Based on systematic surveillance of more than 110 medical journals, 247 studies met criteria as POEMs (patient-oriented evidence that matters) in 2017. Members of the Canadian Medical Association identified 20 of these POEMs as most relevant to practice. This article reviews the clinical questions and bottom-line answers from these studies. Blood pressure should be measured after a period of rest, using a bare arm, and orthostatic blood pressure is more predictive when measured after one minute of standing rather than three minutes. Intensive blood pressure lowering results in cardiovascular benefits but also renal harms in high-risk patients with an average age of 68 years. The initiation of a statin for primary prevention does not reduce cardiovascular events in adults 65 years or older. Sterile gloves do not reduce the risk of infection for common outpatient skin procedures, and the preferred approach to managing onychomycosis is empiric oral terbinafine. Routine home glucose monitoring is not needed in patients with type 2 diabetes mellitus, and trying to achieve an A1C target level of 6.0% rather than 7.0% to 7.9% does not improve outcomes and may be harmful. Fasting blood glucose and A1C levels have limited accuracy for identifying glucose intolerance, and patients 65 years and older with thyroid-stimulating hormone levels between 4.6 and 10.0 mIU per mL should be rechecked before considering treatment. Gabapentin and pregabalin are not effective for acute or chronic low back pain, even in patients with sciatica. Physical therapy does not provide any additional benefit over usual care in patients with acute ankle sprain, and corticosteroid injections for knee osteoarthritis are ineffective and may damage cartilage. A two-question screening test can rule out depression in older adults; a large U.S. trial continued to find no benefit to prostate cancer screening; and clinicians need to be thoughtful about how they discuss recommendations to stop screening for cancer in older patients. Finally, ibuprofen, naproxen, and celecoxib have similar risks of adverse events, and continuous positive airway pressure in patients with obstructive sleep apnea does not reduce the risk of cardiovascular events.
The volume of studies published annually has expanded greatly in recent decades. For example, 6,762 studies were indexed as randomized controlled trials in PubMed in 1990, compared with 24,434 in 2015. It is increasingly difficult for primary care physicians, who have a broad scope of practice, to remain current with the most important new research. To address this issue, for more than 20 years, a group of clinicians who are experts in evidence-based medicine has systematically reviewed more than 110 English-language research journals to identify the evidence most likely to change primary care practice. The group includes experts in family medicine, pharmacology, hospital medicine, and women's health.1,2
The goal of the review process is to identify POEMs: patient-oriented evidence that matters. A POEM must report patient-oriented outcomes, such as improvement in symptoms, morbidity, or mortality; be free of important methodologic bias; and recommend a change in practice for many physicians. Adopting valid POEMs in clinical practice could therefore result in improved patient outcomes. Of more than 20,000 research studies published in 2017 in these journals, 247 met these criteria for validity, relevance, and practice change.
Since 2005, the Canadian Medical Association (CMA) has paid for a subscription to POEMs for all of its members. Each member has the option to receive the daily POEM by e-mail. When members read the POEM, they can also rate it with a validated tool called the Information Assessment Method. This tool addresses relevance to clinicians, cognitive impact, use in practice, and expected health benefits if that POEM is applied in practice.3 For this article we identified the 20 POEMs that were rated highest for clinical relevance by CMA members in 2017. In the seventh installment of this annual series,4–9 we summarize the clinical question and bottom-line answer for each of the top 20 research studies identified as POEMs, organized by topic and followed by a brief discussion. We also review the five most relevant practice guidelines.
Cardiovascular Disease and Hypertension
TABLE 1. Cardiovascular Disease and Hypertension

| Clinical question | Bottom-line answer |
|---|---|
| 1. Measuring blood pressure What is the best way to measure blood pressure?10 | Measure blood pressure using a completely bare arm. To get the most accurate measure, let patients relax for a few minutes, and then measure their blood pressure on a completely bare arm. Does a difference of 4 mm Hg systolic and 6 to 7 mm Hg diastolic matter? It might, especially when deciding whether to add a second or third drug. |
| 2. Measuring blood pressure How well does monitoring blood pressure for 30 minutes in the office compare with a single office reading in patients suspected of having white coat hypertension?11 | Let patients rest, and consider using an average of several automated cuff measures. In this Dutch study, monitoring blood pressure readings in the office for 30 minutes resulted in markedly lower readings compared with the last office reading (approximately 23/12 mm Hg lower). The clinicians report they would be much less likely to intensify treatment if they used these readings. |
| 3. Harms of intensive blood pressure control Does intensive systolic blood pressure lowering in older patients increase the likelihood of renal dysfunction?12 | In older patients, targeting 120/80 mm Hg has benefits but also increases the risk of renal dysfunction. In this post-hoc analysis of the previously published Systolic Blood Pressure Intervention Trial (SPRINT), lowering the systolic blood pressure of patients who are at increased risk of cardiovascular events (average age = 68 years) will decrease their risk of CVD but increase their likelihood of developing moderate renal dysfunction. It will not, at least over three years, increase their likelihood of developing end-stage renal disease. |
| 4. Measuring orthostatic blood pressure Is it better to evaluate for orthostatic hypotension after one minute or three minutes of standing?13 | Measure blood pressure after the patient has been standing for one minute, not three minutes. Finding an orthostatic drop within the first minute after standing more accurately predicts dizziness and future adverse events than finding it at the currently recommended three minutes. |
| 5. Treating hyperlipidemia in older patients In patients older than 65 years with elevated low-density lipoprotein levels but no CVD, does cholesterol lowering decrease mortality or morbidity?14 | There is no clear evidence of benefit for treating hyperlipidemia in older patients, especially in those older than 75 years. If a patient makes it to 65 years of age without developing CVD, lowering his or her cholesterol level at this point is not effective, and might even be harmful if treatment is started at 75 years of age. Given the lack of benefit also shown in other studies, it might be time to stop checking—and treating—high cholesterol in these age groups. |
CVD = cardiovascular disease.
The first group of POEMs focuses on cardiovascular disease (CVD) and hypertension (Table 1),10–14 and two of these POEMs address the proper way to measure blood pressure, a part of the care of almost every patient. Although it may be tempting to save a few seconds and measure the blood pressure through a patient's shirt or sweater, Study 1, a Japanese study, found that measuring through clothing can add 6 to 7 mm Hg to the diastolic blood pressure and 4 mm Hg to the systolic blood pressure.10 In Study 2, Dutch patients with suspected white coat hypertension were asked to sit quietly in a room while an automated cuff measured their blood pressure every five minutes. The mean of these six measurements was 23/12 mm Hg lower than the initial office blood pressure.11 Study 3 is a reanalysis of data from the Systolic Blood Pressure Intervention Trial (SPRINT). It concluded that for patients with hypertension but without diabetes mellitus who are at increased risk of CVD (average age = 68 years; 61% with a 10-year cardiovascular risk of 15% or greater), a more aggressive blood pressure target has cardiovascular benefits and renal harms, and requires more medications.12 As with the Dutch study, the SPRINT trial used a similar measurement approach (i.e., the mean of three automated blood pressure measurements after the patient had rested quietly for at least five minutes), so before increasing the number of blood pressure medications that patients use to hit those targets, it is critical to measure blood pressure the same way as the SPRINT investigators. Another study of blood pressure measurement, Study 4, concluded that when evaluating a patient for possible orthostatic hypotension, it is better to measure the blood pressure one minute after standing rather than three minutes.13
Statins are commonly prescribed to patients 65 years and older, but are they effective for primary prevention of CVD? Study 5 randomized nearly 3,000 adults 65 years and older without known CVD to receive pravastatin (Pravachol; 40 mg per day) or placebo. No reduction in coronary events or all-cause mortality was found, and a nonsignificant trend toward higher mortality in patients older than 75 years was observed in those taking the statin (hazard ratio = 1.34; 95% confidence interval, 0.98 to 1.84).14
Infections
TABLE 2. Infections

| Clinical question | Bottom-line answer |
|---|---|
| 6. Use of sterile gloves Does the use of sterile gloves when performing minor outpatient cutaneous surgeries reduce the risk of infection?15 | Sterile gloves offer no benefit for minor outpatient skin procedures. Eight studies with more than 2,700 patients found no difference in the risk of infection between sterile or nonsterile gloves for common outpatient skin procedures, such as laceration repair and lesion excision. The relative risk of infection was a nonsignificant 0.95 (95% confidence interval, 0.65 to 1.40). |
| 7. Diagnosing onychomycosis Is confirmatory diagnostic testing cost-effective for the management of clinically suspected onychomycosis?16 | Confirmatory testing is generally unnecessary for clinically suspected onychomycosis. The most cost-effective approach to a patient with clinically suspected onychomycosis is empiric therapy with oral terbinafine (Lamisil). The chance of liver injury is estimated to be only one in 50,000 to one in 120,000, so testing to confirm the diagnosis would cost tens of millions of dollars per case of liver injury avoided. If you plan to prescribe the less effective and much more expensive topical solution efinaconazole (Jublia), then confirmatory testing with periodic acid–Schiff stain reduces costs. |
Two POEMs address the prevention and treatment of common infections in primary care (Table 2).15,16 Study 6 is a systematic review that found no increase in infections or complications when outpatient skin procedures were performed with nonsterile gloves.15 Study 7 questions the requirement by many insurance companies that clinicians must first test a toenail with clinically obvious onychomycosis for fungal infection before they will pay for a course of an antifungal drug. This also delays treatment unnecessarily. This cost-effectiveness analysis found that empiric therapy with oral terbinafine (Lamisil) without diagnostic testing was the most cost-effective strategy.16
Diabetes Mellitus and Thyroid Disease
TABLE 3. Diabetes Mellitus and Thyroid Disease
| Clinical question | Bottom-line answer |
|---|---|
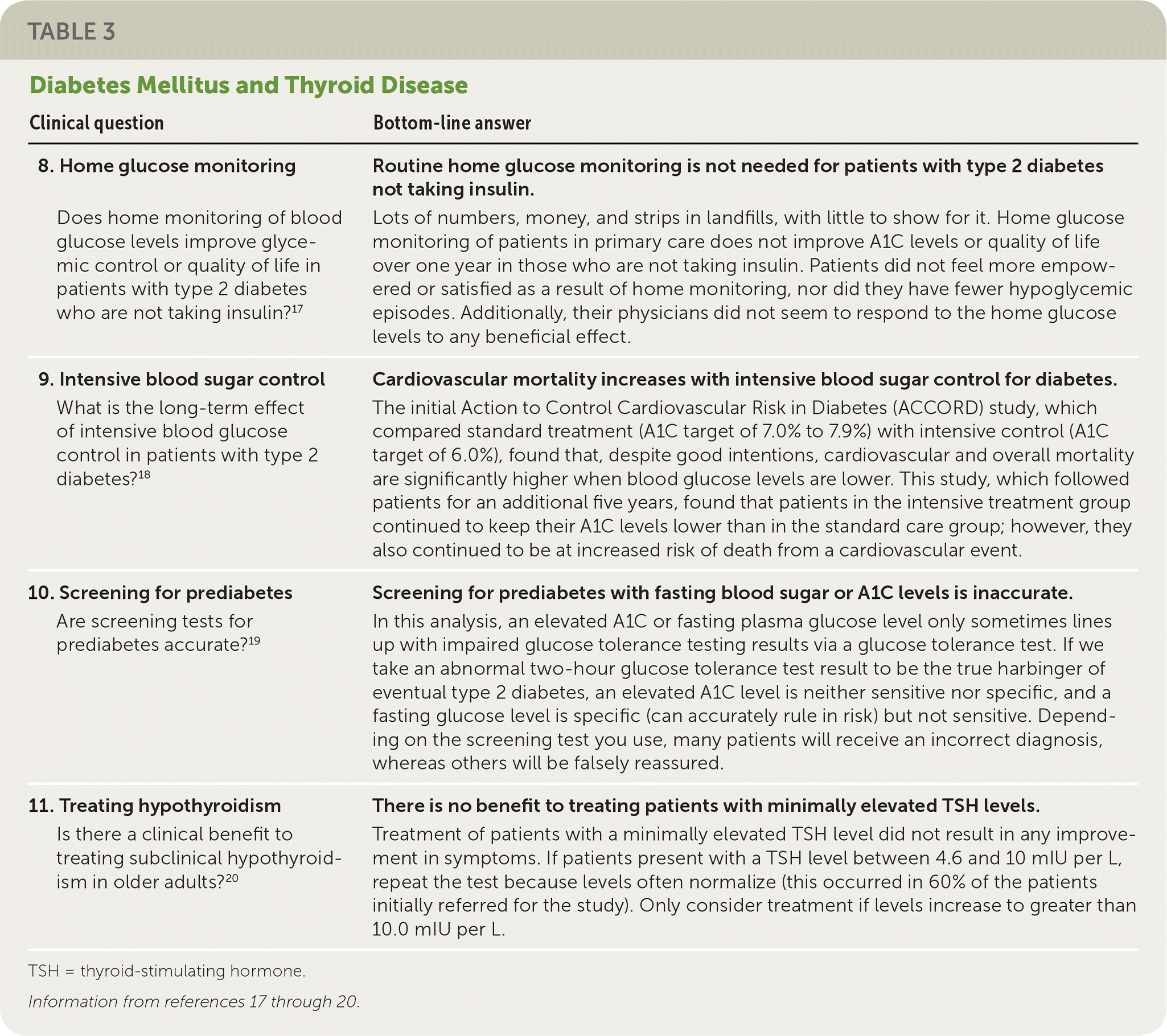
| 8. Home glucose monitoring Does home monitoring of blood glucose levels improve glycemic control or quality of life in patients with type 2 diabetes who are not taking insulin?17 | Routine home glucose monitoring is not needed for patients with type 2 diabetes not taking insulin. Lots of numbers, money, and strips in landfills, with little to show for it. Home glucose monitoring of patients in primary care does not improve A1C levels or quality of life over one year in those who are not taking insulin. Patients did not feel more empowered or satisfied as a result of home monitoring, nor did they have fewer hypoglycemic episodes. Additionally, their physicians did not seem to respond to the home glucose levels to any beneficial effect. |
| 9. Intensive blood sugar control What is the long-term effect of intensive blood glucose control in patients with type 2 diabetes?18 | Cardiovascular mortality increases with intensive blood sugar control for diabetes. The initial Action to Control Cardiovascular Risk in Diabetes (ACCORD) study, which compared standard treatment (A1C target of 7.0% to 7.9%) with intensive control (A1C target of 6.0%), found that, despite good intentions, cardiovascular and overall mortality are significantly higher when blood glucose levels are lower. This study, which followed patients for an additional five years, found that patients in the intensive treatment group continued to keep their A1C levels lower than in the standard care group; however, they also continued to be at increased risk of death from a cardiovascular event. |
| 10. Screening for prediabetes Are screening tests for prediabetes accurate?19 | Screening for prediabetes with fasting blood sugar or A1C levels is inaccurate. In this analysis, an elevated A1C or fasting plasma glucose level only sometimes lines up with impaired glucose tolerance testing results via a glucose tolerance test. If we take an abnormal two-hour glucose tolerance test result to be the true harbinger of eventual type 2 diabetes, an elevated A1C level is neither sensitive nor specific, and a fasting glucose level is specific (can accurately rule in risk) but not sensitive. Depending on the screening test you use, many patients will receive an incorrect diagnosis, whereas others will be falsely reassured. |
| 11. Treating hypothyroidism Is there a clinical benefit to treating subclinical hypothyroidism in older adults?20 | There is no benefit to treating patients with minimally elevated TSH levels. Treatment of patients with a minimally elevated TSH level did not result in any improvement in symptoms. If patients present with a TSH level between 4.6 and 10 mIU per L, repeat the test because levels often normalize (this occurred in 60% of the patients initially referred for the study). Only consider treatment if levels increase to greater than 10.0 mIU per L. |
TSH = thyroid-stimulating hormone.
Three POEMs addressed the management of type 2 diabetes (Table 3).17–20 In Study 8, a well-designed U.S. randomized trial confirmed what had been previously observed in a number of European studies: routine self-monitoring in patients with type 2 diabetes who are not taking insulin does not improve any clinical outcomes.17 Patients should have a glucometer and can use it when they are sick or symptomatic from diabetes, but routine use is not needed. Study 9 is a long-term follow-up to the landmark ACCORD (Action to Control Cardiovascular Risk in Diabetes) trial. Like the ACCORD trial, it found that although patients randomized to tighter glycemic control had lower mean A1C levels, they also continued to have a greater risk of cardiovascular events.18 Study 10 is a systematic review of the accuracy of A1C levels and fasting glucose levels at identifying patients with an abnormal glucose tolerance test. Neither test was sensitive (25% to 49%), although fasting glucose levels were more specific, providing moderately strong evidence for abnormal glucose tolerance when elevated.19 The final study in this group, Study 11, provides guidance on how to treat patients with subclinical hypothyroidism. This randomized trial of patients 65 years and older with moderately elevated thyroid-stimulating hormone levels but no or minimal symptoms found that if the level is between 4.6 and 10.0 mIU per mL, it often normalizes on repeat testing, and treating this group does not improve symptoms.20
Musculoskeletal Conditions
TABLE 4. Musculoskeletal Conditions

| Clinical question | Bottom-line answer |
|---|---|
| 12. Pregabalin (Lyrica) for sciatica Is pregabalin an effective treatment for the pain of acute or chronic sciatica?21 | Pregabalin is not effective for patients with acute or chronic sciatica. This study randomized 207 patients with moderate to severe sciatica, and followed them for one year. The authors concluded that pregabalin does not relieve pain, improve function, or improve any other outcomes in patients with sciatica. |
| 13. Gabapentin (Neurontin) and pregabalin for back pain Are gabapentinoids safe and effective in treating patients with chronic low back pain?22 | Gabapentinoids are ineffective for patients with chronic low back pain. The existing data on gabapentinoids for chronic low back pain are limited in number and quality. The amount of pain reduction is low to moderate, whereas the rate of adverse effects is high. The few studies that assessed function found no improvement. |
| 14. Physical therapy for ankle sprain In patients with mild to moderate ankle sprain, does physical therapy (physiotherapy) hasten or improve recovery?23 | Physical therapy is not helpful for acute ankle sprain. Physical therapy (up to seven sessions) does not hasten resolution of symptoms or improve function in adults with ankle sprain. Approximately 60% of patients who receive usual care or physical therapy do achieve excellent resolution. Send patients home with the usual RICES protocol: rest, ice, compression, elevation, and splinting. |
| 15. Corticosteroid injections for knee osteoarthritis Do intra-articular corticosteroids improve pain and function and decrease cartilage loss in adults with osteoarthritis of the knee?24 | Corticosteroid injections do not improve outcomes for knee osteoarthritis, and may be harmful. This well-done study found that regular three-month intra-articular injections of triamcinolone for two years resulted in no significant difference in pain and function assessments compared with saline. However, a significant increase in cartilage loss and damage occurred in patients receiving corticosteroids compared with saline. |
The next group of POEMs addresses musculoskeletal conditions (Table 4).21–24 Gabapentin (Neurontin) and pregabalin (Lyrica) have become popular options for the management of acute and chronic low back pain. Study 12, a well-designed Australian randomized trial, found that in patients with moderate to severe sciatica, pregabalin did not improve any clinical outcomes.21 Similarly, Study 13, a systematic review of gabapentin and pregabalin for chronic back pain, found at best limited evidence for benefit and consistent evidence of adverse events.22 Unless other studies find evidence of more benefit than harm for these drugs, they should not be prescribed for patients with low back pain.
Study 14 randomized 503 adults with ankle sprain to supervised physical therapy or usual care. It found that 65% of those receiving usual care had an excellent recovery at three months compared with 56% in the physical therapy group (P = .09).23 Finally, a previous Cochrane review concluded that corticosteroid injections provide modest benefit for patients with osteoarthritis of the knee.25 However, many of those studies were poorly controlled or compared injections with no treatment rather than placebo injections. Study 15 randomized 140 adults with knee osteoarthritis to regular triamcinolone, 40 mg, or saline injection every three months for two years. The authors found no benefit in pain or function and a worrisome reduction in cartilage thickness in the corticosteroid group when comparing magnetic resonance imaging studies performed before and after the study period.24
Screening
TABLE 5. Screening
| Clinical question | Bottom-line answer |
|---|---|
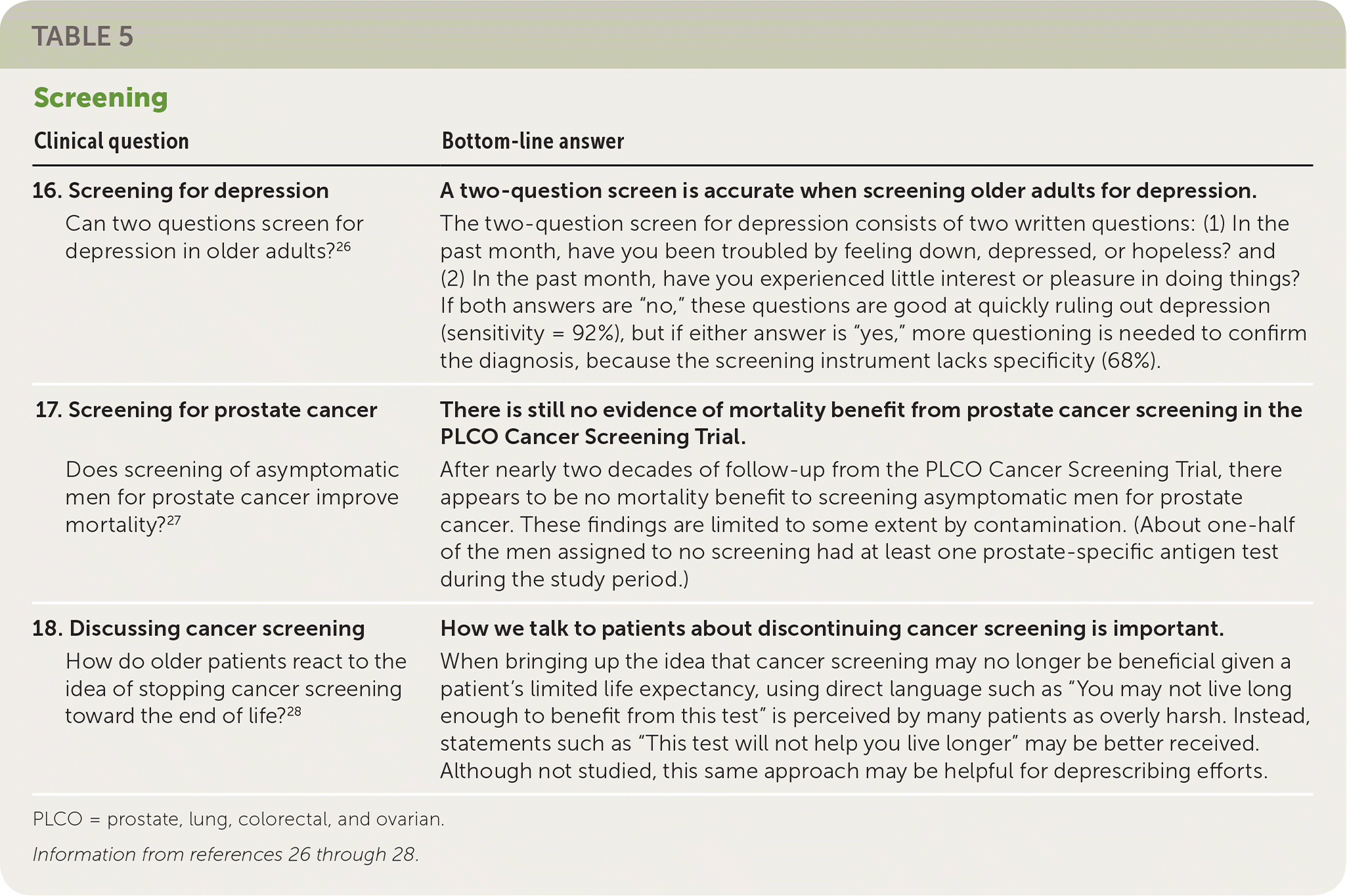
| 16. Screening for depression Can two questions screen for depression in older adults?26 | A two-question screen is accurate when screening older adults for depression. The two-question screen for depression consists of two written questions: (1) In the past month, have you been troubled by feeling down, depressed, or hopeless? and (2) In the past month, have you experienced little interest or pleasure in doing things? If both answers are “no,” these questions are good at quickly ruling out depression (sensitivity = 92%), but if either answer is “yes,” more questioning is needed to confirm the diagnosis, because the screening instrument lacks specificity (68%). |
| 17. Screening for prostate cancer Does screening of asymptomatic men for prostate cancer improve mortality?27 | There is still no evidence of mortality benefit from prostate cancer screening in the PLCO Cancer Screening Trial. After nearly two decades of follow-up from the PLCO Cancer Screening Trial, there appears to be no mortality benefit to screening asymptomatic men for prostate cancer. These findings are limited to some extent by contamination. (About one-half of the men assigned to no screening had at least one prostate-specific antigen test during the study period.) |
| 18. Discussing cancer screening How do older patients react to the idea of stopping cancer screening toward the end of life?28 | How we talk to patients about discontinuing cancer screening is important. When bringing up the idea that cancer screening may no longer be beneficial given a patient's limited life expectancy, using direct language such as “You may not live long enough to benefit from this test” is perceived by many patients as overly harsh. Instead, statements such as “This test will not help you live longer” may be better received. Although not studied, this same approach may be helpful for deprescribing efforts. |
PLCO = prostate, lung, colorectal, and ovarian.
Three POEMs address screening (Table 5).26–28 Study 16 is a meta-analysis that confirms that the widely used two-question screen for depression helps rule out depression in older adults; however, as in younger patients, one or more positive responses is not diagnostic for depression and requires further confirmation.26 Study 17 is long-term follow-up of the Prostate, Lung, Colorectal, and Ovarian Cancer Screening trial, and continues to find no mortality benefit for prostate cancer screening.27 Current guidelines from the American College of Physicians (ACP), the American Urological Association, and the U.S. Preventive Services Task Force recommend that screening should be considered only for men 55 (age 50 for ACP) to 69 years of age after a discussion of the potential benefits (which are small) and the potential harms (which are common). Finally, discussing the decision to discontinue cancer screening can be difficult for patients and physicians. Study 18, a qualitative study, found that saying “This test will not help you live longer,” rather than focusing on the patient's limited lifespan, is the preferred approach.28
Miscellaneous
TABLE 6. Miscellaneous
| Clinical question | Bottom-line answer |
|---|---|
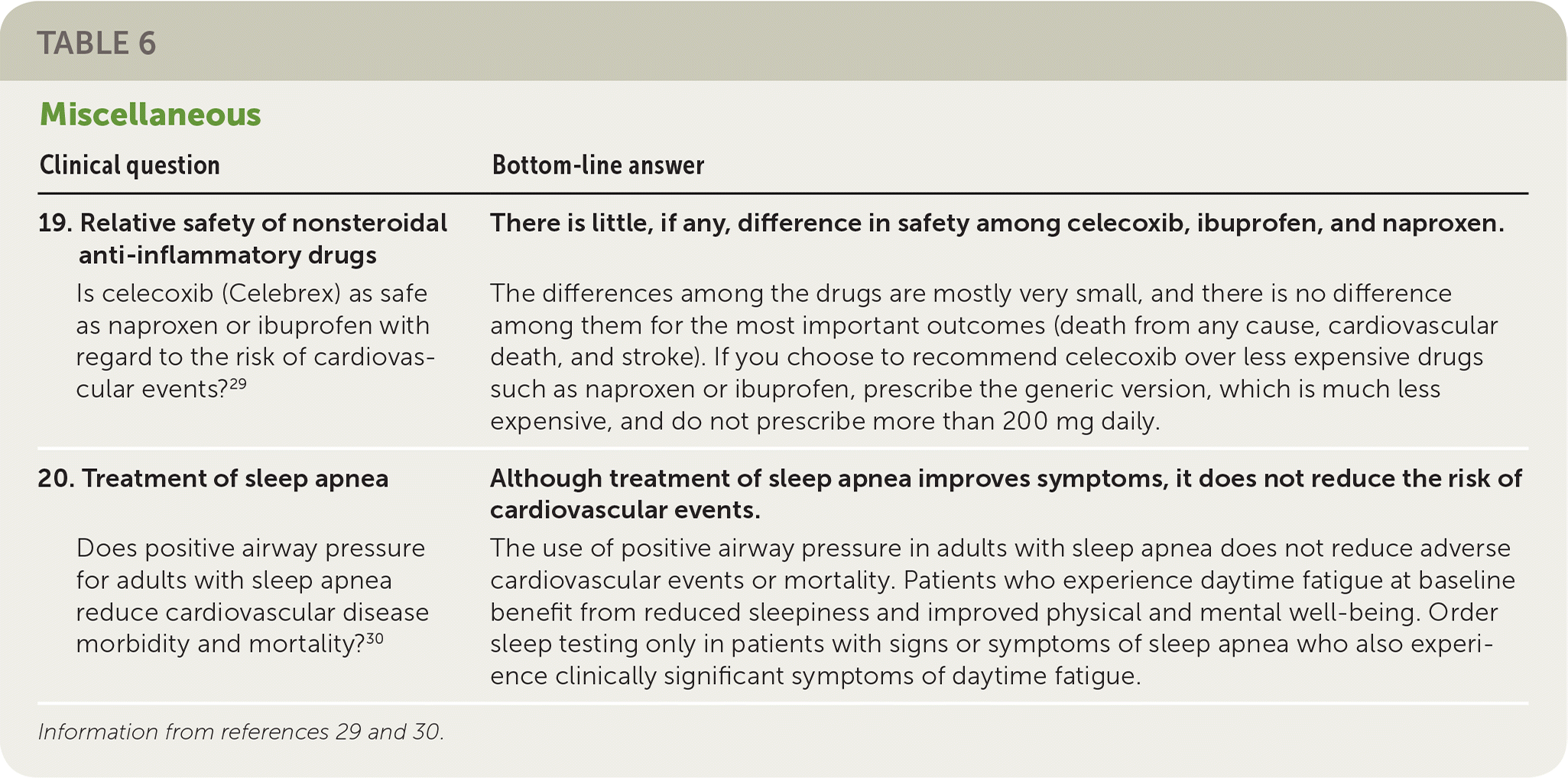
| 19. Relative safety of nonsteroidal anti-inflammatory drugs Is celecoxib (Celebrex) as safe as naproxen or ibuprofen with regard to the risk of cardiovascular events?29 | There is little, if any, difference in safety among celecoxib, ibuprofen, and naproxen. The differences among the drugs are mostly very small, and there is no difference among them for the most important outcomes (death from any cause, cardiovascular death, and stroke). If you choose to recommend celecoxib over less expensive drugs such as naproxen or ibuprofen, prescribe the generic version, which is much less expensive, and do not prescribe more than 200 mg daily. |
| 20. Treatment of sleep apnea Does positive airway pressure for adults with sleep apnea reduce cardiovascular disease morbidity and mortality?30 | Although treatment of sleep apnea improves symptoms, it does not reduce the risk of cardiovascular events. The use of positive airway pressure in adults with sleep apnea does not reduce adverse cardiovascular events or mortality. Patients who experience daytime fatigue at baseline benefit from reduced sleepiness and improved physical and mental well-being. Order sleep testing only in patients with signs or symptoms of sleep apnea who also experience clinically significant symptoms of daytime fatigue. |
Two studies are included as miscellaneous POEMs (Table 6).29,30 Study 19 compared ibuprofen, naproxen, and celecoxib (Celebrex) and found no difference in cardiovascular events and only very small differences in gastrointestinal or renal events (less than 0.5%) among the three drugs.29 The choice of drug should therefore be based on other factors, such as cost and patient preference, rather than the likelihood of adverse events. To round out the top 20 list, Study 20 is a systematic review of 10 randomized trials with 7,266 patients who had obstructive sleep apnea. There was no evidence that use of continuous positive airway pressure reduced the risk of cardiovascular events or death.30 The decision to recommend continuous positive airway pressure should be based only on tolerability and effect on symptoms.
Practice Guidelines
TABLE 7. Practice Guidelines

| Organization and topic | Key recommendations |
|---|---|
| ACP: Oral medications for type 2 diabetes mellitus31 | Patients with type 2 diabetes should begin with metformin, adding a second oral treatment (a sulfonylurea, a thiazolidinedione, a sodium glucose cotransporter-2 inhibitor, or a dipeptidyl peptidase-4 inhibitor) if needed for glycemic control. None of the drug classes for second-tier therapy is preferred, with the decision based on a consideration of patient preference, adverse effects, and cost. |
| ACP and AAFP: Drug therapy for patients 60 years and older with hypertension32 | Try to remember 60–150–140: in patients older than 60 years, consider treatment if the systolic blood pressure is 150 mm Hg or higher, or 140 mm Hg or higher in patients with a history of stroke or transient ischemic attack and in those at high cardiovascular risk. The guideline suggests initiating therapy only after a discussion of the benefits and risks with each patient; physicians should avoid making treatment decisions based just on the numbers. |
| ACP: Noninvasive treatment of acute, subacute, and chronic low back pain33 | These guidelines recommend starting with nondrug approaches to the treatment of acute low back pain and chronic low back pain, given the low evidence of benefit and the risks associated with medication. There is evidence of some benefit for a wide variety of nondrug approaches, which allows patients to choose the one that makes the most sense for them. |
| ACP: Management of gout34 | There is good evidence that acute gout should be treated with a corticosteroid, a nonsteroidal anti-inflammatory drug, or low-dose colchicine (1.2 mg, followed by 0.6 mg after one hour). Prophylaxis should not be initiated in most patients after a first gout attack or in patients with infrequent attacks. Patients should be informed of the benefits, harms, and costs to help them decide whether prophylaxis meets their needs. If preventive therapy is started, there is no need for 24-hour urine monitoring or ongoing uric acid monitoring; just use standard doses of allopurinol or febuxostat (Uloric). |
| USPSTF: Statins for the primary prevention of cardiovascular events35 | Adults without a history of CVD should use a low- to moderate-dose statin for the primary prevention of CVD events when the patient meets all three of the following criteria: (1) age 40 to 75 years, (2) at least one CVD risk factor (i.e., dyslipidemia, diabetes, hypertension, or smoking), and (3) a calculated 10-year risk of a CVD event of 10% or greater. Adults 40 to 70 years of age with at least one CVD risk factor and a 10-year CVD event risk of 7.5% to 10% may also consider using a statin for primary prevention, although the likelihood of benefit is smaller. Finally, the USPSTF concluded that current evidence is insufficient to assess whether to initiate statin therapy for prevention of CVD events in adults 76 years or older, although one of the studies cited above found that statins are not helpful in this group and might be harmful.14 |
AAFP = American Academy of Family Physicians; ACP = American College of Physicians; CVD = cardiovascular disease; USPSTF = U.S. Preventive Services Task Force.
Although most POEMs address individual research studies or systematic reviews, important practice guidelines are often summarized. The five guidelines that were rated most highly by CMA readers for relevance to practice are listed in Table 7 with their key recommendations.14,31–35 All of these guidelines have been fully endorsed by the American Academy of Family Physicians (AAFP). They are also available on the AAFP's Clinical Practice Guidelines website at https://www.aafp.org/patient-care/browse/type.tag-clinical-practice-guidelines.html.
The authors thank Wiley-Blackwell, Inc., for giving permission to excerpt the POEMs; Drs. Allen Shaughnessy, Henry Barry, David Slawson, Nita Kulkarni, and Linda Speer for their work in selecting and writing the original POEMs; the academic family medicine fellows and faculty of the University of Missouri–Columbia for their work as peer reviewers; Pierre Pluye, PhD, for his work in codeveloping the Information Assessment Method; and Maria Vlasak for her assistance with copyediting the POEMs for the past 24 years.
A list of top POEMs from previous years is available at https://www.aafp.org/journals/afp/authors/ebm-toolkit/resources/top-poems.html.
Editor's Note: This article was cowritten by Dr. Mark Ebell, who was a member of the U.S. Preventive Services Task Force (USPSTF) from 2012 to 2015 and currently serves as a consultant to the USPSTF. This article does not necessarily represent the views and policies of the USPSTF. Dr. Ebell is deputy editor for evidence-based medicine for American Family Physician (AFP) and cofounder and editor-in-chief of Essential Evidence Plus, published by Wiley-Blackwell, Inc. Because of Dr. Ebell's dual roles and ties to Essential Evidence Plus, the concept for this article was independently reviewed and approved by a group of AFP's medical editors. In addition, the article underwent peer review and editing by three of AFP's medical editors. Dr. Ebell was not involved in the editorial decision-making process.—Sumi Sexton, MD, Editor-in-Chief, American Family Physician

