
Am Fam Physician. 2018;97(5):310-311
Author disclosure: No relevant financial affiliations.
Clinical Question
Do written action plans for self-management of chronic obstructive pulmonary disease (COPD) reduce the severity of acute exacerbations?
Evidence-Based Answer
Written self-management plans, especially those that include guidance on smoking cessation, increase health-related quality of life in patients with COPD. They also decrease the need for respiratory-related hospital admissions among patients with high or low baseline risk.1 (Strength of Recommendation: A, based on consistent, good-quality patient-oriented evidence.)
Practice Pointers
Self-management plans for patients with COPD have been shown to decrease respiratory- and all-cause–related hospitalizations and improve dyspnea and health-related quality of life.2 A recent recommendation suggests that COPD self-management should motivate, engage, and support patients to positively adapt their behaviors and develop skills to better manage their disease.3 The authors of this Cochrane review sought to demonstrate whether written management plans for COPD exacerbations would positively affect health-related quality of life and decrease the need for acute hospitalizations.1
This Cochrane review included 22 trials and 3,854 patients with COPD.1 Follow-up ranged from two to 24 months. The authors looked for studies in which the interventions included a written action plan, defined as an agreed strategy with actions to be initiated by a patient with COPD when symptoms deteriorate. Health-related quality of life was measured using the validated St. George's Respiratory Questionnaire (SGRQ)4; normal values on this assessment vary with sex and age, and lower scores represent better health-related quality of life. A change of four points is considered the minimal clinically important difference.
Patients who used a written action plan for COPD exacerbations had lower scores on the SGRQ compared with those receiving usual care (mean difference = 2.69 points; 95% confidence interval [CI], 0.9 to 4.49). This review also revealed a decreased need for respiratory-related hospital admissions among patients using written action plans, whether their baseline risk was high (number needed to treat [NNT] to prevent one admission in one year = 12; 95% CI, 7 to 69) or low (NNT to prevent one admission in one year = 17; 95% CI, 11 to 93). No differences were noted in the number of emergency department or outpatient clinic visits, or in dyspnea scores between patients who received a written action plan and those who received usual care.
Subgroup analysis showed that patients with COPD who participated in programs that included a written smoking cessation plan had an improvement in SGRQ scores of 4.98 points (95% CI, 2.78 to 7.17), whereas those who were involved in programs that did not include written smoking cessation plans had an improvement of only 1.33 points (95% CI, 0.27 to 2.94). Although the clinical significance is uncertain, very-low-quality evidence showed a small increase in respiratory-related mortality rates among patients receiving written intervention. The authors of this review posit that this result should be interpreted with caution, at the very least because a comparison of the all-cause mortality rates between the two groups did not reveal a difference.
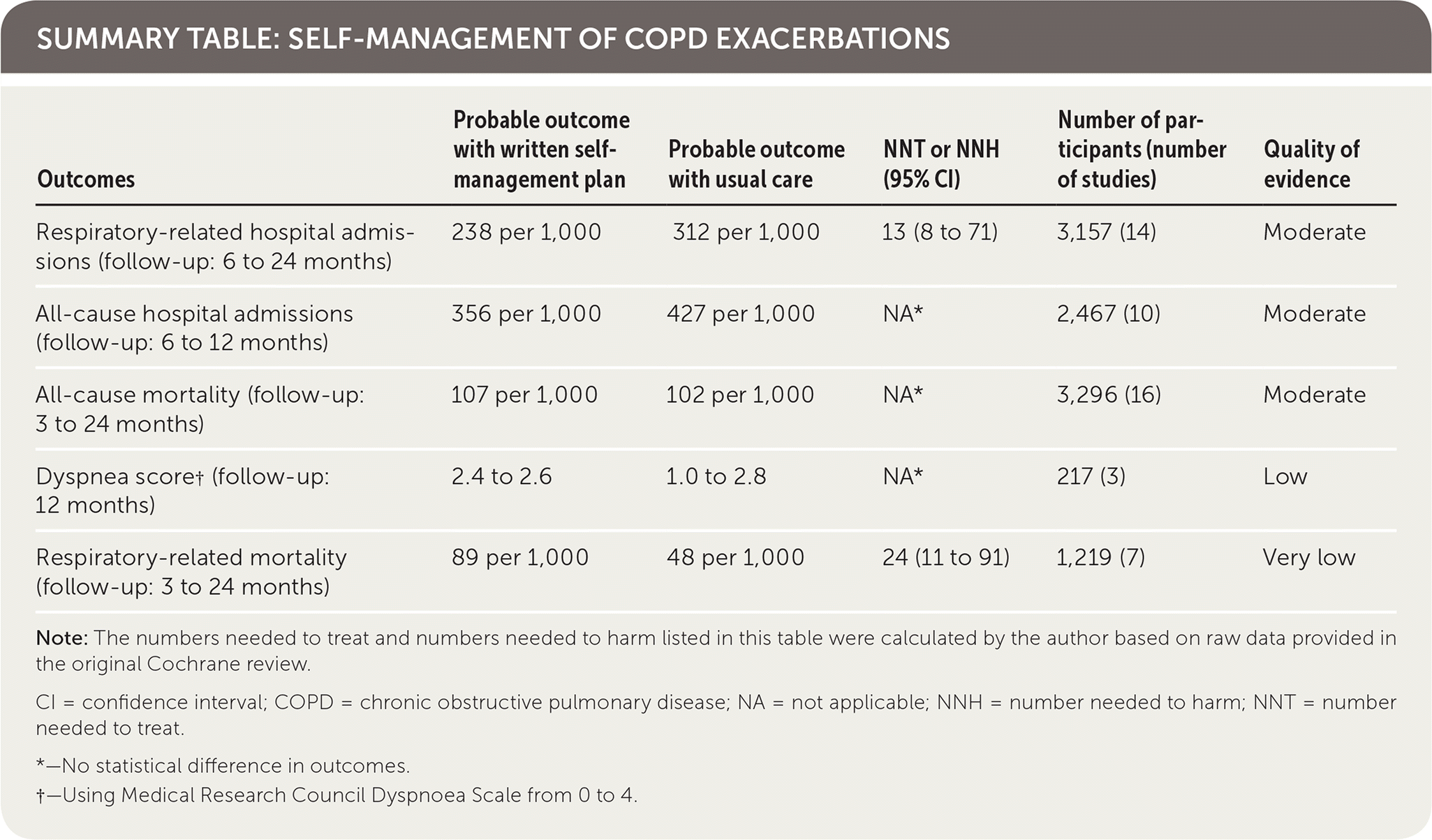
| Outcomes | Probable outcome with written self-management plan | Probable outcome with usual care | NNT or NNH (95% CI) | Number of participants (number of studies) | Quality of evidence |
|---|---|---|---|---|---|
| Respiratory-related hospital admissions (follow-up: 6 to 24 months) | 238 per 1,000 | 312 per 1,000 | 13 (8 to 71) | 3,157 (14) | Moderate |
| All-cause hospital admissions (follow-up: 6 to 12 months) | 356 per 1,000 | 427 per 1,000 | NA* | 2,467 (10) | Moderate |
| All-cause mortality (follow-up: 3 to 24 months) | 107 per 1,000 | 102 per 1,000 | NA* | 3,296 (16) | Moderate |
| Dyspnea score† (follow-up: 12 months) | 2.4 to 2.6 | 1.0 to 2.8 | NA* | 217 (3) | Low |
| Respiratory-related mortality (follow-up: 3 to 24 months) | 89 per 1,000 | 48 per 1,000 | 24 (11 to 91) | 1,219 (7) | Very low |
Current guidelines suggest that patients who have COPD receive a written action plan and participate in case management to prevent and manage exacerbations.5 Family physicians should consider using print copies of individualized plans to review with their patients who have COPD.
The practice recommendations in this activity are available at http://www.cochrane.org/CD011682.
