Tick-borne diseases in the United States include Rocky Mountain spotted fever, Lyme disease, ehrlichiosis, tularemia, babesiosis, Colorado tick fever, and relapsing fever. It is important for family physicians to consider these illnesses when patients present with influenza-like symptoms. A petechial rash initially affecting the palms and soles of the feet is associated with Rocky Mountain spotted fever, whereas erythema migrans (annular macule with central clearing) is associated with Lyme disease. Various other rashes or skin lesions accompanied by fever and influenza-like illness also may signal the presence of a tick-borne disease. Early, accurate diagnosis allows treatment that may help prevent significant morbidity and possible mortality. Because 24 to 48 hours of attachment to the host are required for infection to occur, early removal can help prevent disease. Treatment with doxycycline or tetracycline is indicated for Rocky Mountain spotted fever, Lyme disease, ehrlichiosis, and relapsing fever. In patients with clinical findings suggestive of tick-borne disease, treatment should not be delayed for laboratory confirmation. If no symptoms follow exposure to tick bites, empiric treatment is not indicated. The same tick may harbor different infectious pathogens and transmit several with one bite. Advising patients about prevention of tick bites, especially in the summer months, may help prevent exposure to dangerous vector-borne diseases.
Because people continue to interact with nature, patients will continue to present to physician offices with tick-borne diseases. It is important for family physicians to recognize these illnesses because early, accurate diagnosis may lessen the morbidity and mortality of these treatable diseases. This article provides an update on the more common tick-borne diseases. Agents and characteristics of tick-borne disease are summarized in Tables 1 and 2.1
Strength of Recommendations
| Key clinical recommendation | Label | References |
|---|---|---|
| Appropriate antibiotic therapy should be initiated immediately when there is suspicion of Rocky Mountain spotted fever, ehrlichiosis, or relapsing fever rather than waiting for laboratory confirmation. | C | 7 |
| Treatment with doxycycline (Vibramycin) or tetracycline is recommended for Rocky Mountain spotted fever, Lyme disease, ehrlichiosis, and relapsing fever. | C | 7,16,20 |
| Recommended actions to prevent tick-borne disease include avoidance of tick-infested areas; wearing long pants and tucking the pant legs into socks; applyingN,N-diethyl-m-toluamide (DEET) insect repellents; using bed nets when camping; and carefully inspecting oneself frequently while in an at-risk area. | C | 16 |
| Antibiotic prophylaxis is not routinely recommended for a tick bite to prevent Lyme disease unless the risk of infection is high. | B | 16,17 |
| Recommended treatment for suspected tularemia is streptomycin or gentamicin given empirically before evidence of laboratory confirmation. | C | 24 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, opinion, or case series. See page 2237 for more information.
TABLE 1 Causative Agents, Vectors, and Geographic Distribution of Tick-Borne Diseases
| Disease | Causative agents | Vectors | Geographic regions | |
|---|---|---|---|---|
| Rocky Mountain spotted fever | Rickettsia rickettsii | Wood tick (Dermacentor andersoni) | Limited to Western hemisphere; all states except Maine, Hawaii, and Alaska | |
| Dog tick (Dermacentor variabilis) | Common to eastern and southern states | |||
| Lyme disease | Borrelia burgdorferi | Black-legged or deer tick (Ixodes scapularis) | Majority of cases are reported in the Northeast and Great Lakes area; reported in every state except Montana | |
| Main reservoir: white-footed mouse | ||||
| Ehrlichiosis | ||||
| Human monocytic ehrlichiosis | Ehrlichia chaffeensis | Lone Star tick (Amblyomma americanum) | South-central United States | |
| Dog tick (D. variabilis) | Southeastern United States | |||
| Human granulocytic ehrlichiosis | Anaplasma phagocytophilum | Black-legged or deer tick (I. scapularis) | Upper midwestern and northeastern United States | |
| Tularemia | Francisella tularensis | Lone Star tick (A. americanum) | Occurs in rural areas in all states except Hawaii, mostly in south-central and southeastern United States | |
| Wood tick (D. andersoni) | Western United States | |||
| Dog tick (D. variabilis) | Southeastern United States | |||
| Babesiosis | Babesia microti | Black-legged or deer tick (I. scapularis) | Most cases occur in the northeasternUnited States. | |
| Babesia divergens | ||||
| Colorado tick fever | RNA orbivirus | Wood tick (D. andersoni) | Found predominantly in Rocky Mountain region | |
| Relapsing fever | Spirochete withinBorrelia genus | Ticks of the Ornithodoros genus | Most cases occur west of the MississippiRiver, especially in mountainous areas. | |
| Main reservoirs: rodents, rabbits, and hares | ||||
TABLE 2 Clinical Characteristics of Tick-Borne Diseases
| Disease | Signs and symptoms | Diagnosis | Treatment |
|---|---|---|---|
| Rocky Mountain spotted fever | Malaise, myalgias, fever, frontal headache, nausea, vomiting, nonproductive cough, sore throat, pleuritic chest pain, abdominal petechial rash affecting pads and soles of feet | Clinical signs and symptoms; skin biopsy of rash with immunofluorescent staining (60 percent sensitive); laboratory testing is of limited usefulness; routine findings include thrombocytopenia and hyponatremia | Doxycycline (Vibramycin); tetracycline; chloramphenicol (Chloromycetin) |
| Lyme disease | Stage 1 (early localized): erythema migrans rash at bite of bite, influenza-like symptoms, fever, fatigue, arthralgias, headache, cough, lymphadenopathy | Laboratory testing usually not necessary; enzyme-linked immunosorbent assay, confirmed by Western blotting; polymerase chain reaction of joint fluid may be helpful if available, but culture is difficult and lengthy | Children: amoxicillin; doxycycline (if older than 12 years) Adults: doxycycline; amoxicillin; cefuroxime (Ceftin) or erythromycin (if allergic to penicillin) |
| Stage 2 (early disseminated): secondary cutaneous annular lesions, fever, adenopathy, central nervous system symptoms; cough and pharyngitis may occur | |||
| Stage 3 (late chronic): arthritis, central nervous system impairment, dermatitis, keratitis, neurologic and myocardial abnormalities | |||
| Ehrlichiosis | Influenza-like syndrome, fever, chills, cough, malaise, headache, and myalgia; macular, maculopapular, or petechial rash (rare with human granulocytic ehrlichiosis) | Laboratory findings include leukopenia, thrombocytopenia, and elevated serum transaminase levels; diagnosis made with seroconversion during convalescence | Doxycycline; tetracycline |
| Tularemia | Fever, chills, headache, malaise, fatigue, myalgia; may include: cough, sore throat, skin ulcers, pleural effusions, pneumonia, acute respiratory distress syndrome, pericarditis, nausea, or vomiting | Clinical signs and symptoms; exposure to rabbits, wild rodents, or ticks; acute and convalescenttiters; presence of leukocytosis (however, white blood cell count may be normal); chest radiograph showing triad of oval opacities, hilar adenopathy, and pleural effusions | Streptomycin; gentamicin |
| Babesiosis | Influenza-like symptoms, fever, sweating, myalgia, headache, hemolytic anemia, hemoglobinuria, jaundice, renal failure | Fever, hemolytic anemia, and exposure history; peripheral smear shows protozoa in “Maltese cross” pattern; serologic testing and polymerase chain reaction tests also are used | Quinine (Quinamm) plus clindamycin (Cleocin); mild disease requires only symptomatic treatment; exchange transfusion can be used in severely ill patients |
| Colorado tick fever | Influenza-like symptoms, sore throat, “saddleback” fever | Diagnosis usually made with blood smears stained with immunofluorescence; laboratory findings may include leukopenia or thrombocytopenia | Supportive only |
| Relapsing fever | Influenza-like symptoms, arthralgias, dizziness, nausea, vomiting, high fever with irregular pattern, delirium, splenomegaly, meningeal signs; may include: epistaxis, hemoptysis, iridocyclitis, coma, cranial nerve palsy, pneumonitis, myocarditis, and rupture of the spleen | Detection of spirochetes in blood, bone marrow, cerebrospinal fluid during febrile episode; laboratory findings may include normal or elevated leukocyte count thrombocytopenia | Doxycycline; erythromycin treatment may lead to Jarisch-Herxheimer reaction |
Rocky Mountain Spotted Fever
EPIDEMIOLOGY
Rocky Mountain spotted fever is caused by Rickettsia rickettsii and is the most common rickettsial disease in the United States.2 The disease is limited to the Western hemisphere and occurs in all states except Maine, Hawaii, and Alaska. The disease is more common in the coastal Atlantic states from April to September, although infections may occur year-round further south3 The wood tick (Dermacentor andersoni) is the principal vector in the western United States, whereas the dog tick (Dermacentor variabilis) is the most common vector in the eastern and southern United States. Transmission from person to person is not thought to occur. The incidence of Rocky Mountain spotted fever is highest in children five to nine years of age.4
SIGNS AND SYMPTOMS
Typically in tick-borne diseases, a tick bite is recalled by 50 to 70 percent of patients.3,4 The onset of symptoms of Rocky Mountain spotted fever usually begins five to seven days after inoculation. Common symptoms include generalized malaise, myalgias (especially in the back and leg muscles), fever, frontal headaches, nausea, and vomiting. Other symptoms may include nonproductive cough, sore throat, pleuritic chest pain, and abdominal pain. The classic presenting symptoms include sudden onset of headache, fever, and chills accompanied by an exanthem appearing within the first few days of symptoms. Initially, lesions appear on the palms, soles, wrists, ankles, and forearms. The lesions are pink and macular and fade with applied pressure. The rash then extends to the axilla, buttocks, trunk, neck, and face, becoming maculopapular and then petechial (Figure 15). The lesions may then coalesce to form large areas of ecchymosis and ulceration. Respiratory and circulatory failure, as well as neurologic compromise, may occur.6 Patients with glucose-6-phosphate dehydrogenase (G6PD) deficiency are at especially high risk for complications and poor outcomes.7
Figure 1.
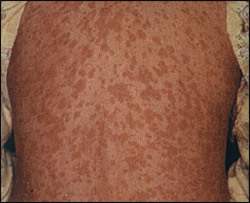
Image of a patient with Rocky Mountain spotted fever; note late rash on trunk. Reprinted with permission from Drage LA. Life-threatening rashes: dermatologic signs of four infectious diseases. Mayo Clin Proc 1999;74:70.
DIAGNOSIS
The diagnosis of Rocky Mountain spotted fever is based primarily on clinical signs and symptoms. If a rash is present, the use of skin biopsy and immunofluorescent staining for Rickettsia is highly specific, although with only slightly more than 60 percent sensitivity. Laboratory testing is of limited usefulness but may include thrombocytopenia and hyponatremia.8 Elevation of specific enzyme-linked immunosorbent assay (ELISA) and latex agglutination titers usually is delayed until the convalescence period.
TREATMENT
Fever and headache during peak months of tick exposure in endemic areas should suggest Rocky Mountain spotted fever. Rash, thrombocytopenia, and hyponatremia make immediate treatment imperative. Antimicrobial agents for the treatment of Rocky Mountain spotted fever include tetracycline, doxycycline (Vibramycin), and chloramphenicol (Chloromycetin) for a minimum of seven days.9 Fluoroquinolones also may be effective, but are not recommended for routine use in patients with Rocky Mountain spotted fever because of a lack of evidence.10 For optimal effect, it is critical to treat patients early in the course of their illness. According to the Centers for Disease Control and Prevention, appropriate antibiotic treatment should be initiated immediately when there is a suspicion of Rocky Mountain spotted fever on the basis of clinical and epidemiologic findings. Treatment should not be delayed until laboratory confirmation is obtained.7
Lyme Disease
EPIDEMIOLOGY
Lyme disease is the most common vector-borne infectious disease in the United States.9 The disease is caused by the spirochete Borrelia burgdorferi. In the United States, the main vector is Ixodes scapularis (Figure 211), commonly referred to as the black-legged or deer tick because the female tick often attaches itself to the white-tailed deer during the winter. Natural reservoirs for B. burgdorferi include the white-footed mouse and other small mammals. The larvae or nymphs of the tick feed on the white-footed mouse and become infected. Adult ticks or, more commonly, nymphs may then infect humans. Studies using animals have shown that infected nymphal-stage ticks must remain attached for 36 to 48 hours or longer, and infected adult ticks must remain attached for 48 to 72 hours or longer, before the risk of transmission of B. burgdorferi becomes substantial.12–15There is no evidence that Lyme disease can be transmitted by mosquitoes, flies, or fleas. Blood products have never been associated with transmission of Lyme disease.16
SIGNS AND SYMPTOMS
Lyme disease typically develops in three stages. Stage 1 (early localized) Lyme disease occurs seven to 10 days after tick bite. Findings include typical rash (erythema migrans) in 75 percent of patients at the site of the tick bite. The rash typically develops as an annular macule or papule with central clearing that may expand to a diameter of up to 50 cm. Other indications include influenza-like symptoms of low-grade fevers, fatigue, arthralgias, headaches, cough, and regional lymphadenopathy. Stage 2 (early disseminated) Lyme disease occurs a few weeks after the initial infection. Symptoms include multiple secondary cutaneous annular lesions, fever, adenopathy, and central nervous system symptoms. Cough and pharyngitis may occur. Stage 3 (late chronic disease) symptoms include chronic arthritis, central nervous system impairment, dermatitis, and keratitis. Other symptoms may include neurologic abnormalities such as meningoencephalitis, Bell’s–like palsy, and radiculopathies, and myocardial abnormalities such as atrioventricular block, pericarditis, and cardiomegaly.8
DIAGNOSIS
Early diagnosis of Lyme disease in a patient with typical erythema migrans in an endemic area does not require laboratory confirmation. However, ELISA testing is 89 percent sensitive and 72 percent specific. Positive results on ELISA testing should be confirmed with Western blotting. Polymerase chain reaction testing, although not widely available, may be useful for the diagnosis, especially with fluid from the joints of the affected patient.3 Isolation of B. burgdorferi from most tissues and body fluids by culture is difficult to achieve and requires weeks to grow before it can be analyzed.
TREATMENT
The risk of infection with B. burgdorferi after a recognized tick bite is minimal, and is almost nonexistent if the tick was attached less than 36 hours. Routine antibiotic prophylaxis is not indicated.8,16 A cost-effectiveness analysis showed that prophylaxis with one 200-mg dose of doxycycline was cost-effective only if the likelihood of infection exceeded 3.5 percent, much higher than in the typical practice setting.17 If symptoms develop, antibiotic treatment is curative in most cases. Recommended antibiotic treatment includes doxycycline (100 mg orally twice per day if patient is older than 12 years) or amoxicillin (500 mg orally three times per day or 50 mg per kg per day orally for patients 12 years and younger). Cefuroxime (Ceftin; 500 mg orally, twice per day) or erythromycin (250 mg orally, four times per day) can be prescribed for persons who are allergic to penicillin or cannot take tetracyclines. Treatment usually lasts 14 to 21 days for uncomplicated cases. Late or severe disease, particularly with neurologic or cardiovascular manifestations, requires treatment with intravenous antibiotics, with a switch to oral therapy once the patient is no longer in high-degree atrioventricular block. Treatment in these advanced cases should be administered for at least 30 days. Late disease may be associated with treatment failures, and re-treatment may be necessary.18
Ehrlichiosis
EPIDEMIOLOGY
Human ehrlichiosis has been reported in the United States with two identifiable subtypes. Human monocytic ehrlichiosis (HME) is caused by Ehrlichia chaffeensis, and human granulocytic ehrlichiosis (HGE) is caused by Anaplasma phagocytophilum (formerly called Ehrlichia equi or Ehrlichia phagocytophila). The two subtypes are clinically indistinguishable but epidemiologically distinct.19
HME occurs most frequently in the south-central and southeastern United States. It occurs year-round with the highest incidence in June and July. In contrast to the tendency of Lyme disease and Rocky Mountain spotted fever to occur in children, HME typically affects adults. E. chaffeensis is found in Amblyomma americanum (Lone Star tick) and D. variabilis (dog tick). The white-tailed deer is the principal animal reservoir.
The majority of cases of HGE occur in the upper midwestern and northeastern United States. Adults who live in rural areas or have exposure to tick-infested areas are most likely to be affected. The I. scapularis species are the principal vectors, and the white-footed mouse and white-tailed deer are the principal hosts.
SIGNS AND SYMPTOMS
The signs and symptoms of ehrlichiosis include an influenza-like syndrome consisting of fever, chills, cough, malaise, headache, and myalgia. Symptoms begin approximately seven days after tick bite and include a maculopapular, macular, or petechial rash that affects the trunk and upper extremities and, in rare cases (less than 5 percent), the palms and soles. HME and HGE present with similar signs and symptoms, but HGE rarely presents with the rash. Clinical differentiation from Rocky Mountain spotted fever is difficult.
DIAGNOSIS
Laboratory findings in patients with HME and HGE include leukopenia, thrombocytopenia, and elevated serum transaminase levels. Patients presenting with a nonspecific influenza-like syndrome of fever, chills, malaise, headache, and myalgia coupled with leukopenia and thrombocytopenia should be treated empirically. The principal method of diagnosing human ehrlichiosis is detection of seroconversion during convalescence. A fourfold rise or fall in antibody titer with a minimum peak of 1:64 and a single serum antibody titer greater than or equal to 1:128 is necessary for the diagnosis.
TREATMENT
As with other tick-borne diseases, treatment of ehrlichiosis should be started before laboratory tests confirm the diagnosis. Doxycycline at a dosage of 100 mg twice per day for adults or 4.4 mg per kg per day in two divided doses for children who weigh less than 45.4 kg (99 lb, 14 oz) is the treatment of choice.20 Tetracycline 500 mg orally four times per day is an alternative. Chloramphenicol is considered an alternative to prevent tooth staining, but there is a small risk of aplastic anemia with its use. Treatment should be continued for at least three days after fever subsides and until evidence of clinical improvement, for a minimum of five to seven days.20Severe cases may require longer treatment courses.
Tularemia
EPIDEMIOLOGY
Francisella tularensis is the bacterium that causes tularemia (also known as rabbit fever). The tick vectors include A. americanum and D. variabilis in the southeastern and south-central United States and D. andersoni in the west. Transmission of the bacteria occurs by ingestion, inoculation, inhalation, or contamination. In the winter, the most common route is through microlesions in the skin of hunters who have skinned infected rabbits. In the summer, transmission occurs via ticks, deer flies, and horse flies. Although less common, consumption of undercooked infected meat and contaminated water also can lead to infection.
SIGNS AND SYMPTOMS
Clinical manifestations of tularemia can be divided into various syndromes, including ulceroglandular (the most common), oculoglandular, oropharyngeal/gastrointestinal tract, pulmonary, and typhoidal tularemia.8 Illness usually begins three to five days after inoculation, with rapid onset of fever, chills, headache, malaise, fatigue, and myalgias. Cough is present in about one third of patients Other findings may include skin ulcers, sore throat, pleural effusions, pneumonia, acute respiratory distress syndrome, and pericarditis.21 Nausea and vomiting also may occur. Within 24 to 48 hours, an inflamed papule appears at the infected site (e.g., finger, arm, eye, roof of the mouth) except in glandular or typhoidal tularemia. The papule becomes pustular and ulcerates, producing an ulcer crater with colorless exudate. Regional lymphadenopathy occurs and may suppurate and drain. In children, the cervical or posterior auricular nodes commonly are affected. In adults, the inguinal and femoral nodes are more likely to be affected.
DIAGNOSIS
Tularemia should be suspected if the patient has been exposed to rabbits, wild rodents, or ticks; has characteristic symptoms; and has a primary pustular lesion on an extremity. Isolation of the organism from skin lesions, lymph nodes, or sputum is diagnostic but dangerous because the organism can be highly infectious. The disease is considered a potential biologic weapon. Extreme caution should be maintained when handling infected tissues or culture media. Acute and convalescent titers also can confirm the diagnosis. Leukocytosis is common, but the white blood cell count may be normal. Abnormal chest radiographic findings (i.e., triad of oval opacities, hilar adenopathy, and pleural effusions) are more likely with tularemia than in other tick-borne diseases.22,23
TREATMENT
Treatment should begin before confirmatory laboratory tests are obtained. If available, the treatment of choice for tularemia is streptomycin (0.5 g intramuscularly every 12 hours until the patient’s body temperature is normal; thereafter, 0.5 g per day for five days). Gentamicin (3 to 5 mg per kg per day, intramuscularly or intravenously in three divided doses for seven to 14 days) also is effective.24 If renal disease is present, the dose of gentamicin needs to be reduced. Chloramphenicol or tetracyclines also have been used, but relapses occasionally occur with these medications, and they may not prevent node suppuration.3
Babesiosis
EPIDEMIOLOGY
Babesiosis is the only tick-borne disease in the United States that is caused by a protozoan (Babesia divergens o rBabesia microti). Transmission occurs by the vector tick (various species of Ixodes). Most cases occur in the northeastern United States.
SIGNS AND SYMPTOMS
Symptoms are similar to those of other tick-borne diseases and include influenza-like symptoms one week after inoculation. Fever, sweating, myalgias, and headache also occur. Babesiosis may resemble falciparum malaria, with high fever, hemolytic anemia, hemoglobinuria, jaundice, and renal failure, especially in asplenic patients. Asymptomatic infection may persist for years in younger adults.
DIAGNOSIS AND TREATMENT
Babesiosis usually is suspected in a patient with fever, hemolytic anemia, and an appropriate exposure history. The diagnosis is made by detection of protozoa in blood smears. A characteristic tetrad, the “Maltese cross,” appears. Serologic testing and polymerase chain reaction testing also are available.
Mild disease requires only symptomatic treatment. For severe cases (e.g., persistent high fever, progressive anemia, rising parasitemia), patients should be treated with quinine (Quinamm; 650 mg of salt orally, three times per day for seven days) plus clindamycin (Cleocin; 600 mg orally, three times per day or 1.2 g administered intravenously twice per day for seven to 10 days), or with atovaquone (Mepron; 750 mg orally twice per day for seven to 10 days) plus azithromycin (Zithromax; 600 mg orally per day for seven to 10 days).25 Reduced dosing is required in children. Exchange transfusion has been used in severely ill patients with high parasitemia.
Colorado Tick Fever
EPIDEMIOLOGY AND TRANSMISSION
Colorado tick fever is caused by an RNA orbivirus transmitted by the D. andersoni wood tick. Between 200 and 300 cases are diagnosed each year, predominantly in the Rocky Mountain region. Because of its benign presentation, the infection often may go undetected, and the annual incidence probably is much higher.26 Patients who are immunocompromised or who have undergone a splenectomy are at increased risk for severe complications.
SIGNS AND SYMPTOMS
Influenza-like symptoms usually begin within one week after inoculation. Although approximately one third of patients have a sore throat, more extensive involvement of the respiratory system rarely occurs.2 The most significant feature is a biphasic or “saddleback” fever associated with meningitis, rash, and conjunctivitis.8 The disease usually lasts seven to 10 days.
DIAGNOSIS
Diagnosis usually is made with blood smears, which are stained for the virus with immunofluorescence. Other laboratory abnormalities may include leukopenia and thrombocytopenia.
TREATMENT
Treatment is supportive. No specific medication is indicated. At the onset of symptoms, most patients will be treated empirically with tetracycline, doxycycline, or chloramphenicol to cover for other tick-borne diseases.
Relapsing Fever
EPIDEMIOLOGY AND TRANSMISSION
Relapsing fever is caused by the spirochete within the genus Borrelia. Ticks of the Ornithodoros genus are the chief vectors. Hosts include rodents (e.g., rats, mice, chipmunks, squirrels), rabbits, and hares. In the United States, most cases occur west of the Mississippi River, especially in mountainous areas. The disease typically occurs sporadically or in small, often familial, clusters.8
SIGNS AND SYMPTOMS
The average inoculation period is one week. Influenza-like symptoms, arthralgias (possibly severe), dizziness, nausea, and vomiting are common. Fever usually is high (greater than 40°C [104°F]) and irregular in pattern, and sometimes is associated with delirium. Most patients have splenomegaly. Meningeal signs may be present. Other complications can include epistaxis, hemoptysis, iridocyclitis, coma, cranial nerve palsy, pneumonitis, myocarditis, and rupture of the spleen.
DIAGNOSIS
Diagnosis is made most easily by detection of spirochetes in blood, bone marrow, or cerebrospinal fluid during a febrile episode. Other laboratory findings may include normal or moderate elevations in the leukocyte count and thrombocytopenia.
TREATMENT
The treatment of choice is doxycycline (100 mg orally, twice per day for five to 10 days). Alternative therapy includes erythromycin (500 mg orally four times per day for five to 10 days).27 Therapy may lead to a Jarisch-Herxheimer reaction (i.e., generalized malaise, headache, fever, sweating, rigors, seizures, or stroke), especially if given during the late febrile stage. Administering acetaminophen two hours before and after antibiotic administration may lessen the severity of the reaction. Steroids and nonsteroidal anti-inflammatory drugs do not prevent or modify the cardiopulmonary disturbances of the reaction.8
Combined Infections
The same tick may harbor different infectious pathogens and transmit several with one bite.28 For example, I. scapularis may transmit ehrlichiosis, Lyme disease, and babesiosis. Babesiosis occurs in 23 percent of patients with Lyme disease29; ehrlichiosis occurs in 10 to 30 percent of patients with Lyme disease; and 10 to 30 percent of patients with ehrlichiosis acquire Lyme disease or babesiosis concurrently. Combined infections are thought to cause more severe symptoms.19,28
Prevention of Tick Exposure
Measures to help prevent tick exposure include avoiding tick-infested areas (especially during the summer months), wearing long pants and tucking pant legs into socks, using tick repellents containing N,N-diethyl-m-toluamide(DEET) for the skin and permethrin for clothing, and using bed nets when sleeping on the ground or camping.
Early removal of ticks can help prevent disease because at least 24 to 48 hours of attachment to the host are required before infection occurs.19 The body of the tick should be grasped gently and vertical traction applied until it dislodges. Blunt, medium-tipped, angled forceps offer the best results. Commercially available devices are recommended over tweezers for tick removal. Tick removal methods that are not recommended include applying a hot match to the tick body; covering the tick with petroleum jelly, nail polish, alcohol, or gasoline; using injected or topical lidocaine; and passing a needle through the tick. When an improper technique is applied, parts of the proboscis may remain in the skin, which can lead to infection or granuloma formation.30

