
You might be surprised at how much doctors can help one another improve in coding and documentation.
Fam Pract Manag. 2000;7(4):28-32
Given the federal government's increasing interest in ferreting out health care fraud and abuse, practices that don't implement compliance programs could be putting themselves at risk. While the development of a formal compliance program is outside the scope of this article, I do want to call your attention to one aspect of such a program that is relatively easy to implement, educational for you and your colleagues and potentially even remunerative: a self-audit of coding and documentation. (For more information on developing a compliance plan for your group, see “Protect Your Practice With a Medicare and Medicaid Compliance Program,” FPM, July/August 1998.)
We have made self-audit work for our group of 14 family physicians and one nurse practitioner. It's easy and cheap, especially compared with the cost of external audits, which may be prohibitive for smaller groups (a small practice can expect to pay from $2,500 to more than $10,000 for an external audit, depending on its extent and the number of physicians involved). The only prerequisite for self-audits is having a good grasp of your coding and billing procedures before you implement the process.
KEY POINTS:
A vital part of an effective compliance program is implementing a method to monitor your practice's coding and documentation.
The peer-review self-audit process minimizes demands on physicians' time, requires no special audit training and can be completed in four one-hour sessions annually.
A peer-review self-audit is not only a cost-effective way to protect against fraud and abuse, it's also a valuable educational tool for physicians to improve their coding and documentation skills.
Getting started
We began self-audits in response to our university medical center's requirement for periodic record reviews. Our first step was to form a departmental compliance record committee. The committee, composed of three physicians and our financial manager, identified the peer-review approach as the most efficient and effective method of conducting chart reviews. Physicians in our group were already familiar with peer review, so initial training time was minimal. In addition, the process provides a forum for discussion and timely feedback, which the committee felt would be a valuable educational tool.
Physician reviewers need no special auditing experience to make the peer-review self-audit process successful, but they must be well-versed in the principles of good documentation. If they aren't, you will need to invest time and resources in training before you begin the self-audits.
The Health Care Financing Administration's (HCFA) Web site is an excellent source of free, convenient training. It offers interactive, self-paced provider training programs on topics such as fraud and abuse, ICD-9 diagnosis coding and the HCFA-1500 form. Modules can be downloaded to your computer from www.medicaretraining.com/cbt.htm. Free videotapes of 1999 HCFA satellite broadcasts on a range of Medicare-related topics are also available on the Web site at www.medicaretraining.com/satellite.htm.
Physicians in our group use Superbills to do their own diagnosis and procedure coding at the time of service so they already had a good grasp of coding and documentation. In addition, the university requires that our physicians, nurses and billing staff attend periodic training sessions in billing, and coding and documentation policies and procedures. Past training sessions have included a review of basic billing and coding procedures; use of the CPT and ICD-9 resources; a review of the “Documentation Guidelines for Evaluation and Management Services” from HCFA and the AMA; and, equally important, a review of our institution's billing compliance program. Most sessions are led by billing and coding experts at our institution, but consultants are also available. Both the Medical Group Management Association (MGMA) (www.mgma.com/) and the AAFP (www.aafp.org/) maintain a list of consultants on their Web sites. You can also contact your state medical association for a list of billing and coding consultants in your area.
During the development stage, our committee had to determine the scope and purpose of the record review. How many charts could we evaluate during our quarterly one-hour sessions? What standard evaluation criteria should we use? Where should we focus our efforts?
Since the purpose of the review was to determine whether the medical record documentation could reasonably support the codes we had submitted (or planned to submit) to our insurers, we used the documentation guidelines as our benchmark criteria. Because inpatient and outpatient evaluation and management (E/M) services are a significant source of revenue for our group, we chose them as the primary focus of our self-audits; however, each group should base its choice on the characteristics of its practice (see “Possible target areas for audits”).
For the peer-review self-audit to be most effective, all providers in the group should be involved. We held a special one-hour training session for our providers to explain the peer-review process, discuss the purpose of a self-audit and perform a sample chart review.
If your group's practice includes inpatient as well as outpatient services, as ours does, or if your physicians practice at more than one clinic site, be sure to allow time for obtaining copies of those records to include in your audits.
Possible target areas for audits
Outpatient evaluation and management (E/M) services are major revenue sources in most family practices and should be the focus of coding and documentation audits. Audits should be tailored to the characteristics of each practice, however. Other target areas to consider include these:
Inpatient services,
Visits that combine E/M services and procedures,
Nursing home visits,
Home health care supervision (if billed),
X-rays or ECGs read by consultants,
Laboratory services.
Performing a self-audit review
To minimize demands on the providers' time, we use the beginning of our quarterly one-hour review session to evaluate progress notes (rather than asking providers to review them beforehand); copies of the documentation guidelines are available during the review. We've found it works well to use a chart review form (see the example) and to review two services for each provider per one-hour audit session. So, with 15 providers, we review a total of 30 charts each time. The providers evaluate only the progress notes from individual patient visits, not the entire chart. Of course, providers aren't asked to review their own charts. Nurses and office staff who perform coding and billing functions are also included in the audit sessions to ensure that the physicians' documentation is linked with the correct CPT and ICD-9 codes.
The remainder of the session is devoted to a group discussion of the charts and the providers' coding practices. Although differences in interpreting the guidelines haven't been a major issue in our group, our providers do challenge one another about their progress notes. Despite the potential for conflict, we've noticed that even comments such as, “Your handwriting is very difficult to read!” or, “Why did you organize your note in such a complicated way?” have been well-received and seem to carry more weight when made by a peer.
CHART REVIEW FORM
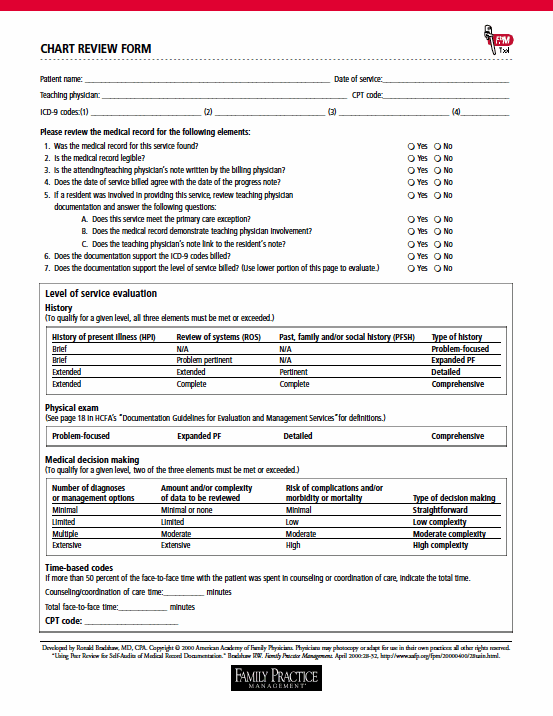
Post-audit follow-up
Shortly after the review session, each provider receives a summary report of the review's overall findings in table format (for example, the report might show that there were three instances in which a service was billed as 99212 but documentation would have supported 99213) as well as a copy of his or her charts with the reviewers' comments. Other follow-up actions may include:
Revise policies and procedures. Our group's management staff members also receive copies so that appropriate changes can be made in policies and procedures to correct systemic errors and, if necessary, corrective action can be initiated. (Disciplinary action generally does not result from self-audits.)
Provide additional training in specific areas. For their education and to improve their coding and documentation, providers receive individual feedback as needed. For example, a physician with a pattern of under-coding may be asked to review the appropriate CPT or ICD-9 codes, as well as the documentation guidelines, to strengthen his or her coding skills.
The physicians in our group willingly participate in the peer-review process. We've found that if they receive data to support the coding and documentation changes they're being asked to make, they adapt their behavior accordingly.
Make refunds, if appropriate. Your self-audits may reveal that incorrect codes have been submitted or that certain bills should not have been submitted at all. To cope with these situations, your senior management should determine procedures for correcting the errors and refunding payments; these procedures may vary from payer to payer. If you identify significant errors, the payments should be refunded to the insurer and correct bills should be submitted. The disadvantage of this approach, of course, is that it may amount to “waving a red flag” in front of the insurer. However, doing so is better than not correcting a billing error that you have identified. The best way to avoid the problem is by performing your reviews prospectively, which allows you to correct improper codes before bills are submitted — and to correct undercoding before it turns into underbilling.
Take disciplinary action, if necessary. If a physician refuses to adapt his or her coding and documentation patterns to ensure compliance with applicable regulations, disciplinary action may be warranted.
Change the focus of the audits. Issues and problem areas identified in a self-audit may help determine the scope of the next round of auditing.
Challenges of the peer-review process
One of our biggest concerns about the peer-review self-audit process was that physicians would be unwilling or unenthusiastic participants. Since the educational aspect of the peer-review approach hinged on physicians' active participation, we knew that we had to get their buy-in in order to succeed. Fortunately, we did.
Another concern was that the physicians who needed the most improvement in their own documentation might be weak links in our self-audit process. We addressed this concern by requesting that our institution's billing compliance reviewers evaluate our process and validate our results. It proved to be very helpful and confirmed that our self-audit process was effective even though it included physicians who needed help with their documentation skills.
This validation step may be impractical for small practices who generally do not have access to an internal audit group. However, an outside auditor can provide validation if a small practice has concerns about the effectiveness of its self-audits —and auditing the output of a couple of self-audit meetings should be considerably less documentation in the practice as a whole.
Benefits of the peer-review process
Peer review has been a mainstay of medical quality-assurance programs, and it provided a number of advantages in our self-audit process:
Education. Reviewing other providers' charts reinforces the essential points of good documentation.
Focus. A self-audit can focus on particular issues relevant to a certain group. For example, if you are concerned about the proper documentation and coding for office visits that involve both E/M services and a procedure, you can target those visits only.
Cost-effectiveness. The peer-review self-audit process requires no additional expenditures, although the opportunity cost of physician time must be taken into account. We estimate one hour per physician each quarter for participation in the actual peer-review process.
Timeliness of feedback. Some of the feedback to providers is immediate (occurring during the group's discussion of the charts while the review is under way). In addition, the overall results of the review can be reported quite soon after the review is completed, particularly as the group gains experience in performing self-audits.
Selected FPM articles on coding and documentation
For more information on improving your coding and documentation skills, review these articles from the Family Practice Management archives:
“Identifying Patterns of Over- and Undercoding.” Kikano GE, Chao J, Gotler RS, et al. November/December 1999:12–13.
“Sneak Preview of the (Revised) Revised Documentation E/M Documentation Guidelines.” Backer LA. September 1999:43–47.
“Improve Your ICD-9 Coding Accuracy.” Hill E. July/August 1999:27–31.
“A Quick-Reference Card for Identifying Level-4 Visits.” Giovino JM. July/August 1999:32–34.
“Take Charge of Coding: Don't Lose Income to Neglect.” Epperson WJ, Hubach KS, Menn KE, et al. March 1999:37–38.
“CPT Changes for 2000.” Moore KJ. January 2000:15.
“Protect Your Practice With a Medicare and Medicaid Compliance Program.” McKessy AM, Saner RJ II. July/August 1998:56–66.
“Avoiding Fraud and Abuse in Medicare Claims: What FPs Need to Know.” Gosfield AG. September 1997:73–82.
It's worth the effort
Our practice has found that using peer review in our self-audits of medical record documentation and coding is efficient, cost-effective and educational. Granted, it's not fun, it takes time away from patient care and it may not always generate revenue. But you'll be grateful that you have a self-auditing mechanism in place as part of a larger compliance plan if HCFA investigators come knocking on your door.