
Am Fam Physician. 2021;103(4):252-253
Author disclosure: No relevant financial affiliations.
Key Points for Practice
• EAH risk can be reduced by limiting drinking only to respond to thirst with prolonged exertion.
• Because EAH and heat illness symptoms overlap, rectal temperature measurement is critical when assessing altered mental status associated with prolonged exertion.
• Severe EAH is best treated with hypertonic saline boluses. Aggressive cooling can be added if heat illness is also suspected.
• Mild EAH is treated with fluid restriction and oral hypertonic solutions, or salty foods can be added.
From the AFP Editors
Exercise-associated hyponatremia (EAH) occurs when exertion results in sodium concentration less than 135 mEq per L (135 mmol per L), and symptoms can present up to 24 hours after physical activity. When asymptomatic ultramarathon participants are screened, up to one-half demonstrate hyponatremia. The usual cause of EAH is overhydration with hypotonic fluids such as water or sports drinks.
EAH must be differentiated from heat illness to avoid inappropriate treatment and adverse outcomes. Mild EAH symptoms of weakness, malaise, fatigue, irritability, headache, bloating, dizziness, and nausea and vomiting can also occur with heat exhaustion. Severe EAH presents with mental status changes similar to exertional heat stroke. High ambient temperatures increase the risk of EAH as well as heat illness. Injury logs from a national park showed that one in five nonfatal incidents initially characterized as heat-related were due to EAH. The Wilderness Medical Society has published updated guidelines for prevention, diagnosis, and treatment of EAH.
Prevention
EAH prevention centers on avoiding overhydration. No specific fluid volume intake recommendations have been shown to prevent hyponatremia, so the best recommendation is to limit drinking to respond to thirst. Limiting fluid availability during distance events reduces EAH rates.
Although fluids are lost through sweat during exercise, determining fluid replacement based on weight loss during prolonged exercise does not prevent EAH. Changes in antidiuretic hormone (ADH) levels can predispose to EAH, and ADH levels increase with pain, stress, exercise, nausea, and hypoglycemia. Common medications such as nonsteroidal anti-inflammatory drugs and selective serotonin reuptake inhibitors can also increase ADH.
Because EAH is caused by overconsumption of hypotonic oral fluids and inappropriately elevated ADH levels, affected people most often have elevated or normal total body water. Hypovolemic EAH is uncommon and associated with chronic diuretic use and older age.
The increased desire for high-sodium foods after prolonged sweating suggests that salt can be replaced orally. Sodium-rich foods and fluids should be available during lengthy exertion in high temperatures, although they will not prevent EAH when overdrinking occurs.
Assessment
Because EAH symptoms overlap those of heat illness, rapid assessment of rectal temperature is essential when altered mental status is associated with prolonged exertion. Sodium point-of-care testing can be helpful if concomitant EAH is suspected, but availability is limited by high cost and requirement to keep testing kits within specified temperature ranges. If available, point-of-care testing for sodium and glucose is recommended for symptomatic athletes.
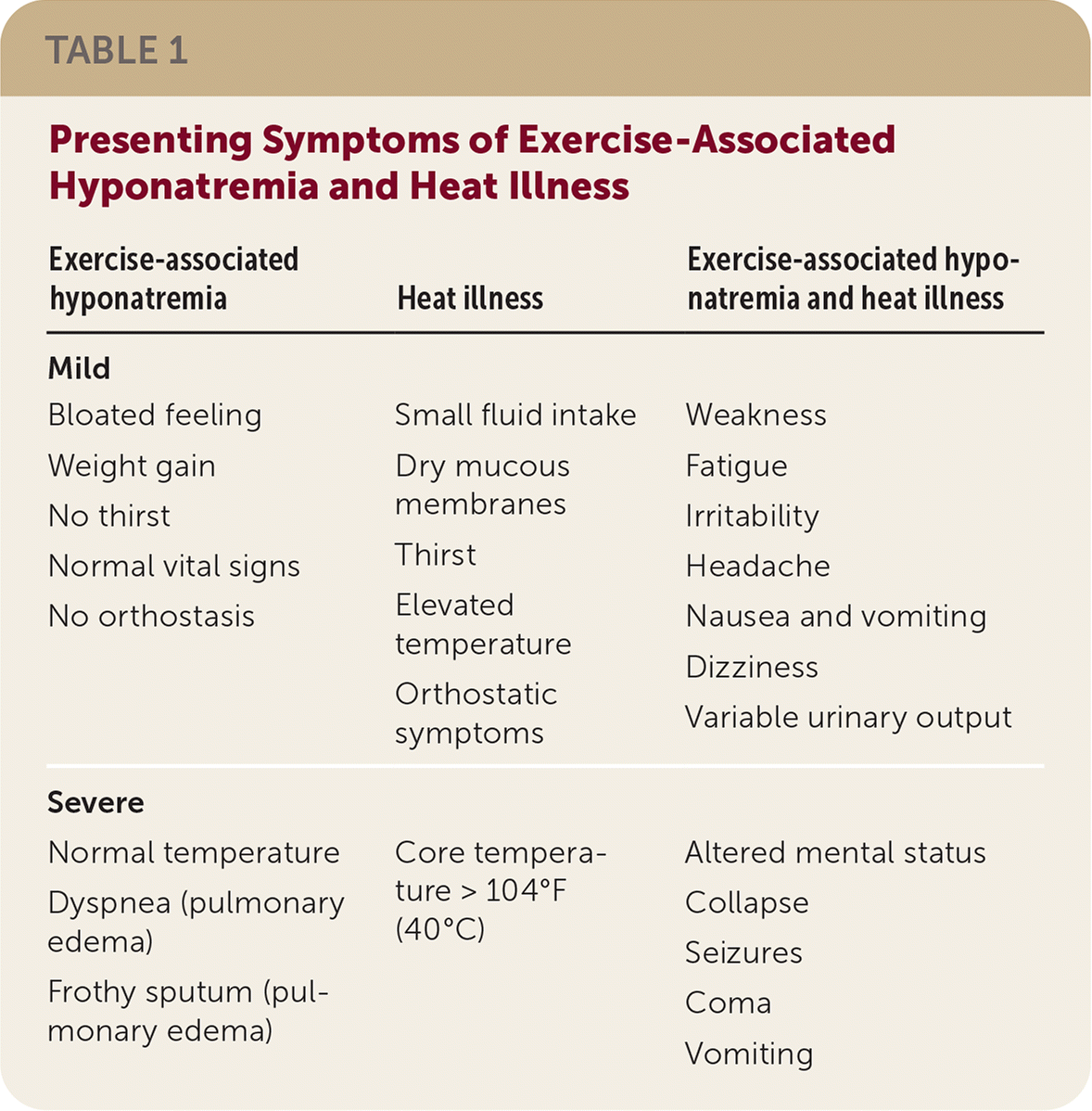
Diagnosis of EAH will most often depend on a history of aggressive hydration and temperatures that are normal or minimally elevated. Overlapping symptoms make clinical assessment challenging (Table 1). Without mental status changes, orthostatic symptoms and thirst can suggest heat illness, whereas bloating and lack of thirst can suggest EAH.
| Exercise-associated hyponatremia | Heat illness | Exercise-associated hyponatremia and heat illness |
|---|---|---|
| Mild | ||
| Bloated feeling Weight gain No thirst Normal vital signs No orthostasis | Small fluid intake Dry mucous membranes Thirst Elevated temperature Orthostatic symptoms | Weakness Fatigue Irritability Headache Nausea and vomiting Dizziness Variable urinary output |
| Severe | ||
| Normal temperature Dyspnea (pulmonary edema) Frothy sputum (pulmonary edema) | Core temperature > 104°F (40°C) | Altered mental status Collapse Seizures Coma Vomiting |
Treating heat illness as EAH can delay critically important rapid cooling, whereas treating EAH as heat illness can worsen hyponatremia through further dilution from fluid boluses. Even after treatment, observation for at least one hour is recommended.
Treatment
EXERTIONAL HEAT STROKE
Exertional heath stroke requires immediate treatment. Altered mental status and temperatures above 104°F (40°C) are emergently treated with aggressive immersive cooling. Additionally, 1-L isotonic fluid boluses with or without glucose can be considered. Worsening symptoms or lack of expected improvement can suggest concomitant severe EAH.
SEVERE EAH
Severe EAH should be assumed when mental status changes are noted with normal or minimally elevated rectal temperatures. Severe EAH should be rapidly treated with 100-mL intravenous boluses of hypertonic saline, which may be repeated every 10 minutes for three total boluses. These doses increase serum sodium by up to 2 mEq per L and do not increase risk of osmotic demyelination.
If heat illness is suspected with EAH or the diagnosis is uncertain, hypertonic saline boluses can be combined with rapid cooling. Hypotonic fluids should be avoided in EAH to prevent pulmonary edema.
Further hypertonic saline treatment can be considered if necessary. Large hypertonic saline volumes have been used without adverse effects, including 600 mL over one hour and 950 mL over seven hours.
MILD EAH
Mild EAH often manifests as bloating, weight gain, and lack of orthostasis. Fluid restriction is the primary treatment until significant diuresis occurs. External cooling can be added, and intravenous hypotonic or isotonic fluid should be avoided.
In mild EAH, salt can be replaced through oral hypertonic solutions such as three to four bouillon cubes or three ramen seasoning packets per 125 mL of water, or by consumption of salty foods. Intravenous hypertonic saline may be used if anti-emetics are ineffective in enabling oral intake.
MILD HEAT ILLNESS
With elevated temperatures below 104°F and orthostatic symptoms and thirst, mild heat illness should be treated. Initial treatment is external cooling and monitoring. Fluid consumption can be allowed for comfort if EAH is not suspected.
Coordination with Hospital Care
Communication between prehospital and hospital care is essential for EAH and heat illness. Assessment of clinical signs and relaying details on the amount and type of fluids given are particularly important. In stable patients, further treatments will likely depend on laboratory results.
Editor's Note: Although a previous AFP article (https://www.aafp.org/afp/2007/0715/p237.html) suggested a specific limit to hydration during endurance activities, the Wilderness Medical Society notes that no fluid recommendations have been shown to reduce EAH and recommends drinking in response to thirst. This guideline highlights the difficulty and importance of differentiating EAH from heat illness because treatments for one can worsen the other.—Michael J. Arnold, MD, Contributing Editor
The views expressed in this article are those of the authors and do not necessarily reflect the official policy or position of the Department of the Navy, Department of the Air Force, Uniformed Services University of the Health Sciences, Department of Defense, Air Force Medical Corps or Surgeon General, or any U.S. government official or office.
Guideline source: Wilderness Medical Society
Evidence rating system used? Yes
Systematic literature search described? Yes
Guideline developed by participants without relevant financial ties to industry? Yes
Recommendations based on patient-oriented outcomes? Yes
Published source: Wilderness Environ Med. March 2020;31(1):50–62
