
Am Fam Physician. 1999;59(5):1259-1260
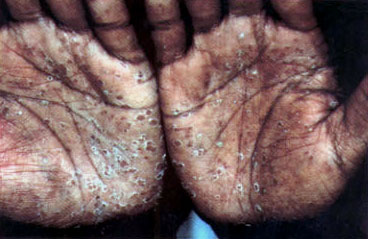
A 28-year-old man presented to the physician with a rash (see the accompanying photograph) and a hearty handshake. The patient described the rash as slightly pruritic and said it had started as scaly patches on the palms of his hands and then spread over his entire body. The physician initially gave the patient topical clotrimazole (Lotrimin) for what was thought to be a tinea infection and a five-day course of prednisone for possible pityriasis rosea. The patient showed no improvement except for some decreased itching while taking prednisone.
Question
Discussion
LOUIE'S LUES
The correct answer is D. This patient has secondary syphilis and should be treated with penicillin. Secondary syphilis has a myriad of potential presentations, including a scaly macular rash that tends to become generalized but may be especially prominent on the palms of the hands and soles of the feet. Condyloma lata are another manifestation of secondary syphilis and appear as moist, hypertrophic papules and plaques in the oral, anal or genital areas. Either of these types of eruptions may be accompanied by fever, malaise, arthralgias, lymphadenopathy and splenomegaly.1
Topical or oral antifungal agents would be the appropriate therapy for severe tinea manuum and, although this condition would appear on the palms, it would rarely present as multiple small-scaled macules, but rather as larger, scaly red plaques. A potassium hydroxide preparation should be used to confirm this diagnosis. Prednisone is not routinely recommended but may benefit patients with symptomatic pityriasis rosea, but in the case of the patient discussed here, prednisone helped mask and delay the proper diagnosis. Biopsy may be necessary to distinguish cases of atypical pityriasis rosea from papulosquamous conditions that are similar in appearance.
Acyclovir might be useful in the treatment of patients with varicella, but eruptions characteristic of varicella appear as vesicles and pustules and do not usually occur on the hands. Contact dermatitis may also be a possible diagnosis because of the rash's location on the hands; however, the affected area would be more eczematous, with erythema, papulosquamous eruption, and weeping or crusted lesions.
A serologic test for syphilis, such as the rapid plasma reagin test, may be appropriate in any patient who presents with widespread scaly eruptions, even in patients in whom pityriasis rosea is considered the most likely diagnosis. However, physicians should be reminded of the possibility of false-negative results. This “prozone effect” occurs when the antigenic load is so high that the normal complementation fixation process is interfered with, and no reaction takes place. This has been reported in patients with syphilis who are in various states of immune deficiency. If, because of the clinical history, the prozone effect is a possibility, the laboratory must be alerted to dilute the sample and repeat the test.
The chancre of primary syphilis may be missed if it is in a concealed oral, anal or genital location. Many patients who delay seeking care after noticing a chancre will be falsely reassured when the chancre spontaneously resolves and will fail to seek treatment until manifestations of secondary syphilis appear. In most cases, Treponema pallidum (spirochetes) is readily identifiable in biopsy tissue, but only with special staining for spirochetes. Patients such as the man in the case presented here are considered contagious and, if you shake hands with them, you should remember the importance of washing afterward.