Understanding the distinctions between the management of clinical problems in nursing homes compared with the community setting helps improve the overall care of nursing home residents. Liberalizing diets helps avoid unintentional weight loss in nursing home residents, although the use of feeding tubes usually does not improve nutrition or decrease aspiration risk. Medical assessment, treatment of comorbidities, and appropriate use of rehabilitation therapies minimize the frequency of falls. Toileting programs may be used to treat incontinence and retention in cooperative patients. Adverse effects and drug interactions should be considered when initiating pharmacologic treatment of overactive bladder. Urinary tract infection and pneumonia are the most common bacterial infections in nursing home residents. Signs and symptoms of infection include fever or hypothermia, and functional decline. Virus identification is recommended for influenza-like illnesses. Nonpharmacologic behavioral management strategies are the preferred treatment for dementia-related problem behaviors. The Beers criteria, which outline potentially inappropriate medication use in older persons, provide guidance for medication use in the nursing home.
Nursing home residents often need specific clinical care, such as management of malnutrition and unintentional weight loss, chronic pain, and declining physical function and cognition. Recognizing the distinctions between treating these residents versus community-dwelling patients is important in optimizing care. This article, part II of a two-part series, focuses on the clinical aspects of nursing home care. Part I covers the elements and challenges of nursing home care, including advance care and financial planning, record keeping, transfers, and abuse.1
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Liberalizing the diet of nursing home residents may improve nutritional status and quality of life. | C | 8, 9 |
| Cornerstone interventions for frailty in nursing home residents focus on reconditioning exercises, nutrition, comorbidities, disability, and symptoms. | C | 15–17 |
| Systematic, structured pain assessment has been demonstrated to be effective in nursing home residents. A multidisciplinary approach to pain treatment is necessary in this population. | B | 18, 19 |
| Systematic, structured pain assessment has been demonstrated to be more effective than episodic pain assessment in identifying and treating pain in nursing home residents. | B | 19 |
| Evaluation and treatment goals for urinary incontinence and retention in nursing home residents should be individualized based on feasibility, appropriateness, and resident and family preference. | C | 20 |
| Systematic, prioritized multidisciplinary interventions based on fall assessment can reduce frequency and complications of falls. | B | 22 |
| In nonemergency situations, physical restraints should be used in nursing home residents only after careful and comprehensive review, assessment, and documentation provide substantial evidence that no safer alternative can be used. | C | 23 |
| Individualized care plans for nursing home residents with dementia are developed based on the stage of dementia and associated impairments. | C | 31, 32 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Nutrition
Malnutrition and unintentional weight loss are significant problems in nursing home residents and can lead to multiple complications, such as pressure ulcers and infections.2,3 Treating malnutrition in the nursing home resident may involve a full medical evaluation and appropriate laboratory testing.4,5 However, environmental, social, and staffing factors are also associated with unintentional weight loss. An appealing eating environment and one-on-one staffing to assist residents who are unable to feed themselves may help residents regain or maintain weight.6,7
Liberalizing diets may also promote weight gain in residents with unintentional weight loss. The American Dietetic Association recommends liberalizing diets to improve nutritional status and quality of life in older adults.8 A small study demonstrated equivalent glycemic control in nursing home residents who ate a regular diet versus those who ate a restricted American Diabetes Association diet.9
If unintentional weight loss continues, discussions regarding artificial nutrition and hydration via feeding tube may develop between the family and nursing home staff. However, studies have shown that percutaneous endoscopic gastrostomy does not improve nutritional status or quality of life for residents with dementia,10,11 and residents with dysphagia after a stroke who receive tube feedings do not have a decreased risk of aspiration pneumonia.12 Feeding tubes can cause discomfort and agitation and increase the use of restraints.13 Educational interventions may improve physician, staff, resident, and family knowledge of the risks and limitations of tube feeding.14
Frailty
Key characteristics of frailty are weight loss, fatigue/exhaustion, weakness, slowness, and inactivity.15 Table 1 presents clinical criteria for frailty that predict increased falls, worsening impairment in activities of daily living, hospitalization, and death.15,16 Persons with at least three of these criteria are deemed frail and have six times the mortality over three years than those who are not frail. Persons with two of these findings are considered “pre-frail” and are at twice the risk of progression to the full syndrome.15 Other models for characterizing frailty include cognitive impairment, mood disturbance, and disability.16 No biochemical markers are useful to diagnose frailty.15 Cornerstone interventions for frailty focus on reconditioning exercises, nutrition, comorbidities, disability, and symptoms.15–17
Table 1. Clinical Criteria and Management Strategies for Frailty
| Symptom | Criteria for frailty | Management strategies | |
|---|---|---|---|
| Fatigue/exhaustion* | Patient responds to the following statements about the previous week: | Physical therapy Treatment of underlying conditions Energy conservation measures Medication review Daily activity to promote function, balance, flexibility, and socialization | |
| “I felt as if everything I did was an effort.” | |||
| “I could not get going.” | |||
| Score each response as: 0 points = never or rarely; 1 point = 1 to 2 days; 2 points = 3 to 4 days; 3 points = most of the time | |||
| Patients with a total score of 2 or 3 points are considered frail | |||
| Inactivity | Men: < 383 kcals of activity expended per week (sitting or inactive) | Same as for fatigue/exhaustion Family presence Socialization with activities | |
| Women: < 270 kcals | |||
| Slowness | Men | Resistance strength training Tai chi Physical therapy Family presence Socialization with activities | |
| Height ≤ 173 cm (68 in): | |||
| ≥ 7 seconds to walk 15 ft | |||
| Height > 173 cm: | |||
| ≥ 6 seconds | |||
| Women | |||
| Height ≤ 159 cm (62.6 in): | |||
| ≥ 7 seconds | |||
| Height > 159 cm: | |||
| ≥ 6 seconds | |||
| Weakness† | Men | Resistance strength training Tai chi and walking Physical therapy Family presence Socialization with activities | |
| BMI ≤ 24 kg per m2: grip strength ≤ 29 kg | |||
| BMI 24.1 to 28: grip strength ≤ 30 kg | |||
| BMI > 28: grip strength ≤ 32 kg | |||
| Women | |||
| BMI ≤ 23: grip strength ≤ 17 kg | |||
| BMI 23.1 to 26: grip strength ≤ 17.3 kg | |||
| BMI 26.1 to 28: grip strength ≤18 kg | |||
| BMI > 28: grip strength ≤ 21 kg | |||
| Weight loss | Unintentional weight loss of ≥ 10 lb or ≥ 5 percent of body weight in the previous year | Liberal, culturally appropriate diet Frequent, small feedings Nutritional supplements between meals Resistance strength training Oral and dental care Family presence Socialization with activities Assessment for feeding disability Feeding assistance Appetite stimulants (limited role) | |
note: Persons with at least three of these criteria are deemed frail and have six times the mortality over three years than those who are not frail. Persons with two of these findings are considered “pre-frail” and are at twice the risk of progression to the full syndrome.15
BMI = body mass index.
*—Self-reported exhaustion is an indicator of maximum volume of oxygen utilization and a predictor of cardiovascular disease.
†—Measured using a grip dynamometer.
Pain Management
An estimated 45 to 80 percent of nursing home residents experience chronic pain.18 These patients have atypical signs and symptoms of pain, as well as communication barriers, cognitive loss, polypharmacy, and multiple comorbidities that make diagnosis and treatment difficult. Pain can also complicate other conditions by causing depression, anxiety, deconditioning, disability, impaired sleep, and social withdrawal.18 Pain may be a major cause of disordered behavior in nursing home residents.
Nursing home residents with cognitive impairment are able to reliably self-report pain using established pain scales. Noncommunicative residents can be observed for pain behaviors, such as noisy breathing, negative vocalizations, sad or frightened facial expressions (e.g., frowning), fidgeting, and tense body language. Systematic, structured pain assessment has been demonstrated to be more effective than episodic assessment in identifying and treating pain in nursing home residents.19
Treatment of pain in this population requires a systematic, prioritized, multidisciplinary approach that may include resident, family, and staff education and communication; pastoral counseling; music therapy; exercise; hot or cold compresses; baths or showers; and pharma-cotherapy.18 Regular administration of pain medications should be considered if an agent is requested often, the pain is chronic, or the resident is unable to communicate his or her needs. Principles of opioid management in the nursing home setting are similar to those in other health care settings. The risks of opioid therapy in frail older persons are constipation, ileus, anorexia, hypotension, and falls. Before initiating opioid therapy, the patient's medications should be reviewed, and discontinuation or modification should be considered for those that may adversely interact with the opioid.18
Urinary Incontinence and Retention
Incontinence affects 55 percent of nursing home residents and is associated with increased risk of falls, depression, anxiety, embarrassment, and social isolation.20 Evaluation and treatment goals should be individualized based on feasibility, appropriateness, and resident and family preference.20 Evaluation of urinary incontinence and retention in nursing home residents is similar to that in the community setting, but includes particular attention to the resident's overall care plan and medications associated with incontinence. Tables 2 and 3 include the causes of urinary incontinence and retention.20
Table 2. Possible Causes and Treatments of Urinary Incontinence
| Possible causes of incontinence* |
| Anxiety |
| Arthritis |
| Benign prostatic hyperplasia |
| Cancer (bladder or prostate) |
| Congestive heart failure |
| Constipation |
| Deconditioning |
| Delirium |
| Dementia |
| Depression |
| Diabetes mellitus |
| Environment (access, assistance, restraints) |
| Fecal impaction |
| Fluid consumption |
| Hypercalcemia |
| Hyperglycemia |
| Medications (anticholinergics; antihistamines; diuretics, including caffeine; narcotics) |
| Neurodegenerative disorders |
| Pelvic organ prolapse (women) |
| Recent hospitalization, surgery, catheterization |
| Self-neglect |
| Stroke |
| Urethral stricture |
| Urinary retention |
| Urinary tract infection/urethritis |
| Vaginitis |
| Common treatments for urge incontinence† |
| Darifenacin (Enablex) |
| Oxybutynin (Ditropan) |
| Tolterodine (Detrol) |
| Trospium (Sanctura) |
| Solifenacin (Vesicare) |
*—General types of incontinence include stress, urge, overflow, and functional.
†—Use of these agents contraindicated in persons with urinary retention, gastric obstruction, or uncontrolled narrow-angle glaucoma. Caution should be used in patients who may be predisposed to delirium or who are taking cholinergic medications for dementia.
Information from reference 20.
Table 3. Possible Causes of Urinary Retention
| Infectious/inflammatory |
| Men: prostatitis, prostate abscess, balanitis |
| Women: vulvovaginitis, vaginal lichen planus |
| Men and women: urinary tract infection, cystitis, Guillain-Barré syndrome, herpes simplex virus, periurethral abscess, urethritis, transverse myelitis |
| Neurologic |
| Men and women: spinal cord injuries, progressive neurologic disease, diabetic neuropathy, stroke |
| Obstructive |
| Men: benign prostatic hyperplasia, meatal stenosis, phimosis, prostate cancer |
| Women: pelvic organ prolapse, pelvic mass, uterine fibroids |
| Men and women: bladder calculi, bladder neoplasm, fecal impaction, gastrointestinal or retroperitoneal mass, urethral stricture |
| Other conditions |
| Men: penile trauma, fracture, or laceration |
| Women: urethral sphincter dysfunction |
| Men and women: obstructed urinary catheter, disruption of posterior urethra and bladder neck associated with trauma, postoperative complication |
| Medications |
| Antiarrhythmics: disopyramide (Norpace), procainamide, quinidine |
| Anticholinergics: belladonna, dicyclomine (Bentyl), hyoscyamine (Levsin), oxybutynin (Ditropan), scopolamine |
| Antidepressants: amitriptyline, doxepin, imipramine (Tofranil), nortriptyline (Pamelor) |
| Antihistamines: chlorpheniramine, diphenhydramine (Benadryl), hydroxyzine (Vistaril) |
| Antihypertensives: hydralazine, nifedipine (Procardia) |
| Antiparkinsonian medications: amantadine, benztropine (Cogentin), bromocriptine (Parlodel), levodopa |
| Antipsychotics: chlorpromazine, fluphenazine, haloperidol (formerly Haldol), prochlorperazine (formerly Compazine) |
| Hormones: estrogen, progesterone, testosterone |
| Muscle relaxants: baclofen (Lioresal), cyclobenzaprine (Flexeril), diazepam (Valium) |
| Sympathomimetics: phenylephrine, pseudoephedrine |
| Miscellaneous: analgesics, anesthetics, carbamazepine (Tegretol), nonsteroidal anti-inflammatory drugs, opioids |
Information from reference 20.
Toileting programs, which may be used in cooperative patients, include scheduled toileting habit training (i.e., assistance according to the resident's established behavioral pattern) and prompted voiding (i.e., teaching the resident to recognize bladder and bowel filling). “Check-and-change” programs involve regular evaluation of the resident's continence status, and changing of undergarments or pads at regular intervals. Check-and-change programs are generally a last resort, and reserved for residents with severe dementia or disability who are unable to participate in other continence programs.20
Certain residents may be candidates for pharmacologic therapy for stress incontinence or overactive bladder. However, risk-versus-benefit assessment should include consideration of possible medication adverse effects, such as confusion, urinary retention, and antagonism of cholinesterase inhibitors.
The Omnibus Budget Reconciliation Act requires physicians to have clinically valid reasons before initiating catheterization. Catheterization may be considered as a palliative care measure in some debilitated residents, with thorough documentation by the physician.20
Falls
Nursing home residents account for 20 percent of persons who die as a result of falls.21 The complications of falling (e.g., fear of subsequent falls) compound existing resident conditions.21 The cause of falls in nursing home residents is usually multifactorial. Muscle weakness and gait problems account for approximately one fourth of falls in nursing homes, and environmental hazards (e.g., wet floors, incorrect bed height, poorly fitted wheelchairs) account for another 16 to 27 percent.21 Multidisciplinary interventions based on fall assessment can reduce the frequency and complications of falls.21,22
The physician's role involves treating health conditions or injuries, eliminating medications that increase fall risk, and ordering prevention measures and rehabilitation therapies for appropriate patients. The care plan should be reevaluated after falls, and the patient should be observed and receive continued supervision.
Restraints
Policies about resident restraint require an approach that attempts to maintain or improve residents' function, using the least amount of restriction. Barring a clear and well-documented reason, restraints should not be used in nursing home residents. In nonemergency situations, physical restraints should be used in nursing home residents only after careful and comprehensive review, assessment, and documentation provide substantial evidence that no safer alternative can be used. Environmental and behavioral alternatives to restraints for problem behavior are listed in Table 4.23
Table 4. Environmental and Behavioral Approaches to Problem Behavior in Nursing Homes
| Activities: rehabilitation, exercise, recreation, nighttime activities, structured routine, allowed wandering Alarms/sensors: bed, chair, door, resident's wrist Altered nursing practices: increased supervision/observation, staffing, staff education; removal of bothersome treatments (e.g., intravenous lines, catheters) Environmental changes: increased lighting, clear pathways, easy access to safe activities, locked exit doors, cloth barriers across doorways attached with Velcro, floor design to enhance visibility of residents Physiologic alternatives: treatment, medication review, measures to prevent delirium Psychosocial alternatives: companionship, interaction with staff, reality orientation, behavioral modification, sensory aids, sensory stimulation, reduced environmental noise Safety in bed: concave bed, reduced bed height, reduced movement at edge of bed (e.g., cushions, water mattress), soft floor mat, beds without wheels, bed trapeze, call button within resident's reach Seating and position support: supportive chairs, chairs with deep seats, customized seating, wheelchair arm cushions Toileting and continence: frequent assistance, scheduled voiding rounds, cleaning promptly after soiling, bedside commode, bathroom identified with picture Individualized interventions: Address sensory deprivation (e.g., glasses, hearing aids, amplifiers) Control door access Facilitate appropriate physical activity/recreation Identify causes of disruptive behavior Increase socialization, reduce isolation Offer patient, staff, and caregiver education about dementia and agitation Provide orienting stimuli (e.g., clocks, calendars, signs, night-lights) Provide routine and structured environment Reassure and verbally calm the resident Segregate disruptive residents from quieter residents Talk to the resident (distract away from the behavior) |
Information from reference 23.
Infectious Diseases
Diagnosis and management of infectious diseases in nursing home residents are complicated by patient comorbidities, as well as clinical and diagnostic limitations within the nursing home environment. A clear diagnosis of infection and appropriate treatment with culture-specific antibiotics help prevent antimicrobial resistance.24 Clinical practice guidelines are available to assist physicians.25
Urinary tract infection (UTI) is the most common infection in nursing home residents.26 To reduce antibiotic use, criteria have been developed for diagnosis and management of UTIs (Figure 1).27
Figure 1. Evaluation and Management of UTI
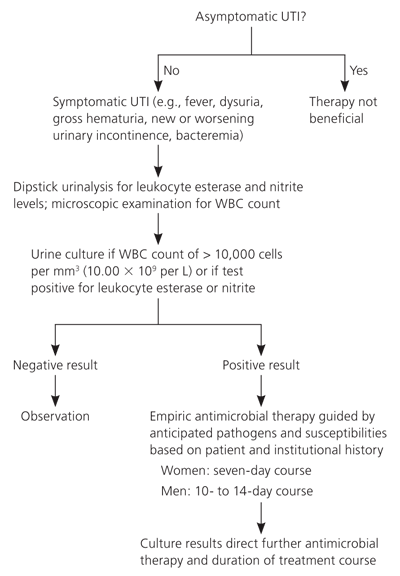
Algorithm for the evaluation and management of UTI in nursing homes. (UTI = urinary tract infection; WBC = white blood cell.)
Information from reference 27.
Pneumonia is the most common cause of infection requiring transfer of nursing home residents to the hospital, and it is a leading cause of mortality.28 Nursing home residents develop pneumonia at a greater rate than community-dwelling older adults.25 Nursing home residents who are hospitalized should receive empiric coverage for methicillin-resistant Staphylococcus aureus, and broad-spectrum coverage for gram-negative and gram-positive organisms. Figure 2 is an algorithm for the management of pneumonia in a nursing home resident.29
Figure 2. Evaluation and Management of Pneumonia

Algorithm for the evaluation and management of pneumonia in nursing homes.
Information from reference 29.
Skin and soft tissue, gastrointestinal, and respiratory infections are also common in nursing home residents. The procedures for evaluating viral respiratory infections are distinct in nursing homes. These procedures include identification of influenza A and other common viruses25 to assist in decisions about patient isolation, and the use of antiviral agents for influenza treatment and prophylaxis.
Table 5 presents guidelines from the Infectious Diseases Society of America for the evaluation and treatment of fever and infection in long-term care facilities.25
Table 5. Evaluation of Fever and Infection in Long-Term Care Facilities
| Signs and symptoms of suspected infection |
| Decline in function, altered cognition, confusion, incontinence, falls, behavior change, decreased appetite (B-II) |
| Fever: single oral temperature of > 100°F (37.8°C), repeated oral temperatures of > 99°F (37.2°C), repeated rectal temperatures of > 99.5°F (37.5°C), or increase in temperature of > 2°F (1.1°C) over baseline (B-III) |
| Resident evaluation |
| Three-tiered approach involving a certified nursing assistant; on-site nurse; and advanced practice nurse, physician assistant, or physician (B-III) |
| Certified nursing assistant should report suspected infection to on-site nurse and document vital signs (B-II) |
| Communication |
| Information should be relayed to responsible advanced practice nurse, physician assistant, or physician for decisions about further evaluation (B-III) |
| The clinical evaluation should be documented in the medical record, and reasoning for withholding any diagnostic and therapeutic interventions documented (B-III) |
| Initial diagnostic testing |
| Advance directives should be reviewed before interventions (B-III) |
| Complete blood count should be performed within 12 to 24 hours of onset of symptoms, consistent with local standards of practice (B-II) |
| Assessment for bacterial infection (with or without fever) warranted with WBC count of ≥ 14,000 cells per mm3 (14.00 × 109 per L) or a left shift (bands or metamyelocytes > 6 percent or total bandneutrophil count of ≥ 1,500 cells per mm3 [1.50 × 109 per L]) (B-II) |
| Additional diagnostic tests may not be indicated in absence of fever, leukocytosis and/or left shift, or evidence of focal infection (C-III) |
| Urinalysis and urine cultures should not be performed in asymptomatic patients (A-I) |
| In noncatheterized patients, laboratory evaluation should be reserved for those with acute onset UTI symptoms; in catheterized patients, evaluation should be considered if urosepsis is suspected, especially in context of recent catheter change or obstruction (A-II) |
| In men, midstream, clean-catch specimens preferred when possible, although freshly applied clean condom external collection system with monitoring of urine output is reasonable (B-II); specimen collection from women may require in-and-out catheterization (B-III) |
| Indwelling catheters should be changed before specimen collection and antibiotic administered in residents with suspected urosepsis (A-II) |
| Urine culture and antibiotic susceptibility testing should be performed only with microscopic or chemical evidence of UTI (B-III) |
| If urosepsis is suspected, urine and paired blood culture specimens and Gram staining of uncentrifuged urine should be obtained (B-III) |
| Blood cultures have low yield and may not influence clinical therapy (B-II), but may be appropriate with suspected bacteremia, adequate access to laboratory facilities, physician coverage of positive cultures, capacity to administer parenteral antibiotics |
| Pneumonia evaluation |
| Pulse oximetry should be performed to document hypoxemia (< 90 percent) and guide decision to transfer to acute care hospital; pulse oximetry should be performed in residents with respiratory rate of > 25 breaths per minute in setting of suspected pneumonia (B-II) |
| Chest radiography should be performed if hypoxemia documented or suspected (B-II) |
| Respiratory viral infection evaluation |
| Nasopharyngeal wash or swab samples of throat and nasopharynx should be performed if respiratory viral infection suspected; sample placed in a single refrigerated viral transport media; virus isolation and rapid testing for influenza A and other common viruses should be initiated (A-III) |
| Evaluation of SSTIs |
| Surface cultures not indicated for most bacterial cultures of SSTIs, except conjunctivitis (B-III) |
| Needle aspiration or deep tissue biopsy for Gram stain and culture indicated when unusual pathogens are suspected, fluctuant areas are present, or initial antimicrobial therapy is unsuccessful (C-III) |
| Deep tissue and bone specimens should be obtained for poorly healing pressure ulcers to guide antimicrobial therapy; magnetic resonance imaging most effective modality to detect osteomyelitis (A-III) |
| Mucocutaneous fungal infections: potassium hydroxide 10% slide preparations; culture for refractory conditions appropriate for identification of drug-resistant species (B-III) |
| Herpes simplex or zoster virus: skin scrapings (Tzanck test) and/or culture, immunofluorescent viral antigen studies, or polymerase chain reaction testing (A-III) |
| Scabies: light microscopy of mites, eggs, or feces on mineral oil preparation (B-III) |
| Evaluation of gastrointestinal infection |
| In absence of outbreak, residents with gastroenteritis and stable clinical status should be evaluated within seven days for volume assessment; no evaluation indicated unless patient is ill or symptoms persist beyond seven days; Giardia species or other protozoa should be considered from stool specimen (B-III) |
| Colitis (fever, severe cramps, and diarrhea, with or without blood and WBCs in stool): resident should be evaluated for Clostridium difficile with toxin assay; if symptoms persist and initial result negative, one or two additional stool specimens should be obtained (A-II) |
| If no antibiotic use within 30 days and negative C. difficile assay, sample for invasive enteropathogens should be obtained (A-II) |
| Public health officials should be notified if gastroenteritis or colitis exceeds facility baseline threshold, or if reportable pathogen is isolated (B-III) |
| Evaluation and treatment of intra-abdominal infections or abscesses should be performed in acute care setting (B-III) |
| Suspected outbreak |
| For infection control, testing should be considered in patients with advance directives prohibiting diagnostic testing (B-III) |
note: Canadian Task Force on the Periodic Health Examination grading system:
Strength of recommendation: A = good evidence to support recommendation; B = moderate evidence; C = poor evidence. Quality of evidence: I = at least one properly randomized, controlled trial; II = at least one well-designed trial without randomization, cohort or case-control studies, multiple time series, or dramatic results from uncontrolled experiments; III = opinions of respected authorities, clinical experience, descriptive studies, or reports of expert committees.
SSTI = skin and soft tissue infection; UTI = urinary tract infection; WBC = white blood cell.
Information from reference 25.
Dementia
As many as 67 to 78 percent of nursing home residents have dementia. Dementia-related behavioral and psychological symptoms often prompt the decision to admit a person to a nursing home.30 Individualized care plans for residents with dementia are developed based on the stage of dementia and associated impairments.31,32 Nonpharmacologic treatment of problem behaviors should be emphasized and includes identifying triggers for the behavior, such as pain, and implementing a multidisciplinary management strategy. Management strategies include changes in patient activity and nursing home care practices, environmental modification, and family education to alter the behavior. Figure 3 is a management approach to dementia-related problem behavior.31
Figure 3. Management of Dementia-Related Behavioral Disturbance
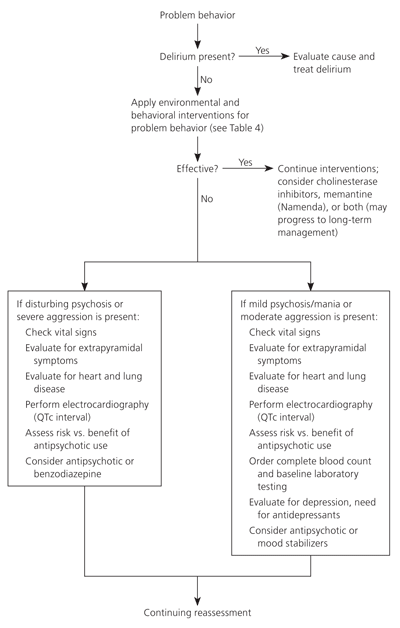
Algorithm for the management of behavioral disturbances in nursing home residents with dementia.
Information from reference 31.
Pharmacologic treatment may be necessary if behavioral issues become dangerous for the resident or for others.31 Antipsychotic therapy is the main treatment for unmanageable behavioral symptoms, such as aggression, hallucinations, and agitation. However, recent literature suggests a 1.6 to 1.7 times higher risk of death in patients treated with antipsychotics versus placebo.31 This risk has led the U.S. Food and Drug Administration to add a warning to all antipsychotic drugs about their use for dementia-related psychosis.31
Delirium
Delirium occurs in up to 60 percent of nursing home residents, and up to 83 percent of all patients at the end of life.33 The diagnostic and treatment approach is no different than for patients admitted to the hospital and includes evaluation for dementia, depression, metabolic disorders, infection, polypharmacy complications, and late-phase disease.33
Depression
It is estimated that 12 to 16 percent of older adults living in nursing homes have major depression.34 The diagnosis of depression is facilitated by multi-disciplinary assessment and the use of screening tools such as the Geriatric Depression Scale, Cornell Scale for Depression in Dementia, Center for Epidemiologic Studies of Depression Scale, and Patient Health Questionnaire.34
Pharmacologic and psychological treatment of depression in a nursing home resident is no different than that for a non-nursing home resident. No antidepressant class is superior; however, selective serotonin reuptake inhibitors and selective norepinephrine reuptake inhibitors are preferred because of their favorable safety and tolerability profiles.35 Choosing which antidepressant is suitable for the individual patient includes recognition of comorbidities, current medications, and the antidepressant's adverse effects. Electroconvulsive therapy may be considered in select patients.
Adverse Drug Events
Adverse drug events are common in nursing homes, ranging from 1.9 to 9.8 events per 100 resident-months. Of these events, 40 to 50 percent are considered preventable.36,37 A general management principle is to consider any new symptom an adverse drug event until proved otherwise.
The Centers for Medicaid and Medicare Services have adopted the Beers criteria, which are based on a list of medications that should be generally avoided in older patients, as regulatory guidance to improve the rate of adverse drug events in nursing homes.38 Other methods for avoiding potentially inappropriate medication use in nursing home residents include reviewing medications at admission, at readmission, at transfers, if any medication is added or discontinued, and when goals of care change; adjusting dosages according to renal function; and closely monitoring patients taking psychotropic medications for benefits versus risks.32,36–38

