Although puncture wounds are common, retained foreign bodies are not. Wounds with a foreign body sensation should be evaluated. The presence of wood or vegetative material, graphite or other pigmenting materials, and pain is an indication for foreign body removal. Radiography may be used to locate foreign bodies for removal, and ultrasonography can be helpful for localizing radiolucent foreign bodies. It is wise to set a time limit for exploration and to have a plan for further evaluation or referral. Injuries at high risk of infection include organic foreign bodies or dirty wounds. These should be treated with plain water irrigation and complete removal of retained fragments. In most cases, antibiotic prophylaxis is not indicated. If a patient presents with an infected wound, the possibility of a retained foreign body should be considered. Tetanus prophylaxis is necessary if there is no knowledge or documentation of tetanus immunization within 10 years, including tetanus immune globulin for the person with a dirty wound whose history of tetanus toxoid doses is unknown or incomplete.
Foreign bodies may be retained in the body through many mechanisms, including ingestion, placement in bodily orifices, and surgical errors. This article is limited to objects that have penetrated the skin. Puncture or impalement injuries are common. In the United States in 1999, there were 8.2 million emergency department visits for open wounds.1 Retained foreign bodies are not common. The authors of one study involving patients injured by broken glass found retained glass in 15 percent of wounds.2 The risk of puncture wounds and retained foreign bodies increases in warmer seasons or climates because of bare skin and outdoor recreation. Persons who work in occupations such as carpentry and the garment industry are at increased risk of impalement with nails or pins. These injuries are more common in children or adults with mental or physical impairment, which may result in behavior or lack of control that increases risk.
Although these injuries may seem minor, wounds with neglected foreign bodies are a common cause of malpractice claims.3 Any wound that penetrates the skin should be evaluated to determine if exploration for foreign bodies is needed. An accurate history of the mechanism of injury and description of the probable object can help localize the problem and determine the need for removal.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Radiography should be used to evaluate deep wounds. | B | 5 |
| Ultrasonography should be used to localize radiolucent foreign bodies. | B | 7 |
| Topical 4% liposomal lidocaine should be used for wound exploration in children. | A | 10 |
| Foreign body wounds should be cleaned with tap water. | A | 14,15 |
| Antiseptic solutions should not be used for cleansing foreign body wounds because they slow healing. | A | 16 |
| Antibiotics should be considered for human bites and bites on the hand. | A | 19 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, see page 612 orhttps://www.aafp.org/afpsort.xml.
Investigating for Possible Foreign Body
Patients may not be aware of retained material, but if there is sensation of a foreign body, it is important to explore the wound. Removal is easier if wounds are examined within 24 hours because the entry wound is visible and open. Older injuries have inflammation, induration, scarring, and/or granulated tissue, making it more difficult to localize the foreign body. The risk of infection increases with time until the wound is fully healed.
The mechanism of injury is important in evaluating for foreign bodies. Bite injuries may include teeth, and punches to the face may include tooth fragments in the punching hand. Broken objects causing wounds may leave embedded fragments. Wounds from nails or other sharp objects puncturing the foot through shoes or socks may include remnants of leather, cloth, or rubber.4
The composition of the foreign body will influence evaluation and removal. Metal objects in soft tissue pose a lower risk of infection than organic matter. Inert metal foreign bodies may not have to be removed, because removal might cause more trauma than simply leaving them in place. The decision to remove a foreign body is also based on symptoms or risk of complications. If a foreign body is producing pain, it should be removed.
Types of Foreign Bodies
SPLINTERS
Splinters are commonly from wood, thorns, or spines from plants but also may be plastic or glass. Wood and vegetative material must be removed from wounds because they are associated with increased inflammation and risk of infection. Larger or buried splinters can result in difficulty removing the entire foreign body or localizing it for removal.
FISHHOOKS
Fishhooks caught in the skin are problematic because of the barbs that are intended to keep fish on the hook. Fishhooks have a straight shank and a curved belly with a barbed point at the end. Some fishhooks have multiple barbs. Others have multiple hooks, and it is necessary to cut off the other hooks for safe removal. Most fishhook injuries occur in the hand, face or scalp, upper extremity, or foot. Fishhooks in the eyelid or eye require immediate ophthalmologic referral.
GLASS
Patients with glass embedded in a wound are more likely to report the sensation of foreign bodies. One study found that patient sensation was more likely for wounds with retained glass than for those without glass. The positive predictive value of patient sensation was 31 percent; negative predictive value was 89 percent. Although the negative predictive value was high, 57 percent of retained glass foreign bodies would have been missed without radiography.2 In patients with sensation of foreign body, superficial wounds that have been adequately explored do not require radiography. Plain films can be clinically beneficial in locating glass foreign bodies in deep wounds with or without exploration.5 In patients without sensation, the history can guide the decision for further investigation. All glass is radiopaque; however, there is limited ability for radiography to detect glass fragments smaller than 2 mm.2 Glass is inert and can be left in place if it is difficult to locate or remove.
OTHER
Pencil lead or graphite foreign bodies can result in pigment tattooing and should be removed. Metallic foreign bodies such as bullets or BBs may be removed without difficulty if superficial and distant from tendons, nerves, or blood vessels. When removal might cause damage, metallic foreign bodies can be left in place unless symptoms occur or infection is present.
Evaluation and Localization
Penetrating wounds can damage nerves or blood vessels. Evaluating patient sensation and circulation is essential. Superficial foreign bodies can sometimes be palpated or visualized. Deeper foreign bodies may require additional methods to localize. Palpation with a gloved finger should be avoided because of the risk of puncturing the glove and finger and being exposed to blood-borne diseases.
Imaging is not necessary if the foreign body is adequately visible for removal or if it does not require removal. For wounds that require imaging, appropriate modalities include radiography, computed tomography (CT), and ultrasonography, depending on the size and type of foreign body. Underpenetrated plain radiography is the most economic and available method for viewing radiopaque foreign bodies, including metal, bone, teeth, pencil graphite, certain plastics, glass, gravel, stone, some fish spines, wood, and aluminum.4 Although CT is more sensitive than radiography, the increased cost limits CT to foreign bodies that are not visible on radiography and pose a risk of infection or joint injury.6
Ultrasonography is widely available and helpful in finding wooden or radiolucent foreign bodies.7 Detection of foreign bodies with ultrasonography has a sensitivity of 50 to 90 percent and a specificity of 70 to 97 percent for gravel, metal, cactus spines, wood, and plastic.4 In one study, ultrasonography localized 19 of 21 foreign bodies not found on radiography.7 Ultrasonography can help determine the depth, size, and shape of the foreign body and its relationship to anatomic structures such as bones, tendons, blood vessels, or joints.
Many foreign bodies are surrounded by a hypoechogenic area representing inflammation.8 Localizing some foreign bodies can be easier with multiple views, metallic markers, or needles inserted close to the foreign body. Table 1 describes appropriate imaging modalities for various types of foreign bodies.4,6–8
Table 1 Imaging Modalities for Localizing Various Types of Foreign Bodies in Skin and Subcutaneous Tissue
| Computed tomography |
| Reserve for failed exploration or infection |
| Radiography |
| Bone |
| Fish spines (some) |
| Glass |
| Gravel/stone |
| Metal/aluminum |
| Pencil graphite |
| Plastic (some) |
| Teeth |
| Wood (e.g., splinters, cactus spines, thorns) |
| Ultrasonography |
| Glass |
| Metal |
| Pencil graphite |
| Plastic (some) |
| Stone |
| Wood |
Removal Techniques
Being adequately prepared for the removal of foreign bodies increases success rates and avoids complications. Wound exploration is aided by optimal lighting, magnification, and adequate hemostasis. The wound and gloves should be cleansed before removal is attempted. Anesthesia is necessary for deeply embedded fishhooks, larger splinters, or wound exploration. Local infiltration or digital block can be used depending on the location of the wound. For children, it may be beneficial to use topical anesthetics.9 Compared with a eutectic mixture of local anesthetics, 4% liposomal lidocaine has a shorter application time and longer duration of action with good pain control.10
SPLINTER REMOVAL
Foreign bodies should be removed using direct visualization rather than blind probing whenever possible. This often requires extending an incision from the entry wound. The area can then be explored by carefully spreading the soft tissue with a hemostat. If the foreign body cannot be visualized, the physician may be able to feel it with the hemostat. The foreign body can then be grasped and removed with an alligator or splinter forceps, or the soft tissue dissected over the end to visualize and remove.
If a sharp foreign body such as a needle enters the skin perpendicularly, the incision may miss the foreign body if parallel to it. One way to approach this situation is to excise an elliptical area of skin around the entry wound incision. Undermining the edges of the excision wound, the physician then applies pressure with the thumbs on both sides of the wound to try to extrude the foreign body.11
To remove a deep foreign body from fat, an elliptical incision is made around the entry wound, and the elliptical area of skin isolated by the incision is grasped with an Allis clamp (Figure 1). With gentle upward traction, incise downward from the edges toward the center on both sides until the foreign body is felt. The entire elliptical area of skin and foreign body can then be grasped and removed.11
Setting a time limit for removal is wise. If attempts are unsuccessful, physicians should consider evaluation with CT or referral to a surgeon.
Figure 1.
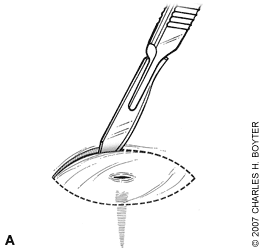
Removal of a deep foreign body.(A) Make an elliptical incision around the entry wound.(B) Grasp the elliptical area of skin with an Allis forceps.(C) With gentle upward traction, incise downward from the edges on both sides toward the center until the foreign body is felt.(D) The entire elliptical area of skin and foreign body can then be grasped and removed.
FISHHOOK REMOVAL
Because there are hundreds of different kinds of fish-hooks, the best way to know what the embedded hook is like is to see an identical sample. Several different removal techniques are used, although none have been evaluated in controlled trials.12 If the hook is embedded superficially, anesthesia may not be needed. Deeper injuries may require local infiltration with 1% lidocaine or a digital block.
The back-out, or retrograde, technique is for hooks that are not barbed. It is performed by grasping the shank of the hook with a hemostat and backing the hook out following the curve of the hook. Depending on the patient and the location of the wound, this technique may not require anesthesia. The push-through or advance-and-cut technique is equally simple. If necessary, lidocaine can be injected. The point of the hook is pushed through the skin and the barbed end of the hook is cut off with a wire cutter. The shank of the hook can then be backed out.
The needle cover technique involves introducing an 18- or 20-gauge needle to cover the barb of the hook. The physician should advance the needle, bevel toward the tip of the fishhook, along the inside curve of the hook until the barb is covered. Then the hook and needle are held firmly together and backed out simultaneously (Figure 2). This technique requires adequate anesthesia, and it works best for larger fishhooks embedded superficially.
Figure 2.

Needle cover technique to remove an embedded fishhook. (A) Advance an 18- or 20-gauge needle, bevel toward the tip of the fishhook, along the inside curve of the hook until the barb is covered. (B) Hold hook and needle firmly together and back out simultaneously.
The string technique, which may also be used by nonprofessionals, may not require anesthesia. Placing a string around the curve of the hook, the physician pulls gently along the line of the shank. The barb of the fish-hook is disengaged by pressing downward on the body of the hook. While maintaining downward pressure, the physician quickly and firmly pulls the string, freeing the tip of the hook (Figure 3).
Figure 3.

String technique to remove an embedded fishhook. (A) Place a string around the curve of the hook and pull gently along the line of the shank. (B) Disengage the barb by pressing downward on the shank of the hook. (C) While maintaining downward pressure, quickly and firmly pull the string to free the tip of the hook.
Complications
Risk of infection is determined by the length of time since the injury occurred, the type of foreign body, whether the wound was clean or dirty, and the patient's health status. Chronic or acute illness that has lowered immune status increases the risk of infection, as do bite injuries or deeper injuries that may include joint spaces, tendons, or bone. A study of traumatic lacerations found the risk of infection to be higher in older patients and those with diabetes, and in wounds that were longer, wider, deeper, jagged, with visible contamination, or with a foreign body.13
The most important way to avoid infection is to completely remove the foreign body. After removal, if the wound is large enough, it can be irrigated with drinkable tap water.14,15 In a puncture wound, injecting saline under pressure may drive contaminants further into tissue and should be avoided. Antiseptic agents such as hydrogen peroxide, chlorhexidine, and povidone iodine should not be used because they are toxic to tissue and slow the healing process.16,17
Although infection is the most common complication, with rates ranging from 1.1 to 12 percent, the use of prophylactic antibiotics is not typically recommended in nonbite wounds.18 Antibiotics may reduce the rate of infection after bites by humans and after bites on the hand.19 If a patient presents with infection following a puncture wound, he or she should be reevaluated and any retained foreign body removed, if necessary. The potential risk of bone or joint infection should be considered in the treatment of these wound infections.
Tetanus surveillance in the United States from 1998 to 2000 showed an average of 43 cases annually, with the highest incidence and most deaths in those older than 60 years.20 Surveysofemergencydepartmentpatientshave shown a 1 to 6 percent incidence of missed tetanus prophylaxis when the patient received medical care for wounds.21 In a study of 1,000 patients in an emergency department, 26 percent of those who stated they had received a tetanus immunization within five years were confirmed by medical records to have no tetanus immunization.22 The wound most often associated with tetanus (50 percent) was a puncture wound.20
All patients with significant puncture wounds should be immunized, and all patients with foreign bodies should have their tetanus status carefully reviewed and be given tetanus toxoid prophylaxis and immune globulin as appropriate. 23 Table 2 outlines the management of tetanus-prone wounds.24,25
Table 2 Management of Tetanus-Prone Wounds
| History of tetanus vaccination | Type of wound | Tetanus vaccine booster* | Tetanus immune globulin | |
|---|---|---|---|---|
| Three or more doses | ||||
| Fewer than five years since previous dose | All wounds | No | No | |
| Five to 10 years since previous dose | Clean, minor wounds | No | No | |
| All other wounds | Yes | No | ||
| More than 10 years since previous dose | All wounds | Yes | No | |
| Fewer than three doses or uncertain vaccination history | Clean, minor wounds | Yes | No | |
| All other wounds | Yes | Yes | ||
*—Use Tdap (tetanus toxoid, reduced diphtheria toxoid, and acellular pertussis [Adacel]) vaccine for adolescents 11 to 18 years of age.25
Adapted with permission from Royal Children's Hospital Melbourne. Clinical practice guidelines: management of tetanus-prone wounds. Accessed April 23, 2007, at:http://www.rch.org.au/clinicalguide/cpg.cfm?doc_id=5221, with additional information from reference 25.

