Am Fam Physician. 2018;98(10):online
See related Putting Prevention into Practice: Screening for Osteoporosis to Prevent Fractures.
As published by the U.S. Preventive Services Task Force.
Summary of Recommendations and Evidence
The USPSTF recommends screening for osteoporosis with bone measurement testing to prevent osteoporotic fractures in women 65 years and older (Table 1). B recommendation.
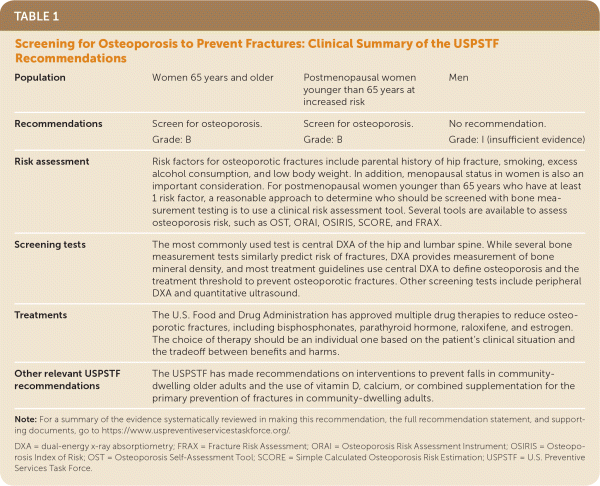
| Population | Women 65 years and older | Postmenopausal women younger than 65 years at increased risk | Men |
| Recommendations | Screen for osteoporosis. Grade: B | Screen for osteoporosis. Grade: B | No recommendation. Grade: I (insufficient evidence) |
| Risk assessment | Risk factors for osteoporotic fractures include parental history of hip fracture, smoking, excess alcohol consumption, and low body weight. In addition, menopausal status in women is also an important consideration. For postmenopausal women younger than 65 years who have at least 1 risk factor, a reasonable approach to determine who should be screened with bone measurement testing is to use a clinical risk assessment tool. Several tools are available to assess osteoporosis risk, such as OST, ORAI, OSIRIS, SCORE, and FRAX. | ||
| Screening tests | The most commonly used test is central DXA of the hip and lumbar spine. While several bone measurement tests similarly predict risk of fractures, DXA provides measurement of bone mineral density, and most treatment guidelines use central DXA to define osteoporosis and the treatment threshold to prevent osteoporotic fractures. Other screening tests include peripheral DXA and quantitative ultrasound. | ||
| Treatments | The U.S. Food and Drug Administration has approved multiple drug therapies to reduce osteoporotic fractures, including bisphosphonates, parathyroid hormone, raloxifene, and estrogen. The choice of therapy should be an individual one based on the patient's clinical situation and the trade-off between benefits and harms. | ||
| Other relevant USPSTF recommendations | The USPSTF has made recommendations on interventions to prevent falls in community-dwelling older adults and the use of vitamin D, calcium, or combined supplementation for the primary prevention of fractures in community-dwelling adults. | ||
The USPSTF recommends screening for osteoporosis with bone measurement testing to prevent osteoporotic fractures in postmenopausal women younger than 65 years who are at increased risk of osteoporosis, as determined by a formal clinical risk assessment tool. B recommendation.
See the Clinical Considerations section for information on risk assessment.
The USPSTF concludes that the current evidence is insufficient to assess the balance of benefits and harms of screening for osteoporosis to prevent osteoporotic fractures in men. I statement.
See the Clinical Considerations section for suggestions for practice regarding the I statement.
Rationale
IMPORTANCE
By 2020, approximately 12.3 million individuals in the United States older than 50 years are expected to have osteoporosis.1 Osteoporotic fractures, particularly hip fractures, are associated with limitation of ambulation, chronic pain and disability, loss of independence, and decreased quality of life, and 21% to 30% of patients who experience a hip fracture die within 1 year.2 Seventy-one percent of osteoporotic fractures occur among women,3 and women have higher rates of osteoporosis than men at any given age; however, men have a higher fracture-related mortality rate than women.2,4 The prevalence of primary osteoporosis (i.e., osteoporosis without underlying disease) increases with age and differs by race/ethnicity. With the aging of the U.S. population, the potential preventable burden is likely to increase in future years.1
DETECTION
The USPSTF found convincing evidence that bone measurement tests are accurate for predicting osteoporotic fractures in women and men. The most commonly used test is central dual-energy x-ray absorptiometry (DXA) of the hip and lumbar spine. Although several bone measurement tests similarly predict risk of fracture, DXA provides measurement of bone mineral density (BMD), and most treatment guidelines use central DXA to define osteoporosis and the threshold at which to start drug therapies to prevent osteoporotic fractures. The USPSTF found adequate evidence that clinical risk assessment tools are moderately accurate in identifying risk of osteoporosis and osteoporotic fractures.
BENEFITS OF EARLY DETECTION AND TREATMENT
Multiple studies show that drug therapies reduce fractures in postmenopausal women with osteoporosis. For women 65 years and older, the USPSTF found convincing evidence that screening can detect osteoporosis and that treatment of women with osteoporosis can provide at least a moderate benefit in preventing fractures. For postmenopausal women younger than 65 years who are at increased risk of osteoporosis, the USPSTF found adequate evidence that screening can detect osteoporosis and that treatment provides a moderate benefit in preventing fractures.
For men, the USPSTF found inadequate evidence on the benefits and harms of treating screen-detected osteoporosis to reduce the risk of osteoporotic fractures.
HARMS OF EARLY DETECTION AND TREATMENT
The USPSTF found a single study that described harms of screening for osteoporosis. It reported no increase in anxiety and no decrease in quality of life from screening.4–6 Based on the nature of screening with bone measurement tests and the low likelihood of serious harms, the USPSTF found adequate evidence to bound these harms as no greater than small. Harms associated with screening may include radiation exposure from DXA and opportunity costs (time and effort required by patients and the health care system).
Harms of drug therapies for osteoporosis depend on the specific medication used. The USPSTF found that the risk of serious adverse events, upper gastrointestinal events, or cardiovascular events associated with the most common class of osteoporosis medication (bisphosphonates) is no greater than small. Overall, the USPSTF found adequate evidence that the harms of osteoporosis medications are small.
USPSTF ASSESSMENT
The USPSTF concludes with moderate certainty that the net benefit of screening for osteoporosis in women 65 years and older is at least moderate.
The USPSTF concludes with moderate certainty that the net benefit of screening for osteoporosis in postmenopausal women younger than 65 years who are at increased risk of osteoporosis is at least moderate.
The USPSTF concludes that the current evidence is insufficient to assess the balance of benefits and harms of screening for osteoporosis in men.
Clinical Considerations
PATIENT POPULATION UNDER CONSIDERATION
This recommendation applies to older adults without a history of low-trauma fractures and without conditions that may cause secondary osteoporosis (such as metabolic bone disease or untreated hyperthyroidism) and patients without conditions that may increase their risk of falls. This recommendation does not apply to persons who take long-term medications that may cause secondary osteoporosis (e.g., glucocorticoids, aromatase inhibitors, or gonadotropin-releasing hormone agonists).
ASSESSMENT OF RISK
In deciding which postmenopausal women younger than 65 years to screen with bone measurement testing, clinicians should first consider factors associated with increased risk of osteoporotic fractures. These include parental history of hip fracture, smoking, excessive alcohol consumption, and low body weight. In addition, menopausal status in women is also an important consideration because studies demonstrating treatment benefit mainly enrolled postmenopausal women. For postmenopausal women younger than 65 years who have at least 1 risk factor, a reasonable approach to determine who should be screened with bone measurement testing is to use a clinical risk assessment tool.
Several tools are available to assess osteoporosis risk: the Simple Calculated Osteoporosis Risk Estimation (SCORE; Merck), Osteoporosis Risk Assessment Instrument (ORAI), Osteoporosis Index of Risk (OSIRIS), and the Osteoporosis Self-Assessment Tool (OST). These tools seem to perform similarly and are moderately accurate at predicting osteoporosis. The Fracture Risk Assessment (FRAX) tool (University of Sheffield), which assesses a person's 10-year risk of fracture, is also a commonly used tool. The FRAX tool includes questions about previous DXA results but does not require this information to estimate fracture risk. Because the benefits of treatment are greater in persons at higher risk of fracture, one approach is to perform bone measurement testing in postmenopausal women younger than 65 years who have a 10-year FRAX risk of major osteoporotic fracture (MOF) (without DXA) greater than that of a 65-year-old white woman without major risk factors. For example, in the United States, a 65-year-old white woman of mean height and weight7 without major risk factors has a 10-year FRAX risk of MOF of 8.4%.4,8 In comparison, a 60-year-old white woman of mean height and weight7 with a parental history of hip fracture has a 10-year FRAX risk of MOF of 13%.4,8
Clinicians should note that the presence of a given risk factor or a certain age does not represent a particular risk threshold. Although the risk of osteoporosis and osteoporotic fractures generally increases with age, the presence of multiple risk factors at a younger age may indicate that the risk-benefit profile is favorable for screening with bone measurement testing.
SCREENING TESTS
The most commonly used bone measurement test used to screen for osteoporosis is central DXA; other screening tests include peripheral DXA and quantitative ultrasound (QUS). Central DXA measures BMD at the hip and lumbar spine. Most treatment guidelines3,4,9–11 recommend using BMD, as measured by central DXA, to define osteoporosis and the treatment threshold to prevent osteoporotic fractures.4,12 All the osteoporosis drug therapy studies reviewed by the USPSTF used central DXA to determine eligibility for study enrollment.4,6 Peripheral DXA measures BMD at the lower forearm and heel. QUS also evaluates peripheral sites and has similar accuracy in predicting fracture risk as DXA, while avoiding the risk of radiation exposure; however, it does not measure BMD. Peripheral DXA and QUS are measured with portable devices and may be less costly and more accessible than central DXA measurement (Table 2).
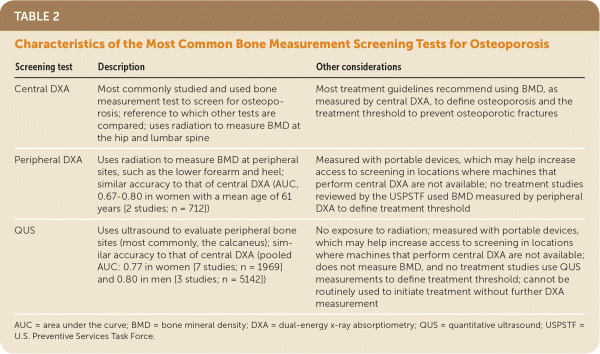
| Screening test | Description | Other considerations |
|---|---|---|
| Central DXA | Most commonly studied and used bone measurement test to screen for osteoporosis; reference to which other tests are compared; uses radiation to measure BMD at the hip and lumbar spine | Most treatment guidelines recommend using BMD, as measured by central DXA, to define osteoporosis and the treatment threshold to prevent osteoporotic fractures |
| Peripheral DXA | Uses radiation to measure BMD at peripheral sites, such as the lower forearm and heel; similar accuracy to that of central DXA (AUC, 0.67–0.80 in women with a mean age of 61 years [2 studies; n = 712]) | Measured with portable devices, which may help increase access to screening in locations where machines that perform central DXA are not available; no treatment studies reviewed by the USPSTF used BMD measured by peripheral DXA to define treatment threshold |
| QUS | Uses ultrasound to evaluate peripheral bone sites (most commonly, the calcaneus); similar accuracy to that of central DXA (pooled AUC: 0.77 in women [7 studies; n = 1969] and 0.80 in men [3 studies; n = 5142]) | No exposure to radiation; measured with portable devices, which may help increase access to screening in locations where machines that perform central DXA are not available; does not measure BMD, and no treatment studies use QUS measurements to define treatment threshold; cannot be routinely used to initiate treatment without further DXA measurement |
SCREENING INTERVALS
Some observational and modeling studies have suggested screening intervals based on age, baseline BMD, and calculated projected time to transition to osteoporosis. However, limited evidence from 2 good-quality studies found no benefit in predicting fractures from repeating bone measurement testing 4 to 8 years after initial screening.4
TREATMENT
The U.S. Food and Drug Administration has approved multiple drug therapies to reduce osteoporotic fractures, including bisphosphonates, parathyroid hormone, raloxifene, and estrogen. The choice of therapy should be an individual one based on the patient's clinical situation and the trade-off between benefits and harms. Clinicians should educate patients on how to minimize the adverse effects of drug therapies, such as reducing esophageal irritation from bisphosphonate therapy by taking the medication with a full glass of water and not lying down for at least 30 minutes afterward.
SUGGESTIONS FOR PRACTICE REGARDING THE I STATEMENT
When deciding whether to screen for osteoporosis to prevent osteoporotic fractures in men, clinicians should consider the following factors.
POTENTIAL PREVENTABLE BURDEN
The prevalence of osteoporosis in men is generally lower than in women (4.3% vs. 15.4%, respectively).1 An estimated 1 to 2 million men in the United States have osteoporosis.5 Although men account for 29% of osteoporotic fractures in the United States, men have higher fracture-related morbidity and mortality rates than women.3,4 Each year, about 80,000 men in the United States will have a hip fracture; 1 in 3 men who experience a hip fracture will die within a year.13
Older age in men is an important risk factor for osteoporotic fracture. In the absence of other risk factors, it is not until age 80 years that the prevalence of osteoporosis in white men starts to reach that of white women at age 65 years.1 For example, in the United States, the 10-year FRAX risk of MOF is 5.0%8 in a 65-year-old white man of mean height and weight7 without any risk factors and 8.4%8 at age 80 years (vs. 8.4% in a 65-year-old white woman of mean height and weight7 without any risk factors8). In the presence of multiple risk factors, the 10-year FRAX risk of MOF in a 55-year-old white man can approximate the risk of a 65-year-old white woman with no risk factors; for example, the 10-year FRAX risk of MOF is 8.9% in a 55-year-old white man of mean height and weight7 with a parental history of hip fracture who currently smokes and drinks 3 or more units of alcohol per day.8
Similar to women, risk factors for fractures in men include low body mass index, excessive alcohol consumption, current smoking, long-term corticosteroid use, previous fractures, and history of falls within the past year. A recent systematic review of risk factors for osteoporosis in men also found that hypogonadism, history of cerebrovascular accident, and history of diabetes are associated with an increased risk of fractures, although their clinical use in identifying men who need further bone measurement testing is unclear.4,14
Although clinical risk assessment tools and imaging tests to diagnose osteoporosis seem to perform as well in men as in women, evidence on the effectiveness of medications to treat osteoporosis in men is lacking.4,6 Although some treatments have been found to be effective in preventing fractures in postmenopausal women with osteoporosis, it cannot be assumed that they will be equally effective in men because the underlying biology of bones may differ in men due to differences in testosterone and estrogen levels. The review identified limited evidence on the effect of treatment of men with osteoporosis on the prevention of fractures.4,6 One good-quality study found a reduction in morphometric vertebral fractures but not clinical (vertebral and nonvertebral) fractures in men with osteoporosis who were treated with zoledronic acid.15 A small study examining treatment with parathyroid hormone in men was consistent in the direction of benefit but the finding was not statistically significant.16
POTENTIAL HARMS OF SCREENING
CURRENT PRACTICE
Data on how frequently men are screened for osteoporosis are limited. Several organizations have issued statements on screening in men at increased risk. Progress toward the Healthy People 2020 objectives for osteoporosis have shown little change in the number of hip fracture hospitalizations among men (464.9 vs. 442.6 hospitalizations per 100,000 men in 2000 and 2010, respectively).17
ADDITIONAL APPROACHES TO PREVENTION
According to the Centers for Disease Control and Prevention, engaging in 120 to 300 minutes of at least moderate-intensity aerobic activity each week can reduce the risk of hip fractures, and performing balance and muscle-strengthening activities each week along with moderate-intensity aerobic activity can help prevent falls in older adults.18 The National Academy of Medicine (formerly the Institute of Medicine) has issued dietary reference intakes for calcium and vitamin D to support health; recommended daily allowances are based on age.19
USEFUL RESOURCES FOR PRIMARY CARE
The USPSTF recommends exercise interventions to prevent falls in community-dwelling adults 65 years and older at increased risk of falls and selectively offering multifactorial interventions based on circumstances of prior falls, presence of comorbid medical conditions, and the patient's values and preferences; it recommends against vitamin D supplementation to prevent falls.20 In a separate recommendation, the USPSTF recommends against supplementation with 400 IU or less of vitamin D and 1000 mg or less of calcium in postmenopausal women to prevent fractures.21 The USPSTF found insufficient evidence on supplementation with higher doses of vitamin D and calcium, alone or combined, to prevent fractures in postmenopausal women, or at any dose in men and premenopausal women.21
This summary is one in a series excerpted from the Recommendation Statements released by the USPSTF. These statements address preventive health services for use in primary care clinical settings, including screening tests, counseling, and preventive medications.
The complete version of this statement, including supporting scientific evidence, evidence tables, grading system, members of the USPSTF at the time this recommendation was finalized, and references, is available on the USPSTF website at https://www.uspreventiveservicestaskforce.org/.