and helpful than “Congestive heart failure, unspecified.” “Recurrent cystitis” is different than “Recurrent pyelonephritis,” and neither should be recorded on the list as “Recurrent urinary tract infection.”
Clear: Even precise diagnoses can be misleading. We recently saw a patient whose colostomy was recorded as a “colo-cutaneous fistula” — not entirely wrong, but it creates confusion because it fails to distinguish between a pathologic condition and a therapeutic one. This underscores the need to be clear as well as precise.
Most patient portals allow patients to view and comment on the problem list. Therefore, avoid medical jargon that may interfere with the patient's understanding of their status. Avoid using stigmatizing language on the problem list as well, while maintaining precision. For example, instead of “morbid obesity,” consider listing the patient's body mass index range (e.g., “BMI 40–45”), which is also more precise.
Concise: The problem list should contain everything that is needed and nothing more. Duplicating problems already entered and adding inconsequential items obscures the meaning and power of the remaining problems. (See “Duplication examples.”)
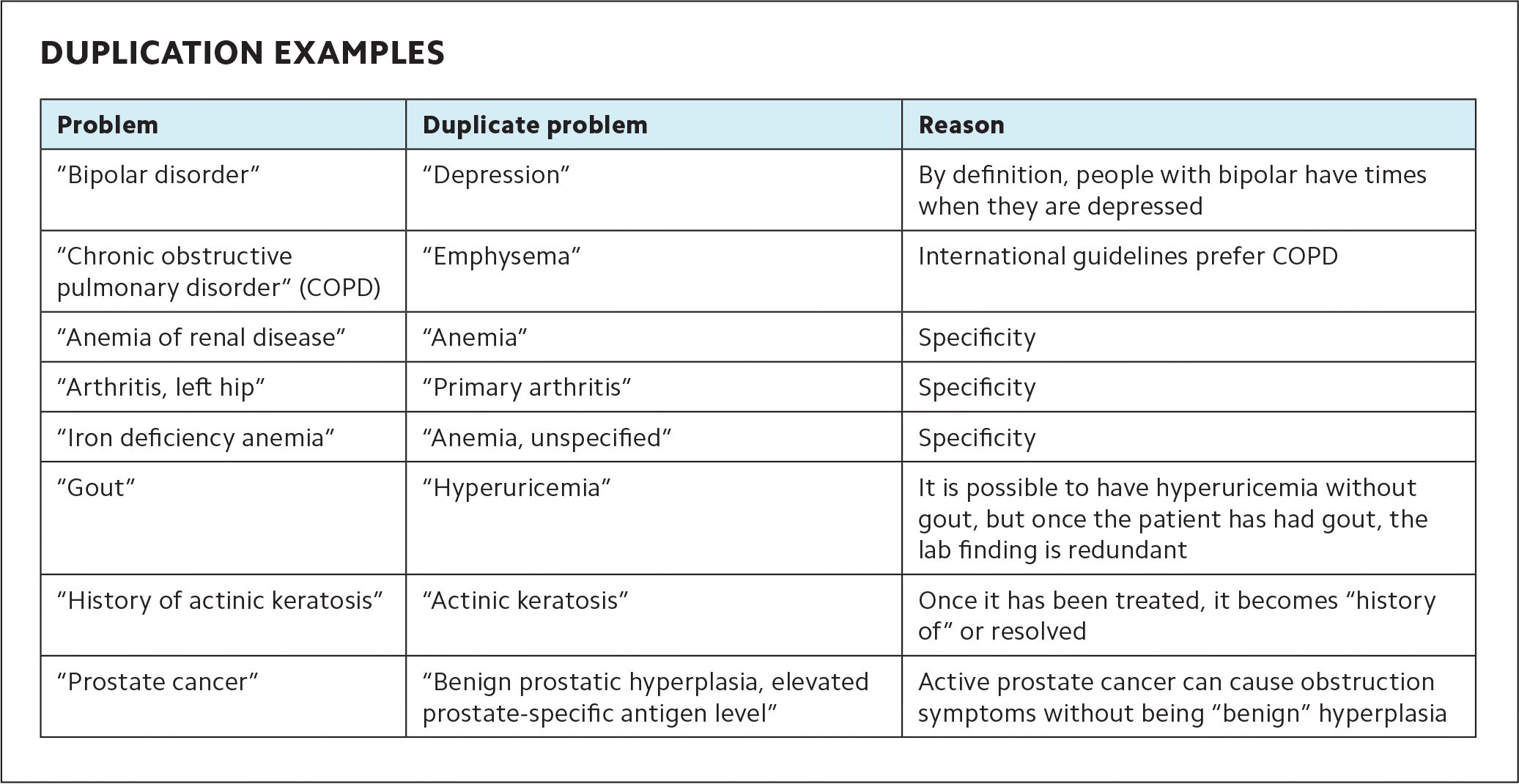
| Problem | Duplicate problem | Reason |
|---|---|---|
| “Bipolar disorder” | “Depression” | By definition, people with bipolar have times when they are depressed |
| “Chronic obstructive pulmonary disorder” (COPD) | “Emphysema” | International guidelines prefer COPD |
| “Anemia of renal disease” | “Anemia” | Specificity |
| “Arthritis, left hip” | “Primary arthritis” | Specificity |
| “Iron deficiency anemia” | “Anemia, unspecified” | Specificity |
| “Gout” | “Hyperuricemia” | It is possible to have hyperuricemia without gout, but once the patient has had gout, the lab finding is redundant |
| “History of actinic keratosis” | “Actinic keratosis” | Once it has been treated, it becomes “history of” or resolved |
| “Prostate cancer” | “Benign prostatic hyperplasia, elevated prostate-specific antigen level” | Active prostate cancer can cause obstruction symptoms without being “benign” hyperplasia |
CURATING THE PROBLEM LIST: A TEAM EFFORT
Because family physicians are responsible for the ongoing care of the patient, curating the problem list often falls to us. However, it should be a team effort. Office or health system policies often govern who is able to add to, resolve, or modify the problem list. In some systems, only clinicians can do so; in others, it is open to nurses, social workers, physical therapists, etc. The problem list should facilitate communication among all users of the chart; if multiple specialties use the same EHR, they should be using and updating the same problem list.
For example, a family physician sees a patient with shoulder pain and adds “Chronic left shoulder pain” to the problem list because only that level of specificity is known at the time. The family physician refers the patient to an orthopedist for further evaluation. Based on the findings, the orthopedist is then responsible for changing that entry to “Partial supraspinatus tear, left shoulder.”
This is ideally how the problem list should function within the medical team. In organizations that adopt a team-based approach, not only does it make the problem list more accurate and useful, but it also saves family physicians considerable time.

