
Am Fam Physician. 2020;101(10):623-624
Author disclosure: No relevant financial affiliations.
A 30-year-old man presented to the family medicine clinic as a new patient. He had a long history of uncontrollable thick callus formations on both hands and feet, which began when he was about six months old. His mother noticed thickened skin and blisters on his knees and hands when he started crawling. By 13 months old, his toenails had thickened and were removed.
Physical examination revealed severe callus formation and a marked keratinized, yellow skin proliferation over the soles of both feet, with skin fissures and cracking. Similar hyperkeratotic lesions were also seen on the palms of both hands (Figure 1 and Figure 2). Hypertrophy of the nail beds was present on both feet and hands.
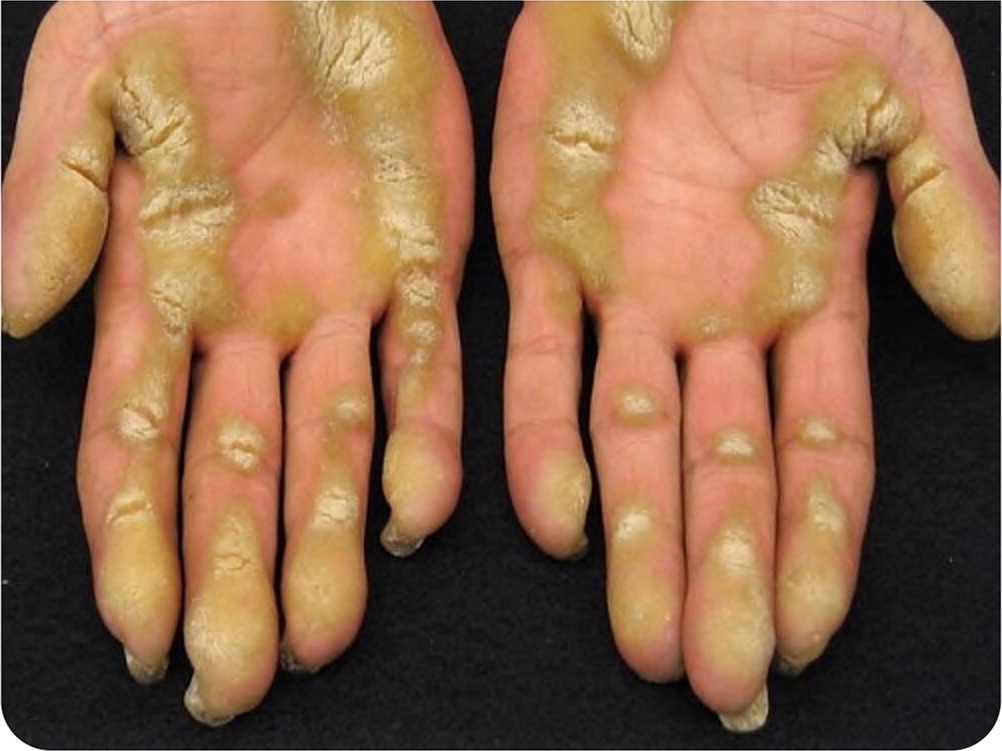
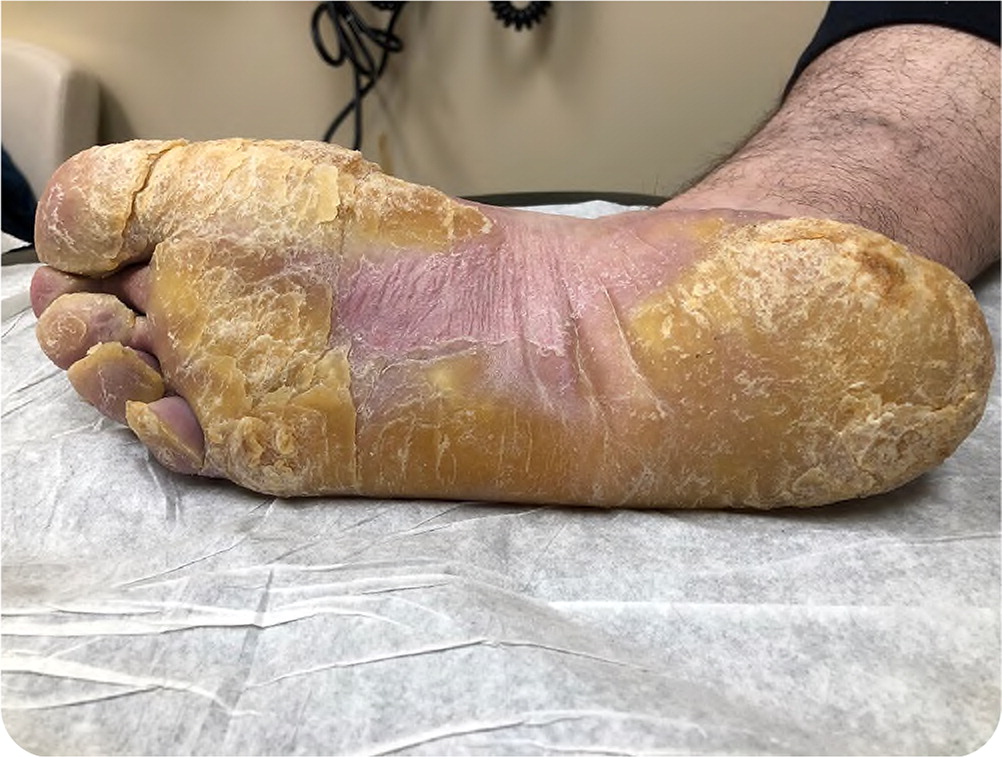
Question
Discussion
The answer is C: pachyonychia congenita. Pachyonychia congenita is an extremely rare genetic skin disorder caused by a mutation in one of the keratin genes (KRT6A, KRT6B, KRT6C, KRT16, KRT17).1 It is inherited in an autosomal dominant pattern. The most common and striking features of the condition are severe callus formation and painful blistering on the soles and palms. A triad of hypertrophic nail dystrophy, plantar/palmar hyperkeratosis, and severe plantar pain occurs across all types. The age of onset is variable, but most cases are clinically apparent during the first few years of life. Adult onset is rare.
Lesions typically begin to develop when a child starts weight-bearing and walking, with diffuse or focal hyperkeratosis of the soles and palms and underlying frictional blisters that cause severe pain. Additional clinical findings may include oral leukoplakia, follicular hyperkeratosis on elbows and knees, palmoplantar hyperhidrosis, and cutaneous cysts.2 The diagnosis is made clinically with the presence of the classic triad. The diagnosis can be confirmed with molecular genetic testing and identification of a mutation in one of the five keratin genes.3
Pachyonychia congenita is chronically debilitating and has no cure. Treatment focuses on relieving symptoms. Mechanical trimming or grinding of lesions with pumice or a sharp instrument, use of topical softening agents containing salicylic acid or urea, use of oral retinoids, and incision and drainage of cutaneous cysts may be helpful. Pain medication is often necessary. Special footwear or orthotics can reduce the pain, and patients may require assistive devices such as canes or wheelchairs.3,4
Oral retinoids, including acitretin (Soriatane) and isotretinoin, are used to treat several hyperkeratotic disorders, but caution should be used because these agents are known to be teratogenic. Pregnancy is contraindicated for three years after discontinuing acitretin; therefore, isotretinoin is commonly used in women.1,2
Ichthyosis vulgaris is a condition present from birth that is characterized by mild xerosis with scaling. It is most pronounced on the lower extremities. Large, thickened scales can develop in severe cases. Lesions on the palms and soles are nonsevere hyperlinear lines without blistering. Ichthyosis vulgaris is associated with atopic dermatitis and keratosis pilaris on the arms and legs.5,6
Palmoplantar psoriasis can present on any area of skin, including the palms and soles, as sharply marginated, erythematous plaques with silvery or yellow scales. The plaques become thickened and keratotic. Hyperkeratotic lesions on the palms and soles are not easily removed, unlike lesions on other areas of the body. Desquamation of the hyperkeratosis reveals an inflammatory plaque at the base.5,6
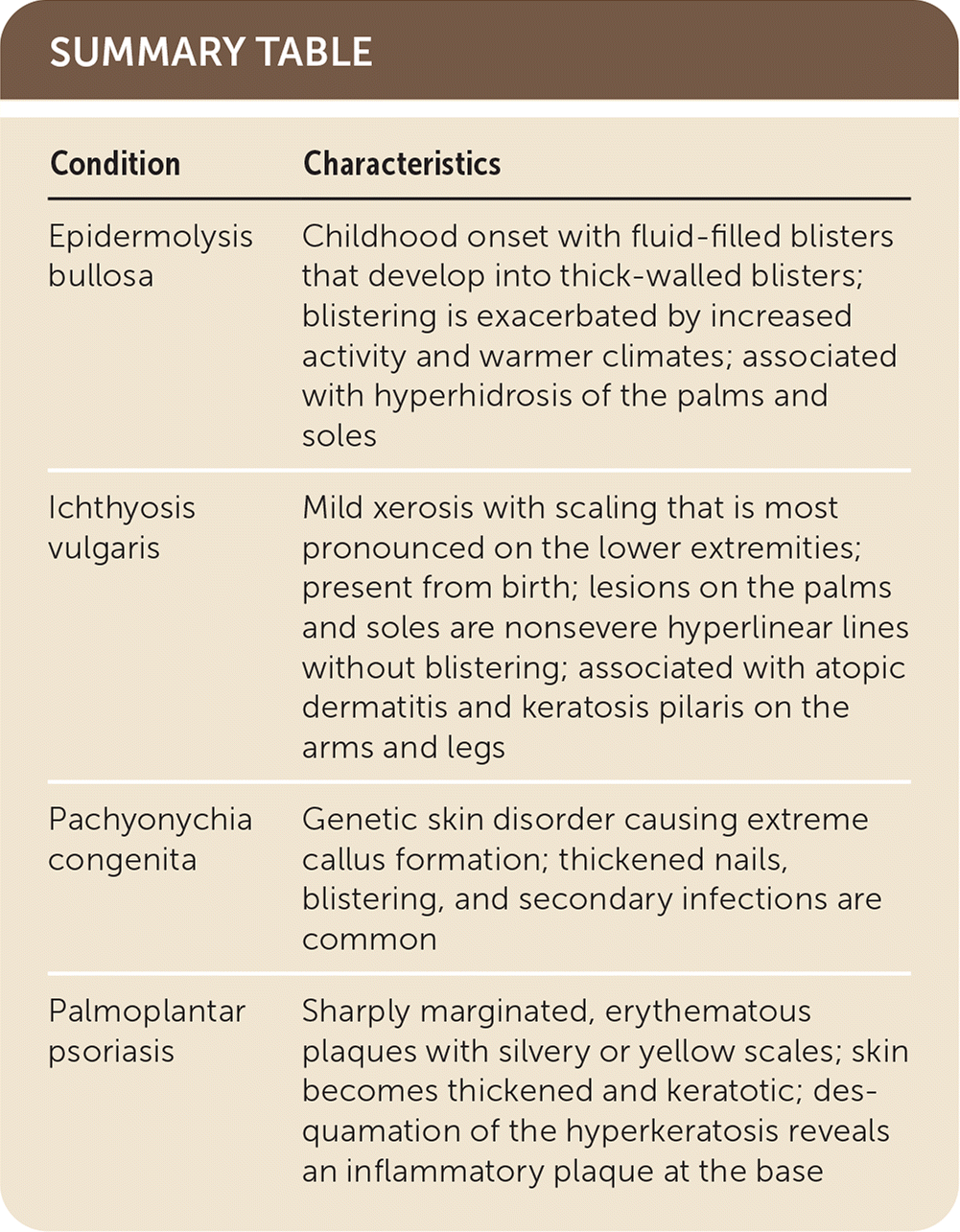
| Condition | Characteristics |
|---|---|
| Epidermolysis bullosa | Childhood onset with fluid-filled blisters that develop into thick-walled blisters; blistering is exacerbated by increased activity and warmer climates; associated with hyperhidrosis of the palms and soles |
| Ichthyosis vulgaris | Mild xerosis with scaling that is most pronounced on the lower extremities; present from birth; lesions on the palms and soles are nonsevere hyperlinear lines without blistering; associated with atopic dermatitis and keratosis pilaris on the arms and legs |
| Pachyonychia congenita | Genetic skin disorder causing extreme callus formation; thickened nails, blistering, and secondary infections are common |
| Palmoplantar psoriasis | Sharply marginated, erythematous plaques with silvery or yellow scales; skin becomes thickened and keratotic; desquamation of the hyperkeratosis reveals an inflammatory plaque at the base |
