Am Fam Physician. 2016;94(2):97-105
Patient information: See related handout on acute sinusitis, written by the authors of this article.
Author disclosure: No relevant financial affiliations.
Acute rhinosinusitis is one of the most common conditions that physicians treat in ambulatory care. Most cases of acute rhinosinusitis are caused by viral upper respiratory infections. A meta-analysis based on individual patient data found that common clinical signs and symptoms were not effective for identifying patients with rhinosinusitis who would benefit from antibiotics. C-reactive protein and erythrocyte sedimentation rate are somewhat useful tests for confirming acute bacterial maxillary sinusitis. Four signs and symptoms that significantly increase the likelihood of a bacterial cause when present are double sickening, purulent rhinorrhea, erythrocyte sedimentation rate greater than 10 mm per hour, and purulent secretion in the nasal cavity. Although cutoffs vary depending on the guideline, antibiotic therapy should be considered when rhinosinusitis symptoms fail to improve within seven to 10 days or if they worsen at any time. First-line antibiotics include amoxicillin with or without clavulanate. Current guidelines support watchful waiting within the first seven to 10 days after upper respiratory symptoms first appear. Evidence on the use of analgesics, intranasal corticosteroids, and saline nasal irrigation for the treatment of acute rhinosinusitis is poor. Nonetheless, these therapies may be used to treat symptoms within the first 10 days of upper respiratory infection. Radiography is not recommended in the evaluation of uncomplicated acute rhinosinusitis. For patients who do not respond to treatment, computed tomography of the sinuses without contrast media is helpful to evaluate for possible complications or anatomic abnormalities. Referral to an otolaryngologist is indicated when symptoms persist after maximal medical therapy and if any rare complications are suspected.
Symptoms of acute rhinosinusitis manifest when the mucosal lining in the paranasal sinuses and nasal cavity becomes inflamed. Because the nasal mucosa is contiguous with mucosa of the paranasal sinuses, inflammation of the sinuses rarely occurs without inflammation of the nasal mucosa. Although this process is commonly called sinusitis, rhinosinusitis is the more accurate term. Each year in the United States, rhinosinusitis affects one in seven adults, resulting in more than 30 million annual diagnoses.1 Rhinosinusitis is the fifth most common diagnosis for which antibiotics are prescribed in the United States.1–3 The management of acute and chronic sinusitis has a direct cost of more than $11 billion per year, not including the economic impact of lost productivity due to illness.1

| Recommendation | Sponsoring organizations |
|---|---|
| Avoid prescribing antibiotics in the emergency department for uncomplicated sinusitis. | American College of Emergency Physicians |
| Do not routinely obtain radiographic imaging for patients who meet diagnostic criteria for uncomplicated acute rhinosinusitis. | American Academy of Otolaryngology–Head and Neck Surgery |
| Do not routinely prescribe antibiotics for acute, mild to moderate sinusitis unless symptoms (which must include purulent nasal secretions and maxillary pain or facial and dental tenderness to percussion) last at least seven days or symptoms worsen after initial clinical improvement. | American Academy of Allergy, Asthma and Immunology |
| American Academy of Family Physicians | |
| American Academy of Otolaryngology–Head and Neck Surgery |
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| For patients with acute rhinosinusitis, diagnostic imaging is not recommended unless a complication or alternative diagnosis is suspected. | C | 1, 3, 4, 10, 11, 18, 19 |
| In uncomplicated acute bacterial rhinosinusitis, watchful waiting (without antibiotics) is an appropriate initial management strategy when there is assurance of follow-up. | A | 1, 22–25 |
| In patients with rhinosinusitis, antibiotic therapy is recommended if symptoms persist seven days or more with no clinical improvement or if symptoms worsen at any time. | C | 1, 3, 25 |
| Amoxicillin with or without clavulanate is the first-line antibiotic for most patients with acute bacterial rhinosinusitis. | A | 1–3, 25 |
| Doxycycline or a respiratory fluoroquinolone (levofloxacin [Levaquin] or moxifloxacin [Avelox]) may be used as an alternative to amoxicillin for treating bacterial rhinosinusitis in patients who are allergic to penicillin. | C | 1, 3 |
| Mild rhinosinusitis symptoms lasting fewer than 10 days can be managed with supportive care, including analgesics, intranasal corticosteroids, and saline nasal irrigation. | A | 1, 3, 32, 33 |
Definition
The American Academy of Otolaryngology–Head and Neck Surgery (AAO-HNS) classifies rhinosinusitis into subtypes based on symptom duration. Acute rhinosinusitis refers to symptoms lasting less than four weeks; subacute, four to 12 weeks3; and chronic, more than 12 weeks.1,4 Acute rhinosinusitis is further categorized as bacterial or viral.
Etiology
Acute bacterial rhinosinusitis is caused by various factors (Table 1).5,6 However, it is most often the result of a viral etiology associated with upper respiratory infection.1–4,7 Sinus mucosa edema, sinus ostia obstruction, and decreased mucociliary activity are three key factors in the pathophysiology of rhinosinusitis. As a result, secretions stagnate, providing a favorable environment for bacterial growth.1,2,5 In adult patients with suspected acute maxillary sinusitis following a viral upper respiratory infection, about one-half were found to have pus or mucopus in the sinus aspirate, and one-third had bacterial pathogens growing in culture.8,9 The most common bacterial organisms in community-acquired bacterial rhinosinusitis are Streptococcus pneumoniae, Haemophilus influenzae, and Moraxella (Branhamella) catarrhalis. The most common viruses in acute viral rhinosinusitis are rhinovirus, adenovirus, influenza virus, and parainfluenza virus.1,2,5,10

| Dental infections and procedures |
| Iatrogenic causes: sinus surgery, nasogastric tubes, nasal packing, mechanical ventilation |
| Immunodeficiency: human immunodeficiency virus infection, immunoglobulin deficiencies |
| Impaired ciliary motility: smoking, cystic fibrosis, Kartagener syndrome, immotile cilia syndrome |
| Mechanical obstruction: deviated nasal septum, nasal polyps, hypertrophic middle turbinates, tumor, trauma, foreign body, Wegener granulomatosis |
| Mucosal edema: preceding viral upper respiratory infection, allergic rhinitis, vasomotor rhinitis |
Diagnosis
CLINICAL SIGNS AND SYMPTOMS
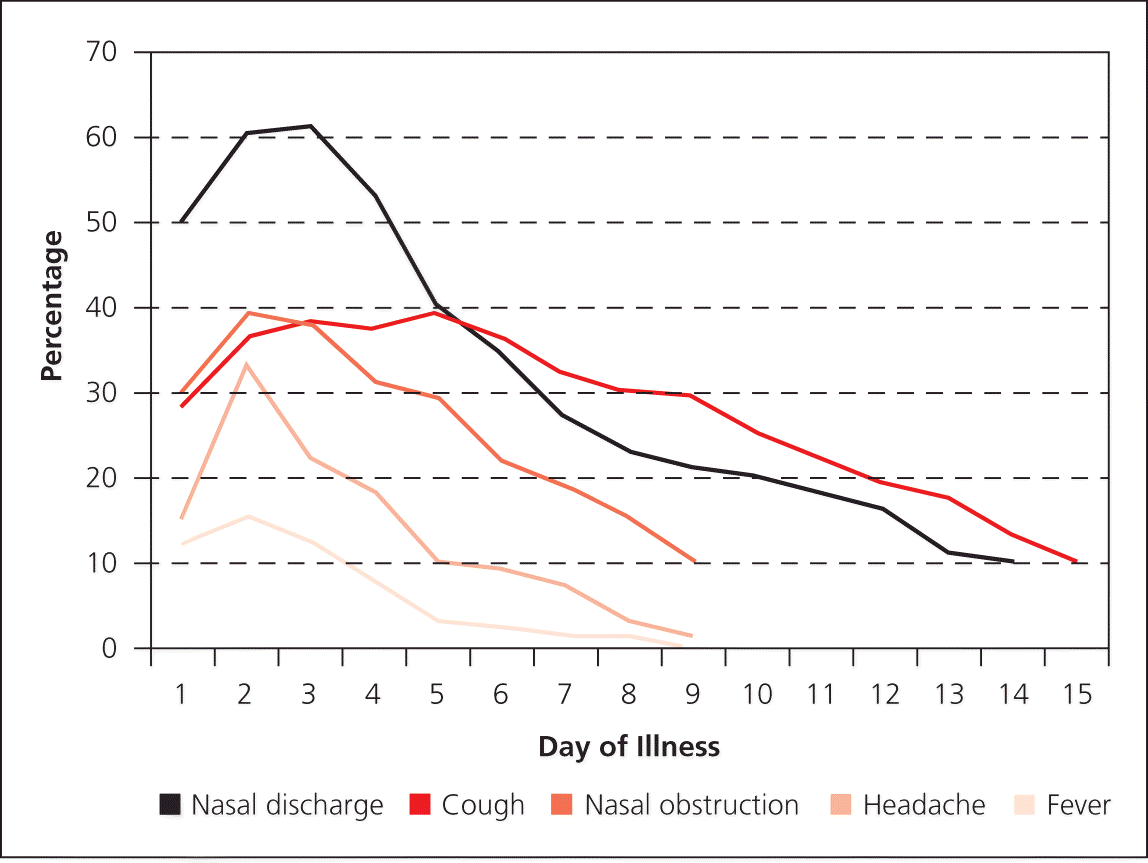
In the first three to four days of illness, viral rhinosinusitis cannot be differentiated from early acute bacterial rhinosinusitis.1 Figure 1 summarizes the natural course of signs and symptoms associated with rhinovirus infections.1 A pattern of initial improvement followed by a worsening of symptoms—called double sickening—between days 5 and 10 of the illness is consistent with acute bacterial rhinosinusitis.1,3,11
Physicians should not rely solely on colored nasal drainage as an indication for antibiotic therapy because it does not predict the likelihood of sinus infection (positive likelihood ratio = 1.5; negative likelihood ratio = 0.5).12 Local sinus pain with unilateral predominance in addition to purulent rhinorrhea had an overall reliability of 85% for diagnosing sinusitis according to one study.13 Another study showed that four signs and symptoms with a high likelihood ratio for acute bacterial sinusitis are double sickening, purulent rhinorrhea, an erythrocyte sedimentation rate greater than 10 mm per hour, and purulent secretion in the nasal cavity. A combination of at least three of these four signs and symptoms has a specificity of 81% and sensitivity of 66% for acute bacterial rhinosinusitis.14 Diagnosis of acute bacterial rhinosinusits is indicated when signs or symptoms of acute rhinosinusitis persist without evidence of improvement for at least 10 days beyond the onset of upper respiratory symptoms.1 After 10 days of upper respiratory symptoms, the probability of bacterial rhinosinusitis is 60%.15
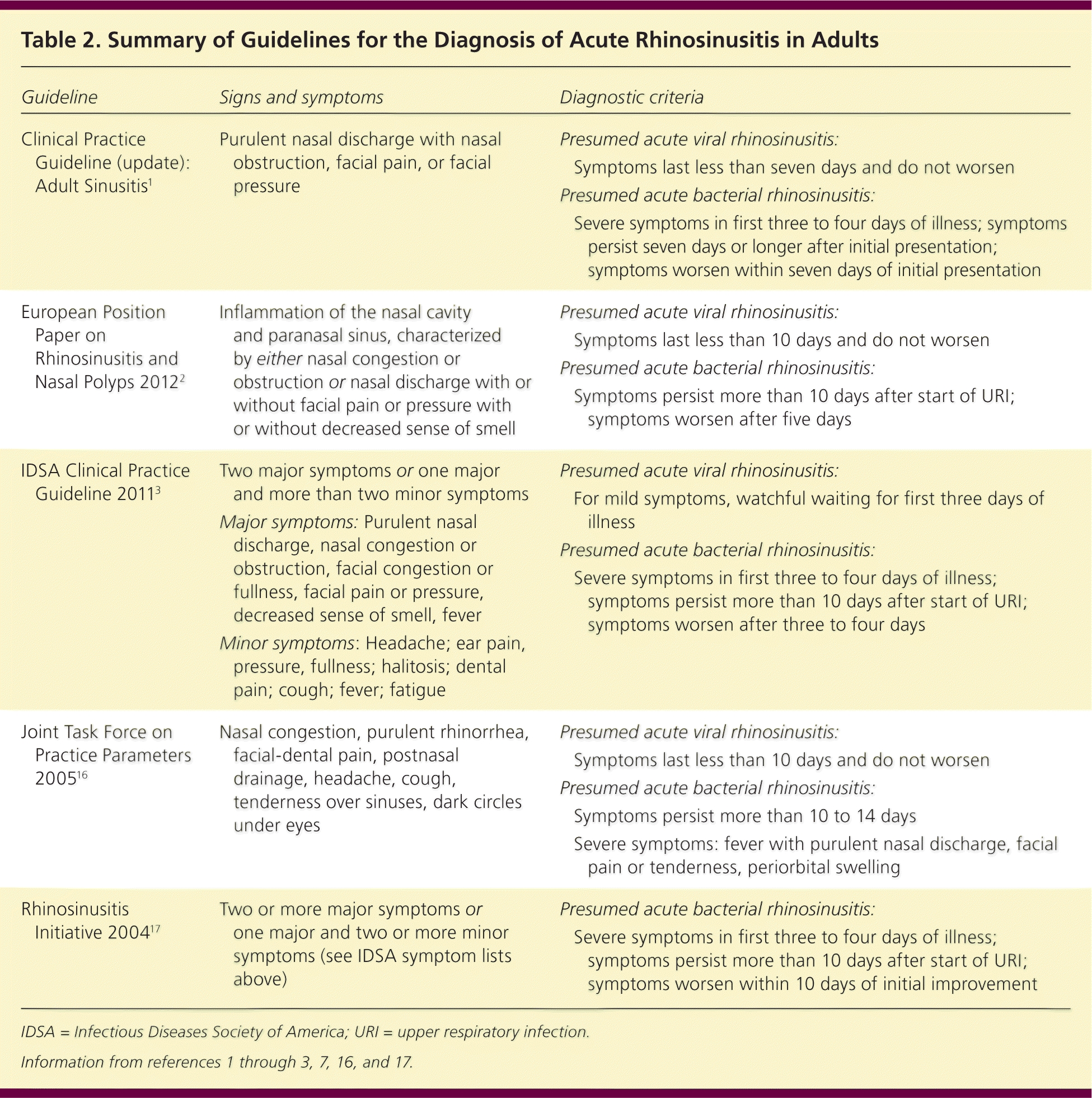
| Guideline | Signs and symptoms | Diagnostic criteria | ||
|---|---|---|---|---|
| Clinical Practice Guideline (update): Adult Sinusitis1 | Purulent nasal discharge with nasal obstruction, facial pain, or facial pressure | Presumed acute viral rhinosinusitis: | ||
| Symptoms last less than seven days and do not worsen | ||||
| Presumed acute bacterial rhinosinusitis: | ||||
| Severe symptoms in first three to four days of illness; symptoms persist seven days or longer after initial presentation; symptoms worsen within seven days of initial presentation | ||||
| European Position Paper on Rhinosinusitis and Nasal Polyps 20122 | Inflammation of the nasal cavity and paranasal sinus, characterized by either nasal congestion or obstruction or nasal discharge with or without facial pain or pressure with or without decreased sense of smell | Presumed acute viral rhinosinusitis: | ||
| Symptoms last less than 10 days and do not worsen | ||||
| Presumed acute bacterial rhinosinusitis: | ||||
| Symptoms persist more than 10 days after start of URI; symptoms worsen after five days | ||||
| IDSA Clinical Practice Guideline 20113 | Two major symptoms or one major and more than two minor symptoms | Presumed acute viral rhinosinusitis: | ||
| Major symptoms: Purulent nasal discharge, nasal congestion or obstruction, facial congestion or fullness, facial pain or pressure, decreased sense of smell, fever | For mild symptoms, watchful waiting for first three days of illness | |||
| Minor symptoms: Headache; ear pain, pressure, fullness; halitosis; dental pain; cough; fever; fatigue | Presumed acute bacterial rhinosinusitis: | |||
| Severe symptoms in first three to four days of illness; symptoms persist more than 10 days after start of URI; symptoms worsen after three to four days | ||||
| Joint Task Force on Practice Parameters200516 | Nasal congestion, purulent rhinorrhea, facial-dental pain, postnasal drainage, headache, cough, tenderness over sinuses, dark circles under eyes | Presumed acute viral rhinosinusitis: | ||
| Symptoms last less than 10 days and do not worsen | ||||
| Presumed acute bacterial rhinosinusitis: | ||||
| Symptoms persist more than 10 to 14 days | ||||
| Severe symptoms: fever with purulent nasal discharge, facial pain or tenderness, periorbital swelling | ||||
| Rhinosinusitis Initiative 200417 | Two or more major symptoms or one major and two or more minor symptoms (see IDSA symptom lists above) | Presumed acute bacterial rhinosinusitis: | ||
| Severe symptoms in first three to four days of illness; symptoms persist more than 10 days after start of URI; symptoms worsen within 10 days of initial improvement | ||||
LABORATORY TESTS
Erythrocyte sedimentation rate and C-reactive protein (CRP) are somewhat useful tests for diagnosing acute bacterial maxillary sinusitis. In a study of 173 patients using antral puncture as the reference standard, 30 of 38 (79%) of those with a CRP level greater than 49 mg per L (466.7 nmol per L) had acute maxillary sinusitis compared with 37 of 61 (61%) of those with a CRP level of 11 to 49 mg per L (104.8 to 466.7 nmol per L) and only 25 of 74 (34%) of those with a CRP level less than 11 mg per L.8
IMAGING
Radiography is not recommended in the evaluation of acute uncomplicated rhinosinusitis.1,3,4,10,11,18–20 It is somewhat helpful in ruling out the presence of fluid when the results are negative. Positive results are not helpful because they cannot differentiate between viral and bacterial sinusitis.
For patients with recurrent acute or chronic rhinosinusitis, computed tomography (CT) of the sinuses without contrast media is the imaging method of choice.1,11,19 CT of the sinuses should be performed only after completing maximal medical therapy. CT is primarily used to define the anatomy of the sinuses before surgery, as well as to assess the extent, pattern, and a probable mechanical cause of the recurrent or chronic rhinosinusitis. A thickened mucosa of 5 mm or greater on CT is a significant sign of sinus infection.14 Antral puncture data from patients with CT evidence of fluid in the maxillary sinus were associated with demonstrated pus or mucopus by sinus lavage in 90% of patients reviewed.14
Treatment
Because viral rhinosinusitis is a self-limited disease, management is primarily directed toward symptom relief and avoidance of unnecessary antibiotics. Physicians continue to overprescribe antibiotics for acute rhinosinusitis.1,3,5,6,10,21 A clinical practice guideline from the AAO-HNS recommends watchful waiting and antibiotic therapy as initial strategies for the management of acute bacterial rhinosinusitis.1
WATCHFUL WAITING
Watchful waiting is appropriate in place of antibiotics for seven to 10 days after upper respiratory symptoms appear when there is assurance of follow-up.1,22–25 Antibiotic therapy should be considered if the patient's condition does not improve by seven to 10 days after initial presentation or if symptoms worsen at any time.1,3,25 Symptomatic therapies should be offered to patients who are under observation. Physicians may also provide these patients with a safety net antibiotic prescription (also called a delayed prescription), with instructions describing when to fill the prescription.1 Watchful waiting is supported by four meta-analyses that were published after the 2007 AAO-HNS clinical practice guideline was released.22–24,26 These studies did not provide evidence confirming or disproving the AAO-HNS position that patients with more severe acute bacterial rhinosinusitis should initially be treated with antibiotics.
A Cochrane review showed that the symptoms of bacterial rhinosinusitis had resolved in 47% of all patients after seven days with or without antibiotic therapy.24 In addition, approximately 70% of patients improved within two weeks without antibiotics.24 Antibiotic therapy did increase cure rates for patients between seven and 15 days compared with placebo; however, the clinical benefit was small, with only 5% of patients having a faster cure.24 Moreover, analysis of individual patient data found that it was not possible to identify which patients with rhinosinusitis would benefit from antibiotics based on the presence of common clinical signs and symptoms.22 The number needed to treat was estimated to be 11 to 15.1,22,24 Adverse effects occurred more often with antibiotics than with placebo (number needed to harm = 8).23,24 The risk of harm outweighs the potential benefit of antibiotic therapy. As a result of this research, the 2015 AAO-HNS guideline recommends offering watchful waiting to patients regardless of illness severity.1
ANTIBIOTIC THERAPY
Antibiotics for the treatment of acute bacterial rhinosinusitis are outlined in Table 3.1,27 Most guidelines recommend amoxicillin with or without clavulanate as a first-line antibiotic for adults because of its safety, effectiveness, low cost, and narrow microbiologic spectrum.1–3,25 Amoxicillin/clavulanate (Augmentin) should be used in patients who are at high risk of bacterial resistance or who have comorbid conditions, as well as in those with moderate to severe infection.1 No significant differences in acute bacterial rhinosinusitis cure rates are noted between different antibiotic classes.1–3
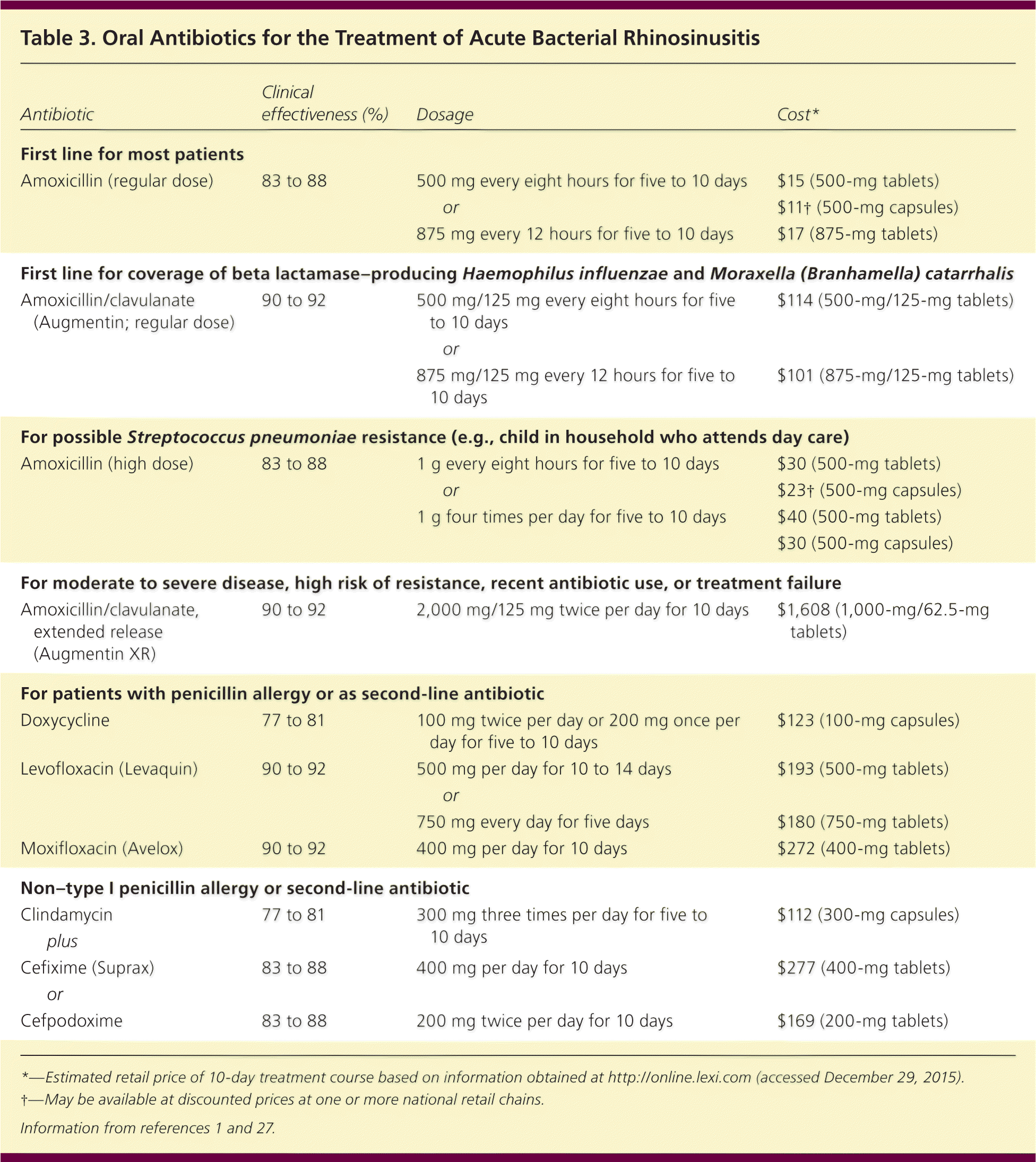
| Antibiotic | Clinical effectiveness (%) | Dosage | Cost* | ||
|---|---|---|---|---|---|
| First line for most patients | |||||
| Amoxicillin (regular dose) | 83 to 88 | 500 mg every eight hours for five to 10 days | $15 (500-mg tablets) | ||
| or | $11† (500-mg capsules) | ||||
| 875 mg every 12 hours for five to 10 days | $17 (875-mg tablets) | ||||
| First line for coverage of beta lactamase–producing Haemophilus influenzae and Moraxella (Branhamella) catarrhalis | |||||
| Amoxicillin/clavulanate (Augmentin; regular dose) | 90 to 92 | 500 mg/125 mg every eight hours for five to 10 days | $114 (500-mg/125-mg tablets) | ||
| or | |||||
| 875 mg/125 mg every 12 hours for five to10 days | $101 (875-mg/125-mg tablets) | ||||
| For possible Streptococcus pneumoniae resistance (e.g., child in household who attends day care) | |||||
| Amoxicillin (high dose) | 83 to 88 | 1 g every eight hours for five to 10 days | $30 (500-mg tablets) | ||
| or | $23† (500-mg capsules) | ||||
| 1 g four times per day for five to 10 days | $40 (500-mg tablets) | ||||
| $30 (500-mg capsules) | |||||
| For moderate to severe disease, high risk of resistance, recent antibiotic use, or treatment failure | |||||
| Amoxicillin/clavulanate, extended release (Augmentin XR) | 90 to 92 | 2,000 mg/125 mg twice per day for 10 days | $1,608 (1,000-mg/62.5-mg tablets) | ||
| For patients with penicillin allergy or as second-line antibiotic | |||||
| Doxycycline | 77 to 81 | 100 mg twice per day or 200 mg once per day for five to 10 days | $123 (100-mg capsules) | ||
| Levofloxacin (Levaquin)‡ | 90 to 92 | 500 mg per day for 10 to 14 days | $193 (500-mg tablets) | ||
| or | |||||
| 750 mg every day for five days | $180 (750-mg tablets) | ||||
| Moxifloxacin (Avelox)‡ | 90 to 92 | 400 mg per day for 10 days | $272 (400-mg tablets) | ||
| Non–type I penicillin allergy or second-line antibiotic | |||||
| Clindamycin | 77 to 81 | 300 mg three times per day for five to10 days | $112 (300-mg capsules) | ||
| plus | |||||
| Cefixime (Suprax) | 83 to 88 | 400 mg per day for 10 days | $277 (400-mg tablets) | ||
| or | |||||
| Cefpodoxime | 83 to 88 | 200 mg twice per day for 10 days | $169 (200-mg tablets) | ||
Respiratory fluoroquinolones are not recommended as first-line antibiotics because they conferred no benefit over beta-lactam antibiotics and are associated with a variety of adverse effects.1,3,28 According to a recent U.S. Food and Drug Administration safety alert, fluoroquinolones should be reserved for patients who do not have other treatment options.29 Macrolides, including azithromycin (Zithromax), trimethoprim/sulfamethoxazole, and second- or third-generation cephalosporins, are no longer recommended as initial therapy for acute bacterial rhinosinusitis because of high rates of resistance in S. pneumoniae and H. influenzae.1,3
The recommended duration of therapy for uncomplicated acute bacterial rhinosinusitis is five to 10 days for most adults.1,3 This recommendation is based primarily on findings from a meta-analysis of 12 randomized controlled trials.30 A shorter treatment course (median of five days) may be just as effective as a longer course of treatment (median of 10 days) and is associated with fewer adverse effects.30 Regardless, clinicians should assess disease and symptom response before stopping antibiotic therapy prematurely, especially in older adults and in patients with underlying disease.
Treatment failure occurs when a patient's symptoms do not improve by seven days after diagnosis or when they worsen at any time, with or without antibiotic therapy.1 If treatment failure occurs following initial antibiotic therapy, an alternative antibiotic with a broader spectrum is required. High-dose amoxicillin/clavulanate, a respiratory fluoroquinolone, or the combination of clindamycin plus a third-generation oral cephalosporin may be considered.1,3
SYMPTOMATIC TREATMENT
Current guidelines consider analgesics, intranasal corticosteroids, and saline nasal irrigation to be options for the management of rhinosinusitis symptoms.1,3 They are recommended for use within the first 10 days but may be continued if antibiotics are initiated. Selection of interventions should be based on shared decision making. Decongestants, antihistamines, and guaifenesin are not recommended for patients with acute bacterial rhinosinusitis because of their unproven effectiveness, potential adverse effects, and cost.3 Table 4 summarizes adjunctive therapies for acute rhinosinusitis.31–35

| Treatment | Evidence summary | Comment |
|---|---|---|
| Intranasal corticosteroids | Two systematic reviews of randomized controlled trials showed minimal benefit and symptom relief occurred late (at 15 to 21 days)32,33 | Some agents available over the counter |
| Saline nasal irrigation | One small randomized controlled trial found hypertonic saline decreased nasal symptoms35 | Available in a low-pressure method using a spray or squeeze bottle or a gravity-flow method using a vessel with a nasal spout |
| Another study found no significant difference between groups receiving no treatment vs. those treated with saline nasal solutions, topical decongestants, and intranasal corticosteroids34 | ||
| Oral decongestants | No clinical trial evidence for patients with acute sinusitis | Significant adverse effects; phenylephrine is similar in effectiveness to placebo for nasal congestion due to seasonal allergic rhinitis31 |
| Topical decongestants | One comparative trial found no significant difference in improvement among groups receiving no treatment vs. those treated with saline nasal solutions, topical decongestants, and intranasal corticosteroids34 | May cause rebound congestion when used for prolonged periods |
Analgesics. An over-the-counter analgesic, such as acetaminophen or a nonsteroidal anti-inflammatory drug, is often sufficient to relieve pain or fever in acute rhinosinusitis. Narcotics are not recommended because of potential adverse effects.1
Intranasal Corticosteroids. Intranasal corticosteroids may be helpful in reducing mucosal swelling of inflamed tissue and facilitating sinus drainage because of an anti-inflammatory effect.1 However, data on intranasal corticosteroids as monotherapy for symptomatic relief in patients with acute sinusitis are limited.24 Several studies suggest that they provide additional benefit in symptom improvement when used with antibiotics in patients with acute sinusitis.36–41 A meta-analysis of six trials37,38,40–43 concluded that intranasal corticosteroids offered a modest therapeutic benefit in patients with acute sinusitis (number needed to treat = 13).32
Similarly, a 2013 Cochrane review found that patients receiving intranasal corticosteroids were more likely to experience symptom improvement after 15 to 21 days compared with those receiving placebo (73% vs. 66.4%; P < .05; number needed to treat = 15).33 Higher doses of intranasal corticosteroids had a greater effect on symptom relief than lower doses. Even though their benefits are only marginal,3 intranasal corticosteroids are often used as an adjunct to antibiotic therapy in the symptomatic treatment of acute bacterial sinusitis. They are likely most beneficial in patients with concurrent allergic rhinitis.3
Saline Nasal Irrigation. Intranasal irrigations with either physiologic or hypertonic saline have been shown to improve mucociliary clearance and may be beneficial for the treatment of acute rhinosinusitis.34,44,45 One randomized controlled trial of 76 patients with frequent sinusitis found that daily hypertonic saline nasal irrigation decreases nasal symptoms and medication use.35 A Cochrane review concluded that saline nasal irrigation may relieve symptoms of upper respiratory infection.46 Despite limited evidence regarding effectiveness, saline nasal irrigation can be a safe and inexpensive adjunctive therapy for symptom relief in acute rhinosinusitis. It is important to inform patients to prepare irrigations using distilled, boiled, or filtered water because there have been reports of amebic encephalitis due to contaminated tap water rinses.47,48
Decongestants. Oral decongestants have been shown to be modestly effective for short-term relief of symptoms in adults with the common cold by reducing nasal airway resistance.49 However, the effect of decongestants in the nasal cavity does not extend to the paranasal sinuses.50 There are currently no randomized controlled trials evaluating the effectiveness of decongestants in patients with sinusitis. Oral decongestants should be used with caution in patients with hypertension or cardiovascular disease. Topical decongestants should not be used for longer than 72 hours, owing to the potential for rebound congestion (rhinitis medicamentosa).
Antihistamines. Antihistamines are often used to relieve symptoms of excessive secretions and sneezing. However, there are no studies to support the effectiveness of antihistamine in acute rhinosinusitis.1,3 Antihistamines may also worsen congestion by overdrying the nasal mucosa. Current guidelines do not recommend antihistamines as an adjunctive therapy for acute bacterial rhinosinusitis, except in patients with a history of allergy.1,3,51
Complications and Referral
If symptoms worsen or if they recur with clearing between episodes, physicians should reevaluate the patient to confirm the diagnosis of acute bacterial rhinosinusitis, exclude other causes of illness, and detect complications.11 Patients who are immunocompromised, seriously ill, or continue to deteriorate despite an extended course of antibiotics should be referred to a subspecialist.3 Complications of acute bacterial rhinosinusitis are estimated at approximately one in 1,000 episodes.11 Although rare in the United States, sinonasal cancer should also be included in the differential diagnosis.52 Table 5 summarizes indications for subspecialist referral in patients with acute bacterial rhinosinusitis.2,3,6,11

| Anatomic defects causing obstruction |
| Complications, such as orbital cellulitis, subperiosteal abscess, intraorbital abscess, altered mental status, meningitis, cavernous sinus thrombosis, intracranial abscess, Pott puffy tumor (osteomyelitis of frontal bone) |
| Evaluation of immunotherapy for allergic rhinitis |
| Frequent recurrences (three to four episodes per year) |
| Fungal sinusitis, granulomatous disease, or possible neoplasm |
| Immunocompromised host |
| Nosocomial infection |
| Severe infection with persistent fever greater than 102°F (39°C) |
| Treatment failure after extended antibiotic courses |
| Unusual or resistant bacteria |
Data Sources: A PubMed search was completed in Clinical Queries using the key terms rhinosinusitis, sinusitis, maxillary sinusitis, diagnosis, and treatment. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. We also searched the Cochrane database, National Guideline Clearinghouse database, Clinical Evidence, and Agency for Healthcare Research and Quality evidence reports. Essential Evidence Plus was also used. Search date: March 30, 2015.