
Am Fam Physician. 2021;103(1):55-56
Author disclosure: No relevant financial affiliations.
Computed tomography (CT) colonography, or virtual colonoscopy, was developed in the mid-1990s and approved by the U.S. Food and Drug Administration for colorectal cancer screening in 2006.1 Patient preparation for the study typically includes using a bowel cathartic. Following ingestion of oral contrast, insufflation of gas via the rectum, and CT of the abdomen, specialized computer software reconstructs the images to create a two- or three-dimensional image of the colon.
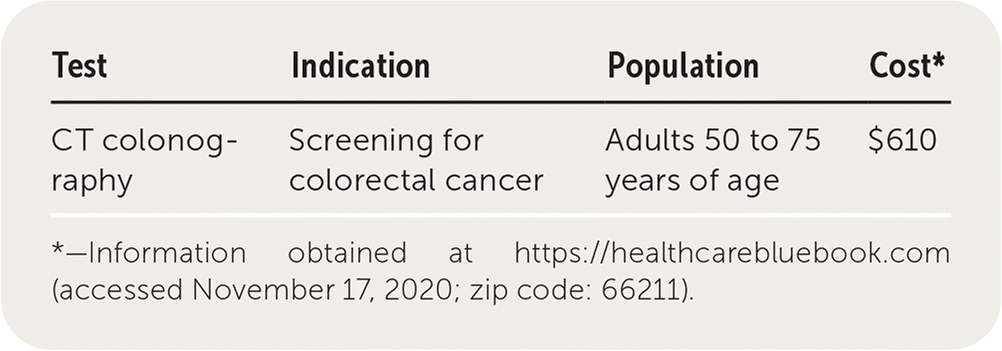
| Test | Indication | Population | Cost* |
|---|---|---|---|
| CT colonography | Screening for colorectal cancer | Adults 50 to 75 years of age | $610 |
Accuracy
Studies of CT colonography have reported a wide range of sensitivities and specificities, possibly because of differences in study design, protocols for reading imaging or test results, radiologist experience, bowel preparation, or fecal tagging (ingestion of oral contrast).
In a meta-analysis including 11,151 patients, the sensitivity of CT colonography for the detection of colorectal cancer was 96.1% (95% CI, 93.8% to 97.7%), which is similar to optical colonoscopy.2 CT colonography is less accurate for detecting polyps. In a subsequent meta-analysis, the sensitivity of CT colonography for the detection of polyps 6 mm or larger was 73% to 98%; specificity ranged from 79.6% to 93.1%.3
Accuracy of CT colonography depends on the experience of the radiologist. To perform and interpret the test, radiologists must have specific initial training that includes at least 50 cases, as well as ongoing certification.1 Overall, improvements to CT colonography over the past two decades have yielded performance similar to optical colonoscopy.1
Reporting of CT colonography results has been standardized by use of the CT Colonography Reporting and Data System (C-RADS): C0 = technically inadequate, C1 = absence of polyps larger than 5 mm, C2 = one or two small polyps (6 mm to 9 mm), C3 = large polyps (10 mm or larger), and C4 = mass lesions (3 cm or larger).
A higher C-RADS category translates to higher risk of advanced neoplasia. Among patients with C2 findings, 5.8% had advanced neoplasia on optical colonoscopy, compared with 67.1% and 79.4% of patients with C3 or C4 findings, respectively.4
Benefit
CT colonography offers important advantages over optical colonoscopy. As with stool testing, CT colonography has essentially no risk of bleeding or perforation, does not require sedation, and does not require interruption of therapeutic anticoagulation. CT colonography takes about 15 minutes to perform and offers more detailed findings (e.g., size, volume, location, and number of polyps) than stool tests, which are only positive or negative.
A potential benefit of CT colonography is visualization of extracolonic structures, providing potentially useful information, such as detection of abdominal aortic aneurysm, osteoporosis, and noncolorectal malignancy. There are no long-term studies of colorectal cancer–specific mortality and all-cause mortality in patients receiving CT colonography compared with other screening methods.
All major cancer prevention, gastroenterologic, and radiologic societies in North America support the use of CT colonography to screen for colorectal cancer.1 In 2016, the U.S. Preventive Services Task Force added CT colonography every five years as an option for colorectal cancer screening in adults 50 to 75 years of age.5 However, it is not recommended for colorectal cancer screening by the American Academy of Family Physicians or guideline panels in any other countries.6,7
Harms
Although the CT colonography procedure itself is safer than optical colonoscopy, important questions exist regarding unintended consequences of extracolonic imaging. Between 5% and 37% of CT colonography examinations identify extracolonic findings that necessitate further diagnostic follow-up.3 This can lead to overdiagnosis and overtreatment of potentially benign and unrelated conditions.
In a study of 52 patients and 50 health care professionals in the United Kingdom, participants were asked to complete a choice experiment to determine tolerability of needing follow-up radiography after a hypothetical false-positive CT colonography. Patients and health care professionals were willing to accept CT colonography false-positive rates of greater than 99.8% and greater than 40%, respectively, in exchange for detection of an additional extracolonic malignancy.8 This suggests that the actual specificity will be acceptable to patients and health care professionals.
The dose of radiation for a single CT colonography test is 7 to 8 mSv. Cumulative doses of ionizing radiation are a consideration, although modeling has shown that serial CT colonography screening every five years would yield a higher net benefit of early cancer detection, with 35 to 47 cancer deaths prevented for every cancer caused, compared with no screening.9 Radiation risk was higher in people screened at a younger age. The model did not compare CT colonography with other colorectal cancer screening modalities.
Cost
CT colonography costs approximately $610, with a range of $488 to $1,525, and is performed every five years if normal.10 If CT colonography shows a clinically significant polyp, the patient must undergo optical colonoscopy for identification and removal. Estimates of cost-effectiveness of CT colonography screening vary widely.
In comparison, optical colonoscopy costs approximately $1,710, with a range of $650 to $6,279, and is performed every 10 years in average-risk individuals if normal.8
The fecal immunochemical test for occult blood costs approximately $8, with a range of $4 to $20 or more, and is performed annually if normal.10 Fecal DNA testing, such as Cologuard, is recommended every one to three years. It is covered by many health insurance companies and Medicare, and costs $509 according to the Centers for Medicare and Medicaid Services' 2020 Clinical Laboratory Fee Schedule.11
If a patient is referred for colonoscopy after a positive result on screening CT colonography or fecal testing, there may be significant out-of-pocket costs for a diagnostic colonoscopy.
The five largest national insurance companies (Aetna, Anthem, Cigna, UniCare, and United Healthcare) have moved toward broad coverage for screening CT colonography.1 However, Medicare does not yet cover the test for screening average-risk patients.
Bottom Line
CT colonography performs well as a colorectal cancer screening test and is more acceptable than optical colonoscopy to some patients. Long-term studies are needed to demonstrate its impact on patient morbidity and mortality and to determine the risks, benefits, and costs of extracolonic imaging in comparison with other screening approaches, in particular fecal immunochemical testing and optical colonoscopy.
