
Am Fam Physician. 2009;79(7):583-587
Author disclosure: Nothing to disclose.
Epididymitis and orchitis are commonly seen in the outpatient setting. Men between 14 and 35 years of age are most often affected, and Chlamydia trachomatis and Neisseria gonorrhoeae are the most common pathogens in this age group. In other age groups, coliform bacteria are the primary pathogens. Men with epididymitis and orchitis typically present with a gradual onset of scrotal pain and symptoms of lower urinary tract infection, including fever. This presentation helps differentiate epididymitis and orchitis from testicular torsion, which is a surgical emergency. Typical physical findings include a swollen, tender epididymis or testis located in the normal anatomic position with an intact ipsilateral cremasteric reflex. Laboratory studies, including urethral Gram stain, urinalysis and culture, and polymerase chain reaction assay for C. trachomatis and N. gonorrhoeae, help guide therapy. Initial outpatient therapy is empirical and targets the most common pathogens. When C. trachomatis and N. gonorrhoeae are suspected, ceftriaxone and doxycycline are recommended. When coliform bacteria are suspected, ofloxacin or levofloxacin is recommended.
Epididymitis and orchitis are inflammation of the epididymis and testes, respectively, with or without infection. These conditions can be subclassified as acute, subacute, or chronic based on symptom duration. In acute epididymitis, symptoms are present for less then six weeks and are characterized by pain and swelling. Chronic epididymitis is characterized by pain, generally without swelling, that persists for more than three months. Orchitis usually occurs when the inflammation from the epididymis spreads to the adjacent testicle.
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| If testicular torsion is suspected, the patient should receive urgent referral to a urologist for possible surgery. | C | 12 |
| Most patients with epididymitis and orchitis can be treated in an outpatient setting with close follow-up. | C | 2–4 |
| If epididymitis is thought to be caused by gonococcal or chlamydial infection, treatment should include ceftriaxone (Rocephin), a single 250-mg dose intramuscularly, and doxycycline (Vibramycin), 100 mg orally twice daily for 10 days. Azithromycin (Zithromax), a single 1-g dose orally, may be substituted for doxycycline if treatment compliance is questionable. | C | 12 |
| If epididymitis is thought to be caused by enteric organisms (e.g., coliform bacteria), treatment should include ofloxacin (Floxin; brand no longer available in the United States), 300 mg orally twice daily for 10 days, or levofloxacin (Levaquin), 500 mg orally once daily for 10 days. | C | 12 |
Epidemiology
In 2002, epididymitis or orchitis accounted for 1 in 144 outpatient visits (0.69 percent) in men 18 to 50 years of age.1 There are approximately 600,000 cases of epididymitis per year in the United States, most of which occur in men between 18 and 35 years of age.1 In one study of U.S. Army soldiers, the incidence was highest in men between 20 and 29 years of age.2 In a review of 121 patients with epididymitis in the ambulatory setting, a bimodal distribution was noted with the peak incidence occurring in men 16 to 30 years of age and 51 to 70 years of age.3
Etiology and Pathophysiology
Epididymitis is the most common cause of intrascrotal inflammation,5 and retrograde ascent of pathogens is the usual route of infection. Although epididymitis was historically thought to be caused by chemical irritation from urine reflux, a study published in 1979 showed that bacteria were responsible for most cases.6 The study also showed that the type of bacteria varied with patient age.
In men 14 to 35 years of age, epididymitis is most commonly caused by sexually transmitted Neisseria gonorrhoeae or Chlamydia trachomatis infection.7,8 Nonspecific bacterial epididymitis is caused by various aerobic bacteria and is often associated with anatomic abnormalities. In those younger than 14 years or older than 35 years, epididymitis is generally caused by infection with common urinary tract pathogens, such as Escherichia coli. In men who practice insertive anal intercourse, coliform bacteria (e.g., E. coli) are common causative pathogens, although Haemophilus influenzae infection has also been linked. Other pathogens that are less commonly associated with epididymitis include Ureaplasma urealyticum, Proteus mirabilis, Klebsiella pneumoniae, and Pseudomonas aeruginosa. Epididymitis secondary to Mycobacterium tuberculosis infection is rare but must be considered among those at high risk. In patients with human immunodeficiency virus (HIV) or acquired immunodeficiency syndrome, fungal and viral etiologies, including cytomegalovirus, have been reported.7,8
Noninfectious etiologies of epididymitis have been identified in numerous groups. One study found that the annual incidence of epididymitis in boys two to 13 years of age is 1.2 per 1,000, and that the condition in this age group is primarily a postinfectious inflammatory reaction to pathogens (e.g., Mycoplasma pneumoniae, enteroviruses, adenoviruses) that follows a benign course.9 Other noninfectious causes of epididymitis include vasculitides and certain medications, such as amiodarone (Cardarone).10
Risk factors for epididymitis in all men include sexual activity, strenuous physical activity, bicycle or motorcycle riding, and prolonged periods of sitting (e.g., during travel, with a sedentary job).1,3,4 Risk factors in men older than 35 years and in prepubertal boys include recent urinary tract surgery or instrumentation and anatomic abnormalities, such as prostatic obstruction in older men and posterior urethral valves or meatal stenosis in prepubertal boys.1,2,4,5
With the exception of viral diseases, genitourinary tract infections seldom primarily involve the testis. Orchitis usually occurs in patients with concurrent epididymitis, and the causative pathogens of the conditions are similar. Blood-borne dissemination is the major route of isolated testicular infection. Mumps is the most common cause of viral orchitis (orchitis occurs in 20 to 30 percent of men with mumps infection).11 Pyogenic orchitis usually is caused by an inflammatory process in the epididymis.
Diagnosis
HISTORY AND PHYSICAL EXAMINATION
When evaluating patients with acute testicular or scrotal pain and swelling (acute scrotum), there should be a high index of suspicion for testicular torsion. In fact, testicular torsion is most commonly misdiagnosed as epididymitis. Any patient with acute scrotum and any patient in whom testicular torsion is otherwise suspected should receive urgent referral to a urologist for possible surgery.12 Table 1 presents the selected differential diagnosis of acute scrotum.13–15
| Condition | Typical presentation | Examination findings | Ultrasound findings |
|---|---|---|---|
| Epididymitis | Gradual onset of pain that occasionally radiates to the lower abdomen; symptoms of lower urinary tract infection | Localized epididymal tenderness that progresses to testicular swelling and tenderness; normal cremasteric reflex; pain relief with testicular elevation (Prehn sign) | Enlarged, thickened epididymis with increased blood flow on color Doppler |
| Orchitis | Abrupt onset of testicular pain | Testicular swelling and tenderness; normal cremasteric reflex | Testicular masses or swollen testicles with hypoechoic and hypervascular areas |
| Testicular torsion | Acute onset of pain, usually severe | High-riding transversely oriented testis; abnormal cremasteric reflex; pain with testicular elevation | Normal-appearing testis with decreased blood flow on color Doppler |
Patients with epididymitis usually present with gradual onset of pain that is localized posterior to the testis and that occasionally radiates to the lower abdomen. Although patients often have unilateral pain that begins in the epididymis, the pain can spread to the adjacent testis. Symptoms of lower urinary tract infection, such as fever, frequency, urgency, hematuria, and dysuria, may be present. These symptoms are common with epididymitis and orchitis but are rare with testicular torsion. Recurrent pain is rare with epididymitis and torsion of the appendix testis (upper pole of testis), but can occur with testicular torsion (caused by intermittent torsion with spontaneous resolution).16 The presence or absence of nausea and vomiting is not helpful in differentiating between epididymitis or orchitis and testicular torsion because it may occur with any of the conditions. Viral orchitis is associated with the abrupt onset of scrotal pain and swelling and is primarily unilateral. When associated with mumps infection, orchitis generally appears four to seven days after the development of parotitis.
Although testicular torsion can occur at any age, the incidence is highest between 12 and 18 years, followed by the neonatal period. Torsion is rare in those older than 35 years and, with the exception of the neonatal period, in those younger than eight years. Torsion of the appendix testis usually occurs between seven and 14 years of age and is rare in those older than 20 years.
Patients with epididymitis and orchitis often have tachycardia or fever. Patients may also be uncomfortable while seated, but this is also common with testicular torsion. It is important to check for costovertebral angle tenderness, a sign of concomitant pyelonephritis, and for signs of cystitis by palpating the suprapubic region. The inguinal area should be examined for a hernia or for swollen and tender lymph nodes, which are suggestive of the inflammatory or infectious process of epididymitis and orchitis. The scrotum should be examined for a tender spermatic cord, which is suggestive of epididymitis.
A high-riding, transversely oriented testis is common with testicular torsion,17 whereas the testis is usually in its normal anatomic location with epididymitis and orchitis. Early testicular swelling and tenderness that progress to a reactive hydrocele and scrotal wall erythema is common with testicular torsion. With epididymitis, the epididymis (located posterolateral to the testis) is tender and swollen and often indurated. In later stages, this may progress to testicular swelling (orchitis) with a reactive hydrocele and scrotal wall erythema that mimic testicular torsion. Scrotal swelling also occurs with indirect inguinal hernias, and bowel sounds may be auscultated in the scrotum.
With torsion of the appendix testis, a reactive hydrocele is often present and tenderness is correlated with the anatomic position of the appendix testis. The “blue dot” sign, a bluish discoloration in the area of the appendix testis, may be present on the scrotal wall, indicating infarction and necrosis. The cremasteric reflex, elicited by stroking the skin of the upper medial thigh, should always be evaluated. A normal reflex (i.e., ipsilateral cremasteric muscle contraction producing unilateral testis elevation) is present with epididymitis or orchitis and torsion of the appendix testis, but is almost always absent with testicular torsion.4,18,19 Prehn sign, the relief of pain with the elevation of the testis, may be elicited in patients with epididymitis, although this is not a reliable finding.18,20 Elevation of the testis usually exacerbates the pain of testicular torsion.
DIAGNOSTIC TESTING
In addition to a careful history and physical examination, diagnostic studies can help confirm epididymitis and orchitis and detect the causative pathogen. Diagnostic testing can also identify patients with a tumor or testicular torsion, but referral to a urologist should not be delayed to obtain imaging if testicular torsion is clinically suspected.
A Gram stain and culture of swabbed urethral discharge are recommended to detect urethritis and gonococcal infection. Urinalysis and urine culture should also be obtained, preferably on first-void urine samples. The presence of leukocyte esterase and white blood cells is suggestive of urethritis and helps to differentiate epididymitis from testicular torsion. If epididymitis is suspected, polymerase chain reaction assays for C. trachomatis and N. gonorrhoeae should be performed on urethral swab or urine specimens.
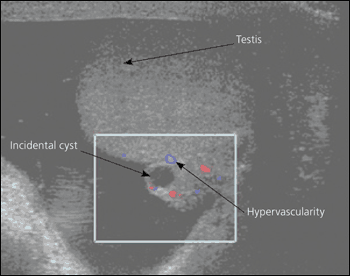
If testicular torsion is clinically probable based on history and physical examination findings, urgent referral to a urologist is warranted. Otherwise, in nearly all patients with suspected epididymitis, color Doppler ultrasonography is needed to rule out testicular torsion by documenting blood flow.13,14 Color Doppler ultrasonography assesses perfusion of the testis and anatomy of the scrotal contents (Figure 1). A normal-appearing testicle with markedly decreased Doppler wave pulsation (decreased blood flow) suggests torsion, whereas an enlarged, thickened epididymis with increased Doppler wave pulsation (increased blood flow) suggests epididymitis. In children, color Doppler ultrasonography has been shown to have a sensitivity of 70 percent and a specificity of 88 percent for epididymitis, and a sensitivity of 82 percent and a specificity of 100 percent for testicular torsion.15
Measurement of acute phase proteins, such as C-reactive protein (CRP) levels and erythrocyte sedimentation rate, have been shown to be useful in differentiating epididymitis from testicular torsion in patients with acute scrotum. In one study, CRP had a sensitivity and specificity for epididymitis of 96.2 and 94.2 percent, respectively.21 If the diagnosis remains unclear, referral and surgical exploration of the scrotum is warranted. Referral should not be delayed pending results of these tests if testicular torsion is clinically suspected.
Treatment
Empiric treatment of epididymitis should be initiated based on likely pathogens, before laboratory testing is complete. Treatment focuses on curing infection, improving symptoms, preventing transmission, and reducing future complications. If gonococcal or chlamydial infection is likely (patients 14 to 35 years of age), treatment should consist of ceftriaxone (Rocephin), a single 250-mg dose intramuscularly, and doxycycline (Vibramycin), 100 mg orally twice daily for 10 days.7,12,13 Azithromycin (Zithromax), a single 1-g dose orally, may be substituted for doxycycline if treatment compliance is questionable.13 If enteric organisms, such as coliform bacteria, are likely (patients younger than 14 years or older than 35 years) or the patient is allergic to cephalosporins or tetracyclines, treatment should include ofloxacin (Floxin; brand no longer available in the United States), 300 mg orally twice daily for 10 days, or levofloxacin (Levaquin), 500 mg orally once daily for 10 days.7,12,13 Patients who are immunocompromised (e.g., those with HIV) should receive the same treatment as those who are immunocompetent.
In addition to antibiotic treatment, analgesics, scrotal elevation, limitation of activity, and use of cold packs are helpful in the treatment of epididymitis. Patients should be advised of possible complications, including sepsis, abscess, infertility, and extension of the infection. Epididymitis and orchitis usually can be treated in the outpatient setting with close follow-up.2–4 Inpatient care is recommended for intractable pain, vomiting (because of the inability to take oral antibiotics), suspicion of abscess, failure of outpatient care, or signs of sepsis.
Orchitis treatment is mostly supportive and should include bed rest and the use of hot or cold packs for pain. Antibacterial medications are not indicated for the treatment of viral orchitis, and most cases of mumps-associated orchitis resolve spontaneously after three to 10 days. Epididymoorchitis requires appropriate antibiotic coverage, as with epididymitis.
Follow-up
Follow-up is recommended three to seven days after initial evaluation and initiation of treatment to evaluate for clinical improvement and for the presence of a testicular mass.4,22 With treatment, pain typically improves within one to three days, but it may take two to four weeks for induration to fully resolve. Prepubescent boys with epididymitis need a urology referral because of the high incidence of urogenital abnormalities.23 Men older than 50 years should be evaluated for urethral obstruction secondary to prostatic enlargement. Because epididymitis in men 14 to 35 years of age is most commonly caused by gonococcal or chlamydial infection, the need for screening tests and treatment of comorbid sexually transmitted infections, for the patient and his sex partners, should be discussed in this population. The importance of completing the full course of antibiotic treatment and condom use to prevent disease should be emphasized.