
The time you spend will be well rewarded — both financially and in improved service to your patients.
Fam Pract Manag. 1999;6(3):37-38
The majority of fee-for-service income generated by physicians is directly related to office charges. However, many family physicians are quick to dismiss coding as “a paperwork hassle” that, like other things that occur outside the exam room, deserves only enough attention to keep the practice out of trouble.
Our practice has taken a different approach. We believe that the way we do business affects the way we take care of patients, and that all issues that affect patients merit our attention. Our patients deserve the best care and the best service we can offer.
With this objective in mind, we've developed a coding audit process based on the principles of total quality management that has significantly reduced patient billing problems, saved personnel time, improved our collections and, best of all, improved our documentation and quality of care.
KEY POINTS:
An internal coding audit can improve the documentation and quality of care.
A coding audit may take just one hour each week per provider.
It's reasonable to expect at least a 3 percent improvement in collections.
The coding audit process
One of the fundamentals of our process is that the clinician is primarily responsible for all coding. We believe that delegating coding can lead to bad business and bad service. We train each member of our office staff to review our coding with the mindset of an outside auditor. They catch errors, ask questions and make suggestions regarding accuracy. Diagnosis and procedure coding manuals are readily available in the patient care, checkout and insurance billing areas of our office.
Here's how our system works: When patients check out of the office, they are given a copy of their superbill. Another copy is printed and returned to the providers' dictation area. We review these at lunch or at the end of the day, while the patient visit is still fresh in our minds. We check for accuracy and to make sure no charges were omitted. This review also helps to guard against embezzlement.
We then hold a weekly 30-minute meeting over lunch, involving our physicians, nurse practitioners, physician assistants, front-office staff and office manager. We choose two or three charts at random from each provider's patient contacts for the previous week. We review each chart as a group, paying attention to the quality of the documentation and the quality of the care that was documented; then each provider proposes a code for the visit. Finally the provider whose chart we're discussing reveals the code that was submitted and defends it. It's important to try to make these discussions positive rather than an exercise in finger-pointing. A negative environment will discourage participation. We frequently refer to the CPT manual and coding tools during these meetings.
The results
Before instituting a system like this and at regular intervals thereafter, it's important to review each provider's coding distribution and collection per encounter. A software program like Excel that allows you to graph the data facilitates this process. In fact, with such programs, these simple graphs are a snap. You should expect your individual physicians' coding patterns and collections per encounter to differ; individual practice styles, patient mix and payer mix will affect these measurements (see “Sample code distributions”). The purpose of this comparison is to examine how individual physicians' information may change over time as a result of the regular audits. If the popular conception that family physicians tend to downcode is true of your practice, you'll probably see a shift in your bell curve.
Sample code distributions
Relatively simple graphs of each provider's code distribution (such as those shown here) can provide helpful feedback for any practice seeking to improve its coding. Physicians' patterns may not be identical because of individual practice styles and patient and payer mixes, but you can track each individual's coding patterns over time. This will help you judge whether coding practices are improving.
Physician A: Established and new patient visits
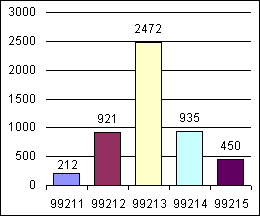
.
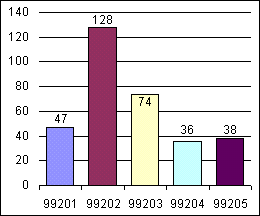
Physician B: Established and new patient visits
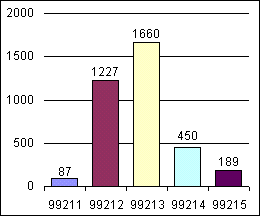
.
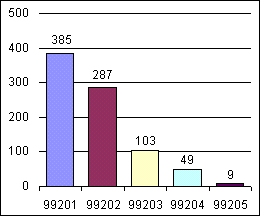
Our practice finances have improved significantly since we instituted coding audits. The weekly, 30-minute lunch meeting combined with five minutes a day spent reviewing our charges is a time investment of one hour a week, or four hours a month, per provider. Is it cost-effective? It is for us. Consider: If a physician has typical monthly collections of $30,000, a 3 percent improvement brought about by the audit process would amount to $900 a month. That increase divided by the four hours of time it took one physician to produce it comes to $225 per hour. We believe this to be a conservative estimate of the value of regular audits for most fee-for-service practices.
Physicians who are already overburdened by paperwork and meetings may resist, but we believe the economic outcomes make the time investment worthwhile. We also know that because we've been proactive, we would probably perform well in an outside audit and avoid the fines and other penalties that might otherwise result.
So take charge of your charges. It's a win-win idea that leads to higher revenues for your practice and better service for your patients.