Both isolated systolic hypertension (> 140 mm Hg/< 90 mm Hg) and systolic/diastolic hypertension (> 140 mm Hg/> 90 mm Hg) are major risk factors for cardiovascular disease in the elderly. Specific antihypertensive drug therapy is available if lifestyle interventions fail to reduce blood pressure to a normal level. Diuretics and beta blockers both reduce the occurrence of adverse events related to cerebrovascular disease; however, diuretics are more effective in reducing events related to coronary heart disease. Treated patients are less likely to develop severe hypertension or congestive heart failure. In most instances, low-dose diuretic therapy should be used as initial antihypertensive therapy in the elderly. A long-acting dihydropyridine calcium channel blocker may be used as alternative therapy in elderly patients with isolated systolic hypertension. Trials are being conducted to evaluate the long-term effects of angiotensin converting enzyme inhibitors and angiotensin-II receptor blockers in elderly patients with uncomplicated hypertension.
The aging of the U.S. population has raised concerns about the social and economic resources that may be necessary to manage the growing number of elderly persons with cardiovascular disease. Coronary heart disease is the major cause of death in both elderly men and elderly women. Hypertension, either systolic/diastolic or isolated systolic, is considered a major risk factor for coronary heart disease.
As late as the 1970s, the prevailing medical opinion was to ignore elevated blood pressures in the elderly, even though epidemiologic data demonstrated the age-related risk of coronary heart disease as a result of hypertension.1 Into the 1980s many physicians still did not believe that antihypertensive drugs could improve outcome in the elderly, despite abundant data from several clinical trials.2,3 It is now generally accepted that effective treatment of isolated systolic or systolic/diastolic hypertension can reduce the morbidity and mortality of coronary heart disease.
Isolated Systolic Hypertension
Data from the Framingham study1 and the Multiple Risk Factor Intervention Trial4 indicated the importance of isolated systolic hypertension in the development of coronary heart disease. These trials concluded that elevated systolic blood pressure in the elderly was probably of more significance than elevated diastolic blood pressure. In other words, a systolic blood pressure of 160 mm Hg with a diastolic blood pressure of 85 mm Hg posed a greater risk for cardiovascular disease than a systolic blood pressure of 135 to 140 mm Hg and a diastolic blood pressure of 95 mm Hg. Isolated systolic hypertension, defined as a blood pressure of greater than 140 mm Hg systolic and less than 90 mm Hg diastolic, occurs in more than 30 percent of women over the age of 65 years and in more than 20 percent of men of the same age.4
Two major randomized, prospective, placebo-controlled treatment trials have been conducted in elderly patients with isolated systolic hypertension.5,6 The Systolic Hypertension in the Elderly Program (SHEP)5 used the diuretic chlorthalidone, in a dosage of 12.5 mg per day, as initial therapy; when necessary, atenolol, in a dosage of 25 mg per day, was added to achieve the goal blood pressure. In the European Trial on Systolic Hypertension Study in the Elderly (Syst-Eur),6 patients were treated initially with a long-acting dihydropyridine calcium channel blocker, nitrendipine (not available in the United States); if required, enalapril or a diuretic was added to achieve goal blood pressure. Several trials of other medications are currently in progress.
At the end of five years, the SHEP trial noted that lowering blood pressure yielded a statistically significant reduction in adverse events related to coronary heart disease, congestive heart failure and overall cardiovascular disease (Figure 1).5 Blood pressures were an average of 12/4 mm Hg lower in the treated patients than in those who received placebo. Although a trend toward decreased mortality was noted, a significant decrease in overall mortality was not demonstrated. No increase in dementia or depression was noted in the treated group compared with the placebo group. The important message of the SHEP study is that a decrease in coronary heart disease events can be achieved by treating isolated systolic hypertension with a relatively simple and inexpensive regimen.
FIGURE 1. SHEP Trial in the Elderly: Risk Reduction for Treatment vs. Placebo
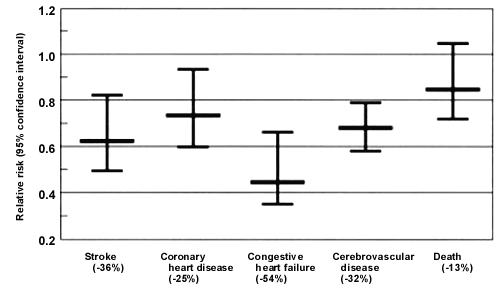
Systolic Hypertension in the Elderly Program (SHEP) trial: comparative reductions in cardiovascular events. The percentage given in parentheses for each event represents the risk reduction experienced by treated patients compared with those who received placebo. Decreases in all events except death are statistically significant. Treated patients received a diuretic as initial therapy; a beta blocker was added to achieve goal blood pressure. Average baseline blood pressure was 171/77 mm Hg in the treated group and 170/76 mm Hg in the placebo group. Average final blood pressure was 144/68 mm Hg in the treated group and 155/71 mm Hg in the placebo group. Thus, average blood pressure was 12/4 mm Hg lower in the treated groups than in the placebo groups.
Most elderly patients with isolated systolic hypertension have other risk factors for coronary disease. In the SHEP trial,5,7 antihypertensive therapy reduced coronary heart disease events by 31 percent in patients with cholesterol levels below 216 mg per dL (5.59 mmol per L), by 29 percent in those with cholesterol levels of 216 to 250 mg per dL (5.59 to 6.47 mmol per L) and by 24 percent in those with levels above 251 mg per dL (6.49 mmol per L). Treatment yielded benefits in patients with either normal or high cholesterol levels (Table 1).7
Many older people with isolated systolic hypertension also have diabetes mellitus or glucose intolerance. In the SHEP trial, the percent reduction in events related to coronary heart disease was greater in the treated diabetic patients than in the treated nondiabetic patients (Table 2).7
The SHEP trial showed that lowering blood pressure using a diuretic with or without a beta blocker reduces the occurrence of coronary heart disease in patients with hyperlipidemia and diabetes. Based on the results of this trial, an estimated 24,000 fewer strokes, 44,000 fewer cardiovascular events and 84,000 fewer hospital admissions would occur each year if isolated systolic hypertension were treated effectively. In addition to the social and medical benefits of this preventive effort, the savings in health care and other expenditures would be considerable. Nonetheless, the use of diuretics has continued to decline for a number of reasons, including the perception that these agents produce adverse metabolic effects and the heavy promotion of other medications.8
The Syst-Eur trial6 was a prospective, placebo-controlled study of patients who primarily had isolated systolic hypertension, which was defined as a blood pressure of greater than 160 mm Hg systolic and less than 95 mm Hg diastolic. The study was stopped after two years because of a marked decrease in nonfatal and total strokes in the nitrendipine-treated group compared with the placebo-treated group. Although a trend toward the reduction of coronary heart disease events and heart failure was noted, statistical significance was not achieved during the trial (Table 3).6 If the study had been continued for a longer period, it is possible that a significant decrease would have been found. As noted in the diuretic-based SHEP trial, coronary heart disease events and heart failure were substantially reduced in treated patients.
At present, no definitive data suggest that a calcium channel blocker reduces morbidity or mortality of coronary heart disease in elderly patients with isolated systolic hypertension. Based on the Syst-Eur trial,6 however, the sixth report of the Joint National Committee on Prevention, Detection, Evaluation and Treatment of High Blood Pressure9 suggested that a long-acting dihydropyridine might be appropriate alternative therapy in patients with isolated systolic hypertension, although a diuretic was still listed as the preferred initial treatment.
Systolic/Diastolic Hypertension
The outcomes of eight randomized, controlled treatment trials in elderly patients with systolic/diastolic hypertension2,3,5,6,10–13 are summarized in Table 4.14 These trials used diuretics or beta blockers as initial therapy. Approximately 20,000 patients with a mean age of more than 70 years were followed for two and one half to five years.
Blood pressure reductions of 12 to 14 mm Hg systolic and 5 to 6 mm Hg diastolic were achieved in the treated groups compared with the control groups. The treated patients had approximately 20 percent fewer fatal and non-fatal coronary events than the patients in the control groups. Treated patients also had a more than 30 percent reduction in strokes and a more than 20 percent reduction in vascular deaths compared with the control groups. The results of these trials verify that treating systolic/diastolic hypertension in the elderly can reduce both coronary and cerebrovascular adverse events.
The recently completed Hypertension Optimal Treatment (HOT) trial15 included 19,000 patients with a mean age of 61 years. This study reported a decrease in “expected” cardiovascular events in three groups of patients whose diastolic blood pressures were carefully controlled at levels below 90, 85 or 80 mm Hg, respectively. Initial therapy consisted of a long-acting calcium channel blocker, felodipine; however, to achieve goal blood pressure, an angiotensin converting enzyme (ACE) inhibitor, a beta blocker or a diuretic was added in 41 percent, 28 percent and 22 percent of the patients, respectively. Treatment benefits were greater in the diabetic patients in the study. Furthermore, reducing diastolic blood pressure to below 85 mm Hg did not adversely affect outcome. In fact, greater benefit appeared to result at the lower levels of diastolic blood pressure, especially in patients with diabetes.
Significant Outcomes of Hypertension in the Elderly
The prevention of congestive heart failure and progression from less severe to more severe hypertension is probably more significant in the elderly than in younger persons. The overall benefit of hypertension control may have been underestimated in some analyses that focused on more traditional outcomes such as stroke and myocardial infarction.
CONGESTIVE HEART FAILURE
Just as fewer people are dying of strokes, fewer people are dying of acute myocardial infarction. The result is more survivors who may develop congestive heart failure. Hospitalizations for congestive heart failure are increasing dramatically in the United States. Consequently, the prevention of congestive heart failure should be a major treatment goal. Data from the Framingham study indicate that hypertension is a major factor in the development of congestive heart failure.16
A review17 of the major hypertension treatment trials in the elderly demonstrated a highly statistically significant reduction (48 percent) in the occurrence of congestive heart failure as a result of treatment for a relatively short period (three to five years). The data actually underestimate the benefit of treatment in that a large number of patients in the placebo groups received anti-hypertensive therapy because of rising blood pressure.
A great deal of effort is currently expended on preventing the recurrence of congestive heart failure. ACE inhibitors, a relatively new alpha-beta blocker (carvedilol [Coreg]) and certain beta blockers may help with this effort. Emphasis, however, should be focused on lowering blood pressure, especially in the elderly, to actually prevent left ventricular hypertrophy and congestive heart failure.
PREVENTION OF PROGRESSIVE HYPERTENSION
Another factor to consider in estimating the benefit of antihypertensive therapy is the number of patients who progress from less severe to more severe disease without therapy. For example, in the Medical Research Council (MRC) trial,13 175 of 2,213 elderly patients in the placebo group progressed to severe hypertension, which was defined as a blood pressure higher than 110 mm Hg diastolic and higher than 200 mm Hg systolic. In contrast, progression to severe hypertension occurred in only 13 of 2,183 treated patients.
Response of the Elderly to Different Antihypertensive Drugs
In the Swedish Trial in Old Patients with Hypertension (STOP-Hypertension),12 therapy with three beta blockers (metoprolol, atenolol and pindolol) was compared to therapy using a diuretic with a potassium-sparing component. Systolic blood pressures were reduced to a greater degree with the diuretic than with the beta blockers. Diastolic blood pressures were reduced to the same degree with all agents. The same findings have been noted in other studies.
The superior blood pressure–lowering response to diuretics may explain some of the outcome differences in trials conducted in elderly patients with hypertension. In the MRC trial,13 for example, diuretic therapy reduced coronary heart disease events, strokes and overall cardiovascular disease events, whereas beta blocker therapy did not produce a statistically significant reduction in events related to coronary heart disease.
Outcome data from other studies indicate that a lower percentage of elderly patients with hypertension achieve goal blood pressure with beta blockers than with diuretics. Although reductions in strokes and congestive heart failure have been reported for beta-blocker therapy, a statistically significant effect on coronary heart disease events has not been consistently noted. The greater decrease in systolic blood pressure noted with diuretic therapy may account for at least part of the outcome differences reported by the various trials. However, numerous studies conducted in patients with ischemic heart disease show that beta blockers reduce recurrent infarctions and death, especially after myocardial infarction.18 Recent data from the HOT trial suggest that outcomes may be improved if more vigorous attention is given to lowering diastolic blood pressures below 90 mm Hg using different medications.15
Only limited long-term data are available on the use of either dihydropyridine calcium channel blockers (other than nitrendipine) or nondihydropyridine calcium channel blockers in the treatment of hypertension in elderly patients. Yet other such drugs have been used for antihypertensive therapy for more than 15 years. One nonrandomized, poorly designed, long-term study19 showed that long-acting nifedipine reduced the occurrence of strokes and severe arrhythmias. Only two myocardial infarctions occurred in the control group and two in the treated group. This study could not determine the outcome for coronary heart disease.
Some long-term data are available on the use of ACE inhibitors in patients with hypertension who experience heart failure or decreased ejection fractions, but no outcome data are available on the efficacy of these drugs in elderly patients with uncomplicated hypertension. In one study,20 events related to congestive heart failure were reduced in a subgroup of patients with hypertension who had ejection fractions below 35. Many of these patients were over 65 years of age. In the same study, ACE inhibitor therapy reduced the occurrence of angina or myocardial infarction in normotensive patients but not in hypertensive patients. It is possible that when long-term studies such as the U.S. Anti-hypertensive Therapy and Lipid Lowering Heart Attack Prevention Trial have been completed, the data may show that ACE inhibitors reduce the occurrence of events related to coronary heart disease in both elderly and younger patients with hypertension. At present, however, such data are not available.
Approach to Therapy
Based on available information, isolated systolic hypertension and systolic/diastolic hypertension in the elderly should be treated with the expectation that morbidity and mortality will be reduced. A suggested management approach is provided in Figure 2.
FIGURE 2. Treatment of Elderly Patients with Hypertension
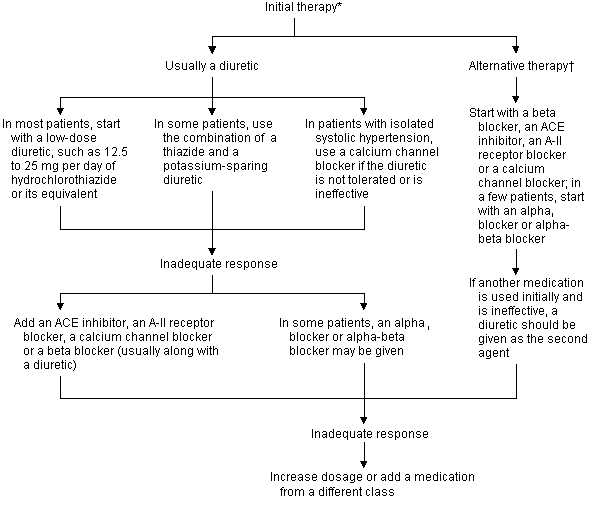
Suggested approach to the management of hypertension in the elderly (ACE = angiotensin converting enzyme; A-II = angiotensin II).
A small dosage of a diuretic should be chosen as initial therapy for most elderly patients with hypertension.14,19 Compared with younger persons, the elderly require smaller dosages, such as 12.5 mg to a maximum of 25 mg per day of hydrochlorothiazide (Esidrix) or its equivalent. The combination of a thiazide and a potassium-sparing agent may be indicated, although hypokalemia is not usually a major problem with low-dose diuretic therapy.
For initial antihypertensive therapy, a beta blocker may be preferable to a diuretic in patients with angina. In patients with diabetes or diabetic nephropathy, the therapy of choice is probably a diuretic plus an ACE inhibitor or possibly an angiotensin-II (A-II) receptor blocker.
Based on data from the Syst-Eur trial,6 a long-acting dihydropyridine calcium channel blocker may be an alternative therapy in patients with isolated systolic hypertension who cannot take a diuretic or who respond poorly to diuretic therapy; however, cost may be a factor in this decision. More data on long-acting dihyropyridines are needed.
Combinations of small doses of two drugs from different classes may also be effective in elderly patients. For example, a diuretic may be given with a beta blocker, an ACE inhibitor or an A-II receptor blocker. In some patients, an ACE inhibitor and a calcium channel blocker may be given together; a diuretic may then be added if a goal blood pressure below 140/90 mm Hg is not achieved. Response rates are usually higher when a diuretic is part of the combination.
When a drug other than a diurectic is used as initial therapy, a diuretic should be added if the response is inadequate. If a diuretic proves to be ineffective as initial therapy, an ACE inhibitor, an A-II receptor antagonist, a beta blocker or a long-acting calcium channel blocker should be tried.
In general, elderly patients adhere to therapy as well as or better than younger patients, and they tolerate medication if it is administered appropriately. Postural hypotension may be a problem, and standing blood pressures should be used to guide therapy. Cognitive function is not adversely affected by the medications that have thus far been evaluated.
Antihypertensive drug therapy can reduce blood pressure to below 140/90 mm Hg in up to 70 percent of elderly patients with hypertension.21 This percentage is lower than the control rates in younger patients with hypertension. Yet even a decrease in systolic pressure of 15 to 20 mm Hg without achieving a goal blood pressure of less than 140/90 mm Hg may be useful in reducing events related to coronary heart disease in the elderly.

