The geriatric assessment is a multidimensional, multidisciplinary assessment designed to evaluate an older person's functional ability, physical health, cognition and mental health, and socioenvironmental circumstances. It is usually initiated when the physician identifies a potential problem. Specific elements of physical health that are evaluated include nutrition, vision, hearing, fecal and urinary continence, and balance. The geriatric assessment aids in the diagnosis of medical conditions; development of treatment and follow-up plans; coordination of management of care; and evaluation of long-term care needs and optimal placement. The geriatric assessment differs from a standard medical evaluation by including nonmedical domains; by emphasizing functional capacity and quality of life; and, often, by incorporating a multidisciplinary team. It usually yields a more complete and relevant list of medical problems, functional problems, and psychosocial issues. Well-validated tools and survey instruments for evaluating activities of daily living, hearing, fecal and urinary continence, balance, and cognition are an important part of the geriatric assessment. Because of the demands of a busy clinical practice, most geriatric assessments tend to be less comprehensive and more problem-directed. When multiple concerns are presented, the use of a “rolling” assessment over several visits should be considered.
Approximately one-half of the ambulatory primary care for adults older than 65 years is provided by family physicians,1 and approximately 22 percent of visits to family physicians are from older adults.2,3 It is estimated that older adults will comprise at least 30 percent of patients in typical family medicine outpatient practices, 60 percent in hospital practices, and 95 percent in nursing home and home care practices.4
A complete assessment is usually initiated when the physician detects a potential problem such as confusion, falls, immobility, or incontinence. However, older persons often do not present in a typical manner, and atypical responses to illness are common. A patient presenting with confusion may not have a neurologic problem, but rather an infection. Social and psychological factors may also mask classic disease presentations. For example, although 30 percent of adults older than 85 years have dementia, many physicians miss the diagnosis.5,6 Thus, a more structured approach to assessment can be helpful.
The geriatric assessment is a multidimensional, multidisciplinary assessment designed to evaluate an older person's functional ability, physical health, cognition and mental health, and socioenvironmental circumstances. It includes an extensive review of prescription and over-the-counter drugs, vitamins, and herbal products, as well as a review of immunization status. This assessment aids in the diagnosis of medical conditions; development of treatment and follow-up plans; coordination of management of care; and evaluation of long-term care needs and optimal placement.
The geriatric assessment differs from a typical medical evaluation by including nonmedical domains; by emphasizing functional capacity and quality of life; and, often, by incorporating a multidisciplinary team including a physician, nutritionist, social worker, and physical and occupational therapists. This type of assessment often yields a more complete and relevant list of medical problems, functional problems, and psychosocial issues.7
Because of the demands of a busy clinical practice, most geriatric assessments tend to be less comprehensive and more problem-directed. For older patients with many concerns, the use of a “rolling” assessment over several visits should be considered. The rolling assessment targets at least one domain for screening during each office visit. Patient-driven assessment instruments are also popular. Having patients complete questionnaires and perform specific tasks not only saves time, but also provides useful insight into their motivation and cognitive ability.
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References |
|---|---|---|
| The U.S. Preventive Services Task Force found insufficient evidence to recommend for or against screening with ophthalmoscopy in asymptomatic older patients. | C | 15 |
| Patients with chronic otitis media or sudden hearing loss, or who fail any hearing screening tests should be referred to an otolaryngologist. | C | 21, 23 |
| Hearing aids are the treatment of choice for older patients with hearing impairment, because they minimize hearing loss and improve daily functioning. | A | 23 |
| The U.S. Preventive Services Task Force has advised routinely screening women 65 years and older for osteoporosis with dual-energy x-ray absorptiometry of the femoral neck. | A | 37 |
| The Centers for Medicare and Medicaid Services encourages the use of the Beers criteria as part of an older patient's medication assessment to reduce adverse effects. | C | 39, 40 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Functional Ability
Functional status refers to a person's ability to perform tasks that are required for living. The geriatric assessment begins with a review of the two key divisions of functional ability: activities of daily living (ADL) and instrumental activities of daily living (IADL). ADL are self-care activities that a person performs daily (e.g., eating, dressing, bathing, transferring between the bed and a chair, using the toilet, controlling bladder and bowel functions). IADL are activities that are needed to live independently (e.g., doing housework, preparing meals, taking medications properly, managing finances, using a telephone). Physicians can acquire useful functional information by simply observing older patients as they complete simple tasks, such as unbuttoning and buttoning a shirt, picking up a pen and writing a sentence, taking off and putting on shoes, and climbing up and down from an examination table. Two instruments for assessing ADL and IADL include the Katz ADL scale (Table 1)8 and the Lawton IADL scale (Table 2).9 Deficits in ADL and IADL can signal the need for more in-depth evaluation of the patient's socioenvironmental circumstances and the need for additional assistance.
Table 1 Katz Index of Independence in Activities of Daily Living

| Activities (1 or 0 points) | Independence (1 point)* | Dependence (0 points)† | |
|---|---|---|---|
| Bathing | Bathes self completely or needs help in bathing only a single part of the body, such as the back, genital area, or disabled extremity | Needs help with bathing more than one part of the body, getting in or out of the bathtub or shower; requires total bathing | |
| Points:______ | |||
| Dressing | Gets clothes from closets and drawers, and puts on clothes and outer garments complete with fasteners; may need help tying shoes | Needs help with dressing self or needs to be completely dressed | |
| Points:______ | |||
| Toileting | Goes to toilet, gets on and off, arranges clothes, cleans genital area without help | Needs help transferring to the toilet and cleaning self, or uses bedpan or commode | |
| Points:______ | |||
| Transferring | Moves in and out of bed or chair unassisted; mechanical transfer aids are acceptable | Needs help in moving from bed to chair or requires a complete transfer | |
| Points:______ | |||
| Fecal and urinary continence | Exercises complete self-control over urination and defecation | Is partially or totally incontinent of bowel or bladder | |
| Points:______ | |||
| Feeding | Gets food from plate into mouth without help; preparation of food may be done by another person | Needs partial or total help with feeding or requires parenteral feeding | |
| Points:______ | |||
| Total points‡: _________ | |||
*—No supervision, direction, or personal assistance.
†—With supervision, direction, personal assistance, or total care.
‡—Score of 6 = high (patient is independent); score of 0 = low (patient is very dependent).
Adapted with permission from Katz S, Downs TD, Cash HR, Grotz RC. Progress in development of the index of ADL. Gerontologist. 1970;10(1):23.
Table 2 Lawton Instrumental Activities of Daily Living Scale (Self-Rated Version)

| For each question, circle the points for the answer that best applies to your situation. | |||
| 1. Can you use the telephone? | |||
| Without help | 3 | ||
| With some help | 2 | ||
| Completely unable to use the telephone | 1 | ||
| 2. Can you get to places that are out of walking distance? | |||
| Without help | 3 | ||
| With some help | 2 | ||
| Completely unable to travel unless special arrangements are made | 1 | ||
| 3. Can you go shopping for groceries? | |||
| Without help | 3 | ||
| With some help | 2 | ||
| Completely unable to do any shopping | 1 | ||
| 4. Can you prepare your own meals? | |||
| Without help | 3 | ||
| With some help | 2 | ||
| Completely unable to prepare any meals | 1 | ||
| 5. Can you do your own housework? | |||
| Without help | 3 | ||
| With some help | 2 | ||
| Completely unable to do any housework | 1 | ||
| 6. Can you do your own handyman work? | |||
| Without help | 3 | ||
| With some help | 2 | ||
| Completely unable to do any handyman work | 1 | ||
| 7. Can you do your own laundry? | |||
| Without help | 3 | ||
| With some help | 2 | ||
| Completely unable to do any laundry | 1 | ||
| 8a. Do you use any medications? | |||
| Yes (If “yes,” answer question 8b) | 1 | ||
| No (If “no,” answer question 8c) | 2 | ||
| 8b. Do you take your own medication? | |||
| Without help (in the right doses at the right time) | 3 | ||
| With some help (take medication if someone prepares it for you or reminds you to take it) | 2 | ||
| Completely unable to take own medication | 1 | ||
| 8c. If you had to take medication, could you do it? | |||
| Without help (in the right doses at the right time) | 3 | ||
| With some help (take medication if someone prepares it for you or reminds you to take it) | 2 | ||
| Completely unable to take own medication | 1 | ||
| 9. Can you manage your own money? | |||
| Without help | 3 | ||
| With some help | 2 | ||
| Completely unable to handle money | 1 | ||
note: Scores have meaning only for a particular patient (e.g., declining scores over time reveal deterioration). Some questions may be sex-specific and can be modified by the interviewer.
Adapted with permission from Lawton MP, Brody EM. Assessment of older people: self-maintaining and instrumental activities of daily living. Gerontologist. 1969;9(3):181.
Physical Health
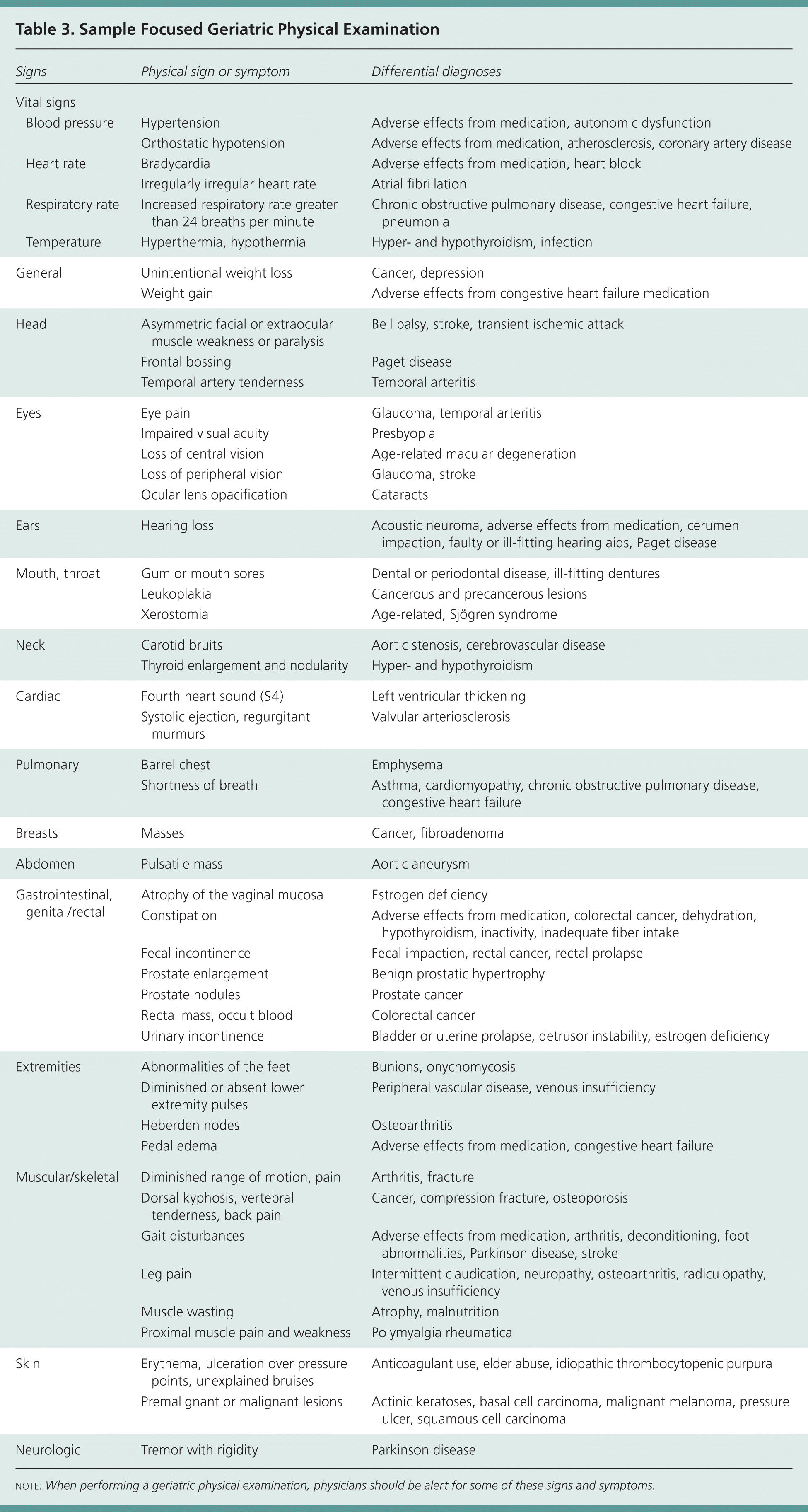
The geriatric assessment incorporates all facets of a conventional medical history, including main problem, current illness, past and current medical problems, family and social history, demographic data, and a review of systems. The approach to the history and physical examination, however, should be specific to older persons. In particular, topics such as nutrition, vision, hearing, fecal and urinary continence, balance and fall prevention, osteoporosis, and polypharmacy should be included in the evaluation. Table 3 is an example of a focused geriatric physical examination.
Table 3 Sample Focused Geriatric Physical Examination
| Signs | Physical sign or symptom | Differential diagnoses | |
|---|---|---|---|
| Vital signs | |||
| Blood pressure | Hypertension | Adverse effects from medication, autonomic dysfunction | |
| Orthostatic hypotension | Adverse effects from medication, atherosclerosis, coronary artery disease | ||
| Heart rate | Bradycardia | Adverse effects from medication, heart block | |
| Irregularly irregular heart rate | Atrial fibrillation | ||
| Respiratory rate | Increased respiratory rate greater than 24 breaths per minute | Chronic obstructive pulmonary disease, congestive heart failure, pneumonia | |
| Temperature | Hyperthermia, hypothermia | Hyper- and hypothyroidism, infection | |
| General | Unintentional weight loss | Cancer, depression | |
| Weight gain | Adverse effects from congestive heart failure medication | ||
| Head | Asymmetric facial or extraocular muscle weakness or paralysis | Bell palsy, stroke, transient ischemic attack | |
| Frontal bossing | Paget disease | ||
| Temporal artery tenderness | Temporal arteritis | ||
| Eyes | Eye pain | Glaucoma, temporal arteritis | |
| Impaired visual acuity | Presbyopia | ||
| Loss of central vision | Age-related macular degeneration | ||
| Loss of peripheral vision | Glaucoma, stroke | ||
| Ocular lens opacification | Cataracts | ||
| Ears | Hearing loss | Acoustic neuroma, adverse effects from medication, cerumen impaction, faulty or ill-fitting hearing aids, Paget disease | |
| Mouth, throat | Gum or mouth sores | Dental or periodontal disease, ill-fitting dentures | |
| Leukoplakia | Cancerous and precancerous lesions | ||
| Xerostomia | Age-related, Sjögren syndrome | ||
| Neck | Carotid bruits | Aortic stenosis, cerebrovascular disease | |
| Thyroid enlargement and nodularity | Hyper- and hypothyroidism | ||
| Cardiac | Fourth heart sound (S4) | Left ventricular thickening | |
| Systolic ejection, regurgitant murmurs | Valvular arteriosclerosis | ||
| Pulmonary | Barrel chest | Emphysema | |
| Shortness of breath | Asthma, cardiomyopathy, chronic obstructive pulmonary disease, congestive heart failure | ||
| Breasts | Masses | Cancer, fibroadenoma | |
| Abdomen | Pulsatile mass | Aortic aneurysm | |
| Gastrointestinal, genital/rectal | Atrophy of the vaginal mucosa | Estrogen deficiency | |
| Constipation | Adverse effects from medication, colorectal cancer, dehydration, hypothyroidism, inactivity, inadequate fiber intake | ||
| Fecal incontinence | Fecal impaction, rectal cancer, rectal prolapse | ||
| Prostate enlargement | Benign prostatic hypertrophy | ||
| Prostate nodules | Prostate cancer | ||
| Rectal mass, occult blood | Colorectal cancer | ||
| Urinary incontinence | Bladder or uterine prolapse, detrusor instability, estrogen deficiency | ||
| Extremities | Abnormalities of the feet | Bunions, onychomycosis | |
| Diminished or absent lower extremity pulses | Peripheral vascular disease, venous insufficiency | ||
| Heberden nodes | Osteoarthritis | ||
| Pedal edema | Adverse effects from medication, congestive heart failure | ||
| Muscular/skeletal | Diminished range of motion, pain | Arthritis, fracture | |
| Dorsal kyphosis, vertebral tenderness, back pain | Cancer, compression fracture, osteoporosis | ||
| Gait disturbances | Adverse effects from medication, arthritis, deconditioning, foot abnormalities, Parkinson disease, stroke | ||
| Leg pain | Intermittent claudication, neuropathy, osteoarthritis, radiculopathy, venous insufficiency | ||
| Muscle wasting | Atrophy, malnutrition | ||
| Proximal muscle pain and weakness | Polymyalgia rheumatica | ||
| Skin | Erythema, ulceration over pressure points, unexplained bruises | Anticoagulant use, elder abuse, idiopathic thrombocytopenic purpura | |
| Premalignant or malignant lesions | Actinic keratoses, basal cell carcinoma, malignant melanoma, pressure ulcer, squamous cell carcinoma | ||
| Neurologic | Tremor with rigidity | Parkinson disease | |
note: When performing a geriatric physical examination, physicians should be alert for some of these signs and symptoms.
SCREENING FOR DISEASE
In the normal aging process, there is often a decline in physiologic function that is usually not disease-related. However, treatment of diabetes mellitus, hypertension, and glaucoma can prevent significant future morbidity. Screening for malignancies may allow for early detection, and some are curable if treated early. It is important that physicians weigh the potential harms of screening before screening older patients. It is essential to consider family preferences regarding treatment if a disease is detected, and the patient's functional status, comorbid conditions, and predicted life expectancy. If an asymptomatic patient has an expected survival of more than five years, screening is generally medically warranted, assuming that the patient is at risk of the disease and would accept treatment if early disease was detected.10,11
The Agency for Healthcare Research and Quality has developed an online tool called the Electronic Preventive Services Selector (http://epss.ahrq.gov/ePSS/search.jsp) that can be downloaded to smartphones. It can assist physicians in identifying age-appropriate screening measures.
NUTRITION
A nutritional assessment is important because inadequate micronutrient intake is common in older persons. Several age-related medical conditions may predispose patients to vitamin and mineral deficiencies. Studies have shown that vitamins A, C, D, and B12; calcium; iron; zinc; and other trace minerals are often deficient in the older population, even in the absence of conditions such as pernicious anemia or malabsorption.12 There are four components specific to the geriatric nutritional assessment: (1) nutritional history performed with a nutritional health checklist; (2) a record of a patient's usual food intake based on 24-hour dietary recall; (3) physical examination with particular attention to signs associated with inadequate nutrition or overconsumption; and (4) select laboratory tests, if applicable. One simple screening tool for nutrition in older persons is the Nutritional Health Checklist (Table 4).13 Table 4Nutritional Health Checklist
Statement
Yes
I have an illness or condition that made me change the kind or amount of food I eat.
2
I eat fewer than two meals per day.
3
I eat few fruits, vegetables, or milk products.
2
I have three or more drinks of beer, liquor, or wine almost every day.
2
I have tooth or mouth problems that make it hard for me to eat.
2
I don't always have enough money to buy the food I need.
4
I eat alone most of the time.
1
I take three or more different prescription or over-the-counter drugs per day.
1
Without wanting to, I have lost or gained 10 lb in the past six months.
2
I am not always physically able to shop, cook, or feed myself.
2
note: The Nutritional Health Checklist was developed for the Nutrition Screening Initiative. Read the statements above, and circle the number in the “yes” column for each statement that applies to you. Add up the circled numbers to get your nutritional score.
scoring
0 to 2 = You have good nutrition. Recheck your nutritional score in six months.
3 to 5 = You are at moderate nutritional risk, and you should see what you can do to improve your eating habits and lifestyle. Recheck your nutritional score in three months.
6 or more = You are at high nutritional risk, and you should bring this checklist with you the next time you see your physician, dietitian, or other qualified health care professional. Talk with any of these professionals about the problems you may have. Ask for help to improve your nutritional status.
Adapted with permission from The clinical and cost-effectiveness of medical nutrition therapies: evidence and estimates of potential medical savings from the use of selected nutritional intervention. June 1996. Summary report prepared for the Nutrition Screening Initiative, a project of the American Academy of Family Physicians, the American Dietetic Association, and the National Council on the Aging, Inc.
VISION
The most common causes of vision impairment in older persons include presbyopia, glaucoma, diabetic retinopathy, cataracts, and age-related macular degeneration.14 The U.S. Preventive Services Task Force (USPSTF) found insufficient evidence to recommend for or against screening with ophthalmoscopy in asymptomatic older patients.15 In 1995, the Canadian Task Force on the Periodic Health Examination advised primary care physicians to use a Snellen chart to screen for visual acuity, and recommended that older patients who have had diabetes for at least five years have an assessment by an ophthalmologist. Additionally, the task force advised that patients at high risk of glaucoma, including black persons and those with a positive family history, diabetes, or severe myopia, undergo periodic assessment by an ophthalmologist.16
HEARING
Presbycusis is the third most common chronic condition in older Americans, after hypertension and arthritis.17 The USPSTF is updating its 1996 recommendations, but currently recommends screening older patients for hearing impairment by periodically questioning them about their hearing.18 Audioscope examination, otoscopic examination, and the whispered voice test are also recommended. The whispered voice test is performed by standing approximately 3 ft behind the patient and whispering a series of letters and numbers after exhaling to assure a quiet whisper. Failure to repeat most of the letters and numbers indicates hearing impairment.19 As part of the Medicare-funded initial preventive physical examination, physicians are encouraged to use hearing screening questionnaires to evaluate an older patient's functional ability and level of safety.20 Questionnaires such as the screening version of the Hearing Handicap Inventory for the Elderly accurately identify persons with hearing impairment21 (Table 522 ). Additionally, patients' medications should be examined for potentially ototoxic drugs. Patients with chronic otitis media or sudden hearing loss, or who fail any screening tests should be referred to an otolaryngologist.21,23 Hearing aids are the treatment of choice for older persons with hearing impairment, because they minimize hearing loss and improve daily functioning.23
Table 5 Screening Version of the Hearing Handicap Inventory for the Elderly

| Question | Yes (4 points) | Sometimes (2 points) | No (0 points) |
|---|---|---|---|
| Does a hearing problem cause you to feel embarrassed when you meet new people? | _____ | _____ | ______ |
| Does a hearing problem cause you to feel frustrated when talking to members of your family? | ______ | ______ | ______ |
| Do you have difficulty hearing when someone speaks in a whisper? | ______ | ______ | ______ |
| Do you feel impaired by a hearing problem? | ______ | ______ | ______ |
| Does a hearing problem cause you difficulty when visiting friends, relatives, or neighbors? | ______ | ______ | ______ |
| Does a hearing problem cause you to attend religious services less often than you would like? | ______ | ______ | ______ |
| Does a hearing problem cause you to have arguments with family members? | ______ | ______ | ______ |
| Does a hearing problem cause you difficulty when listening to the television or radio? | ______ | ______ | ______ |
| Do you feel that any difficulty with your hearing limits or hampers your personal or social life? | ______ | ______ | ______ |
| Does a hearing problem cause you difficulty when in a restaurant with relatives or friends? | ______ | ______ | ______ |
| Raw score (sum of the points assigned to each of the items) | ______ |
note: A raw score of 0 to 8 = 13 percent probability of hearing impairment (no handicap/no referral); 10 to 24 = 50 percent probability of hearing impairment (mild to moderate handicap/referral); 26 to 40 = 84 percent probability of hearing impairment (severe handicap/referral).
Adapted with permission from Ventry IM, Weinstein BE. Identification of elderly people with hearing problems. ASHA. 1983;25(7):42.
URINARY CONTINENCE
Urinary incontinence, the unintentional leakage of urine, affects approximately 15 million persons in the United States, most of whom are older.24 Urinary incontinence has important medical repercussions and is associated with decubitus ulcers, sepsis, renal failure, urinary tract infections, and increased mortality. Psychosocial implications of incontinence include loss of self-esteem, restriction of social and sexual activities, and depression. Additionally, incontinence is often a key deciding factor for nursing home placement.25 An assessment for urinary incontinence should include the evaluation of fluid intake, medications, cognitive function, mobility, and previous urologic surgeries.14 The single best question to ask when diagnosing urge incontinence is, “Do you have a strong and sudden urge to void that makes you leak before reaching the toilet?” (positive likelihood ratio = 4.2; negative likelihood ratio = 0.48). A good question to ask when diagnosing stress incontinence is, “Is your incontinence caused by coughing, sneezing, lifting, walking, or running?” (positive likelihood ratio = 2.2; negative likelihood ratio = 0.39).26
BALANCE AND FALL PREVENTION
Impaired balance in older persons often manifests as falls and fall-related injuries. Approximately one-third of community-living older persons fall at least once per year, with many falling multiple times.27,28 Falls are the leading cause of hospitalization and injury-related death in persons 75 years and older.29
The Tinetti Balance and Gait Evaluation is a useful tool to assess a patient's fall risk.28,30 This test involves observing as a patient gets up from a chair without using his or her arms, walks 10 ft, turns around, walks back, and returns to a seated position. This entire process should take less than 16 seconds. Those patients who have difficulty performing this test have an increased risk of falling and need further evaluation.31
Older persons can decrease their fall risk with exercise, physical therapy, a home hazard assessment, and withdrawal of psychotropic medications. Guidelines addressing fall prevention in older persons living in nursing homes have been published by the American Medical Directors Association and the American Geriatrics Society.32,33
OSTEOPOROSIS
Osteoporosis may result in low-impact or spontaneous fragility fractures, which can lead to a fall.14 Osteoporosis can be diagnosed clinically or radiographically.34 It is most commonly diagnosed by dual-energy x-ray absorptiometry of the total hip, femoral neck, or lumbar spine, with a T-score of –2.5 or below.35,36 The USPSTF has advised routinely screening women 65 years and older for osteoporosis with dual-energy x-ray absorptiometry of the femoral neck.37
POLYPHARMACY
Polypharmacy, which is the use of multiple medications or the administration of more medications than clinically indicated, is common in older persons. Among older adults, 30 percent of hospital admissions and many preventable problems, such as falls and confusion, are believed to be related to adverse drug effects.38 The Centers for Medicare and Medicaid Services encourages the use of the Beers criteria, which list medication and medication classes that should be avoided in older persons, as part of an older patient's medication assessment to reduce adverse effects.39,40 In 2003, a consensus panel of experts revised the criteria.41 The Beers criteria can be found at http://www.dcri.duke.edu/ccge/curtis/beers.html.
Cognition and Mental Health
DEPRESSION
The USPSTF recommends screening adults for depression if systems of care are in place.42 Of the several validated screening instruments for depression, the Geriatric Depression Scale and the Hamilton Depression Scale are the easiest to use and most widely accepted.43 However, a simple two-question screening tool (“During the past month, have you been bothered by feelings of sadness, depression, or hopelessness?” and “Have you often been bothered by a lack of interest or pleasure in doing things?”) is as effective as these longer scales.43,44 Responding in the affirmative to one or both of these questions is a positive screening test for depression that requires further evaluation.
DEMENTIA
Early diagnosis of dementia allows patients timely access to medications and helps families to make preparations for the future. It can also help in the management of other symptoms that often accompany the early stages of dementia, such as depression and irritability. As few as 50 percent of dementia cases are diagnosed by physicians.45 There are several screening tests available to assess cognitive dysfunction; however, the Mini-Cognitive Assessment Instrument is the preferred test for the family physician because of its speed, convenience, and accuracy, as well as the fact that it does not require fluency in English (Table 646,47 ).
Table 6 Mini-Cognitive Assessment Instrument

| Step 1. Ask the patient to repeat three unrelated words, such as “ball,” “dog,” and “window.” |
| Step 2. Ask the patient to draw a simple clock set to 10 minutes after eleven o'clock (11:10). A correct response is drawing of a circle with the numbers placed in approximately the correct positions, with the hands pointing to the 11 and 2. |
| Step 3. Ask the patient to recall the three words from Step 1. One point is given for each item that is recalled correctly. |
| Interpretation |
Adapted with permission from Ebell MH. Brief screening instruments for dementia in primary care. Am Fam Physician. 2009;79(6):500, with additional information from reference 47.
Socioenvironmental Circumstances
According to the U.S. Census Bureau, approximately 70 percent of noninstitutionalized adults 65 years and older live with their spouses or extended family, and 30 percent live alone.48 Determining the most suitable living arrangements for older patients is an important function of the geriatric assessment. Although options for housing for older persons vary widely, there are three basic types: private homes in the community, assisted living residences, and skilled nursing facilities (e.g., rehabilitation hospitals, nursing homes). Factors affecting the patient's socioenvironmental circumstances include their social interaction network, available support resources, special needs, and environmental safety.
Problem List
As assessment data are obtained, they need to be recorded to allow all members of the health care team to easily access the information. The family physician can generate a problem list that includes any condition or event requiring new or ongoing care; the medical, nutritional, functional, and social implications; and proposed interventions. This type of assessment allows older patients to benefit from an interdisciplinary team that is effectively assessing and actively managing their health care.

