Vitamin B12 (cobalamin) deficiency is a common cause of megaloblastic anemia, a variety of neuropsychiatric symptoms, and elevated serum homocysteine levels, especially in older persons. There are a number of risk factors for vitamin B12 deficiency, including prolonged use of metformin and proton pump inhibitors. No major medical organizations, including the U.S. Preventive Services Task Force, have published guidelines on screening asymptomatic or low-risk adults for vitamin B12 deficiency, but high-risk patients, such as those with malabsorptive disorders, may warrant screening. The initial laboratory assessment of a patient with suspected vitamin B12 deficiency should include a complete blood count and a serum vitamin B12 level. Measurements of serum vitamin B12 may not reliably detect deficiency, and measurement of serum homocysteine and/or methylmalonic acid should be used to confirm deficiency in asymptomatic high-risk patients with low normal levels of vitamin B12. Oral administration of high-dose vitamin B12 (1 to 2 mg daily) is as effective as intramuscular administration in correcting the deficiency, regardless of etiology. Because crystalline formulations are better absorbed than naturally occurring vitamin B12, patients older than 50 years and strict vegetarians should consume foods fortified with vitamin B12 and vitamin B12 supplements, rather than attempting to get vitamin B12 strictly from dietary sources. Administration of vitamin B12 to patients with elevated serum homocysteine levels has not been shown to reduce cardiovascular outcomes in high-risk patients or alter the cognitive decline of patients with mild to moderate Alzheimer disease.
Vitamin B12 (cobalamin) is a water-soluble vitamin that is crucial to normal neurologic function, red blood cell production, and DNA synthesis. Vitamin B12 is essential for three enzymatic processes: the conversion of homocysteine to methionine; the conversion of methylmalonic acid to succinyl coenzyme A; and the conversion of 5-methyltetrahydrofolate to tetrahydrofolate, a process necessary for DNA synthesis and red blood cell production.1 It cannot be manufactured by humans and must be regularly obtained from the ingestion of animal proteins or fortified cereal products. Gastric acid liberates vitamin B12 from animal proteins, after which it combines with intrinsic factor produced by gastric parietal cells and is absorbed in the terminal ileum.
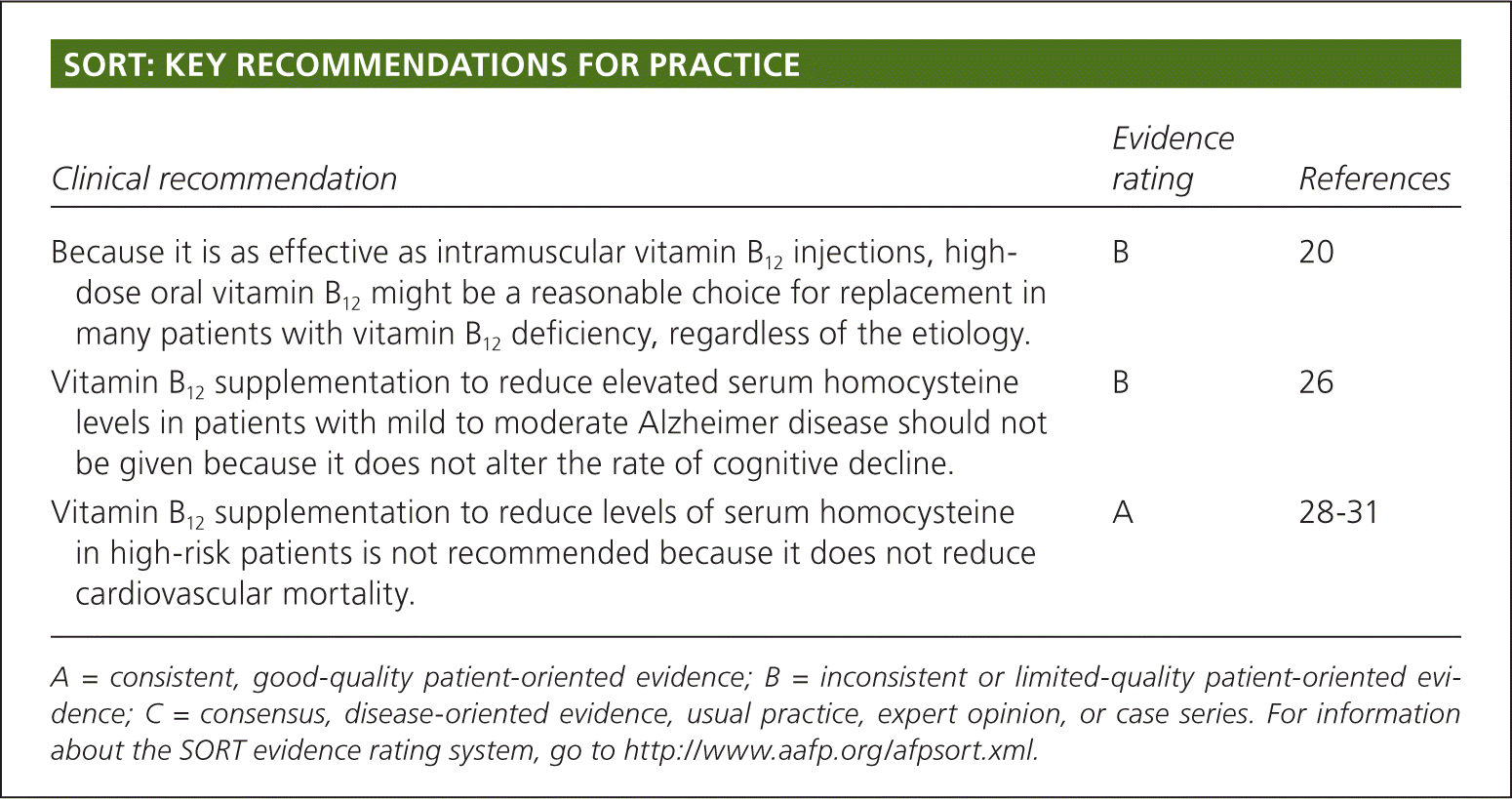
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Because it is as effective as intramuscular vitamin B12 injections, high-dose oral vitamin B12 might be a reasonable choice for replacement in many patients with vitamin B12 deficiency, regardless of the etiology. | B | 20 |
| Vitamin B12 supplementation to reduce elevated serum homocysteine levels in patients with mild to moderate Alzheimer disease should not be given because it does not alter the rate of cognitive decline. | B | 26 |
| Vitamin B12 supplementation to reduce levels of serum homocysteine in high-risk patients is not recommended because it does not reduce cardiovascular mortality. | A | 28–31 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Pernicious anemia, which is characterized by an autoimmune-mediated chronic atrophic gastritis, is a classically described cause of vitamin B12 deficiency2; other common causes include postsurgical malabsorption, dietary deficiencies, and vitamin B12 malabsorption from food.3 Because of extensive hepatic stores of vitamin B12, there may be a five- to 10-year delay between the onset of deficiency and the appearance of clinical symptoms.4
In asymptomatic patients with low-normal levels of vitamin B12 (200 to 350 pg per mL [147.56 to 258.23 pmol per L]), elevated levels of the precursor compounds homocysteine and methylmalonic acid may prompt a decision to supplement patients with vitamin B12.5
The true prevalence of vitamin B12 deficiency is difficult to estimate because reports are based on values that vary because of inclusion criteria and individual laboratory methodology. In 1994, the Framingham Heart Study reported the prevalence of vitamin B12 deficiency, as defined by a serum vitamin B12 level less than 200 pg per mL and elevated levels of serum homocysteine, methylmalonic acid, or both, to be 12 percent among 548 community-dwelling older patients.6 However, most deficient patients did not have hematologic manifestations, and neurologic manifestations were not assessed. According to unpublished data from the National Health and Nutrition Examination Survey, 3.2 percent of U.S. adults older than 50 years are estimated to have a serum vitamin B12 level less than 200 pg per mL.1 Risk factors for vitamin B12 deficiency are listed in Table 1.1–3,6,7
Table 1. Risk Factors for Vitamin B12 Deficiency

| Decreased ileal absorption |
| Crohn disease |
| Ileal resection |
| Tapeworm infestation |
| Decreased intrinsic factor |
| Atrophic gastritis |
| Pernicious anemia |
| Postgastrectomy syndrome (includes Roux-en-Y gastric bypass) |
| Genetic |
| Transcobalamin II deficiency |
| Inadequate intake |
| Alcohol abuse |
| Older persons |
| Vegetarians (includes exclusively breastfed children of vegetarian mothers) |
| Prolonged medication use |
| Histamine H2 blockers |
| Metformin (Glucophage) |
| Proton pump inhibitors |
Of particular interest to family physicians, an association between metformin (Glucophage) use and vitamin B12 deficiency has been observed. A multicenter trial of 390 patients with diabetes mellitus receiving insulin therapy who were randomized to receive metformin, 850 mg three times daily, or placebo assessed the risk of vitamin B12 deficiency and low vitamin B12 levels over four years.7 Compared with placebo, patients taking metformin had an increased risk of vitamin B12 deficiency (number needed to harm = 14 per 4.3 years) and low vitamin B12 levels (number needed to harm = 9 per 4.3 years). The effect increased with the duration of therapy. Although it is not known if prophylactic vitamin B12 supplementation prevents deficiency, it seems prudent to monitor vitamin B12 levels periodically in patients taking metformin.
Manifestations
Table 2. Clinical Manifestations of Vitamin B12 Deficiency
Although the classic hematologic expression of vitamin B12 deficiency is a megaloblastic macrocytic anemia characterized by an elevated mean corpuscular volume and mean corpuscular hemoglobin, and a peripheral smear containing macroovalocytes and hypersegmented neutrophils, up to 28 percent of affected patients may have a normal hemoglobin level, and up to 17 percent may have a normal mean corpuscular volume.8 Although folate deficiency may also produce a megaloblastic anemia, it is less common in the United States because of required folate fortification of enriched grain and cereal products.9 Clinical manifestations of megaloblastic anemia include pallor, tachycardia, weakness, fatigue, and palpitations. The evaluation and management of macrocytosis has been recently reviewed in American Family Physician (https://www.aafp.org/afp/2009/0201/p203.html).
Unlike hematologic manifestations, the specific mechanism by which vitamin B12 deficiency affects the neurologic system is unknown. Common neurologic manifestations include paresthesias, weakness, gait abnormalities, and cognitive or behavioral changes.
Vitamin B12 crosses the placenta and is present in breast milk. Pregnant women with low or marginal levels of vitamin B12 are at increased risk of having children with neural tube defects.10 Exclusively breastfed children of mothers with vitamin B12 deficiency are at increased risk of failure to thrive, hypotonia, ataxia, developmental delays, anemia, and general weakness.11 Women at high risk of or with known vitamin B12 deficiency should supplement with vitamin B12 while pregnant or breastfeeding.12,13
Screening and Laboratory Assessment
Currently, the U.S. Preventive Services Task Force does not have published guidelines on screening asymptomatic adults for vitamin B12 deficiency.14 Other major medical organizations do not have any recommendations for screening low-risk patients. Family physicians should consider screening patients who have any risk factors listed in Table 1.1–3,6,7
The initial laboratory assessment of a patient with suspected vitamin B12 deficiency should include a complete blood count and a serum vitamin B12 level. Several coexisting conditions may falsely lower serum B12 levels, including oral contraceptive use, multiple myeloma, pregnancy, and folate deficiency.15 In contrast, falsely normal levels may be seen in patients with liver disease, myeloproliferative disorders, or renal disease.15 Although many research studies and clinical laboratories define vitamin B12 deficiency at a level of less than 150 pg per mL (110.67 pmol per L), or in some cases 200 pg per mL, patients with values above these levels may be symptomatic and benefit from treatment.1 Vitamin B12 levels greater than 350 pg per mL seem to be protective against symptoms of vitamin B12 deficiency.15,16
In patients with clinical symptoms of vitamin B12 deficiency and low levels of serum vitamin B12, no further confirmatory testing is generally needed before treatment is initiated. Verification with serum methylmalonic acid and/or serum homocysteine level may be necessary in asymptomatic patients with high-risk conditions, symptomatic patients with low-normal levels of vitamin B12 (200 to 350 pg per mL), or symptomatic patients in whom vitamin B12 deficiency is unlikely but must be excluded. Elevated levels of serum homocysteine and methylmalonic acid have been shown to be highly sensitive markers for vitamin B12 deficiency. Testing is widely available,5,8 but expensive, and multiple conditions may falsely elevate serum homocysteine and methylmalonic acid levels (Table 3).15 Because serum methylmalonic acid level is as sensitive as, but more specific than, serum homocysteine level for vitamin B12 deficiency, it is the confirmatory test of choice.8,15 Serum holotranscobalamin level, which is reduced in vitamin B12 deficiency, compared favorably with homocysteine and methylmalonic acid levels as a confirmatory test in one study, but further trials are needed before its widespread use for this purpose can be recommended.17
Table 3. Causes of Falsely Elevated Serum Homocysteine and Methylmalonic Acid Levels

| Homocysteine |
| Familial hyperhomocysteinemia |
| Folate deficiency |
| Levodopa therapy |
| Renal insufficiency |
| Methylmalonic acid |
| Renal insufficiency |
| Volume depletion |
Information from reference 15.
Pernicious anemia should be suspected in patients without an obvious cause of malabsorption or who have a coexisting autoimmune disorder, such as vitiligo or thyroiditis. The Schilling test, which was previously used to diagnose pernicious anemia, is no longer available in the United States, and testing for elevated levels of anti-intrinsic factor antibodies and elevated serum gastrin or pepsinogen is recommended.18 Because of the association between pernicious anemia and a higher incidence of gastric cancer and carcinoids, it is important to pursue a diagnosis and, if confirmed, recommend endoscopy.19
Treatment
Treatment of clinical vitamin B12 deficiency has traditionally been accomplished by intramuscular injection of crystalline vitamin B12 at a dosage of 1 mg weekly for eight weeks, followed by 1 mg monthly for life.1,2 In a 2005 Cochrane review, patients who received high dosages of oral vitamin B12 (1 to 2 mg daily) for 90 to 120 days had an improvement in serum vitamin B12 similar to patients who received intramuscular injections of vitamin B12.20 These results were consistent in patients regardless of the etiology of their vitamin B12 deficiency, including malabsorption states and pernicious anemia. Given the lower cost and ease of administration of oral vitamin B12, this might be a reasonable choice for replacement in many patients. In cases of megaloblastic anemia, reticulocytosis generally occurs within a few days, and the hematocrit generally normalizes over several weeks.21 Advanced neurologic symptoms may not respond to replacement.1 Vitamin B12 has been demonstrated to be safe in doses up to 1,000 times the recommended dietary allowance and is safe in pregnancy.21 The bioavailability of sublingual vitamin B12 appears to be equivalent to oral vitamin B12, but there is no evidence that sublingual delivery offers any advantage over oral preparations.22
There are no clinical guidelines for the treatment of subclinical vitamin B12 deficiency (asymptomatic patients with decreased levels of vitamin B12 and elevated levels of homocysteine and/or methylmalonic acid). Physicians may opt to treat these patients and monitor for improvement of metabolic markers, particularly in populations at high risk of clinical vitamin B12 deficiency, or observe these patients and periodically reassess their levels of vitamin B12, homocysteine, and/or methylmalonic acid. Patients with subclinical vitamin B12 deficiency will need at least 1 mg of vitamin B12 daily.20,23
Prevention
The Institute of Medicine estimates that adults younger than 50 years absorb approximately 50 percent of dietary vitamin B12, and that between 10 and 30 percent of older patients may not be able to absorb adequate amounts from normal dietary sources.21 The Institute of Medicine recommends daily consumption of 2.4 mcg of vitamin B12 in adults older than 18 years to prevent vitamin B12 deficiency. Because crystalline formulations are better absorbed than naturally occurring vitamin B12, patients older than 50 years should consume foods fortified with vitamin B12 and vitamin B12 supplements, rather than attempting to get vitamin B12 strictly from dietary sources. Strict vegetarians must obtain their vitamin B12 from supplements or consumption of fortified cereal products to prevent deficiency.21 Because of the high incidence of vitamin B12 deficiency in patients undergoing gastric bypass surgery, daily prophylactic supplementation with 1 mg is recommended.18,24
Special Considerations
The American Academy of Neurology Practice Parameter on dementia lists vitamin B12 deficiency as a common comorbidity in older persons and recommends routine assessment of vitamin B12 levels in older patients with dementia.25 No trials have specifically addressed the effects of treatment of vitamin B12 deficiency on dementia prevention or treatment. Trials have evaluated elevated homocysteine levels as a focus for potential treatment with vitamin B12 but did not note if the participants were also vitamin B12 deficient. Although treatment lowered serum homocysteine levels compared with placebo, no effect was seen on the progression of cognitive decline in patients with mild to moderate Alzheimer disease26 or in preserving cognitive function in healthy adults.27 Thus, it remains uncertain how vitamin B12 deficiency may be linked to dementia and what the potential benefits are of treatment with supplementation.
There has been a great deal of interest in the link between elevated levels of homocysteine, a direct consequence of vitamin B12 deficiency, and cardiovascular disease. No studies have directly evaluated the cardiovascular effects of correcting vitamin B12 deficiency in patients with known cardiovascular disease, although numerous studies have failed to demonstrate that correction of hyperhomocysteinemia itself reduces cardiovascular mortality or cardiovascular complications.28–31 The routine use of vitamin B12 to lower levels of serum homocysteine in patients at high risk of cardiovascular events is not recommended.
Data Sources: A PubMed search was completed using the key terms vitamin B12 deficiency and cobalamin deficiency. Also searched were the Cochrane database and the National Guideline Clearinghouse database. Search date: July 2010.


