Case Scenario
A 65-year-old woman presented on the second day of my week-long volunteer medical brigade to a migrant camp in Mexico. The patient had a blood pressure of 180/110 mm Hg and a heart rate of 78 beats per minute. Her presenting symptoms were itchy eyes and sneezing, which she reported were worse when she worked outside harvesting produce. She was otherwise asymptomatic.
I was primarily concerned about her blood pressure (she seemed unaware that it was elevated); however, the only antihypertensive available in our brigade was lisinopril. I did not want to prescribe it without checking the patient's renal function, but the clinic did not have a laboratory. I would not be in the area long enough to follow up with my patient. The nearest local clinic was more than an hour away, and the patient did not have transportation. Should I have prescribed the medication? How do volunteer physicians on short-term medical trips (STMTs) best manage for local health care needs?
Commentary
This case identifies several common problems that can arise from participation in STMTs. Global health has gained popularity in North America as a means of providing learning experiences during medical school and enabling practicing physicians to volunteer in low- and middle-income countries. Approximately 26% of undergraduate students1 and more than 40% of graduate medical students2 have reported participating in STMTs during their training, and approximately 30% of U.S. physicians have engaged in similar trips, many more than once.3,4 STMTs generally range in duration from one day to two months5 and involve travel to a location outside the learner's or physician's home country. Pretravel preparation varies for each trip; volunteers may focus on one location or may move between several communities, and they often spend full days seeing hundreds of patients. Despite the volunteers' goodwill, these trips may introduce risks to the patients, including diagnostic mistakes, cultural miscommunication, and unreliable treatment, principally through not ensuring adequate continuity of care for the patients.6–9 As a result, some within the medical community have challenged the value of such trips for the patients who are meant to be served.7–11 To address these concerns, several groups have developed STMT guidelines.6,7,10 With proper preparation and engagement in the local community, STMT participants can provide meaningful patient care. Based on these guidelines, the following principles should be considered for conscientious involvement in STMTs (Table 16,7,10,12–14 ).
TABLE 1. Practical Approaches to Address Potential Pitfalls of Short-Term Medical Trips
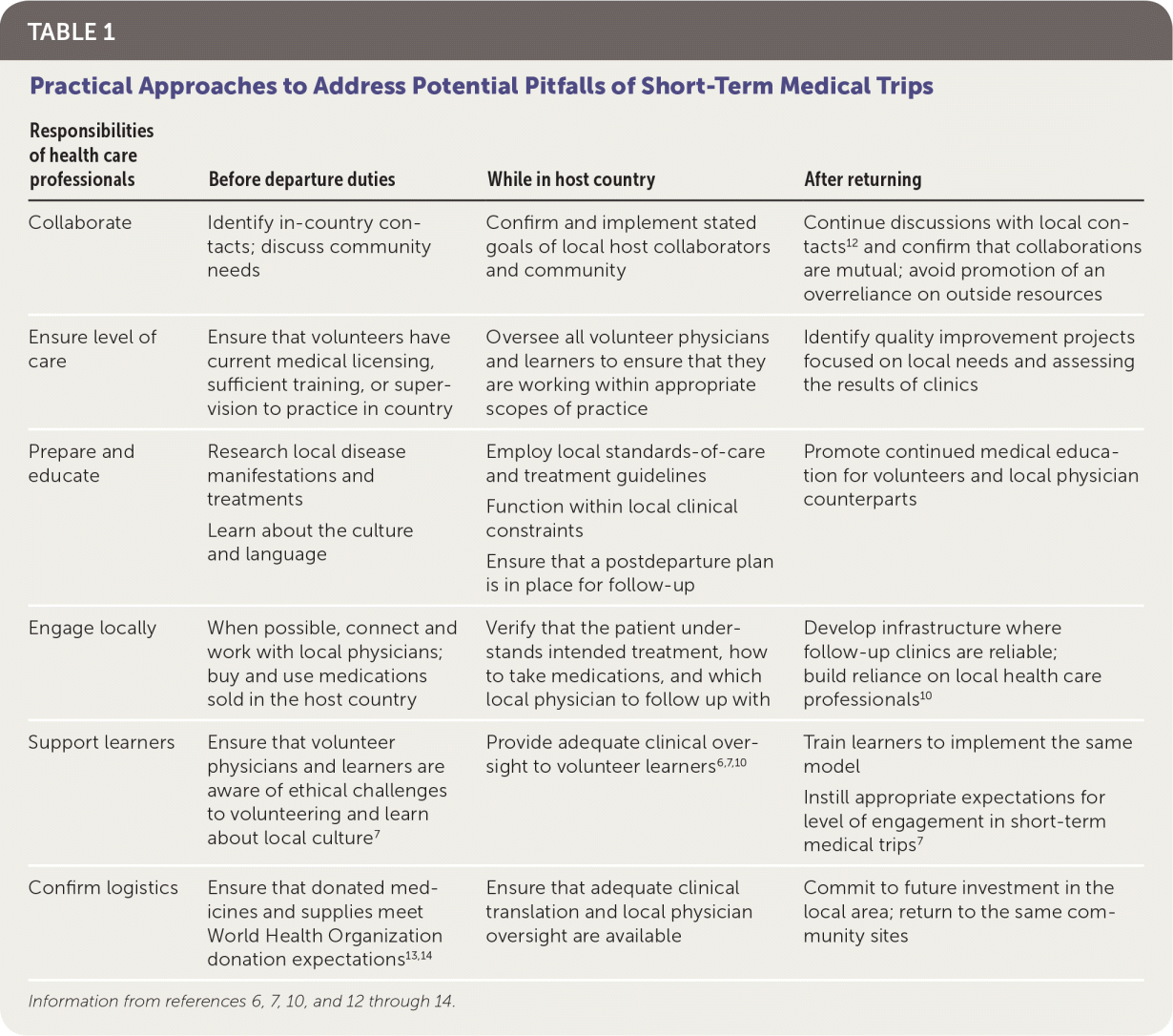
| Responsibilities of health care professionals | Before departure duties | While in host country | After returning |
|---|---|---|---|
| Collaborate | Identify in-country contacts; discuss community needs | Confirm and implement stated goals of local host collaborators and community | Continue discussions with local contacts12 and confirm that collaborations are mutual; avoid promotion of an overreliance on outside resources |
| Ensure level of care | Ensure that volunteers have current medical licensing, sufficient training, or supervision to practice in country | Oversee all volunteer physicians and learners to ensure that they are working within appropriate scopes of practice | Identify quality improvement projects focused on local needs and assessing the results of clinics |
| Prepare and educate | Research local disease manifestations and treatments Learn about the culture and language | Employ local standards-of-care and treatment guidelines Function within local clinical constraints Ensure that a postdeparture plan is in place for follow-up | Promote continued medical education for volunteers and local physician counterparts |
| Engage locally | When possible, connect and work with local physicians; buy and use medications sold in the host country | Verify that the patient understands intended treatment, how to take medications, and which local physician to follow up with | Develop infrastructure where follow-up clinics are reliable; build reliance on local health care professionals10 |
| Support learners | Ensure that volunteer physicians and learners are aware of ethical challenges to volunteering and learn about local culture7 | Provide adequate clinical oversight to volunteer learners6,7,10 | Train learners to implement the same model Instill appropriate expectations for level of engagement in short-term medical trips7 |
| Confirm logistics | Ensure that donated medicines and supplies meet World Health Organization donation expectations13,14 | Ensure that adequate clinical translation and local physician oversight are available | Commit to future investment in the local area; return to the same community sites |
Primarily, STMT leaders and volunteer physicians and learners must engage the local leaders and physicians currently practicing in the area, elicit locally identified goals for volunteer work, and then focus efforts to accomplish those objectives. These collaborations can result in volunteers providing meaningful assistance to the local health care system rather than simply providing health care while on the trip. After these goals are established, STMT leaders should focus on relationships with local contacts and support existing health care efforts. These collaborations should be reassessed frequently, ensuring continued benefit to the host community.10
When providing STMT clinical care, physician use of health care resources and treatment guidelines from the World Health Organization (WHO; http://www.who.int/publications/guidelines/en/) or local Ministry of Health organizations (see individual websites for specific countries) is advised to inform appropriate decision making on available diagnostics and treatments. When possible, the STMT organization should purchase and dispense medications available in the host country after verifying which medications are locally accessible and inexpensive.13,15 If donated medicines are used, WHO guidelines should be followed to provide nonexpired, standard-issue medications to patients.13,14
NONCOMMUNICABLE AND CHRONIC DISEASE MANAGEMENT
Per WHO, chronic disease is a major source of universal mortality and morbidity, contributing to nearly one-half of the global burden of disease around the world, with a substantial portion of the mortality occurring in developing countries.16 As a result, many patients encountered during STMTs will need chronic disease management (such as the patient in this case scenario). What steps can volunteers take to guarantee that treating chronic diseases will result in helping rather than harming the patient?
Principally, STMT volunteers must assure continuity of care for patients with chronic diseases by partnering with local physicians and existing health care systems.8,17 STMT protocols should require a postdeparture plan to arrange patient access to necessary referrals, transportation, laboratory work, medication refills, and follow-up visits. By connecting patients with the local health care community for further care, continuity is maintained.8,10 When no local physician is available, the establishment of regular STMT visits to the same clinic sites may fill a gap in the health care system and help maintain reliable follow-up while local infrastructure develops.8,10 In this way, treating chronic disease abroad can be practical, safe, and potentially sustainable.
COMMUNICABLE AND ACUTE DISEASE MANAGEMENT
For physicians and learners participating in short-term work in low- and middle-income countries, the ultimate target should be promoting sustainable interventions that benefit local patients and communities by prioritizing prevention and self-engagement in disease management.8,10 For example, rather than simply prescribing antibiotics for patients with acute diarrhea, the focus should be on education for that community: personal hygiene, water hygiene, nutrition, or diarrheal disease education. To achieve this, STMT volunteers must understand their patients in the context of the local environment, culture, and infectious disease prevalence. Such insight requires preparation, including understanding the community health needs and learning about the endemic communicable diseases, their clinical presentations, and region-appropriate treatments. Treating acute illness in this way—by employing focused, location-specific care—contributes lasting benefits to patients in low- and middle-income countries.
SURGERY
Many different surgical procedures, from laceration closures to cleft palate repairs, are commonly performed during STMTs, but the procedures carry risks, including improper consent for or understanding of the procedure, postoperative infections or complications, and lack of proper follow-up.11,15,18 Such risks can be mitigated by determining whether the surgery improves their patients' quality of life.4,18 It is best if local surgeons or general physicians with surgical skills make this assessment via presurgical counseling with patients.14,18 The patients must understand the proposed procedure and actively consent via adequate translational services, which, when not available, preclude surgical intervention.18 Volunteer physicians must demonstrate prior training in the procedures they will perform.7 Ultimately, in-country surgical physicians should, if possible, oversee all procedures performed during STMTs and then follow up with the patients.12,18,19
CASE RESOLUTION
For the patient in the case scenario, the volunteer physician should identify a local health care professional who is able to obtain baseline laboratory work and continue follow-up visits for the patient. By using guidelines established when working with the local health care community, transportation can be arranged for her to accomplish the visits. This will allow the STMT physician to prescribe the lisinopril and to confirm that the patient can receive refills of this medication.
Editor's Note: Dr. McCurry is currently at the University of Pittsburgh Medical Center, McKeesport Family Medicine Residency and the Global Health Track, McKeesport, Pennsylvania.

