Rotational and angular problems are two types of lower extremity abnormalities common in children. Rotational problems include intoeing and out-toeing. Intoeing is caused by one of three types of deformity: metatarsus adductus, internal tibial torsion, and increased femoral anteversion. Out-toeing is less common than intoeing, and its causes are similar but opposite to those of intoeing. These include femoral retroversion and external tibial torsion. Angular problems include bowlegs and knock-knees. An accurate diagnosis can be made with careful history and physical examination, which includes torsional profile (a four-component composite of measurements of the lower extremities). Charts of normal values and values with two standard deviations for each component of the torsional profile are available. In most cases, the abnormality improves with time. A careful physical examination, explanation of the natural history, and serial measurements are usually reassuring to the parents. Treatment is usually conservative. Special shoes, cast, or braces are rarely beneficial and have no proven efficacy. Surgery is reserved for older children with deformity from three to four standard deviations from the normal.
Parents often seek medical advice about lower extremity appearance in their children. In most cases, the complaint is a variation of normal growth and development, and the problem resolves without treatment as the child grows. Common variations include rotational problems (intoeing, out-toeing) and angular problems (genu varum [bowlegs], genu valgum [knock-knees]).
The normal range of rotation of the foot, leg, and hip includes measurements that fall within two standard deviations of the mean. A variation becomes a deformity when the amount of deviation from normal for that particular age is more than two standard deviations. For example, normal external hip rotation for a five-year-old child is between 30 and 65 degrees. Those with hip rotation values outside this range are said to have a deformity. A careful history and physical examination are all that are necessary to determine whether a complaint requires further evaluation.
History and Physical Examination
Table 1 defines orthopedic terminology used in the history, examination, and diagnosis. Table 21,2 includes important aspects to obtain when evaluating a child with a lower extremity problem.
TABLE 1 Orthopedic Terminology
| Term | Definition |
|---|---|
| Anteversion | Anterior twist or angulation of the femoral head away from the frontal plane. |
| Adduction | The movement of a limb toward the midline of the body in the coronal plane. |
| Valgum | Angulation of a bone distal to a joint or in a part of a bone away from the midline. Genu valgum results in knock-knees, because angulation distal to the knees is away from the midline. |
| Varum | Angulation of a bone or within a bone toward the midline. Genu varum results in bowlegs. |
TABLE 2 History Taking in the Child with Lower Extremity Problems
| Chief complaint | Know exactly what concerns the parents in order to provide prognostic information and discussion of natural history. |
| Complete medical history | Include maternal pregnancy, birth, and development. Questioning perinatal events and motor development may reveal a diagnosis of cerebral palsy. |
| Duration of complaint and progression | History should clarify if the problem began at birth, or before or after walking. How has the problem changed during the past few months? |
| Family history | Lower extremity abnormalities frequently demonstrate a familial tendency. Knowing the parents’ experience and attitudes toward similar problems may help with the discussion later. |
| Why the concern? | Know why the child is in your office or clinic. Is it gait or cosmesis? A toddler’s gait and legs are different from those of an adult. Parental concern often stems from a lack of understanding regarding the maturation of the gait. |
| Signs and symptoms | Ask about pain, limping, tripping, and falling. |
| Sitting habits | Internal tibial torsion is commonly associated with sitting on the feet, while increased femoral anteversion is associated with sitting in a “W” position. |
| Aggravating factors | Torsional deformities become more apparent with fatigue. |
Physical examination should include assessment of height and weight. Normal size for age makes pathologic conditions (e.g., hypophosphatemic rickets, metabolic bone disease) unlikely.3,4 The spine should be examined for scoliosis, hairy patches, or sinus openings. A neurologic examination should be done to rule out neuromuscular disorders.1,5 The lower extremities should be examined for Trendelenburg’s Sign (Figure 1) and leg length discrepancy to rule out hip dysplasia.1,4,5 The range of motion of the hips, knees, and ankles should be determined. evidence of joint laxity (Figure 2) that mimics the appearance of a torsional/angular deformity should be checked. The majority of children less than three years of age will have all the findings. Therefore, these characteristics become more meaningful as children grow older.
FIGURE 1.
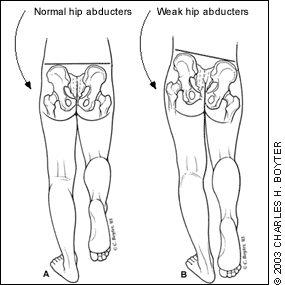
FIGURE 2.
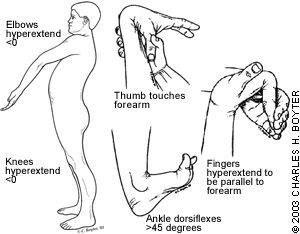
Systems of recording laxity in children.
Presence or absence of flat feet should be determined. The lateral border of the foot should be checked; if it is curved inwardly, the child has metatarsus adductus. Normal ankle dorsiflexion above the neutral position (Figure 3) should be checked to determine if the foot deformity is flexible.4
FIGURE 3.
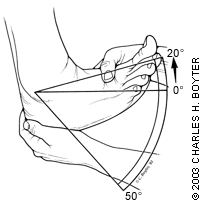
The normal range of ankle dorsiflexion is 20 degrees. Normal plantar flexion is 50 degrees.
Torsional Profile
Torsional profile is a composite of measurements of the lower extremities.6 It differentiates thigh, leg, and foot variations as the anatomic basis of a torsional abnormality. It also documents the severity of the abnormality. Rotational problems should be clinically evaluated and the findings compared with normal values. Figure 4 describes normal values and values with two standard deviations for three of the four components of the torsional profile, which are the foot progression angle, forefoot alignment, hip rotation, and thigh-foot angle.
FIGURE 4.
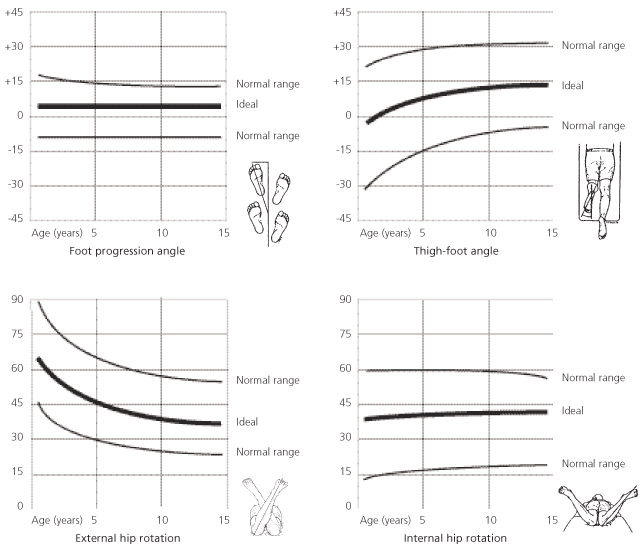
Torsional Profiles. The charts include normal values and two standard deviations, and can be used to record findings and show to parents.
Adapted from Wenger DR, Rang M. The art and practice of children’s orthopaedics. New York: Raven Press, 1993.
Foot Progression Angle
Also known as gait angle, this is the angle made by the foot with respect to a straight line plotted in the direction the child is walking.7 The child’s feet can be dusted with chalk prior to walking on a long strip of paper toward his or her parents.6 The angle can then be measured. A plus sign denotes an out-toeing angle, and a minus sign denotes an intoeing angle. Foot progression angle can be normal in children with combined torsional deformity (e.g., medial femoral torsion compensated by lateral tibial torsion).4
Forefoot Alignment
Metatarsus adductus exists if the sole of the foot is adducted (deviates medially) and if the lateral border is “C” shaped.
Hip Rotation
The range of internal and external rotation of the hips should be measured with the child prone and knees flexed to 90 degrees. Internal rotation is determined by fully abducting the legs. External rotation is determined by fully adducting the legs. The degrees of internal and external rotation are generally equal, about 45 degrees. In children with excess femoral anteversion, the femoral neck axis is rotated anteriorly in relation to the frontal plane of the femoral condyles. The internal rotation will far exceed external rotation, while the opposite is true in femoral retroversion.
Thigh-Foot Angle
The angle between the axis of the foot and the axis of the thigh should be measured with the child prone and knees flexed to 90 degrees. Intoeing angles are given negative values while out-toeing angles are given positive values. The angle describes the degree of tibial torsion. Each leg should be measured because the problem may be unilateral or the legs may differ in degree of torsion.5 Normally, the foot axis out-toes 10 degrees relative to the thigh axis. If the foot turns in relative to the thigh axis, the child has internal tibial torsion.7
Additional Measurements
In addition to the torsional profile test for bowlegs and knock-knees, angulation should be quantified by measuring the intercondylar or intermalleolar distance (Figure 5).3 Standard values for these measurements are shown in Figure 6. Intercondylar measures the degree of genu varum and is the distance between the medial femoral condyles when the lower extremities are positioned with the medial malleoli touching. The intermalleolar measurement quantifies genu valgum and is the distance between the medial malleoli with the medial femoral condyles touching. Intermalleolar and intercondylar have the disadvantage of being relative measurements that are affected by the child’s size. Measuring the femoral tibial angle with a goniometer is a more accurate way to quantify angulation. However, obtaining reliable goniometric measure on a child is often a challenge. A chart by Salenius and Vankka can be used for that purpose.8
FIGURE 5
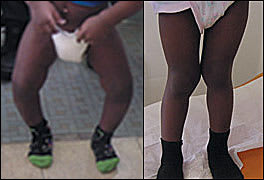
Genu varum (bowlegs), and genu valgum (knock-knees). The intercondylar distance is the width between the knees when the feet are placed as close together as possible (A). The intermalleolar distance is the width between the ankles when the child’s knees are placed together (B).
FIGURE 6.
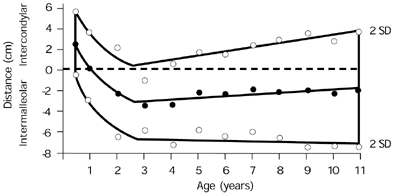
Standard values for intercondylar and intermalleolar distances in a study of 196 white children. Standard (or mean) values are solid dots; circles are two standard deviations.
Adapted from Greene WB. Genu varum and genu valgum in children: differential diagnosis and guidelines for evaluation. Compr Ther 1996;22:22–9.
Clinical Conditions
INTOEING
Intoeing is caused by one of three types of deformity: metatarsus adductus, internal tibial torsion, and increased femoral anteversion (Figure 7). The cause of intoeing varies with the age of the child.9 In the first year of life, metatarsus adductus, alone or combined with internal tibial torsion, is usually the cause. In toddlers, the cause is internal tibial torsion alone or combined with metatarsus adductus, and may involve one or both sides. In early childhood, the cause is usually femoral anteversion, and is nearly always bilateral and symmetrical.
FIGURE 7.
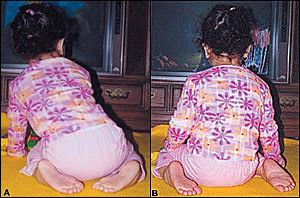
Intoeing. The origin of intoeing may lie in the leg or the foot. Internal tibial torsion is commonly associated with sitting on the feet (A). Increased femoral anteversion is commonly associated with sitting in a “W” position (B).
METATARSUS ADDUCTUS
Metatarsus adductus is the most common congenital foot deformity,9 occurring in one out of 1,000 live births. It occurs more frequently in female children,10 and on the left side more than the right.9 The most likely cause is intrauterine packing. Examination reveals adduction of the forefoot with a convex lateral border. The ankle has normal motion. This entity is different from clubfoot, in which the foot does not plantar flex beyond normal, the heel is in varum (medial deviation), and the sole is kidney-shaped when viewed from the bottom.11 The foot should be assessed for flexibility by holding the heel in neutral position and abducting the forefoot to at least a neutral position (Figure 8).4 If this cannot be done, then the deformity is rigid (i.e., metatarsus varus). Eighty-five to 90 percent of cases of metatarsus adductus identified at birth resolve without treatment by one year of age.4 [evidence level B, nonrandomized studies]
FIGURE 8.
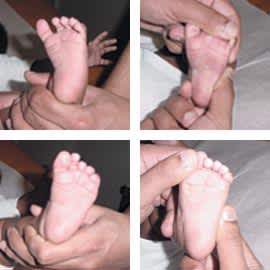
Technique for assessing flexibility of metatarsus adductus. The hind part of the foot is stabilized by lateral pressure over the calcaneal cuboid joint, and the forefoot is abducted.
Flexible metatarsus adductus is managed by stretching exercises during the first eight months of life. Parents are instructed to hold the infant’s hindfoot in one hand, the forefoot in the other, and stretch the midfoot, opening the “C”-shaped curve and slightly overcorrecting it. This exercise should be performed five times at each diaper change.11 Flexible deformities that persist beyond eight months, and rigid deformities, may need a cast (the patient can be referred to an orthopedist for cast application). Better results occur if treatment is begun before eight months of age.2 [evidence level B, nonrandomized studies]
Casts should be changed biweekly with correction usually achieved after three or four casts. Residual adductus causes no long-term disability. Surgery is not recommended because surgical complications are frequent.9
Infants may present with moderate metatarsus adductus and extreme adduction of great toe (metatarsus primus varus). Treatment is surgical release of the abductor hallucis tendon performed between six and 18 months of age.11
INTERNAL TIBIAL TORSION
Internal tibial torsion is the most common cause of intoeing.9,12 It affects males and females equally, and is often asymmetrical with the left side affected more than right. The cause is believed to be intrauterine position, sleeping in the prone position after birth, and sitting on the feet (Figure 7). The child with internal tibial torsion walks with the patella facing forward and the feet pointing inward. This results in an internal foot progression angle and an internal foot-thigh angle. In 90 percent of cases, internal tibial torsion gradually resolves on its own by the time the child reaches eight years of age.9 [evidence level B, nonrandomized studies] Avoiding prone sleeping and sitting on feet enhance resolution. Treatment with night splints, shoe wedges, and orthotics are unnecessary and ineffective.9 Osteotomy of the tibia has been associated with a high complication rate because of compartment syndrome or peroneal nerve injury. Conditions that may support operative correction include (1) being older than eight years of age, (2) a child with significant or functional deformity, and (3) a thigh-foot angle of greater than three standard deviations beyond the mean.13
INCREASED FEMORAL ANTEVERSION
Femoral anteversion describes the normal position of the femur, which is medially rotated on its long axis at birth. It is often familial and is usually bilateral, affecting females more than males.5,9 The child with increased femoral anteversion walks with his or her patellae and feet pointing inward. The gait appears clumsy and the child may trip as a result of crossing his or her feet.9 The child will have strong tendency to sit in a “W” position (Figure 7). Physical examination reveals increased internal hip rotation (up to 90 degrees) and decreased external rotation. Increased femoral anteversion is usually diagnosed after three years of age, peaks at four to six years, and then gradually resolves.12 Spontaneous resolution occurs in more than 80 percent of cases by late childhood.9 [evidence level B, nonrandomized studies] The hip range of motion can be measured every six to 12 months to document gradual decrease in femoral anteversion. Nonoperative treatment is ineffective.9,13 Increased femoral anteversion is a benign condition and complications of surgery are frequent.9 Conditions that may support a surgical approach include (1) being older than eight years of age, (2) severe deformity that creates significant cosmetic and functional disability, (3) anteversion in excess of 50 degrees, (4) deformity more than three standard deviations beyond the mean, and (5) a family who is aware of the risks of the procedure.13
Out-toeing
Out-toeing is less common than intoeing, and its causes are similar but opposite to those of intoeing.
FEMORAL RETROVERSION
Femoral retroversion is common in early infancy and is caused by external rotation contracture of the hip secondary to intrauterine packing.1,7,9 It becomes apparent when the prewalking child stands with his or her feet turned out to nearly 90 degrees (this is sometimes called a “Charlie Chaplin appearance”).12 Femoral retroversion occurs more commonly in obese children. When femoral retroversion is unilateral, it is more common on the right side.1,9
Physical examination reveals increased external rotation to almost 90 degrees and decreased internal rotation. It may gradually improve on its own during the first year of walking.1,7,10 If resolution is not evident and persistent external rotation is present on successive visits at two to three years of age, referral to an orthopedist is indicated because persistent lateral femoral torsion is associated with osteoarthrosis, increased risk of stress fracture of the lower limbs, and slipped capital femoral epiphysis.9 [evidence level C, expert opinion] Nonoperative treatment is ineffective.1,9,10
EXTERNAL TIBIAL TORSION
External tibial torsion is usually seen between four to seven years of age.1,9 It is often unilateral and more common on the right side.9 The tibia rotates laterally with growth, making lateral tibial torsion worse.9,13 Surgery has a high complication rate and should not be done until after the child is more than 10 years of age. The deformity should be severe with a thigh-foot angle of more than 40 degrees to justify operative correction. Disability from lateral tibial torsion is usually caused by patellofemoral instability and pain.9 Therefore, lateral tibial torsion is a more common indication for osteotomy than internal torsion.
FLAT FEET
Flat feet are common in children because arch development occurs primarily before four years of age, and because the development has a wide variation in the rate or onset in any given child.14 Physical examination should test for flexibility. If an arch is reconstituted on toe standing, then it is termed a flexible flat foot. The arch also should recreate when the foot is dependent, hanging over the examination table.
The most common etiology of the flexible flat foot is ligamentous laxity, which allows the foot to sag with weight bearing.11 Spontaneous correction is usually expected within one year of walking.8 No treatment is indicated for painless flexible flat foot. Trauma, occult infection, a foreign body, tarsal coalition, bone tumors, or osteochondrosis of the tarsal navicular bone may cause a stiff and painful flat foot. Referral to an orthopedist is indicated.11
Angular Variations
Many children will look bowlegged when they start to walk and then knock-kneed between three to seven years. The gradual change from varum to valgum may be caused by a widening pelvis.2
TABLE 3 Differential Diagnosis for Genu Varum and Genu Valgum
| Genu varum | Genu valgum |
| Physiologic bowlegs | Hypophosphatemic rickets Previous metaphyseal fracture of the proximal tibia Multiple epiphyseal dysplasia Pseudoachondroplasia |
| Infantile tibia vara | |
| Hypophosphatemic rickets | |
| Metaphyseal chondrodysplasia | |
| Focal fibrocartilaginous dysplasia |
Information from Greene WB. Genu varum and genu valcum in children: differential diagnosis and guidelines for evaluation. Compr Ther 1996;22:22-29.
Genu varum (bowlegs) is seen from birth until two years of age, while genu valgum (knock-knees) peaks from two to four years.3,14 The most common reason is physiologic or a normal developmental variation. Management is by serial measurement of intercondylar/intermalleolar distance to document gradual spontaneous resolution. Unilateral deformity, progressive deformity, or lack of spontaneous resolution should alert the physician to the possibility of pathologic angular deformity (Table 3).3 Guidelines for obtaining radiographs include (1) genu varum or genu valgum that is beyond two standard deviations for the child’s age (Figure 6), (2) height less than 25th percentile, (3) genu varum that has been increasing in severity, and (4) asymmetry of limb alignment.3
Information from Greene WB. Genu varum and genu valgum in children: differential diagnosis and guidelines for evaluation. Compr Ther 1996;22:22–9
If physiologic genu varum or genu valgum persists beyond seven to eight years of age, orthopedic referral is indicated.5 Pathologic conditions should be referred for appropriate management.

