
Am Fam Physician. 2021;103(6):375-376
Author disclosure: No relevant financial affiliations.
Clinical Question
Which adults presenting to the emergency department with syncope should be admitted?
Evidence Summary
Syncope accounts for almost 1% of all emergency department visits.1 Although only approximately 10% of patients presenting with syncope have a serious underlying cardiac condition, nearly one-third are admitted to the hospital.1 Several clinical prediction rules have been developed to help physicians identify patients with syncope who are at higher risk of adverse outcomes and those for whom discharge without hospitalization may be reasonable.
The San Francisco Syncope Rule was originally derived from a cohort of 684 patients and consists of five risk factors: abnormal findings on an electrocardiogram, hematocrit less than 30%, history of congestive heart failure, reported shortness of breath, and systolic blood pressure less than 90 mm Hg. If any of these risk factors are present, the patient is considered at high risk of a serious outcome. A meta-analysis of 12 validation studies with 5,316 patients found that for predicting serious outcomes in those classified as high risk, the San Francisco Syncope Rule has a sensitivity of 87% (95% CI, 79% to 93%), specificity of 52% (95% CI, 43% to 62%), positive likelihood ratio of 1.8 (95% CI, 1.7 to 1.9), and negative likelihood ratio of 0.25 (95% CI, 0.20 to 0.31).2
The ROSE (risk stratification of syncope in the emergency department) rule was derived from a cohort of 529 patients and prospectively validated in a cohort of 550 patients. It consists of six risk factors: brain natriuretic peptide of 300 pg per mL (300 ng per L) or greater, hemoglobin level of 9 g per dL (90 g per L) or less, bradycardia, chest pain, abnormal electrocardiogram finding (bradycardia of 50 beats per minute or less or Q wave present in a lead other than lead III), oxygen saturation of 94% or less, and the presence of fecal occult blood. Admission is recommended if any of these risk factors are present. The ROSE rule has a sensitivity of 87% (95% CI, 73% to 96%), specificity of 66% (95% CI, 61% to 70%), positive likelihood ratio of 2.5 (95% CI, 2.1 to 3.0), and a negative likelihood ratio of 0.20 (95% CI, 0.09 to 0.45).3
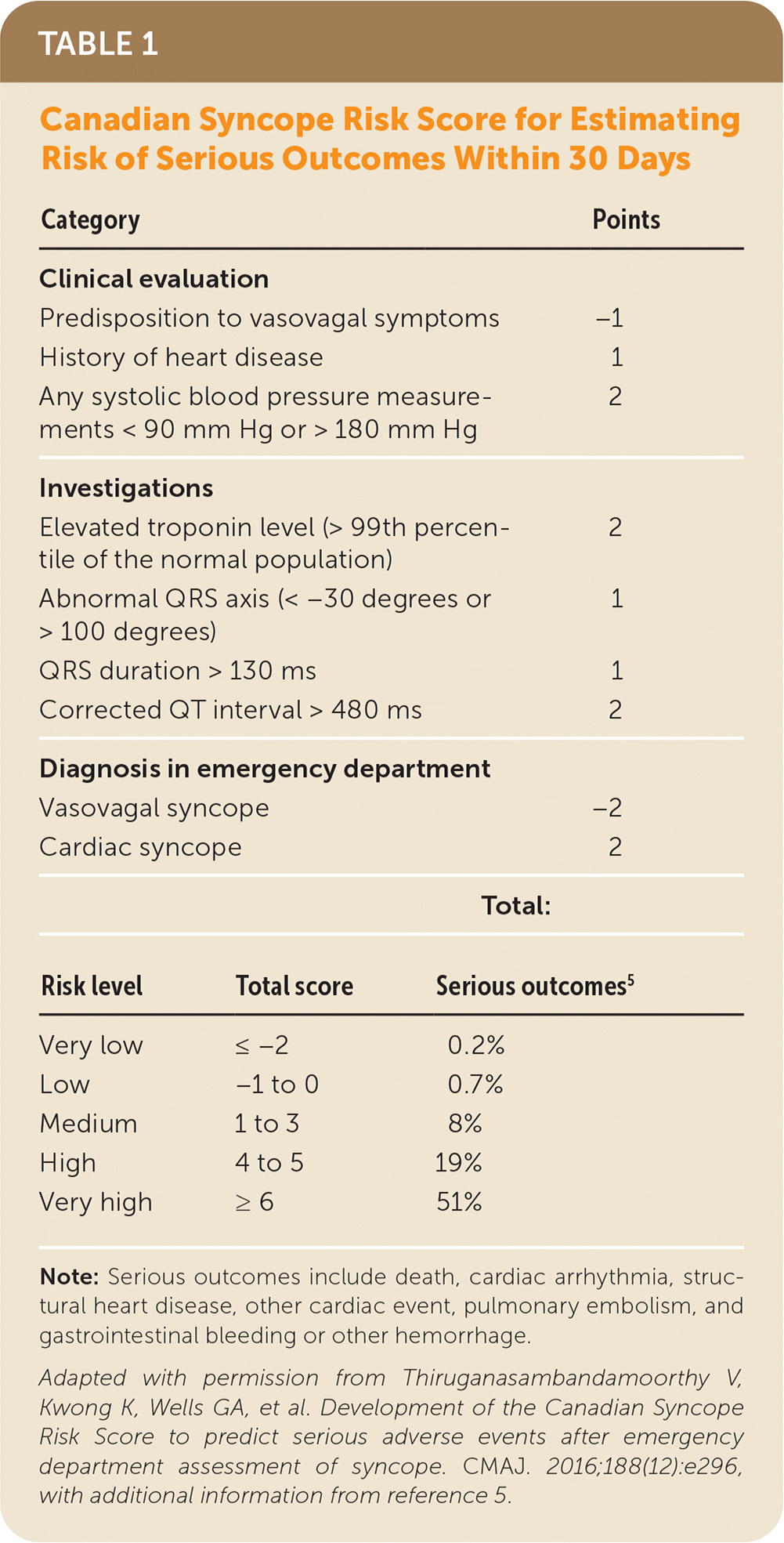
The Canadian Syncope Risk Score (Table 14,5 ) was initially derived from a prospective multi-center study involving six large Canadian academic emergency departments and 4,030 adult patients.4 Patients were excluded if they had immediate postsyncopal complications (prolonged loss of consciousness, altered mental status, seizure, or major trauma), a language barrier affecting the ability to obtain a detailed history, or a serious outcome identified during the initial emergency department visit. Patients were followed for 30 days to assess for serious outcomes. The Canadian Syncope Risk Score includes patient history, electrocardiogram findings, clinical impression, and troponin testing. The probability of a serious outcome was estimated at less than 1% in the low-risk and very low-risk groups and more than 12% in the high-risk and very high-risk groups.4
| Category | Points | |
|---|---|---|
| Clinical evaluation | ||
| Predisposition to vasovagal symptoms | −1 | |
| History of heart disease | 1 | |
| Any systolic blood pressure measurements < 90 mm Hg or > 180 mm Hg | 2 | |
| Investigations | ||
| Elevated troponin level (> 99th percentile of the normal population) | 2 | |
| Abnormal QRS axis (< −30 degrees or > 100 degrees) | 1 | |
| QRS duration > 130 ms | 1 | |
| Corrected QT interval > 480 ms | 2 | |
| Diagnosis in emergency department | ||
| Vasovagal syncope | −2 | |
| Cardiac syncope | 2 | |
| Total: | ||
| Risk level | Total score | Serious outcomes5 |
| Very low | ≤ −2 | 0.2% |
| Low | −1 to 0 | 0.7% |
| Medium | 1 to 3 | 8% |
| High | 4 to 5 | 19% |
| Very high | 6 | 51% |
The Canadian Syncope Risk Score was externally validated in a prospective cohort of 3,819 adults at nine Canadian emergency departments from 2014 to 2018. The area under the curve for the model was 0.91 (95% CI, 0.88 to 0.93), indicating high predictive ability.5 The prevalence of serious outcomes within 30 days was 3.6% (95% CI, 3.1% to 4.3%). Only 0.2% of patients at very low risk and 0.7% of patients at low risk had a serious outcome, compared with 51% of patients at very high risk. No patients in the low-risk or very low-risk groups died or experienced a ventricular arrhythmia, and fewer than 1% experienced a serious adverse outcome, suggesting that patients in these risk groups can be safely discharged from the emergency department without inpatient admission.5
Applying the Evidence
A 32-year-old adult presents to the emergency department after passing out while doing yardwork. The episode lasted roughly 30 seconds and was witnessed by the patient's spouse. No seizure activity or postictal symptoms are reported. The patient has no significant medical history, although the patient reported passing out once before after standing in formation too long during military service.
While in the emergency department, the patient's blood pressure measurements ranged from 115 to 128 mm Hg systolic and 67 to 78 mm Hg diastolic, and electrocardiogram findings are normal other than a corrected QT interval of 492 ms. Laboratory workup is unremarkable, including a normal troponin level. The working diagnosis is vasovagal syncope, but the patient's prolonged QT interval is concerning.
Using the Canadian Syncope Risk Score, the patient receives −1 total points (−1 for predisposition to vasovagal symptoms, 2 for corrected QT interval greater than 480 ms, and −2 for diagnosis of vasovagal syncope). This puts the patient in the low-risk category, with a less than 1% chance of a serious outcome occurring within the next 30 days. You discharge the patient home with appropriate outpatient follow-up.5
Editor's Note: Dr. Saguil is contributing editor for AFP.
The opinions and assertions contained herein are the private views of the authors and are not to be construed as official or as reflecting the views of the Uniformed Services University of the Health Sciences or the Department of the Army.
