A 30-year-old woman reported that her chronic eczema had worsened over the previous several months. She had used emollient creams and topical and oral steroids in the past. Although the rash improved with steroids, it recurred when the treatment stopped. The patient was otherwise healthy.
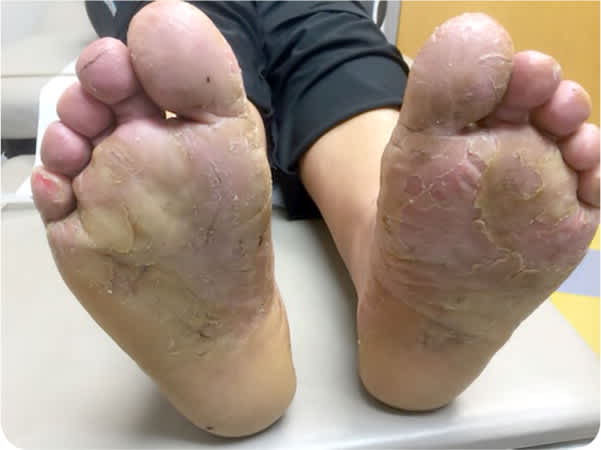
Physical examination revealed a pruritic rash with peeling and cracking on the palmar and plantar surfaces of her hands and feet (Figure 1 and Figure 2). The underlying skin was erythematous. No other areas of her body were affected. She had no occupational exposures or contact with irritants, chemicals, or livestock.
FIGURE 1
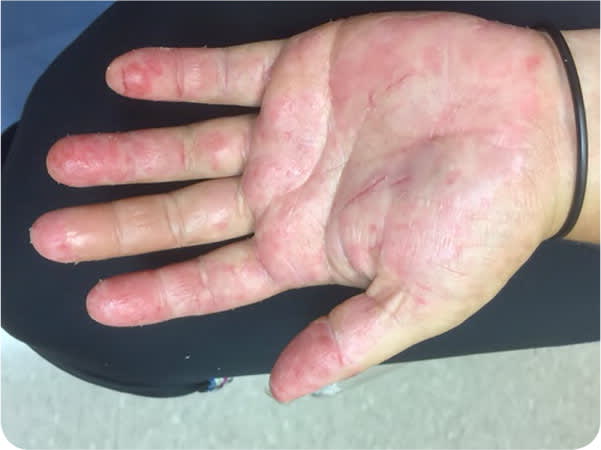
FIGURE 2
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Allergic contact dermatitis.
B. Atopic hand dermatitis.
C. Dyshidrotic eczema.
D. Pemphigus vulgaris.
Discussion
The answer is C: dyshidrotic eczema. This very pruritic condition (also called dyshidrotic dermatitis and pompholyx) is limited to the palms and soles.1,2 It presents as vesicles or larger bullae on the sides of the palms and soles.1 The lesions tend to persist for several weeks and resolve with desquamation. Recurrence is possible. The etiology is probably multifactorial, with some evidence pointing to atopic dermatitis, exposure to contact allergens, systemic exposure to contact allergens (e.g., ingestion of nickel or cobalt), dermatophyte infection, intravenous immune globulin, and hyperhidrosis.3 The diagnosis is based on the history and clinical appearance of the lesions. Patch testing, rapid plasma reagin testing, and potassium hydroxide preparation may be considered for initial workup.
Management of dyshidrotic eczema includes avoiding exposure to known irritants. Mild to moderate cases can be treated with two to four weeks of topical corticosteroids, whereas more severe cases may require an oral steroid taper. Topical immunomodulators, such as tacrolimus (Protopic), and phototherapy are options for refractory cases.1
Allergic contact dermatitis is a delayed hypersensitivity reaction characterized by the appearance of skin lesions in areas exposed to specific allergens. Acute lesions are typically erythematous, pruritic plaques. Chronic lesions demonstrate lichenification over exposed areas of skin.4 Vesiculation may occur in severe cases. Although involvement of extremities, eyelids, lips, and other exposed areas is typical of allergic contact dermatitis, patch testing may be needed to confirm the diagnosis.
Atopic hand dermatitis commonly occurs in children and is characterized by dry skin with severe pruritus and hypersensitivity to multiple stimuli. The lesions typically occur on skin creases and sometimes the dorsal aspect of extremities.5 Patients with atopic hand dermatitis often have a personal or family history of asthma or hay fever.
Pemphigus vulgaris is an autoimmune disorder that primarily affects middle-aged adults. It is characterized by painful mucosal or cutaneous blisters that most commonly occur in the oral cavity, but other mucosal surfaces may be involved. The palms and soles are spared.6 The blisters rupture easily, leading to painful erosions. The Nikolsky sign (mechanical pressure on normal skin elicits blistering) is often positive.6
SUMMARY TABLE

| Condition | Characteristics |
|---|---|
| Allergic contact dermatitis | Skin lesions in areas exposed to an allergen; acute lesions are erythematous, pruritic plaques; chronic lesions demonstrate lichenification over exposed areas of skin; extremities, eyelids, and lips are typically involved |
| Atopic hand dermatitis | Dry skin with severe pruritus and hypersensitivity to multiple stimuli; erythematous papules and lichenification occur on skin creases and sometimes the dorsal aspect of extremities |
| Dyshidrotic eczema | Very pruritic vesicles or larger bullae on the sides of the palms and soles; lesions persist for several weeks and resolve with desquamation |
| Pemphigus vulgaris | Painful mucosal and cutaneous blisters that easily erode; Nikolsky sign is positive |

