Case Scenario
A 23-year-old patient, M.P., presents to your office with upper respiratory symptoms. When you enter the room, M.P. is using earbuds to listen to music on a personal listening device. The volume is loud enough for you to hear the music but not distinguish details. After addressing the patient's symptoms, you ask about M.P.'s listening habits.
M.P. reports using earbuds to listen to music for two to three hours a day while commuting to work, exercising, or just passing time. M.P. sets the volume loud enough to hear the music over ambient noise. Is M.P. at risk of developing hearing problems, and if so, how should the patient be counseled?
Commentary
Noise-induced hearing loss has long been recognized as a preventable occupational disease, but the extent of nonoccupational noise-induced hearing loss has only recently been acknowledged as a public health problem. Audiometry data collected by the National Health and Nutrition Examination Survey identified noise-induced hearing loss in 24.4% of Americans 20 to 69 years of age.1 More than half (53%) of those reported no significant occupational noise exposure.1 An estimated 19% of American teenagers also have noise-induced hearing loss.2
Noise levels in everyday life can cause hearing loss.3–5 Traffic noise is 80 to 85 decibels (dB), motorcycle noise is 95 dB, a subway train is 100 dB, and a siren is 110 to 129 dB. Personal listening devices at maximum volume can reach approximately 100 to 110 dB.6 The only evidence-based safe noise dose to prevent hearing loss is a daily average of 70 dB.7–9 Noise risk is based on the combination of sound level and duration of exposure. A short, high-volume sound can have the same risk for hearing loss as a longer, lower-level sound if the total sound energy is equivalent. The dB scale is logarithmic. For each 3-dB increase in sound level, the exposure time must be cut in half to maintain the same energy exposure. Therefore, an average 24-hour noise dose of 70 dB is equivalent to eight hours at 75 dB or one hour at 85 dB.
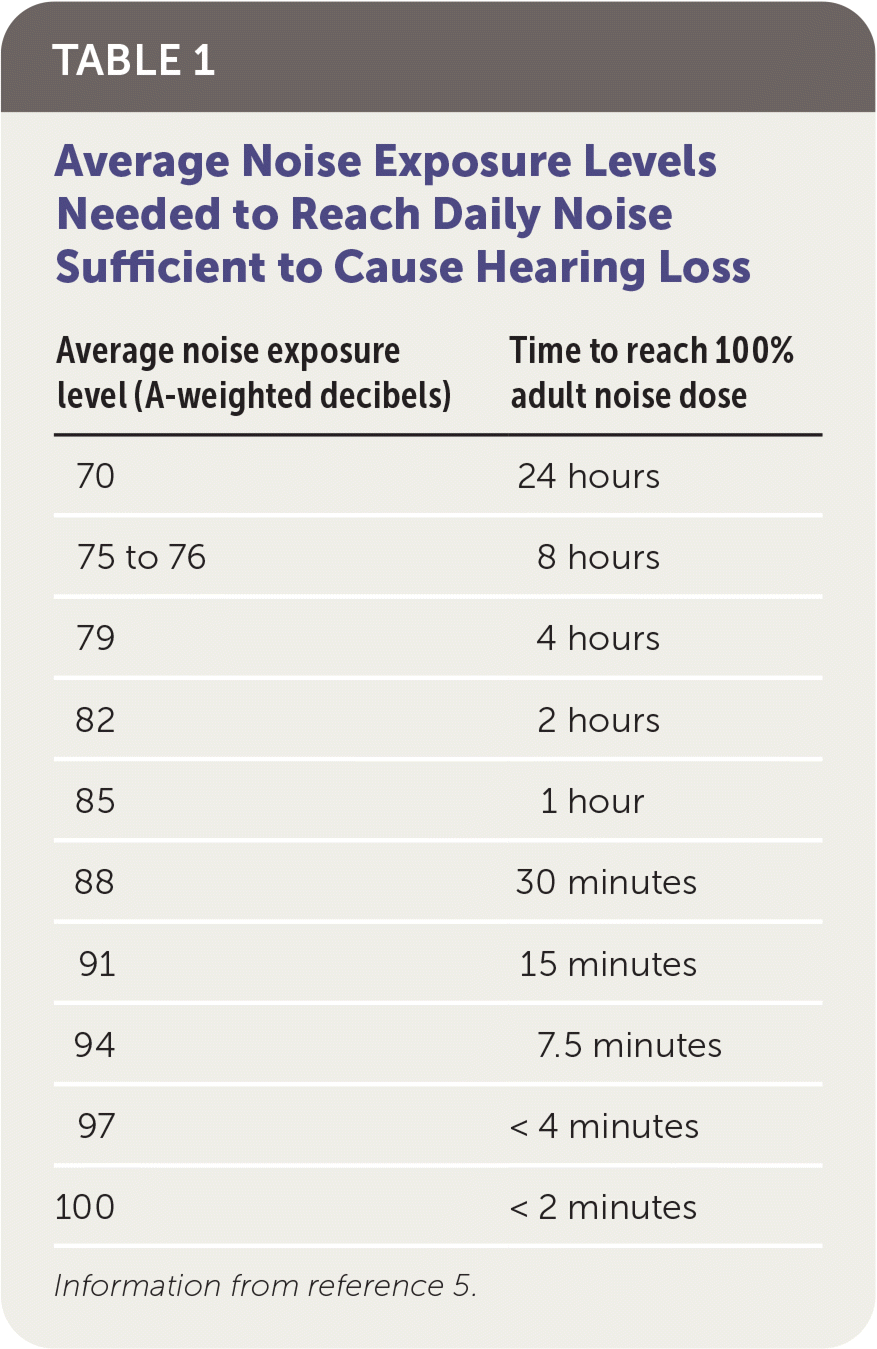
The World Health Organization (WHO) recommends limiting noise exposure to one hour daily at 85 A-weighted dB to prevent hearing loss in adults.10 (A-weighting adjusts noise measurements to mimic the effects of human hearing, which is especially sensitive to frequencies heard in human speech.) Auditory damage can occur after single or very brief exposures to loud noise. Table 1 lists equivalent safe listening times based on the 3-dB exchange rate.5
TABLE 1. Average Noise Exposure Levels Needed to Reach Daily Noise Sufficient to Cause Hearing Loss
| Average noise exposure level (A-weighted decibels) | Time to reach 100% adult noise dose |
|---|---|
| 70 | 24 hours |
| 75 to 76 | 8 hours |
| 79 | 4 hours |
| 82 | 2 hours |
| 85 | 1 hour |
| 88 | 30 minutes |
| 91 | 15 minutes |
| 94 | 7.5 minutes |
| 97 | < 4 minutes |
| 100 | < 2 minutes |
Information from reference 5.
Anecdotally, the average American listens to a personal listening device (e.g., a smart phone) for more than four hours daily, often at high volume.11 High-volume personal listening and unprotected exposure to loud audio material (e.g., music, podcasts) increase the risk of developing permanent noise-induced hearing loss within five to 10 years.
The risk of auditory damage from personal listening devices is likely higher than from ambient noise exposure because earbuds and headphones transmit acoustic energy directly into the external auditory canals. Users of personal listening devices often turn the volume higher than the 50% setting (75 to 80 A-weighted dB or louder) to compensate for ambient noise, especially when using ill-fitting earbuds. Most personal listening devices can produce maximum approximate volumes of 100 to 110 dB, depending on which models are tested.6
Single or repeated noise exposures may cause tinnitus and hyperacusis. These symptoms were believed to be largely reversible, but research now indicates that tinnitus or any muffling of sound denotes permanent auditory damage. Any noise-induced temporary hearing changes increase the risk of developing noise-induced hearing loss.12
Approach to the Patient
After obtaining a medical and family history from the patient, a basic inspection and hearing screening should be conducted in a quiet room. Screening includes finger rub, watch tick, and tuning fork testing; additional testing may be indicated.13 You may also suggest that the patient download the WHO's hearWHO digits-in-noise hearing test app to screen for hearing loss; the app allows users to track their hearing over time.14
Giving advice about noise reduction can be challenging. For younger patients, the immediate pleasurable rewards of listening to audio material at high sound levels often outweigh considerations of potential long-term adverse effects. Additionally, many regard hearing loss as an inevitable part of normal aging. Patients erroneously believe that when they get older, they will probably need hearing aids; however, hearing loss as people age is not inevitable. Usually, the loss represents noise-induced hearing loss. Most hearing loss and related conditions such as tinnitus and hyperacusis can be prevented by avoiding loud noise exposure, starting at a young age.15
The patient should be educated about auditory health. Loud noise exposure is never benign, no matter how brief or occasional. M.P. should be counseled that temporary symptoms of muffled hearing, tinnitus, or hyperacusis indicate increased risk of permanent inner ear and auditory nerve damage. If tinnitus has been experienced, even temporarily—for example after attending a concert—the patient should complete the Tinnitus and Hearing Survey.16 This survey screens for any significant auditory distress in everyday life.
If appropriate, the patient should be told that hearing loss in older adults is strongly correlated with a variety of adverse consequences, including social isolation, depression, falls, accidents, and dementia.13
M.P. should be advised to never use a personal listening device higher than the 50% volume output. Volume-limiting headphones are available, most using the 85-dB volume limit. These are safer than headphones without a volume limit but still do not prevent hearing damage. To enhance satisfactory listening at lower volumes, M.P. should use noise-isolating canal earbuds, noise-canceling headphones, or circumaural headphones to prevent introduction of ambient noise.
Hearing protection should always be used when listening to loud music or when attending activities at venues such as clubs, bars, concerts, or performances. Inexpensive silicone, wax, foam, no-roll foam, or premolded music earplugs are available online or in most stores. Custom-molded high-fidelity earplugs can be obtained from a hearing health care professional.
No cures are available for noise-induced auditory damage, and no medications are approved by the U.S. Food and Drug Administration for tinnitus and hyperacusis; patients with hearing loss can benefit from hearing aids. A variety of evidence-based audiology and psychology treatments for patients with significant distress from tinnitus or hyperacusis are available but do not help all patients and are rarely covered by insurance.17 Patients with significant distress from tinnitus or hyperacusis should be referred to a specialist.
The authors thank David Sykes for his editorial review and helpful comments.

