
Am Fam Physician. 2020;101(12):758-759
Author disclosure: No relevant financial affiliations.
Clinical Question
Which patients presenting with symptoms of acute rhinosinusitis have acute bacterial rhinosinusitis?
Evidence Summary
Acute rhinosinusitis in adults is defined as sinonasal inflammation that lasts less than four weeks and is associated with the sudden onset of symptoms.1 In the 2012 National Health Interview Survey, 12% of respondents reported being diagnosed with rhinosinusitis in the previous 12 months.2 In 2016, there were 8 million U.S. ambulatory visits for acute sinusitis.3 Acute bacterial rhinosinusitis develops in only 0.5% to 2% of all upper respiratory tract infections.4
A 2018 Cochrane review demonstrated that the potential benefit of antibiotics for the treatment of acute rhinosinusitis, diagnosed clinically or confirmed with imaging, is marginal.5 Without antibiotics, rhinosinusitis resolved in 46% of patients after one week and in 64% of patients after 14 days.5 Antibiotics can shorten time to resolution but in only five to 11 more people per 100 compared with placebo or no treatment.5 Despite this, approximately 86% of U.S. ambulatory visits for acute rhinosinusitis result in oral antibiotic prescriptions.1 In Europe, antibiotic prescription rates for acute rhinosinusitis in primary care range from 72% to 92%.6
There is no consensus on the diagnostic criteria for acute bacterial rhinosinusitis. A 2007 European position paper states that acute bacterial rhinosinusitis should be suspected with the presence of at least three of the following symptoms or signs: discolored discharge with unilateral predominance and purulent secretion in the nasal cavity, severe local pain with unilateral predominance, fever greater than 100.4°F (38°C), elevated erythrocyte sedimentation rate or C-reactive protein (CRP) level, and double sickening (i.e., deterioration after an initial milder phase of illness).7
The American Academy of Otolaryngology–Head and Neck Surgery recommends diagnosing acute bacterial rhinosinusitis when symptoms or signs of acute rhinosinusitis (purulent nasal drainage accompanied by nasal obstruction, facial pain/pressure/fullness, or both) persist without evidence of improvement for at least 10 days after the onset of symptoms, or when symptoms or signs of acute rhinosinusitis worsen within 10 days of initial improvement or milder phase of illness (double sickening).8 However, a 2016 international consensus statement on rhinosinusitis concluded that symptoms such as purulent nasal discharge, fever, or facial pain alone cannot distinguish between viral and bacterial infection and that further studies are needed.1
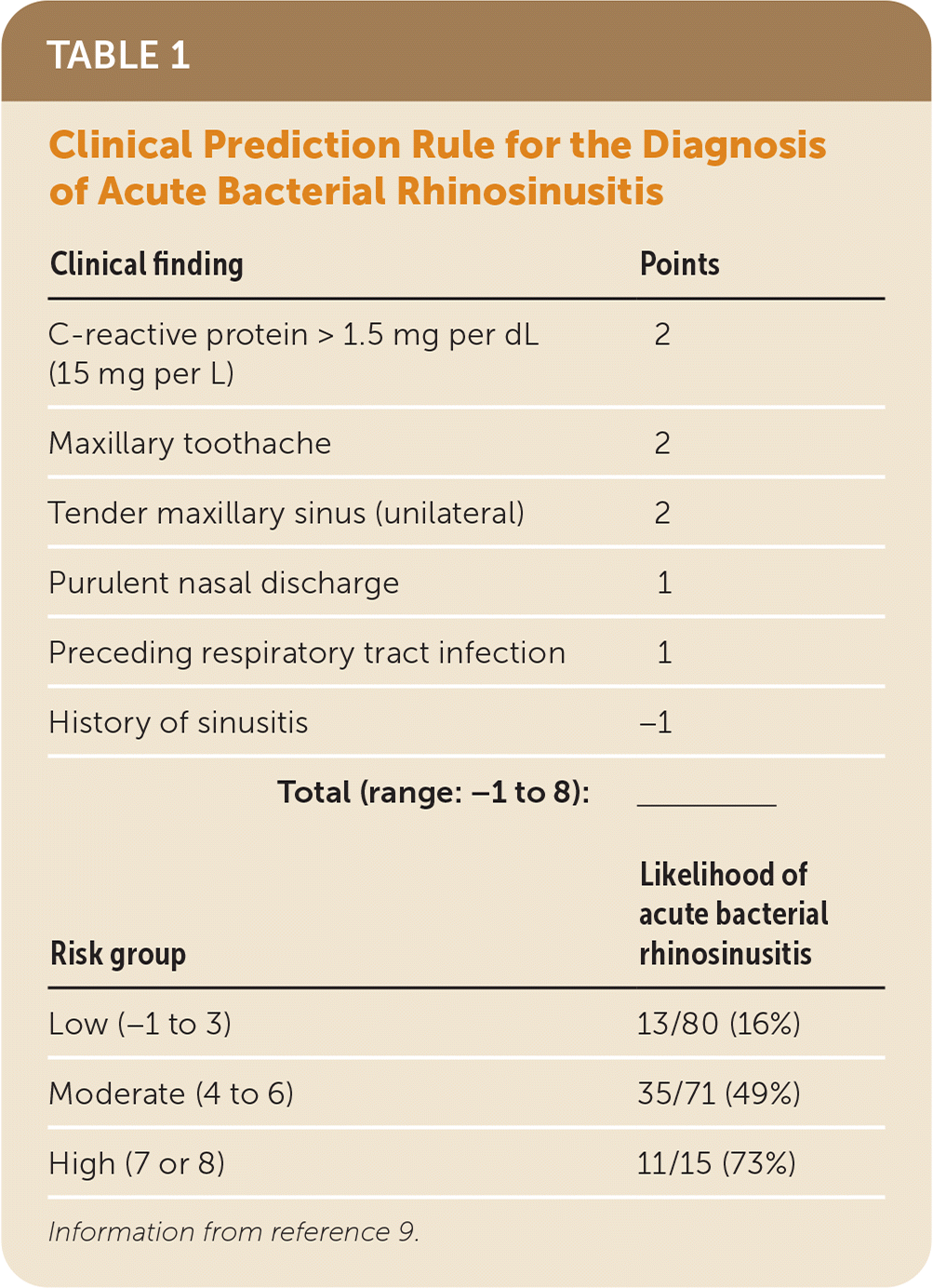
In 2017, a clinical prediction rule (Table 1) was created for the diagnosis of acute rhinosinusitis and acute bacterial rhinosinusitis using 175 adult Danish patients in whom acute maxillary sinusitis was clinically suspected.9 CRP and erythrocyte sedimentation rate were measured and computed tomography of the sinuses was performed; antral puncture was also performed if computed tomography showed mucosal thickening or fluid. If a culture of antral fluid was positive for bacteria, the patient was deemed to have acute bacterial rhinosinusitis (about one-third of all patients). Of those with a low risk based on the clinical prediction rule (score of −1 to 3 points), 16% had acute bacterial rhinosinusitis, whereas of those with moderate risk (4 to 6 points) or high risk (7 to 8 points), 49% and 73% had acute bacterial rhinosinusitis, respectively.9 About one-third of patients with acute rhinosinusitis have a bacterial cause.10
| Clinical finding | Points |
|---|---|
| C-reactive protein > 1.5 mg per dL (15 mg per L) | 2 |
| Maxillary toothache | 2 |
| Tender maxillary sinus (unilateral) | 2 |
| Purulent nasal discharge | 1 |
| Preceding respiratory tract infection | 1 |
| History of sinusitis | −1 |
| Total (range: −1 to 8): | ____________ |
| Risk group | Likelihood of acute bacterial rhinosinusitis |
| Low (−1 to 3) | 13/80 (16%) |
| Moderate (4 to 6) | 35/71 (49%) |
| High (7 or 8) | 11/15 (73%) |
This clinical prediction rule is limited by the need for a point-of-care CRP measurement, which is unavailable in many primary care practices. In addition, a number of other clinical factors, including double sickening, transillumination, and prolonged symptoms, were not taken into consideration in the study. Although internally validated, the rule should also be externally validated in a different population. Nevertheless, it does help identify the key elements of the history and examination.
In a recent systematic review and meta-analysis, the physician’s overall clinical impression (clinical gestalt) was shown to predict acute bacterial rhinosinusitis.10 Using inspection or culture of antral fluid as a reference standard, clinical gestalt had a positive likelihood ratio (LR+) of 3.9 (95% CI, 2.4 to 5.9) and a negative likelihood ratio (LR–) of 0.33 (95% CI, 0.20 to 0.50) for the diagnosis of acute bacterial rhinosinusitis in adults.10 A further study of patients presenting with sinus symptoms found a 31% prevalence of imaging-confirmed acute bacterial rhinosinusitis. The best predictors of the diagnosis were clinical gestalt (LR+ = 3.8; LR– = 0.34), cacosmia (fetid breath odor; LR+ = 4.3; LR– = 0.86), and teeth pain (LR+ = 2.0; LR– = 0.77).11
Because no clinical prediction rule for acute bacterial rhinosinusitis has been validated and undergone impact analysis, physicians must rely on guidance from existing studies and guidelines. Moreover, because the benefits of antibiotics for acute rhinosinusitis are marginal,5 focusing on treating symptoms or providing a delayed antibiotic prescription may be considered initially if bacterial infection is not suspected. Patients who are more likely to have acute bacterial rhinosinusitis, and thus more likely to benefit from antibiotics, may be those with tender maxillary sinuses, maxillary toothache, a preceding upper respiratory tract infection, cacosmia, or an overall positive physician impression.
Applying the Evidence
A 35-year-old man presents to the primary care clinic with a four-day history of nasal congestion, purulent nasal discharge, and facial pain and pressure that worsen when he bends forward. On examination, he is afebrile, and purulent discharge is visible in his nose and posterior pharynx. He has facial pain with percussion of his sinuses.
Because the role of antibiotics for acute rhinosinusitis is marginal, and the diagnosis of acute bacterial rhinosinusitis is a clinical challenge in primary care, the patient is treated with analgesics and intranasal steroids and given a delayed prescription for an antibiotic to be filled if his symptoms persist or worsen significantly in the next week.
