Underuse and overuse of medical interventions, failure to use interventions known to be effective, and provision of tests or interventions in which benefits do not exceed harms are types of low-value care. The Lown Institute's Right Care Alliance Children's Health Council identified five “do” recommendations that highlight underuse and five “don't” recommendations that highlight overuse in children's health care. The five “do” recommendations include: do provide access to long-acting reversible contraception for adolescents, do use nonpharmacologic interventions first for treatment of attention-deficit/hyperactivity disorder, do discuss quality of life for children with complex medical conditions using a shared decision-making model and access resources such as palliative care subspecialists, do promote childhood literacy development by providing free, age-appropriate books in clinical settings, and do screen for socioeconomic status of the patient and family and provide access to community health and wellness resources. The five “don't” recommendations include: don't routinely prescribe antibiotics in children two to 12 years of age with a middle ear infection, don't perform computed tomography of the head for children with minor head trauma, don't use albuterol in children with bronchiolitis, don't routinely screen for hyperlipidemia in children and adolescents, and don't routinely perform preparticipation sports evaluations. These 10 examples of underuse and overuse were identified with the intent of improving health care value and promoting “Right Care.”
Underuse and overuse of medical interventions, failure to use interventions known to be effective, and provision of tests or interventions in which benefits do not exceed harms are all types of low-value care.1,2 American Family Physician has addressed overuse in health care in previous discussions of the Choosing Wisely campaign that highlights overuse in an effort to reduce non-beneficial care.3 In this article, the authors discuss recommendations for underuse and overuse from members of the Lown Institute.
The Lown Institute was founded in response to the epidemic of health care underuse and overuse4 and subsequently created the Right Care Alliance, a network of clinicians, patients, and community leaders focused on care that benefits patients. In 2016, the Lown Institute challenged each of its Right Care Alliance councils to develop a list of 10 evidence-based recommendations highlighting opportunities to improve health care value, including five examples of underuse and five examples of overuse.
A subcommittee of the Right Care Alliance Children's Health Council formed a modified Delphi panel, which is a validated method for generating an expert consensus with minimal peer bias through several rounds of anonymous voting, and developed a list of the top 10 do's and don'ts for children's health care based on criteria listed in Table 1. A flowchart depicting the elements involved in the list creation is presented in eFigure A. The initial lists of 31 items are provided in eTable A and eTable B, and the final 10 recommendations are listed in Table 2.5–43
TABLE 1 Criteria for Selection and Development of Right Care Recommendations

| Each recommendation should: |
|---|
| 1. Matter to patients. |
| 2. Be an egregious infraction of good care if not followed. |
| 3. Have high potential to benefit or harm. |
| 4. Be rare (underuse) or common (overuse) enough that avoiding or performing the item routinely would move the needle toward the right care. |
| 5. Examine or illustrate how it ties to system failures. |
eFIGURE A

Flowchart of modified Delphi panel process from formation to completion of the final list of recommendations.
eTABLE A Initial List of Do Recommendations for Children and Adolescents

| Perform mental health screening using a validated tool. |
| Provide access to long-acting reversible contraception for adolescents. |
| Use nonpharmacologic interventions as first-line treatment of neonatal abstinence syndrome. |
| Use nonpharmacologic interventions as first-line treatment of attention-deficit/hyperactivity disorder. |
| Discuss quality of life for children with complex medical conditions. |
| Obtain an Adverse Childhood Experience score for children on a yearly basis. |
| Screen for socioeconomic status of patient and family. |
| Follow recommended Centers for Disease Control and Prevention vaccination schedule (https://www.cdc.gov/vaccines/parents/downloads/parent-ver-sch-0-6yrs.pdf). |
| Assess quality of life and health status of children with complex medical conditions. |
| Promote childhood literacy development through programs such as Reach Out and Read. |
| Evaluate nutrition, weight, height, and body mass index (head circumference for infants) during every visit (inpatient and outpatient). |
| Provide a discharge summary including a detailed medication plan and follow-up appointments to every child discharged from a hospital. |
| Screen for mental health well-being at every child visit (inpatient and outpatient). |
| Adhere to the Centers for Disease Control and Prevention immunization schedule as recommended (outpatient care). |
| Measure and plot the patient's height, weight, head circumference, and body mass index, and actively review for abnormal trends. |
| Screen for community environment and access to health and wellness resources when screening for socioeconomic status of the patient and family. |
| Discuss quality of life and health care system navigation capacity for children with chronic medically complex conditions. |
eTABLE B Initial List of Don't Recommendations for Children and Adolescents
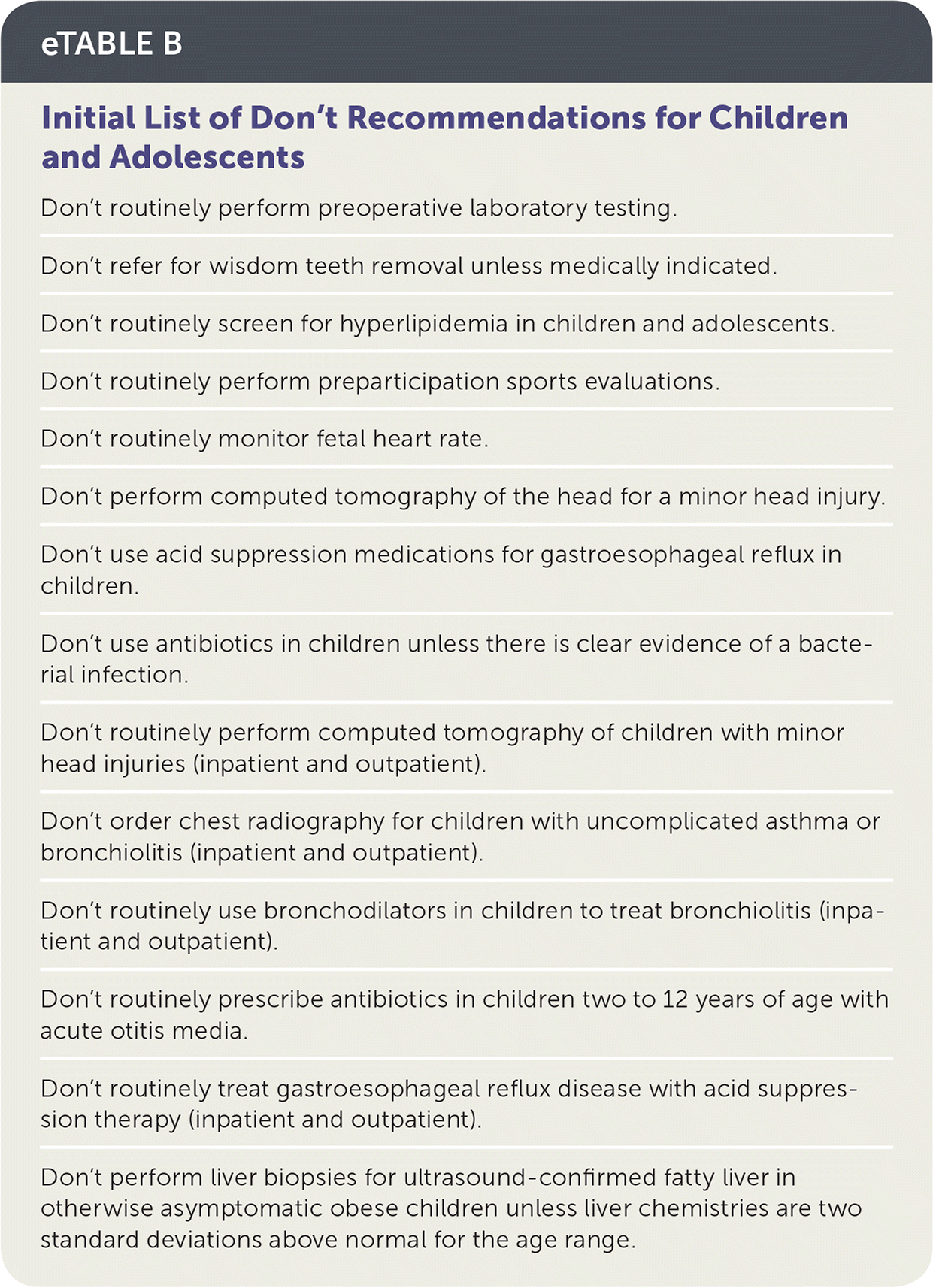
| Don't routinely perform preoperative laboratory testing. |
| Don't refer for wisdom teeth removal unless medically indicated. |
| Don't routinely screen for hyperlipidemia in children and adolescents. |
| Don't routinely perform preparticipation sports evaluations. |
| Don't routinely monitor fetal heart rate. |
| Don't perform computed tomography of the head for a minor head injury. |
| Don't use acid suppression medications for gastroesophageal reflux in children. |
| Don't use antibiotics in children unless there is clear evidence of a bacterial infection. |
| Don't routinely perform computed tomography of children with minor head injuries (inpatient and outpatient). |
| Don't order chest radiography for children with uncomplicated asthma or bronchiolitis (inpatient and outpatient). |
| Don't routinely use bronchodilators in children to treat bronchiolitis (inpatient and outpatient). |
| Don't routinely prescribe antibiotics in children two to 12 years of age with acute otitis media. |
| Don't routinely treat gastroesophageal reflux disease with acid suppression therapy (inpatient and outpatient). |
| Don't perform liver biopsies for ultrasound-confirmed fatty liver in otherwise asymptomatic obese children unless liver chemistries are two standard deviations above normal for the age range. |
TABLE 2 Right Care for Children: Final List of Do's and Don'ts Recommendations
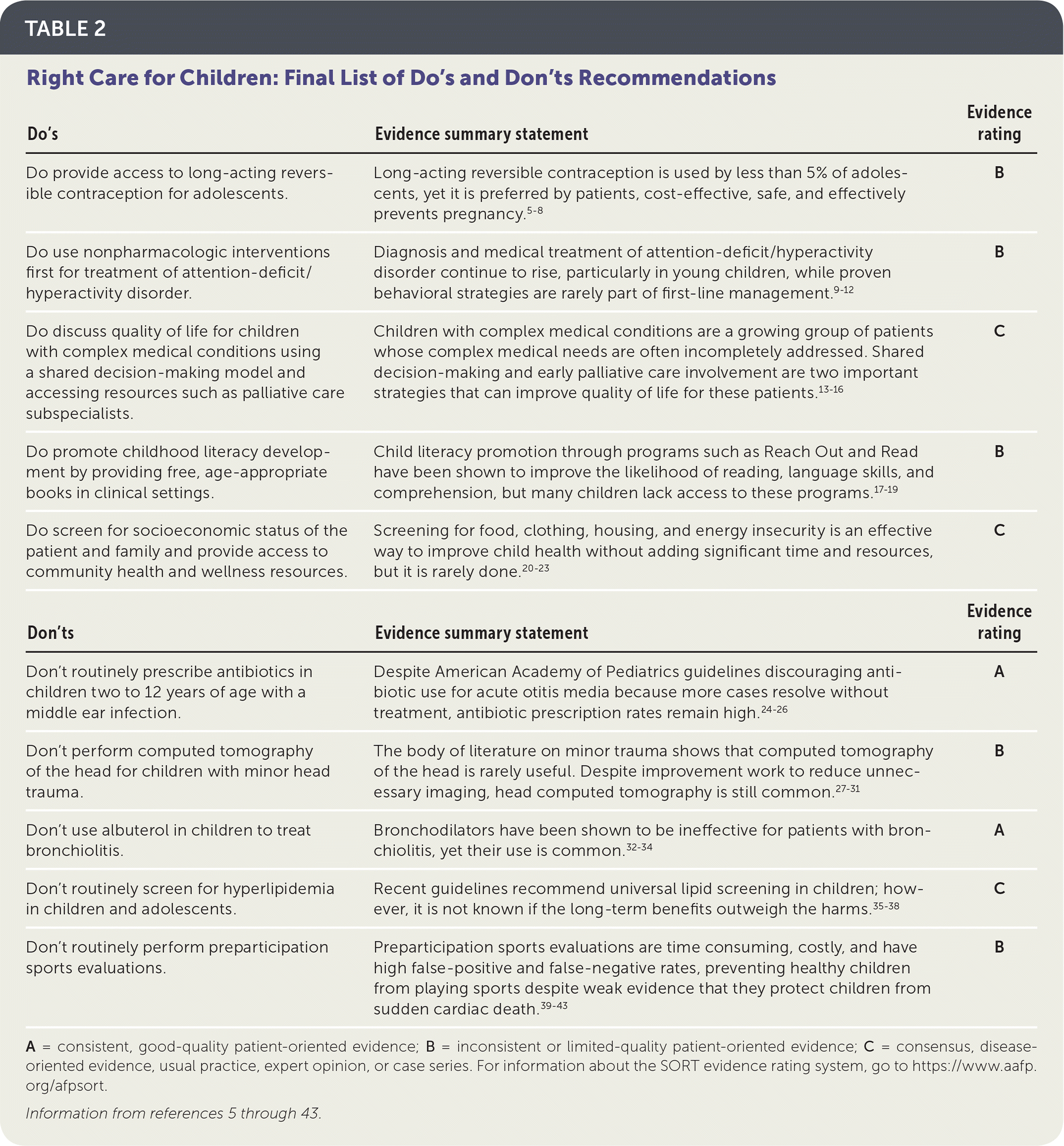
| Do's | Evidence summary statement | Evidence rating |
|---|---|---|
| Do provide access to long-acting reversible contraception for adolescents. | Long-acting reversible contraception is used by less than 5% of adolescents, yet it is preferred by patients, cost-effective, safe, and effectively prevents pregnancy.5–8 | B |
| Do use nonpharmacologic interventions first for treatment of attention-deficit/hyperactivity disorder. | Diagnosis and medical treatment of attention-deficit/hyperactivity disorder continue to rise, particularly in young children, while proven behavioral strategies are rarely part of first-line management.9–12 | B |
| Do discuss quality of life for children with complex medical conditions using a shared decision-making model and accessing resources such as palliative care subspecialists. | Children with complex medical conditions are a growing group of patients whose complex medical needs are often incompletely addressed. Shared decision-making and early palliative care involvement are two important strategies that can improve quality of life for these patients.13–16 | C |
| Do promote childhood literacy development by providing free, age-appropriate books in clinical settings. | Child literacy promotion through programs such as Reach Out and Read have been shown to improve the likelihood of reading, language skills, and comprehension, but many children lack access to these programs.17–19 | B |
| Do screen for socioeconomic status of the patient and family and provide access to community health and wellness resources. | Screening for food, clothing, housing, and energy insecurity is an effective way to improve child health without adding significant time and resources, but it is rarely done.20–23 | C |
| Don'ts | Evidence summary statement | Evidence rating |
| Don't routinely prescribe antibiotics in children two to 12 years of age with a middle ear infection. | Despite American Academy of Pediatrics guidelines discouraging antibiotic use for acute otitis media because more cases resolve without treatment, antibiotic prescription rates remain high.24–26 | A |
| Don't perform computed tomography of the head for children with minor head trauma. | The body of literature on minor trauma shows that computed tomography of the head is rarely useful. Despite improvement work to reduce unnecessary imaging, head computed tomography is still common.27–31 | B |
| Don't use albuterol in children to treat bronchiolitis. | Bronchodilators have been shown to be ineffective for patients with bronchiolitis, yet their use is common.32–34 | A |
| Don't routinely screen for hyperlipidemia in children and adolescents. | Recent guidelines recommend universal lipid screening in children; however, it is not known if the long-term benefits outweigh the harms.35–38 | C |
| Don't routinely perform preparticipation sports evaluations. | Preparticipation sports evaluations are time consuming, costly, and have high false-positive and false-negative rates, preventing healthy children from playing sports despite weak evidence that they protect children from sudden cardiac death.39–43 | B |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Top Five Do's: Underused Interventions
DO: PROVIDE ACCESS TO LONG-ACTING REVERSIBLE CONTRACEPTION FOR ADOLESCENTS
Studies including participants 14 years and older have demonstrated that long-acting reversible contraception for adolescents, such as intrauterine devices and dermal implants, are safe, cost-effective, and often preferred by patients.5 Long-acting reversible contraception lowers the rate of unintended pregnancy and the risk of treatment-related adverse events more than oral contraception or tubal ligation.6 State-funded programs offering long-acting reversible contraception have reduced rates of unplanned pregnancy, abortion, and preterm birth, resulting in substantial cost savings.44 Young women prefer reversible contraception because of convenience, duration of action, and reduced frequency and duration of menstrual bleeding.7 Compared with patients who use short-acting contraception, those who use long-acting reversible contraception are much more likely to continue use three years later.5 Long-acting reversible contraception use among all adolescent females in the United States ranges from 2% to 5%.45 Barriers to the use of long-acting reversible contraception, including cost and insurance coverage, availability, parental concerns, and lack of health care professional knowledge, should be addressed to increase access to this effective intervention.8
DO: USE NONPHARMACOLOGIC INTERVENTIONS FIRST FOR THE TREATMENT OF ATTENTION-DEFICIT/HYPERACTIVITY DISORDER
The prevalence of attention-deficit/hyperactivity disorder has significantly increased over the past 20 years.9 Both pharmacologic and behavioral therapy are effective, but pharmacologic therapy is expensive (costing more than $900 per patient per year in medication alone46) and can be associated with decreased appetite, sleep problems, and delayed growth.10,47
Behavioral therapy includes cognitive behavior therapy, parent training, classroom behavioral management, peer interventions, and other therapies. For children four to five years of age, parent behavioral training results in better conduct when compared with stimulant medications alone.11 Despite multiple studies recommending behavioral therapy as first-line treatment, almost one-half of U.S. children with attention-deficit/hyperactivity disorder are not receiving behavioral therapy.12 Barriers including a lack of qualified therapists, inadequate insurance coverage for behavioral therapy, and insufficient coordination of care should be addressed to make these interventions more accessible.
DO: DISCUSS QUALITY OF LIFE FOR CHILDREN WITH COMPLEX MEDICAL CONDITIONS USING A SHARED DECISION-MAKING MODEL AND ACCESS RESOURCES SUCH AS PALLIATIVE CARE SUBSPECIALISTS
Children with complex medical conditions are at greater risk of adverse medical, developmental, psychosocial, and familial outcomes.13 In 2011, children with medical complexity accounted for only 5.8% of childhood Medicaid enrollees, but 34% of Medicaid spending and 71% of 30-day unplanned readmissions.14
Patients and families report gaps in care that could be filled by comprehensive clinics with the expertise, time, and resources to create care plans.15 Shared decision-making is the preferred model of care delivery for children with medical complexity and may improve clinical outcomes and relationships between the family and the health care professional.48 Although studies on the impact of clinics that treat children with medical complexity have yielded mixed results, recent work is beginning to show decreased emergency department visits, hospital admissions, and costs.49
Children with complex medical conditions who receive early palliative care, both inpatient and outpatient, have high health care–related quality of life, decreased length of hospital stay, decreased invasive procedures, and decreased costs.16,50 However, significant barriers lead to underutilization of appropriate palliative care; in one study, the most frequently mentioned issues included uncertain prognosis, families not ready to acknowledge incurable conditions, language barriers, and time constraints.51
DO: PROMOTE CHILDHOOD LITERACY DEVELOPMENT BY PROVIDING FREE, AGE-APPROPRIATE BOOKS IN CLINICAL SETTINGS
Programs encouraging childhood literacy52 such as Reach Out and Read first gained significant support after several studies suggested that parents who received books were more likely to read to and with their children.17 Literacy promotion efforts among Hispanic populations similarly demonstrate increased engagement.18 The likelihood of reading increased significantly for non–English speaking families even when English language books were used.53 Further research has shown that receptive and expressive language scores were higher among children 18 to 25 months of age who received literacy promotion during their well-child visits.19 Despite this evidence, childhood literacy development programs only reach around 4.5 million children, less than one-third of the recent U.S. census estimate of 20.2 million children younger than five years living in the United States.54,55
DO: SCREEN FOR SOCIOECONOMIC STATUS OF THE PATIENT AND FAMILY AND PROVIDE ACCESS TO COMMUNITY HEALTH AND WELLNESS RESOURCES
Social determinants of health such as poverty, housing insecurity, food insecurity (https://www.aafp.org/afp/2018/0801/p143.html), poor education, and barriers to employment can all be linked to poor health outcomes beginning in childhood and adolescence.55,56 The American Academy of Pediatrics (AAP) and American Academy of Family Physicians (AAFP) support the promotion of health equity using clinical encounters to identify and address social, financial, educational, and environmental needs of patients.21,56 However, concerns about insufficient time, fear of offending parents, and inadequate knowledge about local resources lead to low rates of screening and referral.22 Simple electronic tools may facilitate connecting families to community resources22,57 without placing undue burden on health care professionals. Connecting families to community resources is associated with greater odds of employment and access to child care and fuel assistance, while decreasing the risk of homelessness.23 The AAFP's EveryONE Project (https://www.aafp.org/patient-care/social-determinants-of-health/everyone-project.html) offers several online tools to connect patients to community resources. Resources that address energy, housing, income, and nutrition support can improve health outcomes and lower health care costs.23 Studies in the clinic setting and in the hospital suggest that parental perceptions of health care professional–driven screening for social determinants of health are positive.58,59
Top Five Don'ts: Overused Interventions
DON'T: ROUTINELY PRESCRIBE ANTIBIOTICS IN CHILDREN TWO TO 12 YEARS OF AGE WITH A MIDDLE EAR INFECTION
Health care professionals often misdiagnose middle ear infections, and even for true infections, antibiotics only provide minimal benefit compared with placebo.60 Although a Cochrane review found that the number needed to treat to reduce pain at 10 to 12 days was 7, there was no significant difference in pain reduction at 24 hours, and patients rarely have pain beyond two weeks.24 Compared with expectant observation, immediate antibiotic treatment does not reduce abnormal tympanometry findings at four weeks, tympanic membrane perforation, or acute otitis media (AOM) recurrence. Compared with placebo, antibiotics decrease tympanic membrane perforations (number needed to treat = 33) and the risk of contralateral AOM, but they have a number needed to harm of 14 for any adverse event (e.g., vomiting, diarrhea, rash).24 Antibiotics have not been proven to reduce the risk of serious pathology associated with AOM such as mastoiditis.25 These findings led the AAP and AAFP to recommend against antibiotics for initial management of most children,26 a strategy that has been shown to be cost-effective.61
DON'T: PERFORM COMPUTED TOMOGRAPHY (CT) OF THE HEAD FOR CHILDREN WITH MINOR HEAD TRAUMA
Head CT can be useful to guide interventions in children with severe traumatic brain injury. However, ionizing radiation exposure from CT use has been associated with an increased risk of the development of malignancies.62 In children with minor head injuries, recent Centers for Disease Control and Prevention guidelines27 recommend against CT because it rarely reveals intracranial bleeds or other serious findings but may detect incidental findings (4% in one large study28) and lead to overdiagnosis and overtreatment.29
There is some evidence that CT use for children with minor head injury has decreased during the past decade, likely driven by new clinical prediction rules for the detection of “clinically important traumatic brain injury.”30 This reduction in unnecessary imaging could reduce costs, radiation exposure, and the use of potentially harmful downstream interventions (e.g., repeat imaging, hospitalization, and in some cases, neurosurgery).31
DON'T: USE ALBUTEROL IN CHILDREN TO TREAT BRONCHIOLITIS
In 2014, the AAP revised its bronchiolitis practice guidelines, moving away from the option of trial doses of bronchodilators to recommending against the use of bronchodilators entirely.32 These recommendations are supported by a Cochrane meta-analysis demonstrating that beta agonists do not improve meaningful outcomes such as hospital admission rates, length of stay, or duration of symptoms.63 Quality improvement work has shown early success in decreasing overuse in inpatient settings, with one multicenter collaborative demonstrating decreased bronchodilator use by 29%, reduced steroid use, and reduced length of stay,64 and a meta-analysis demonstrating substantial decreases in repeated bronchodilator dosing.33 However, bronchodilator use, with other ineffective interventions in bronchiolitis such as steroids, is high and extremely variable.34 Additionally, little is known about practice patterns in the outpatient and urgent care settings where most children with bronchiolitis receive care.
DON'T: ROUTINELY SCREEN FOR HYPERLIPIDEMIA IN CHILDREN AND ADOLESCENTS
Universal lipid screening for children was recommended by the National Heart, Lung, and Blood Institute and the AAP in 2011 to identify children with familial hypercholesterolemia missed by family history alone.65,66 Although universal lipid screening does identify additional children with familial hypercholesterolemia, 10 children screen falsely positive by random lipid screen for every true case of hyperlipidemia confirmed by fasting lipids. False positives lead to additional fasting blood work.67 Even after false-positive cases have been excluded, 85% of children who would be started on statin therapy for elevated low-density lipoprotein levels do not have familial hypercholesterolemia.35 Although short-term safety data on statins in children are reassuring, all published trials were exclusively done on children with familial hypercholesterolemia and were industry funded.36 Furthermore, there are no long-term studies on the safety of starting statins in childhood and continuing for decades.37 Although most trials in children demonstrate reductions in low-density lipoprotein and other surrogate markers with statins, evidence that statins decrease cardiovascular events in this population is lacking.36 The U.S. Preventive Services Task Force and the AAFP agree that the current evidence is insufficient to assess the balance of benefits and harms of screening for lipid disorders in children and adolescents.38
DON'T: ROUTINELY PERFORM PREPARTICIPATION SPORTS EVALUATIONS
Preparticipation sports evaluations are often recommended or required by schools and athletic organizations in the United States and other developed countries; however, evidence does not support these recommendations and should inform future policy to emphasize recommendations proven to benefit adolescent health.39,68 Sudden cardiac death in adolescents and young adults is a devastating but rare occurrence, affecting an estimated one in 150,000 sports participants per year, totaling fewer than 100 deaths per year in the United States.40 When sudden cardiac death occurs, preparticipation sports evaluations often do not identify the athletes who were most at risk.41 Typical testing involves a detailed family history and physical examination,69,70 and in some places includes electrocardiography. These evaluations have a high false-positive rate for rhythm and structural abnormalities,42,71 a high false-negative rate for hypertrophic cardiomyopathy,71 and are expensive.43 Children are often unnecessarily held out of a beneficial physical activity until these evaluations are completed.
Data Sources: A PubMed search for each recommendation was completed using key terms drawn from the wording specific to each recommendation. The search included meta-analyses, systematic reviews, Cochrane reviews, randomized controlled trials, review articles, and retrospective cohort studies. Search dates: January and February 2017, and December 21, 2018.
The authors thank Vikas Saini, MD, and Shannon Brownlee for their thoughtful review of this manuscript. They also thank Carissa Fu, the members of the Right Care Alliance Children's Health Council, and the Lown Institute for their support.

