
Am Fam Physician. 2020;101(10):625-629
Author disclosure: No relevant financial affiliations.
Case Scenario
An 81-year-old man came for a routine visit with his wife, who mentioned that her husband has become more forgetful, confused, and requires more assistance with his activities of daily living. She was worried about his safety and would like you to talk to him about not driving anymore. My patient was upset by the suggestion that he may no longer be fit to drive safely. How should a family physician address this?
Commentary
Advancing age on its own is not a reason to stop driving. The ability to drive may enable older adults to maintain family and social interactions and to promote independence by accessing community resources, services, and volunteer opportunities.
Nevertheless, crash fatalities in people older than 65 years have increased 22% from 2008 to 2017; older age increases fatality risk and is highest among driver older than 85 years.1 Several factors influence this trend, including greater numbers of older drivers and miles driven, and older age increases fatality risk and is highest among drivers older than 85 years.2 If an accident occurs, older drivers are also more likely to sustain more serious injury than younger occupants of vehicles.
Despite the age-related increase in potential for harm associated with driving, only 7% of older adults report discussing driving safety issues with a family member.3 It is often a family member or caregiver who forces the issue by bringing it to the attention of the family physician. Table 1 describes some age-related changes that family members, caregivers, or patients might notice that might affect a person's ability to drive safely.4–10
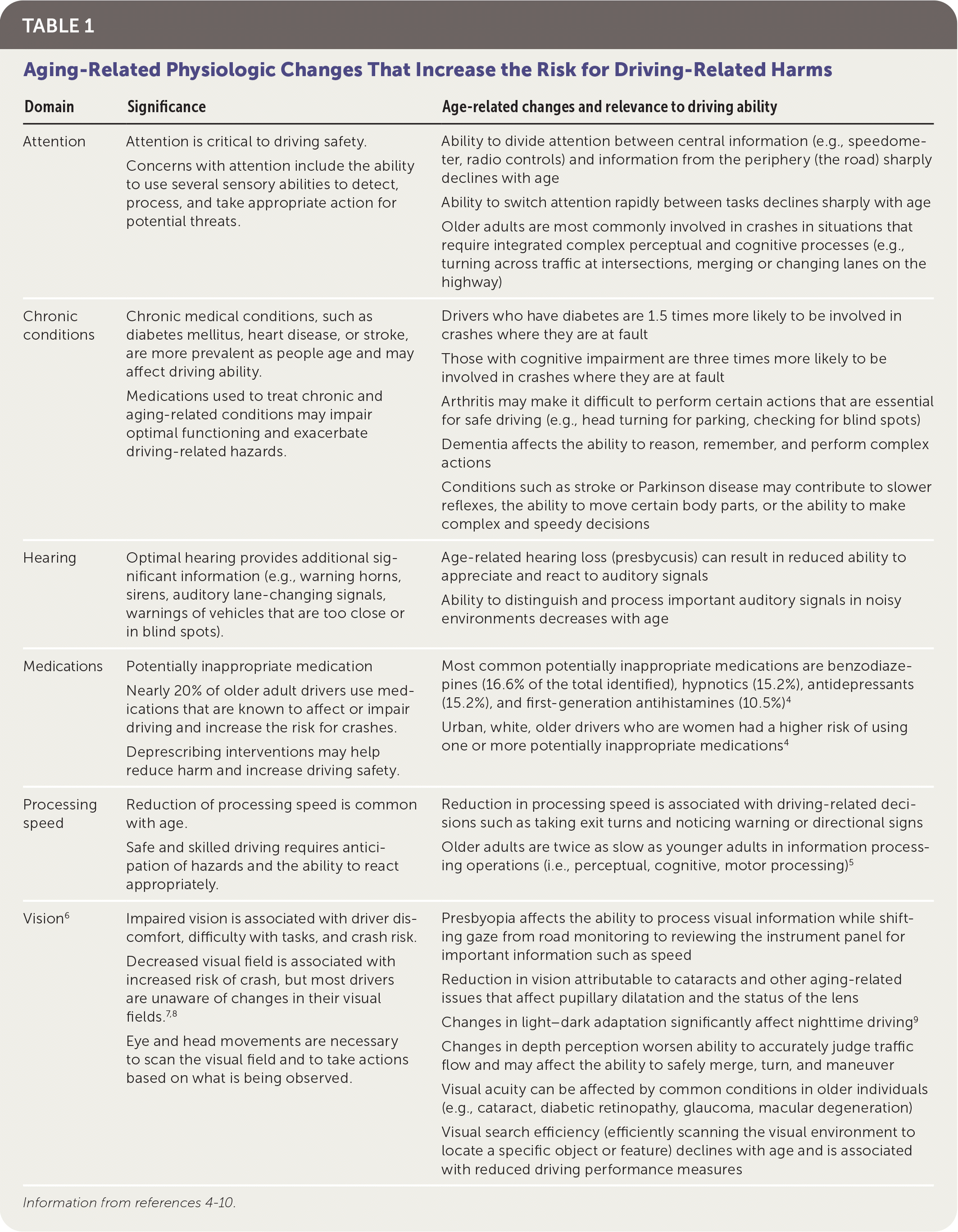
| Domain | Significance | Age-related changes and relevance to driving ability |
|---|---|---|
| Attention | Attention is critical to driving safety. Concerns with attention include the ability to use several sensory abilities to detect, process, and take appropriate action for potential threats. | Ability to divide attention between central information (e.g., speedometer, radio controls) and information from the periphery (the road) sharply declines with age Ability to switch attention rapidly between tasks declines sharply with age Older adults are most commonly involved in crashes in situations that require integrated complex perceptual and cognitive processes (e.g., turning across traffic at intersections, merging or changing lanes on the highway) |
| Chronic conditions | Chronic medical conditions, such as diabetes mellitus, heart disease, or stroke, are more prevalent as people age and may affect driving ability. Medications used to treat chronic and aging-related conditions may impair optimal functioning and exacerbate driving-related hazards. | Drivers who have diabetes are 1.5 times more likely to be involved in crashes where they are at fault Those with cognitive impairment are three times more likely to be involved in crashes where they are at fault Arthritis may make it difficult to perform certain actions that are essential for safe driving (e.g., head turning for parking, checking for blind spots) Dementia affects the ability to reason, remember, and perform complex actions Conditions such as stroke or Parkinson disease may contribute to slower reflexes, the ability to move certain body parts, or the ability to make complex and speedy decisions |
| Hearing | Optimal hearing provides additional significant information (e.g., warning horns, sirens, auditory lane-changing signals, warnings of vehicles that are too close or in blind spots). | Age-related hearing loss (presbycusis) can result in reduced ability to appreciate and react to auditory signals Ability to distinguish and process important auditory signals in noisy environments decreases with age |
| Medications | Potentially inappropriate medication Nearly 20% of older adult drivers use medications that are known to affect or impair driving and increase the risk for crashes. Deprescribing interventions may help reduce harm and increase driving safety. | Most common potentially inappropriate medications are benzodiazepines (16.6% of the total identified), hypnotics (15.2%), antidepressants (15.2%), and first-generation antihistamines (10.5%)4 Urban, white, older drivers who are women had a higher risk of using one or more potentially inappropriate medications4 |
| Processing speed | Reduction of processing speed is common with age. Safe and skilled driving requires anticipation of hazards and the ability to react appropriately. | Reduction in processing speed is associated with driving-related decisions such as taking exit turns and noticing warning or directional signs Older adults are twice as slow as younger adults in information processing operations (i.e., perceptual, cognitive, motor processing)5 |
| Vision6 | Impaired vision is associated with driver discomfort, difficulty with tasks, and crash risk. Decreased visual field is associated with increased risk of crash, but most drivers are unaware of changes in their visual fields.7,8 Eye and head movements are necessary to scan the visual field and to take actions based on what is being observed. | Presbyopia affects the ability to process visual information while shifting gaze from road monitoring to reviewing the instrument panel for important information such as speed Reduction in vision attributable to cataracts and other aging-related issues that affect pupillary dilatation and the status of the lens Changes in light–dark adaptation significantly affect nighttime driving9 Changes in depth perception worsen ability to accurately judge traffic flow and may affect the ability to safely merge, turn, and maneuver Visual acuity can be affected by common conditions in older individuals (e.g., cataract, diabetic retinopathy, glaucoma, macular degeneration) Visual search efficiency (efficiently scanning the visual environment to locate a specific object or feature) declines with age and is associated with reduced driving performance measures |
Counseling and Communicating with Patients
Older adult drivers may deny, resist, or resent any suggestion that they may no longer be fit to drive. Patients may be unwilling to engage in a driving evaluation because of impaired insight regarding driving challenges and abilities, and they may be concerned about the effects of losing their driver's license.11,12
Broaching the subject is likely to be uncomfortable for the physician because of insufficient time for full discussion, inadequate knowledge of available resources, concern about negative response from the patient, and potential harm to the physician-patient relationship, especially when other family members are involved.13–15 Despite these potential barriers, studies have found that older drivers are open to engaging in a conversation about driving if it is framed as a discussion about promoting the patient's safety or is presented as a routine part of the health visit.14–17

| Are you still driving? Do you have any issues with that? |
| Did you drive yourself here today? |
| Has anyone expressed concerns about your driving? |
| Have you lost any confidence in your ability to be a safe driver? |
| How do you usually get around? |
Older drivers may be receptive to discussion about driving when it is presented in the context of medical conditions.7,15 Family physicians can explain how medical conditions and medications can affect driving through acute effects (e.g., dizziness, lethargy, vision changes) or chronic functional deficits (e.g., changes in cognition, decreased range of motion). The self-screening tools in eTable A may help increase insight and awareness of driving risk and can facilitate the discussion. These online tools can be time consuming to complete and are best completed before the physician visit.
| Tool | Details |
|---|---|
| Am I a Safe Driver?A1,A2 | 20-point checklist reviewing driving history, recommended by the American Geriatrics Society, although its validity is undetermined. https://granddriver.net/wp-content/uploads/Toolkit_Checklist.pdf |
| Driving Decisions Workbook | Questionnaire created by the University of Michigan that provides individualized answers based on the driver's response to the questions and then gives drivers information about what to do with the results and how to reduce their driving risk. http://deepblue.lib.umich.edu/bitstream/handle/2027.42/1321/94135.0001.001.pdf?sequence=2&isAllowed=y |
| Fitness-to-Drive ScreeningA3 | 54-point test completed by the older driver and a proxy rater (e.g., occupational therapy practitioners, caregiver, family member, friend). This online test predicts the likely outcome of the older drivers on-road assessment and takes about 20 minutes to complete, which may be too long for some. http://fitnesstodrive.phhp.ufl.edu/us/ |
| SAFER Driving survey | Lengthy online assessment that may require assistance from family or professional caregivers; drivers are asked about their medical conditions and medications and then answers are correlated to related driving skills and recommendations for further evaluations are provided. http://um-saferdriving.org |
Assessing Driving Fitness
Assessment of fitness to drive aims to establish any shortcomings in the driver's abilities to meet the demands of the tasks involved in driving, in particular the challenges of turning across opposing traffic, nighttime driving, road-hazard detection, and sign perception.7 After identifying health issues that might cause impairment, including a history of seizures, cardiovascular disease, or syncope, assessment proceeds with a driving history, followed by evaluation of driving-related skills such as cognition, vision, and somatosensory function.7 The patient's medications should be reviewed to identify any that could affect driving ability.7,10,19 Table 3 lists some assessment tools that may be used in the primary care office for assessing driving ability.7,8,20–31
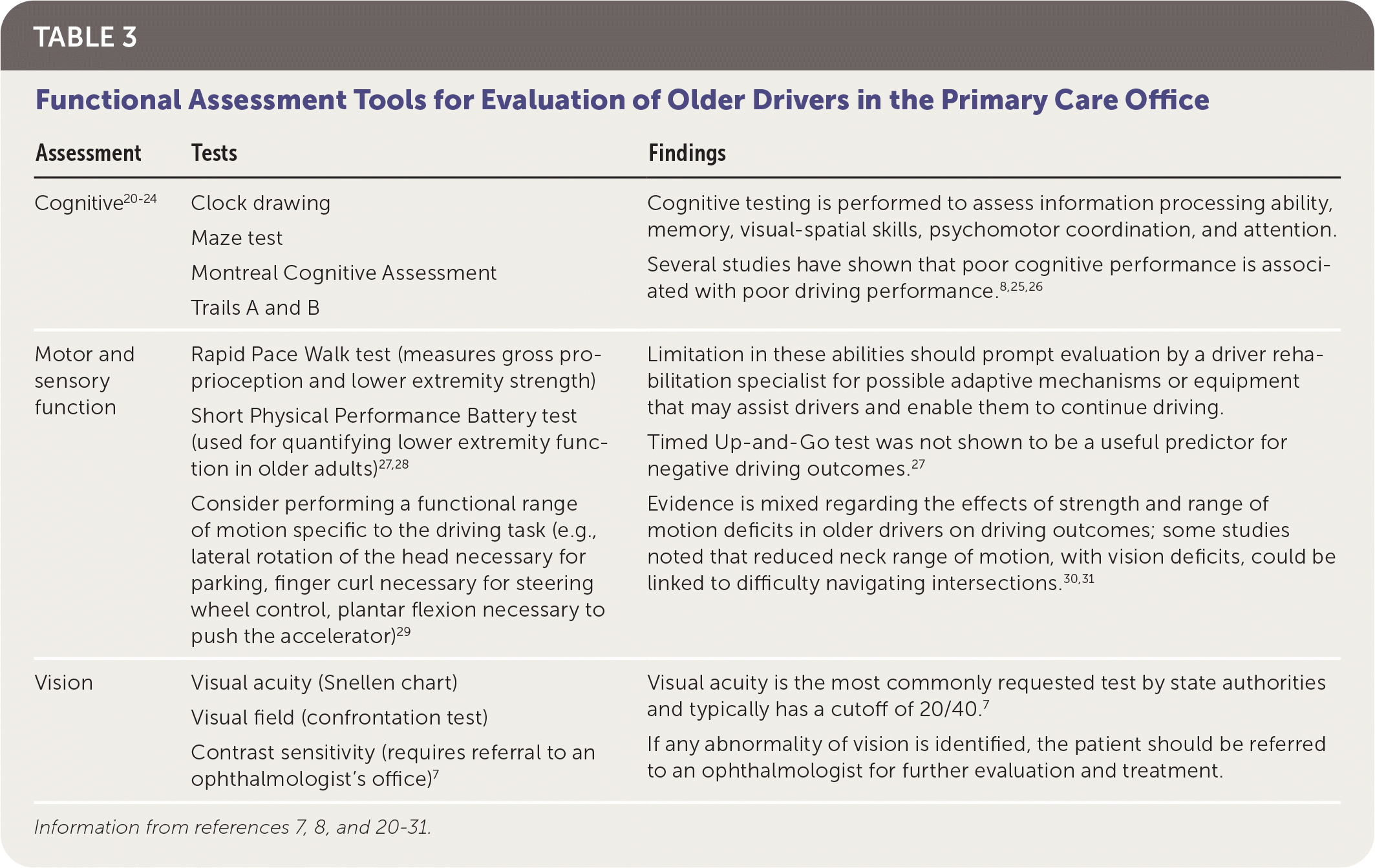
| Assessment | Tests | Findings |
|---|---|---|
| Cognitive 20–24 | Clock drawing Maze test Montreal Cognitive Assessment Trails A and B | Cognitive testing is performed to assess information processing ability, memory, visual-spatial skills, psychomotor coordination, and attention. Several studies have shown that poor cognitive performance is associated with poor driving performance.8,25,26 |
| Motor and sensory function | Rapid Pace Walk test (measures gross proprioception and lower extremity strength) Short Physical Performance Battery test (used for quantifying lower extremity function in older adults)27,28 Consider performing a functional range of motion specific to the driving task (e.g., lateral rotation of the head necessary for parking, finger curl necessary for steering wheel control, plantar flexion necessary to push the accelerator)29 | Limitation in these abilities should prompt evaluation by a driver rehabilitation specialist for possible adaptive mechanisms or equipment that may assist drivers and enable them to continue driving. Timed Up-and-Go test was not shown to be a useful predictor for negative driving outcomes.27 Evidence is mixed regarding the effects of strength and range of motion deficits in older drivers on driving outcomes; some studies noted that reduced neck range of motion, with vision deficits, could be linked to difficulty navigating intersections.30,31 |
| Vision | Visual acuity (Snellen chart) Visual field (confrontation test) Contrast sensitivity (requires referral to an ophthalmologist's office)7 | Visual acuity is the most commonly requested test by state authorities and typically has a cutoff of 20/40.7 If any abnormality of vision is identified, the patient should be referred to an ophthalmologist for further evaluation and treatment. |
Although they are all based on expert opinion rather than evidence, the results of self-assessment tools such as those listed in eTable A can be reviewed by the physician to evaluate risk and to help the driver gain awareness of possible limitations.
On-road driving assessment is the preferred option for assessing safety risk. It typically requires a vehicle equipped with specific safety features such as instructor brakes.7 The test is performed by a rehabilitation specialist. Driving simulators have also been studied as an alternative to on-road testing, and research shows they are valid for identifying at-risk drivers.25,32 Other specialists may also be helpful in assessing driving fitness and making cessation decisions, such as neurologists, psychiatrists, and cardiologists. The physician is not a legal authority, but state rules and regulations about licensure renewal should be reviewed. State-by-state summaries can be found at https://www.claimsjournal.com/news/national/2012/09/19/213818.htm.
Interventions
If the driver demonstrates insight about age-related changes and a plausible ability to self-regulate, the physician can initiate a discussion about adaptation to the road environment. This involves avoiding challenging conditions (bad weather, driving at night), driving at reduced speeds, or planning routes to avoid left turns or busy intersections (see the Driving Decisions Workbook in eTable A). Studies have not shown, however, that self-regulation a lone, without addressing underlying health issues or the roadway environment, reduces crash risk.10,33
Physicians should address remediable deficits and, if needed, provide referrals to the appropriate services (e.g., ophthalmology, physical therapy). Physicians should inform patients about the availability of driving rehabilitation specialists who may be able to assist with improving driving skills and/or incorporating adaptive driving equipment, such as reduced effort steering assistance. Costs vary for specialist assessments, but they are typically at least $200 for an assessment and $100 or more per hour for driving rehabilitation services. Adaptive equipment, such as reduced effort steering assistance, can cost hundreds to thousands of dollars. Insurance coverage varies for evaluation, rehabilitation, and equipment.7
When recommending driving cessation, the significant social, emotional, and psychological ramifications must be considered. Cessation of driving has been associated with depression and nursing home admission.3,34 Physicians should encourage patients and families to ensure that other forms of transportation are available to continue social and community engagement. Quality of life is often maintained after driving cessation if older patients perceive that they have sufficient input regarding the reason for the decision, alternative transportation arrangements, and sufficient time to process and adjust to the changes.12,15,35–37
When considering the patient in the case scenario, the physician could ask the patient some questions about driving (Table 2).7,15 The physician could then have a conversation about how medications and cognitive abilities could affect the patient's driving ability. The physician could finally recommend an on-road driving assessment to further help with the patient's unhappiness with the situation and with the wife's concerns.
