
Am Fam Physician. 2018;97(8):517-522
Author disclosure: No relevant financial affiliations.
Group A beta-hemolytic streptococcus can cause several postinfectious, nonsuppurative immune-mediated diseases including acute rheumatic fever, poststreptococcal reactive arthritis, pediatric autoimmune neuropsychiatric disorders, and poststreptococcal glomerulonephritis. Except for sporadic outbreaks, poststreptococcal autoimmune syndromes occur most commonly in sub-Saharan Africa, India, Australia, and New Zealand. Children younger than three years are rarely affected by group A streptococcus pharyngitis or rheumatic fever, and usually do not require testing. Rheumatic fever is a rare condition that presents as a febrile illness characterized by arthritis, carditis or valvulitis, and neurologic and cutaneous disease, followed many years later by acquired valvular disease. Recurrence rates are high. In addition to evidence of recent streptococcal infection, two major or one major and two minor Jones criteria are required for diagnosis. Electrocardiography, chest radiography, erythrocyte sedimentation rate, and an antistreptolysin O titer are the most useful initial tests. Echocardiography is recommended to identify patients with subclinical carditis. The arthritis usually responds within three days to nonsteroidal anti-inflammatory drugs. Poststreptococcal reactive arthritis is nonmigratory, can affect any joint, and typically does not respond to aspirin. Pediatric autoimmune neuropsychiatric disorders affect the basal ganglia and are manifested by obsessive-compulsive and tic disorders. The presentation of poststreptococcal glomerulonephritis ranges from asymptomatic microscopic hematuria to gross hematuria, edema, hypertension, proteinuria, and elevated serum creatinine levels.
Streptococcus pyogenes (group A beta-hemolytic streptococcus [GABHS]) is an anaerobic gram-positive coccus whose only reservoir is humans. It causes more than 700 million illnesses and more than 500,000 deaths worldwide each year.1 GABHS causes several postinfectious, nonsuppurative immune-mediated diseases, including acute rheumatic fever, poststreptococcal reactive arthritis, pediatric autoimmune neuropsychiatric disorders associated with streptococcal infections (PANDAS), and poststreptococcal glomerulonephritis. This article focuses on the recognition and management of these immune-mediated sequelae.
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Treatment of group A streptococcal pharyngitis with antibiotics is indicated in patients with a positive rapid antigen detection test or throat culture result. | B | 7, 13, 14, 17 |
| Echocardiography should be performed to assess for subclinical carditis in patients with diagnosed or suspected acute rheumatic fever and no auscultatory findings. | C | 33 |
| Nonsteroidal anti-inflammatory drugs (aspirin or naproxen) are recommended for treating arthritis in acute rheumatic fever as soon as the diagnosis is confirmed. | B | 6, 14, 19 |
| Secondary antibiotic prophylaxis is indicated for patients with acute rheumatic fever or poststreptococcal reactive arthritis. | C | 6, 14, 21, 24 |
Over the past century in the United States, the incidence of GABHS disease has decreased sharply, and the clinical presentation has evolved.2–5 Scarlet fever is milder than in historic accounts, acute rheumatic fever is rare (one in 1,000,000 persons), and poststreptococcal glomerulonephritis is now more common in patients older than 60 years who tend to have debilitating conditions.5–11 Except for sporadic outbreaks, poststreptococcal autoimmune syndromes occur most commonly in sub-Saharan Africa, India, Australia, and New Zealand.1,6,12
Early antibiotic treatment in patients with GABHS pharyngitis and positive results on a rapid antigen detection test or throat culture may prevent suppurative complications and rheumatic fever, shorten the clinical course by up to 16 hours, and reduce transmission.7,12–16 Penicillin is the preferred agent; a cephalosporin, azithromycin (Zithromax), clindamycin, or clarithromycin (Biaxin) is recommended for patients with penicillin allergy.7,12–20 Amoxicillin (50 mg per kg per day, up to 1,000 mg) is an acceptable alternative.6,12–14,21 Antibiotics for GABHS pharyngitis and impetigo do not prevent poststreptococcal glomerulonephritis.13,15,19 Although there is some concern that antibiotic treatment within 48 hours of symptom onset may suppress host antibody response and increase the risk of recurrent pharyngitis, treatment should not be delayed.20 Treating GABHS within nine days of symptom onset will prevent acute rheumatic fever in two-thirds of patients.6,15,16,21 Although one study suggested a potential relationship between the carrier state and the neuropsychiatric symptoms of PANDAS, asymptomatic carriers are at low risk of nonsuppurative complications and do not warrant evaluation.12,21,22
Pathophysiology
Antibodies against the streptococcal M protein allow the host to protect itself from future infection from a similar M-type organism.23 However, these antibodies are the pathophysiologic basis for postinfectious autoimmune sequelae: deposition of immune complexes in poststreptococcal glomerulonephritis, antibody-directed molecular mimicry with abnormal host immune response in acute rheumatic fever, and cross-reactive autoantibodies in the basal ganglia in Sydenham chorea.24–26 Genetic susceptibility, humoral immunity, and cellular response also have a role.23–30
Case Study
A healthy 10-year-old girl presents with a sore throat, swollen anterior cervical lymph nodes, and fever of two days' duration. She does not have a cough, congestion, rhinorrhea, or myalgias. Her temperature is 101.5°F (38.6°C), and her tonsils are enlarged with exudates and tender cervical adenopathy. Examination findings are otherwise unremarkable. Results of a rapid antigen test are positive for GABHS, and once-daily amoxicillin is prescribed.6,12–14,21,31 Her parents discontinue the antibiotics after three days. Up to 35% of her close contacts may become infected,14 and four potential scenarios may develop.
SCENARIO 1: ACUTE RHEUMATIC FEVER
Two weeks after her original symptoms resolved, the patient presented to the emergency department with a four-day history of intermittent fever up to 102.7°F (39.3°C). Two days earlier, she had right hip pain and a swollen, tender left knee. On presentation, she had left ankle and right knee pain, which responded to a three-day course of naproxen. She also had sharp chest pain associated with shortness of breath, but no rash or bumps beneath the skin. She had tachycardia (120 beats per minute) and temperature of 102.2°F (39°C). Physical examination revealed a 2/6 holosystolic murmur at the apex with radiation to the axilla. Her erythrocyte sedimentation rate (ESR) was 120 mm per hour, an antistreptolysin O (ASO) titer was positive, chest radiography showed cardiomegaly, and a first-degree heart block with sinus tachycardia was noted on electrocardiography. Echocardiography revealed mild mitral valve regurgitation.
The patient has acute rheumatic fever. This rare condition usually follows GABHS pharyngitis by 10 to 28 days and rarely affects children younger than three years.6,13,14,20,32 In addition to evidence of recent streptococcal infection, two major or one major and two minor Jones criteria are required for diagnosis (Table 1).5,6,14,19,21,32,33

| Major criteria |
| Carditis |
| Erythema marginatum |
| Polyarthritis |
| Subcutaneous nodules |
| Sydenham chorea |
| Minor criteria |
| Arthralgia |
| Fever |
| Increased erythrocyte sedimentation rate or C-reactive protein level |
| Prolonged PR interval |
| Evidence of recent group A streptococcal infection |
| Increased antistreptococcal antibody level |
| Positive rapid antigen test or throat culture |
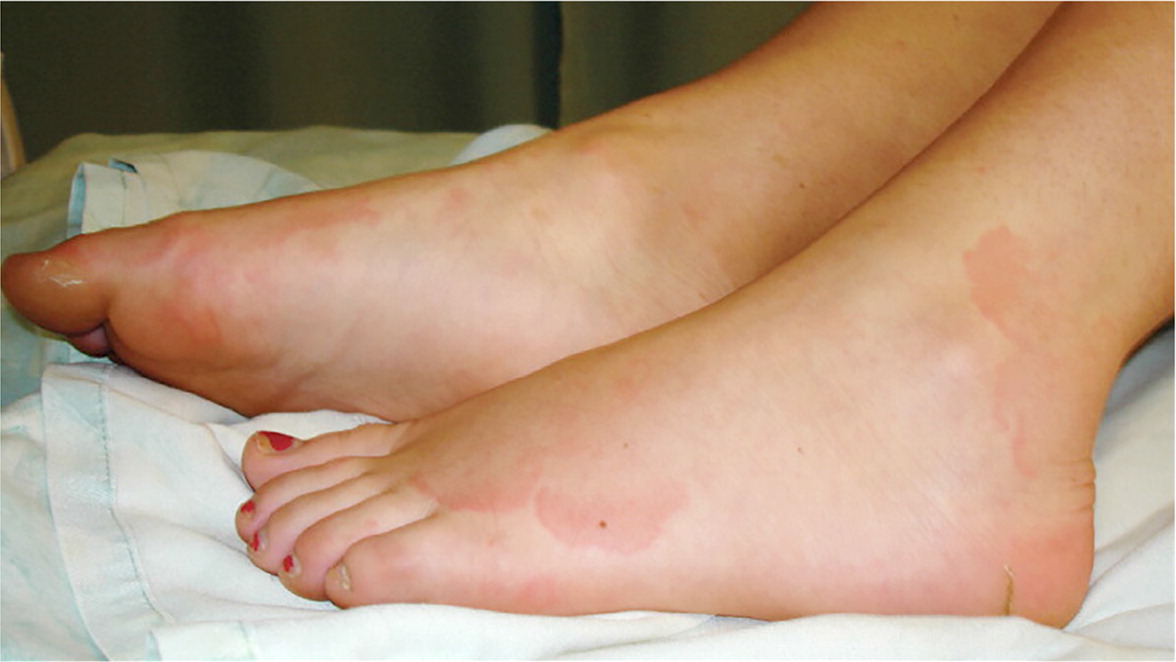
Self-limited migratory polyarthritis affects the large joints in up to 75% of patients with this condition.6,14,32 A dramatic response to aspirin or naproxen is characteristic.6,32 Carditis is present in 50% to 60% of cases.6,23 Evidence of valve disease, various degrees of heart block, and cardiomegaly with heart failure symptoms may be present. Recurrent episodes of acute rheumatic fever lead to rheumatic heart disease in up to 60% of patients; its primary manifestation is valve disease up to 20 years after the initial infection.14 The mitral valve is most commonly affected. Ery thema marginatum and subcutaneous nodules tend to occur only in patients with carditis. Erythema marginatum is an evanescent, nonpruritic, pink to slightly red rash involving the trunk and proximal limbs that rapidly advances (Figure 1).34 The face is usually spared.14,32 Subcutaneous nodules typically last about one month, are usually located over bony prominences or near tendons, and are firm and painless.14,32 Sydenham chorea presents abruptly and consists of purposeless, nonrhythmic involuntary movements that cease during sleep, muscular weakness, and emotional disturbances ranging from inappropriate outbursts to transient psychosis. This condition can present up to eight months after the initial GABHS infection and usually resolves completely within two to three years.14,32
Electrocardiography, chest radiography, ESR, C-reactive protein level, and ASO titer are the most useful initial tests. Echocardiography is recommended to identify patients with subclinical carditis.33 Treatment depends on the presentation. Aspirin or other nonsteroidal anti-inflammatory drugs are effective for treating arthritis and should be started as soon as acute rheumatic fever is diagnosed.6,14,19 Antibiotics are warranted for any active GABHS infection and for secondary prophylaxis to prevent recurrent acute rheumatic fever. Monthly intramuscular injections of penicillin G benzathine are recommended for secondary prophylaxis in patients with carditis with or without valvular disease, and should be continued until the patient is an adult and has no recurrence for 10 years.6,21,24 Longer periods are necessary if the patient has residual heart disease6,21 (Table 221). Household contacts should be tested and treated if necessary.6

| Clinical scenario | Duration of therapy |
|---|---|
| Rheumatic fever with carditis and residual heart disease (persistent valvular disease*) | 10 years or until 40 years of age (whichever is longer); lifetime prophylaxis may be needed |
| Rheumatic fever with carditis but no residual heart disease (no valvular disease*) | 10 years or until 21 years of age (whichever is longer) |
| Rheumatic fever without carditis | 5 years or until 21 years of age (whichever is longer) |
SCENARIO 2: POSTSTREPTOCOCCAL REACTIVE ARTHRITIS
The patient presents to the emergency department with the sudden onset of right hip and knee pain 10 days after being diagnosed with GABHS pharyngitis. She has no rash, subcutaneous nodules, chest pain, shortness of breath, palpitations, or cough. An ASO titer is positive, ESR is 50 mm per hour, and white blood cell count is normal.
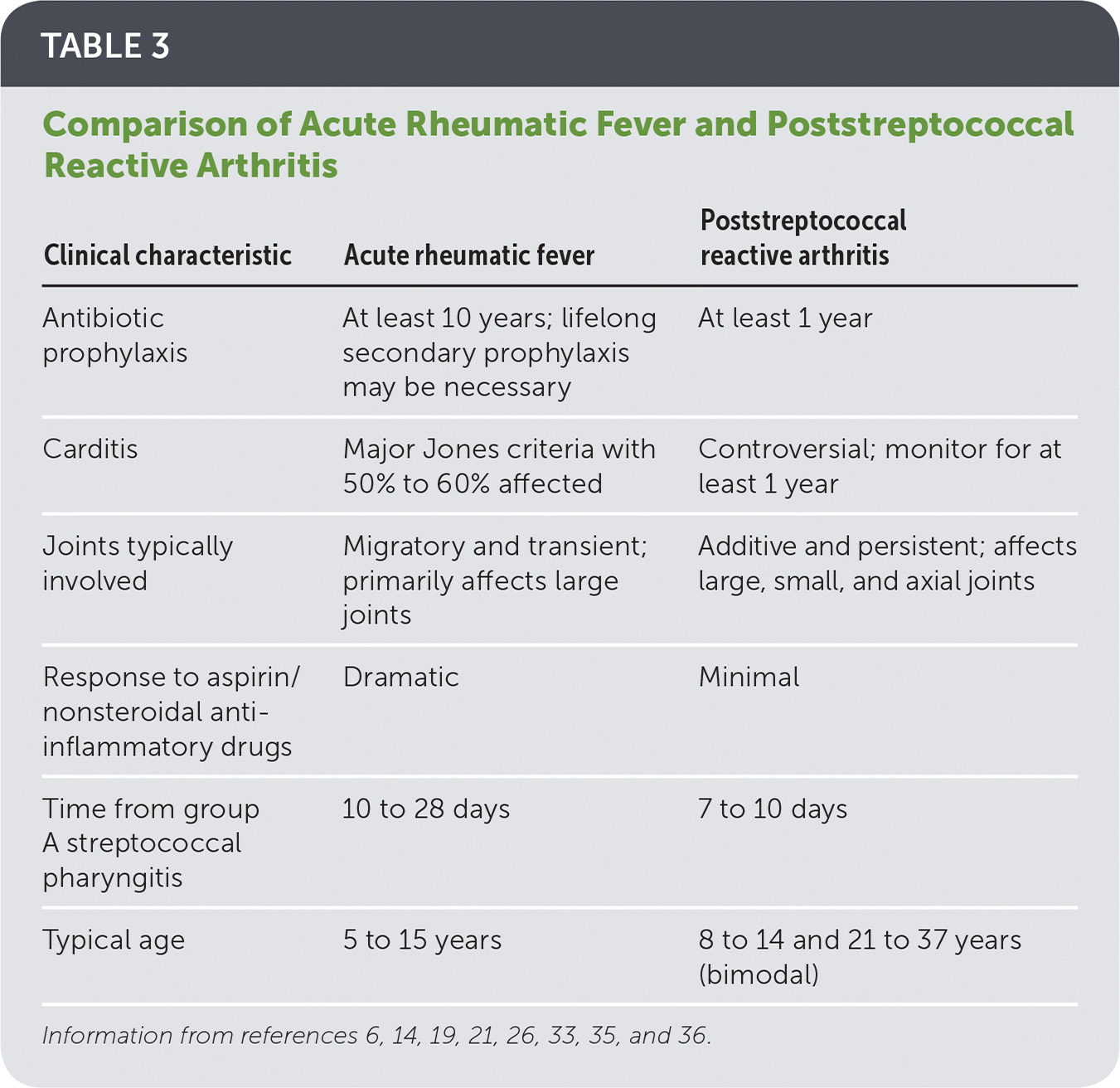
Patients with poststreptococcal reactive arthritis usually present seven to 10 days after GABHS pharyngitis with nonmigratory arthritis and no other Jones criteria for acute rheumatic fever.35,36 The arthritis may be persistent or recurrent, and the knee, ankle, hip, and wrist are most commonly affected.35,36 Joint aspiration may be indicated if effusion is noted. A complete blood count, ESR or C-reative protein level, and ASO titer are reasonable initial tests. Markers of inflammation tend to be much lower than in acute rheumatic fever, and aspirin and other nonsteroidal anti-inflammatory drugs are much less effective. Most experts recommend monitoring for carditis for several months and prescribing secondary antibiotic prophylaxis for at least one year.14,21,35,36 Table 3 compares the clinical characteristics of acute rheumatic fever and poststreptococcal reactive arthritis.6,14,19,21,26,33,35,36
| Clinical characteristic | Acute rheumatic fever | Poststreptococcal reactive arthritis |
|---|---|---|
| Antibiotic prophylaxis | At least 10 years; lifelong secondary prophylaxis may be necessary | At least 1 year |
| Carditis | Major Jones criteria with 50% to 60% affected | Controversial; monitor for at least 1 year |
| Joints typically involved | Migratory and transient; primarily affects large joints | Additive and persistent; affects large, small, and axial joints |
| Response to aspirin/nonsteroidal anti-inflammatory drugs | Dramatic | Minimal |
| Time from group A streptococcal pharyngitis | 10 to 28 days | 7 to 10 days |
| Typical age | 5 to 15 years | 8 to 14 and 21 to 37 years (bimodal) |
SCENARIO 3: PANDAS
Three months after the initial infection, the patient is treated for a second episode of GABHS pharyngitis. Three months after that, she presents with sudden onset of unpleasant thoughts and frequent handwashing for no apparent reason. She also has facial grimacing and head jerking. Her ASO level is elevated.
The patient has the controversial condition known as PANDAS.21,24,37–39 There is some debate about the existence of this condition, originally described in 1998, and its hypothesized pathogenesis. A national health insurance study found that multiple GABHS infections over one year increased the risk of neuropsychiatric symptoms, but no association was demonstrated in other studies.24,37–39 Five clinical criteria have been proposed for diagnosis: obsessive-compulsive or a tic disorder; prepubertal symptom onset; an episodic course characterized by acute, severe onset and dramatic symptom exacerbation; neurologic abnormalities such as choreiform movements during symptom exacerbations; and a temporal relationship between GABHS infection and symptom exacerbation.40,41 Treatment includes cognitive behavior therapy, selective serotonin reuptake inhibitors, steroids, intravenous immunog lobulins, or plasmapheresis.14,21,24,40,41
SCENARIO 4: POSTSTREPTOCOCCAL GLOMERULONEPHRITIS
Two weeks after symptom resolution, the patient presents with bilateral lower extremity edema and dark urine. She has no cough, shortness of breath, palpitations, chest pain, joint pain, or fever. Vital signs are normal, and physical examination findings are unremarkable except for bilateral lower extremity edema. Urinalysis reveals hematuria. The ASO titer is positive, blood urea nitrogen and creatinine levels are mildly elevated, and the C3 complement level is low.
The patient has poststreptococcal glomerulonephritis. The latent period is one to three weeks after GABHS pharyngitis or three to six weeks after GABHS pyoderma. The presentation varies from asymptomatic microscopic hematuria to gross hematuria, edema, hypertension, proteinuria, and elevated serum creatinine levels. More than 97% of the 470,000 annual cases occur in resource-poor settings.42,43 The prognosis is excellent for most children, but less so for older adults or certain high-risk populations.9 Treatment is supportive. Salt and water restriction with concurrent furosemide (Lasix) can help treat the edema and hypertension, if present. Diuresis usually begins within one week; dialysis is rarely required. Renal function normalizes in four to six weeks and hematuria resolves in three to six months, but proteinuria may persist for up to three years.14 Rarely, a patient will have a relapse years after the initial illness.14
This article updates a previous article on this topic by Hahn, et al.19
Data Sources: An online search was conducted using the key terms GAS diseases, GAS pharyngitis, sore throat, Streptococcus pyogenes, acute rheumatic fever, poststreptococcal reactive arthritis, PANDAS, poststreptococcal glomerulonephritis, streptococcal vaccines, evolving GAS disease, immune response/pathogenesis of GAS disease, complications of GAS disease, invasive GAS disease, PAN, rheumatic heart disease, treatment of GAS disease, Jones criteria, echocardiography in RF, antibiotics for GAS disease, once-daily amoxicillin, streptococcal asymptomatic carriers, and primary/secondary prevention of GAS disease. A broad overview of the topic was done on national websites such as Agency for Healthcare Research and Quality, National Guideline Clearinghouse, and Centers for Disease Control and Prevention. After the background reading, the search was refined to identify major scholarly and professional resources using the following databases: National Guideline Clearinghouse, PubMed, Essential Evidence Plus, the Cochrane database, OVID, and the U.S. Preventive Services Task Force, as well as the Agency for Healthcare Research and Quality evidence reports. Search dates: December 2016 to January 2018.
