Benign prostatic hyperplasia is a common condition affecting older men. Typical presenting symptoms include urinary hesitancy, weak stream, nocturia, incontinence, and recurrent urinary tract infections. Acute urinary retention, which requires urgent bladder catheterization, is relatively uncommon. Irreversible renal damage is rare. The initial evaluation should assess the frequency and severity of symptoms and the impact of symptoms on the patient's quality of life. The American Urological Association Symptom Index is a validated instrument for the objective assessment of symptom severity. The initial evaluation should also include a digital rectal examination and urinalysis. Men with hematuria should be evaluated for bladder cancer. A palpable nodule or induration of the prostate requires referral for assessment to rule out prostate cancer. For men with mild symptoms, watchful waiting with annual reassessment is appropriate. Over the past decade, numerous medical and surgical interventions have been shown to be effective in relieving symptoms of benign prostatic hyperplasia. Alpha blockers improve symptoms relatively quickly. Although 5-alpha reductase inhibitors have a slower onset of action, they may decrease prostate size and alter the disease course. Limited evidence shows that the herbal agents saw palmetto extract, rye grass pollen extract, and pygeum relieve symptoms. Transurethral resection of the prostate often provides permanent relief. Newer laser-based surgical techniques have comparable effectiveness to transurethral resection up to two years after surgery with lower perioperative morbidity. Various outpatient surgical techniques are associated with reduced morbidity, but symptom relief may be less durable.
Benign prostatic hyperplasia (BPH) is a common condition in older men. Histologically, it is characterized by the presence of discrete nodules in the periurethral zone of the prostate gland.1 Clinical manifestations of BPH are caused by extrinsic compression of the prostatic urethra leading to impaired voiding. Chronic inability to completely empty the bladder may cause bladder distension with hypertrophy and instability of the detrusor muscle. Some patients with BPH present with hematuria. Because the severity of symptoms does not correlate with the degree of hyperplasia, and other conditions can cause similar symptoms, the clinical syndrome that often accompanies BPH has been described as lower urinary tract symptoms.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Men with suspected BPH can be evaluated with a validated questionnaire to quantify symptom severity. | C | 6 |
| In men with symptoms of BPH, a digital rectal examination and urinalysis should be performed to screen for other urologic disorders. | C | 6 |
| Watchful waiting with annual follow-up is appropriate for men with mild BPH. | C | 6, 10 |
| Alpha blockers provide symptomatic relief of moderate to severe BPH symptoms. | A | 7, 12 |
| In men with a prostate volume greater than 40 mL, 5-alpha reductase inhibitors should be considered for the treatment of BPH. | A | 8, 14 |
| Refer patients for a surgical consultation if medical therapy fails; the patient develops refractory urinary retention, persistent hematuria, or bladder stones; or the patient chooses primary surgical therapy. | C | 6, 31, 32 |
BPH = benign prostatic hyperplasia.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, see page 1360 or https://www.aafp.org/afpsort.xml.
The prevalence of BPH increases with age. One study suggests that the prevalence is 20 percent in 40-year-old men and increases to 90 percent in men in their seventies.2 The most common lower urinary tract symptoms are hesitancy, weak stream, nocturia, and incontinence. BPH may also be complicated by recurrent urinary tract infections (UTIs)3 or bladder stones.4 It is estimated that one half of all men with histologic BPH experience moderate to severe lower urinary tract symptoms.5 Acute urinary retention (the complete inability to void), which requires urgent bladder catheterization, is uncommon with an annual risk of less than 1 percent; irreversible renal insufficiency is rare.6,7 Therefore, management decisions should be based on the presence and severity of symptoms.
Diagnosis
HISTORY AND PHYSICAL EXAMINATION
In men with bothersome lower urinary tract symptoms, a history should be performed to establish the severity of symptoms, evaluate for causes other than BPH (Table 1), and identify contraindications to potential therapies. The American Urological Association (AUA) Symptom Index (Figure 1) is a validated seven-question instrument that can be used to objectively assess the severity of BPH.6
Table 1 Differential Diagnosis of Lower Urinary Tract Symptoms in Men
| Clinical finding | Possible diagnosis |
|---|---|
| Abnormal sphincter tone | Neurogenic bladder |
| Fever | Prostatitis |
| Hematuria | Bladder cancer |
| Prostate nodule or induration | Prostate cancer |
| Prostate tenderness | Prostatitis |
Figure 1. American Urological Association Symptom Index
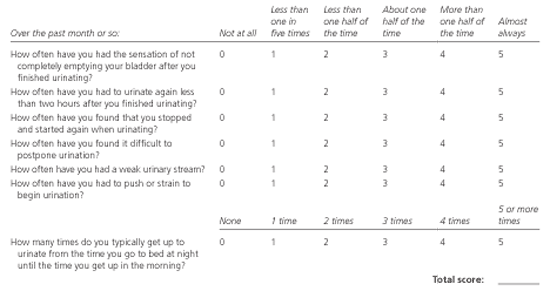
American Urological Association Symptom Index to assess severity of benign prostatic hyperplasia (BPH). A score of 7 or less indicates mild BPH; a score of 8 to 19 indicates moderate BPH; a score of 20 to 35 indicates severe BPH.
Adapted with permission from American Urological Association. Guideline on the management of benign prostatic hyperplasia (BPH). http://www.auanet.org/guidelines/bph.cfm. Accessed September 19, 2007.
Several classes of medications may cause or exacerbate lower urinary tract symptoms, and comorbidities may contribute to these symptoms (Table 2). Previous surgical procedures may increase the risk of urethral strictures or other anatomic abnormalities. Black men and first-degree relatives of patients with prostate cancer have an increased risk of prostate cancer.1
Table 2 Medications and Medical Conditions That May Contribute to Lower Urinary Tract Symptoms in Men
| Factor | Mechanism |
|---|---|
| Medications | |
| Antihistamines | Decreased parasympathetic tone |
| Decongestants | Increased sphincter tone via alpha1-adrenergic receptor stimulation |
| Diuretics | Increased urine production |
| Opiates | Impaired autonomic function |
| Tricyclic antidepressants | Anticholinergic effects |
| Medical conditions | |
| Bladder cancer | Mechanical obstruction |
| Congestive heart failure | Diuresis |
| Diabetes | Osmotic diuresis, autonomic neuropathy |
| Parkinson's disease | Autonomic neuropathy |
| Prostate cancer | Mechanical obstruction |
Symptomatic men should have a digital rectal examination to assess the size and contour of the prostate.6 Prostate volume predicts the response to finasteride (Proscar) therapy. Finasteride is more effective if the prostate volume is greater than 40 mL8 (the normal prostate volume is 20 to 30 mL). A palpable nodule suggests prostate cancer and requires biopsy. Abnormal sphincter tone suggests a neurologic abnormality, which may contribute to urinary symptoms.6 Cognitive or ambulatory impairment may exacerbate incontinence problems.
LABORATORY STUDIES
The AUA recommends urinalysis for all men presenting with lower urinary tract symptoms.6 Normal urinalysis findings help rule out non-BPH causes of the symptoms, such as bladder cancer, bladder stones, UTI, or urethral strictures. Prostate-specific antigen (PSA) levels should be measured in men who have at least a 10-year life expectancy and who would be a candidate for prostate cancer treatment. PSA levels correlate with the risk of symptom progression; men with elevated PSA levels respond better to finasteride.8 PSA levels also correlate with prostate volume, which may affect the treatment choice, if indicated. PSA levels greater than 1.6 ng per mL (1.6 mcg per L) for men in their fifties, 2.0 ng per mL (2.0 mcg per L) for men in their sixties, and 2.3 ng per mL (2.3 mcg per L) for men in their seventies are 70 percent sensitive and 70 percent specific for a prostate volume greater than 40 mL.9
Urine cytology should be obtained in men at risk of bladder cancer (e.g., those with a history of tobacco use, irritative bladder symptoms, or hematuria). Routine measurement of serum creatinine levels is not recommended because BPH does not appear to affect the baseline risk of renal disease.6
Treatment
WATCHFUL WAITING
A randomized trial of medical therapies for patients with moderate to severe BPH showed that the placebo group had clinical progression (i.e., a four-point or more increase in AUA Severity Index score, an episode of acute urinary retention, or recurrent UTI) at a rate of 4.5 per 100 patient-years during a mean follow-up period of 4.5 years.7 The rate of acute urinary retention was 0.6 per 100 patient-years. No cases of renal insufficiency were attributed to BPH.
Watchful waiting is recommended in men who have mild symptoms (AUA Symptom Index score of 7 or less) or who do not perceive their symptoms to be particularly bothersome. Patients who choose this approach should be monitored annually for symptom progression.10
ALPHA BLOCKERS
Smooth muscles in the prostate gland contract in response to alpha-adrenergic receptor stimulation, causing constriction of the prostatic urethra. Alpha1-receptor antagonists improve lower urinary tract symptoms by promoting smooth muscle relaxation. Three of these agents (i.e., doxazosin [Cardura], terazosin [Hytrin], and prazosin [Minipress]) also lower blood pressure through their action on vascular smooth muscles. Although these three agents are indicated for hypertension, they are less effective than thiazide diuretics and angiotensin-converting enzyme inhibitors in preventing adverse cardiovascular outcomes, and they should not be considered first-line antihypertensive agents.11 Tamsulosin (Flomax) and alfuzosin (Uroxatral) are more selective agents for treating constriction of prostatic smooth muscles; they have no effect on blood pressure.
Alpha blockers relieve symptoms in men with moderate to severe BPH.7,12 A randomized trial comparing terazosin, finasteride, and placebo showed significant symptom reduction in patients receiving terazosin compared with patients in the other groups.12 Combination therapy with terazosin and finasteride was no more effective than terazosin alone. Participants in this trial had lower prostate volumes than those in trials showing benefit with finasteride.
A more recent trial comparing doxazosin, finasteride, and placebo showed that doxazosin was more effective than placebo in reducing clinical progression (number needed to treat [NNT] = 14 patients over four years).7 The benefit of doxazosin was driven by improvements in symptom scores. Doxazosin delayed the occurrence of acute urinary retention, but did not significantly decrease its overall incidence; however, the trial was underpowered for this end point. The benefit of doxazosin monotherapy was comparable to finasteride monotherapy, although combination therapy was more effective than either agent alone.7 Symptom improvement is typically noted within two to four weeks of initiating alpha-blocker therapy.10
Alpha blockers may cause orthostatic hypotension. Therapy with nonselective agents should begin at a low dose and then be titrated upward. The risk of orthostatic hypotension is increased when these agents are combined with phosphodiesterase inhibitors used to treat erectile dysfunction; therefore, low starting doses and cautious titration are advised when these agents are used in combination. Sildenafil (Viagra) in doses greater than 25 mg should not be taken within four hours of alpha-blocker use.13
5-ALPHA REDUCTASE INHIBITORS
Prostate growth is stimulated by androgenic hormones, especially dihydrotestoster-one.1 Finasteride and dutasteride (Avodart) inhibit the conversion of testosterone to dihydrotestosterone, suppressing prostate growth.13 These agents appear to be most beneficial when the prostate volume is 40 mL or greater.8 The 5-alpha reductase inhibitors do not provide immediate symptom relief, and approximately six months of therapy is required to achieve clinical benefit.10 Unlike alpha blockers, 5-alpha reductase inhibitors have been shown to affect the clinical course of BPH, reducing the risk of acute urinary retention (NNT = 26) and surgical intervention (NNT = 18) four years after therapy.14 Adverse effects of finasteride include decreased libido, ejaculatory dysfunction, and erectile dysfunction.15
The Prostate Cancer Prevention Trial raised questions about the long-term safety of finasteride.16 The trial showed that men treated with finasteride for seven years had a lower overall incidence of prostate cancer (NNT = 17); however, the incidence of high-grade cancer (Gleason score of 7 or more) was slightly increased in the finasteride group (number needed to harm = 77). The significance of this finding is unclear because finasteride may cause artifactual changes in prostate cancer histology.17 However, patients considering finasteride therapy should be aware of the possible increased risk of high-grade prostate cancer. Finasteride decreases PSA levels; therefore, when screening for prostate cancer, the measured PSA level should be doubled to correct for this effect.18
Medical therapies for BPH are summarized in Table 3.
Table 3 Medical Therapies for Benign Prostatic Hyperplasia
| Medication | Dosage | Cost per month (generic)* | Comments | |
|---|---|---|---|---|
| Alpha blockers | ||||
| Doxazosin (Cardura) | Start at 1 mg daily; maximum 8 mg daily | $45 (26 to 28) | Risk of orthostatic hypotension | |
| Prazosin (Minipress) | Start at 1 mg twice daily; maximum 5 mg three times daily | 39 (18 to 24) | ||
| Terazosin (Hytrin) | Start with 1 mg taken at bedtime; maximum 20 mg taken at bedtime | 68 (18 to 20) | ||
| Selective alpha blockers | ||||
| Alfuzosin (Uroxatral) | 10 mg daily | 77 (—) | No effect on resting blood pressure; risk of orthostatic hypotension | |
| Tamsulosin (Flomax) | 0.4 mg daily | 77 (—) | ||
| 5-alpha reductase inhibitors | ||||
| Dutasteride (Avodart) | 0.5 mg daily | 96 (—) | Six months of treatment is needed to achieve | |
| Finasteride (Proscar) | 5 mg daily | 100 (94) | symptom relief | |
*— Estimated cost to the pharmacist based on average wholesale prices (rounded to the nearest dollar) in Red Book. Montvale, NJ: Medical Economics Data; 2007. Cost to the patient will be higher, depending on prescription filling fee.
ALTERNATIVE THERAPIES
Saw palmetto plant (Serenoa repens) extract has been used to treat BPH-related lower urinary tract symptoms. A European study showed that one half of German urologists preferred saw palmetto over pharmaceutical agents for treatment of BPH in their patients.19 A Cochrane review concluded that saw palmetto produces mild to moderate improvement in urinary symptoms and flow measures, which is comparable to finasteride.20 However, a more recent high-quality, randomized controlled trial found no benefit with saw palmetto in symptom relief or urinary flow measures after one year of therapy (participants had an average prostate volume of 34 mL).21 If saw palmetto's effect is mediated by 5-alpha reductase inhibition, these patients may not be optimal candidates because 5-alpha reductase inhibitors are most beneficial when the prostate size is greater than 40 mL.8
Cochrane reviews of rye grass pollen extract (Cernilton)22 and pygeum23 found evidence that each agent provides modest symptomatic improvement. However, the studies analyzed were limited by small size, short duration, and lack of standardization. The AUA does not recommend the use of phytotherapy.6
Transurethral Resection of the Prostate
Surgical treatment of BPH (Table 46,24–30) may be appropriate if medical treatment fails or the patient develops refractory urinary retention, persistent hematuria, or bladder stones.6,31,32 Transurethral resection of the prostate (TURP) is considered the benchmark for surgical therapies because its effectiveness is supported by the most extensive data.6 A randomized trial comparing TURP with watchful waiting showed a reduction in symptoms and complications in men who underwent surgery.33
Table 4 Surgical Techniques for the Treatment of Benign Prostatic Hyperplasia
| Technique | Setting | Cost24 | Comments |
|---|---|---|---|
| TURP | Inpatient | High initial cost may be offset by long-term durability of symptom relief | Common complications include hemorrhage, sexual dysfunction, strictures, and hyponatremia caused by absorption of the hypotonic irrigant; TURP is considered the benchmark for surgical therapies |
| Laser prostatectomy | Inpatient | High initial cost may be offset by long-term durability of symptom relief | Less perioperative morbidity and comparable clinical results after two years as TURP; steep learning curve for surgeons |
| Transurethral incision of the prostate | Outpatient or overnight hospitalization | Lower initial cost, but retreatment may be needed | Less risk of retrograde ejaculation than with TURP |
| Transurethral microwave therapy | Outpatient | Lower initial cost, but retreatment may be needed | No need for general anesthesia |
| Transurethral needle ablation | Outpatient | Lower initial cost, but retreatment may be needed | No need for general anesthesia |
TURP = transurethral resection of the prostate.
Although TURP provides definitive relief in most patients, a recent trial showed that two out of 30 patients who underwent TURP required reoperation within two years.25 Common complications of TURP include sexual dysfunction, strictures, hemorrhage, and the TURP syndrome (i.e., hyponatremia caused by absorption of the hypotonic irrigant).26
Newer Surgical Techniques
Newer surgical techniques are intended to provide symptomatic relief while avoiding the morbidity associated with traditional TURP. A Cochrane review concluded that laser prostatectomy is an effective alternative to TURP.34 Holmium: YAG laser enucleation of the prostate, an inpatient surgical procedure, is associated with reduced catheterization time and hospital stay compared with traditional TURP; urodynamic and quality of life scores are similar to TURP after 24 months.25 Although holmium: YAG laser enucleation is associated with retrograde ejaculation, it has minimal effect on potency, libido, or patient satisfaction with sex life.35
Several outpatient procedures are also available, but they have not proved to be as effective as TURP. Transurethral needle ablation is an outpatient procedure in which radio frequency energy is used to remove periurethral prostate tissue. It is suitable for men with mild to moderate symptoms and a prostate volume less than 60 mL.27 Although transurethral needle ablation is not associated with significant morbidity, the rate of treatment failure is reportedly 23 percent at five years28 and 83 percent at 10 years.29
Transurethral incision of the prostate is appropriate in men with smaller prostates (volume less than 30 mL).26 Although it is less likely than TURP to cause retrograde ejaculation (35 versus 68 percent),30 a meta-analysis found less improvement in urodynamic parameters and a nonsignificant trend toward higher reoperation rates with transurethral incision.36 A randomized trial found that transurethral microwave therapy and TURP provided comparable symptom relief after five years, but retreatment rates were higher with transurethral microwave therapy.37 Ultimately, the choice of a surgical procedure depends on the estimated risk of complications from general anesthesia and on patient and surgeon preference.

