Careful examination of the neonate at delivery can detect anomalies, birth injuries, and disorders that may compromise successful adaptation to extrauterine life. A newborn with one anatomic malformation should be evaluated for associated anomalies. If a newborn is found to have an abdominal wall defect, management includes the application of a warm, moist, and sterile dressing over the defect, decompression of the gastrointestinal tract, aggressive fluid resuscitation, antibiotic therapy, and prompt surgical consultation. Hydroceles are managed conservatively, but inguinal hernias require surgical repair. A newborn with developmental hip dysplasia should be evaluated by an orthopedist, and treatment may require use of a Pavlik harness. The presence of ambiguous genitalia is a medical emergency, and pituitary and adrenal integrity must be established. Early diagnosis of spinal lesions is imperative because surgical correction can prevent irreversible neurologic damage.
The newborn examination facilitates the early identification of anomalies and health problems that require immediate intervention. A careful examination is also appropriate after a newborn has completed the transition from fetal to neonatal life. If one anatomic malformation is found, the newborn should be evaluated for associated anomalies. Part II of this two-part article reviews anomalies and disorders of the abdomen, pelvis, extremities, genitalia, and spine.
Abdomen
A scaphoid abdomen suggests the presence of a diaphragmatic hernia. In newborns with abdominal distension, it is important to determine whether the condition is secondary to excess air inside or outside the bowel, fluid in the peritoneal cavity, an enlarged viscus, or a tumor in the abdomen (Table 1).1 A general approach to newborns who have an abdominal mass is provided in Figure 1,2 and approaches to newborns who have hepatomegaly with or without hyperbilirubinemia are presented in Figure 2.3
TABLE 1 Differential Diagnosis of Abdominal Masses in Newborns
| Renal masses: hydronephrosis (ureteropelvic junction obstruction, posterior urethral valves, vesicoureteric reflux), cystic disease of the kidneys (multicystic dysplastic kidneys, polycystic kidneys), renal vein thrombosis, tumors (Wilms' tumor, mesoblastic nephroma) |
| Gastrointestinal masses: duplication cyst, complicated meconium ileus (intraperitoneal meconium cyst), mesenteric or omental cyst, hypertrophic pyloric stenosis |
| Nonrenal retroperitoneal masses: adrenal hemorrhage, tumors (neuroblastoma, teratoma, rhabdomyosarcoma, sacrococcygeal teratoma) |
| Genital masses: hydrometrocolpos, ovarian mass (simple cyst, torsion, teratoma) |
| Hepatobiliary masses: infections (viruses, bacteria), lysosomal storage diseases (glycogen storage diseases), congestive heart failure, tumors (hepatoblastoma), choledochal cyst, hemolytic anemias |
| Splenomegaly: infections (viruses, spirochetes), congenital hemolytic anemias (hereditary spherocytosis, thalassemia, hemoglobinopathies), storage disorders (Gaucher's disease, Niemann-Pick disease), mucopolysaccharide disorders (Hurler's syndrome) |
Adapted with permission from Disease based on age: etiology of neonates (birth to 1 month). In: Kao SC, ed. Pediatric abdominal mass imaging: imaging a child with an abdominal mass. Retrieved October 2001, from:http://www.vh.org/Providers/TeachingFiles/PedAbdomMassImaging/KaosMenu.html.
FIGURE 1. Newborn with Abdominal Mass

Suggested approach to the diagnosis of abdominal masses in newborns. (US = ultrasonography; CT = computed tomographic; MRI = magnetic resonance imaging)
Adapted with permission from Korones SB. Abdominal masses. In: Korones SB, Bada-Ellzey HS, eds. Neonatal decision making. St. Louis: Mosby-Year Book, 1993:90–1.
FIGURE 2. Newborn with Hepatomegaly
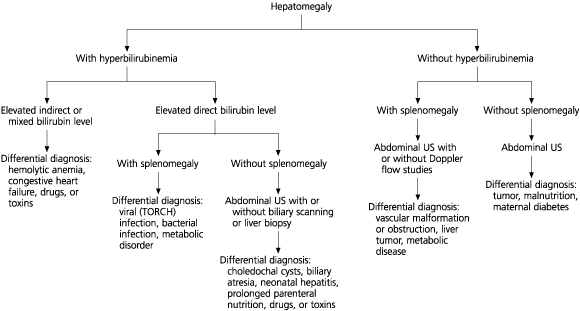
Suggested approach to the evaluation of newborns who have hepatomegaly with or without hyperbilirubinemia (US = ultrasonography; TORCH =toxoplasmosis, other viruses, rubella, cytomegaloviruses, herpes [simplex] viruses).
Adapted with permission from Wolf AD, Lavine JE. Hepatomegaly in neonates and children. Pediatr Rev 2000;21:303–10.
The umbilicus should be inspected for signs of bleeding, infection, granuloma, or abnormal communication with the intra-abdominal organs. A single umbilical artery is present in 0.2 to 1 percent of newborns4 and may be associated with asymptomatic renal anomalies in 7 percent of these infants.5
Abdominal wall defects, including gastroschisis and omphalocele, are usually diagnosed prenatally. Features and management of these defects are summarized in Table 2.6,7
Anal patency is assessed by inspection or by probing with a small finger. Anterior displacement of the anus should be noted.
TABLE 2 Omphalocele and Gastroschisis in Newborns
| Omphalocele |
| Clinical features: defect covered by amnion, with cord attachment to apex of defect; prematurity and intrauterine growth retardation less common than in gastroschisis |
| Herniation through defect: any abdominal organ, but usually the large or small intestine, liver, stomach, gall bladder, urinary bladder, pancreas, spleen, or internal genitalia |
| Associated anomalies in 67% of affected newborns: trisomy 13, 18, or 21 syndrome, congenital heart disease (15% to 25%), gastrointestinal anomalies (midgut volvulus, Meckel's diverticulum, intestinal atresia and duplication, imperforate anus, colonic agenesis), and neurologic and renal anomalies (20%) |
| Overall mortality: ∼30%, related to the presence of major structural and chromosomal anomalies, and to intractable respiratory insufficiency in some newborns with large omphaloceles; with no associated anomalies, minimal mortality |
| Gastroschisis |
| Clinical features: no sac covering the defect; defect in abdominal wall positioned to right of umbilicus; cord attachment to abdominal wall to left of defect; prematurity and intrauterine growth retardation more common than in omphalocele |
| Herniation through defect: usually limited to small intestine and ascending colon, with thickened and matted appearance of intestine |
| Associated anomalies: primarily intestinal atresia |
| Overall mortality: ∼10%, mostly from complications of prematurity and intestinal complications such as severe short gut syndrome |
| Management of defects |
| General measures for initial stabilization and evaluation: application of warm, fluid-impermeable dressing over defect; placement of orogastric tube to decompress stomach and prevent further distension; aggressive fluid resuscitation to compensate for ongoing fluid losses from exposed viscera; blood culture followed by broad-spectrum antibiotic (ampicillin or gentamicin [Garamycin]) |
| Immediate consultation with pediatric surgeon |
Information from Nakayama DK. Omphalocele. In: Nakayama DK, Bose CL, Chescheir NC, Valley RD, eds. Critical care of the surgical newborn. Armonk, N.Y.: Futura, 1997:277–88, and Nakayama DK. Gastroschisis. In: DK, Bose CL, Chescheir NC, Valley RD, eds. Critical care of the surgical newborn. Armonk, N.Y.: Futura, 1997:261–76.
Pelvis and Extremities
Excessive traction of the spinal nerve roots C5-T3 results in brachial plexus injury (Table 3).8,9 Treatment, directed at preventing contractures, involves partial immobilization of the affected arm for one to two weeks, followed by active physiotherapy.8
TABLE 3 Brachial Plexus Injury in Newborns*
| Erb-Duchenne palsy |
| Incidence: most common brachial nerve injury involving spinal nerve roots C5–7 |
| Clinical features: arm adducted and internally rotated, with elbow extension, pronation of arm, flexion of wrist, and intact grasp reflex; “waiter's tip” position if spinal nerve root C7 is involved |
| Klumpke's palsy |
| Incidence: rare (<1% of brachial plexus injuries); involves spinal nerve roots C8-T1 |
| Clinical features: hand paralyzed, with no voluntary movements of wrist and an absence of grasp reflex |
| Paralysis of entire arm |
| Incidence: more common than Klumpke's paralysis |
| Clinical features: entire arm paralyzed and flaccid, with absence of all reflexes |
*—The reported incidence of brachial plexus injury ranges from fewer than one case to four cases per 1,000 term births.9
Information from Mangurten HH. Birth injuries. In: Fanaroff AA, Martin RJ, eds. Neonatal-perinatal medicine: diseases of the fetus and infant. 6th ed. St. Louis: Mosby-Year Book, 1997:425–54.
Developmental hip dysplasia may be unilateral or bilateral and includes subluxated or dislocated hips and malformed acetabula. Soft tissue hip clicks may be confused with Ortolani and Barlow clunks. According to guidelines established by the American Academy of Pediatrics,10 an examination that is positive for developmental hip dysplasia should lead to an orthopedic referral. If the results are inconclusive, the examination should be repeated in two weeks. If the follow-up examination is positive or inconclusive, orthopedic referral is indicated. Although triple diapering is common, no data on its effectiveness are available, and use of this measure may delay initiation of appropriate treatment (e.g., Pavlik harness).10
Metatarsus adductus is identified by the C curve of the lateral border of the foot11 (Figure 3). This defect is commonly associated with a fixed intrauterine position and may be associated with developmental hip dysplasia. When the defect is marked and relatively rigid, it cannot be distinguished from talipes equinovarus, a condition characterized by adduction or inversion of the forefoot, inversion at the ankle, and equinus posturing (toes down, heel up, and malrotation of the calcaneus). Referral to an orthopedist is indicated.
FIGURE 3.
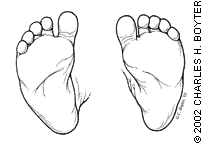
Plantar view of bilateral metatarsus adductus, showing rounding of the lateral border of the feet.
Supernumerary digits occur more often in black infants. This anomaly tends to be hereditary and is frequently lateral to the fifth digit on the hands or feet. The extra digits may have a nail and are attached by a small pedicle, which differentiates the defect from true polydactyly. If bony tissue is not palpable, the application of a ligature around the pedicle allows the digit to fall off.
True polydactyly more commonly occurs on the feet and may be present with malformation syndromes. Syndactyly may involve soft tissue (simple synostosis) or fusion of bone (complex synostosis). Radiographs are necessary to determine the degree of fusion, and affected newborns should be referred to an orthopedic surgeon.
Genitalia
An abnormally small penis (normal values in term newborns: 3.5 ± 0.7 cm in length and 1.1 ± 0.2 cm in diameter) indicates reduced androgen effect or reduced growth hormone action during the second and third trimesters.
Hypospadias (proximally displaced urethral meatus) can vary from a mild glanular form to a more severe perineal form. Chordee (ventral curvature of the penis) without hypospadias occurs less frequently and may be due to skin tethering or a short urethra. Circumcision should be delayed in these newborns. Other anomalies associated with hypospadias include cryptorchidism and inguinal hernia, which are more likely to occur with proximal hypospadias.
The clinical features and management of inguinal hernia and hydrocele are described in Table 4.12,13
TABLE 4 Inguinal Hernia and Hydrocele in Newborns
| Inguinal hernia |
| Incidence: term newborns, 0.5% to 1%; premature newborns, 5% to 10%; location on right side (∼60%), left side (40%), or both sides (10%), with bilateral hernias more common in premature newborns (∼62% of affected infants) |
| Clinical features: soft, nontender, reducible bulge in the inguinal canal, off the midline, especially at times of increased intra-abdominal pressure, with possible extension into scrotum; when incarcerated, tenderness and tenseness of hernia, with discoloration of overlying skin |
| Complications: incarceration and strangulation |
| Treatment: elective surgical repair as soon as possible after diagnosis13 |
| Hydrocele |
| Clinical features: painless, tense, fluctuant scrotal mass that transilluminates; upper border usually movable away from inguinal canal; possibly, testis not palpable |
| Treatment: none usually needed, because hydroceles generally decrease in size and resolve over the first year of life; if not resolved by the age of 1 to 2 years, consideration of elective surgical repair; for communicating hydrocele (i.e., one that fluctuates in size), same treatment as for inguinal hernia |
Information from Nakayama DK. Inguinal hernia and hydrocele. In: Nakayama DK, Bose CL, Chescheir NC, Valley RD, eds. Critical care of the surgical newborn. Armonk, N.Y.: Futura, 1997:289–303.
If a testis is not palpable, it is important to determine if it is retractile, ectopic, or cryptorchid. Cryptorchidism can be unilateral (66 percent of cases) or bilateral (10 percent of cases).14 Cryptorchidism occurs in 2.7 to 5.9 percent of term newborns, but its incidence is 10 times higher in premature infants.14 The scrotum of a neonate with undescended testis is often underdeveloped. The management of infants with this anomaly is described in Figure 4.15
In female newborns, the clitoris can have a relatively prominent appearance, especially if the labia are underdeveloped or the infant is premature. Clitoromegaly may be a sign of masculinization or a virilizing tumor. It may also be caused by increased maternal androgen production or maternal drug use.
Withdrawal of maternal hormones in normal newborns may cause a milky, sometimes bloody secretion from the vagina. The secretion may persist for several days but requires no treatment.
The presence of ambiguous genitalia is a medical emergency. Adrenal and pituitary integrity must be established.
Spine
Malformations affecting the spine are often diagnosed prenatally or are apparent in the delivery room. These defects require neurosurgical intervention. Occult lesions of the spine may be subtle and asymptomatic at birth. Early diagnosis is imperative because surgical correction can prevent irreversible neurologic damage. When neurologic signs or symptoms become apparent, most are irreversible (Table 5).16
TABLE 5 Neurologic Impairment in Newborns
| Causes: ischemia (intrapartum or postnatal), cerebral birth trauma (including intracranial hemorrhages), congenital malformations, sepsis or meningitis, prenatal infections, neuromuscular disorders, maternal medications, metabolic disorders, degenerative diseases |
| Clinical features of neurologic impairment in newborns: hypotonia (less frequently, hypertonia), weakness (decreased strength), asymmetry of muscle tone and/or movement, alterations in level of consciousness, seizures, single or multiple cranial nerve involvement, fasciculations |
Adapted with permission from Vannucci RC, Yager JY. Newborn neurologic assessment. In: Fanaroff AA, Martin RJ, eds. Neonatal-perinatal medicine: diseases of the fetus and infant. 6th ed. St. Louis: Mosby-Year Book, 1997:812–26.
Overlying cutaneous markers are found in 50 to 90 percent of newborns with spinal malformation and may be the only indication of a tethered cord.17 Cutaneous manifestations associated with occult spinal lesions include hypertrichosis, lipomas and lipomyelomeningocele, large hemangiomas overlapping the midline, and large dimples above the gluteal crease and anal verge. Healthy newborns often have smaller dimples within the gluteal crease. Dimples should never be probed and should be evaluated with magnetic resonance imaging before neurosurgical intervention.17

