
Am Fam Physician. 2021;103(8):503-504
Author disclosure: No relevant financial affiliations.
An 80-year-old patient presented to the emergency department in October 2020 with several days of increasing shortness of breath. Three days before that, the patient went to urgent care because of intermittent fevers up to 103°F (39.4°C) and a dry cough. The patient went to the emergency department after the symptoms continued to worsen. The medical history included atrial fibrillation, hypertension, and hyperlipidemia. The patient lived independently at home and had never smoked cigarettes.
On examination, the patient's vital signs included a pulse rate of 113 beats per minute, respiratory rate of 26 breaths per minute, and temperature of 100.8°F (38.2°C). The patient required 5 L of oxygen via nasal cannula to maintain an oxygen saturation of 96%. Lung auscultation revealed diffuse rales bilaterally.
Relevant laboratory results included a white blood cell count of 13,000 per μL (13.0 × 109 per L) with 48% lymphocytes. A chest radiograph demonstrated moderate multifocal, bilateral, patchy airspace and interstitial opacities (Figure 1).
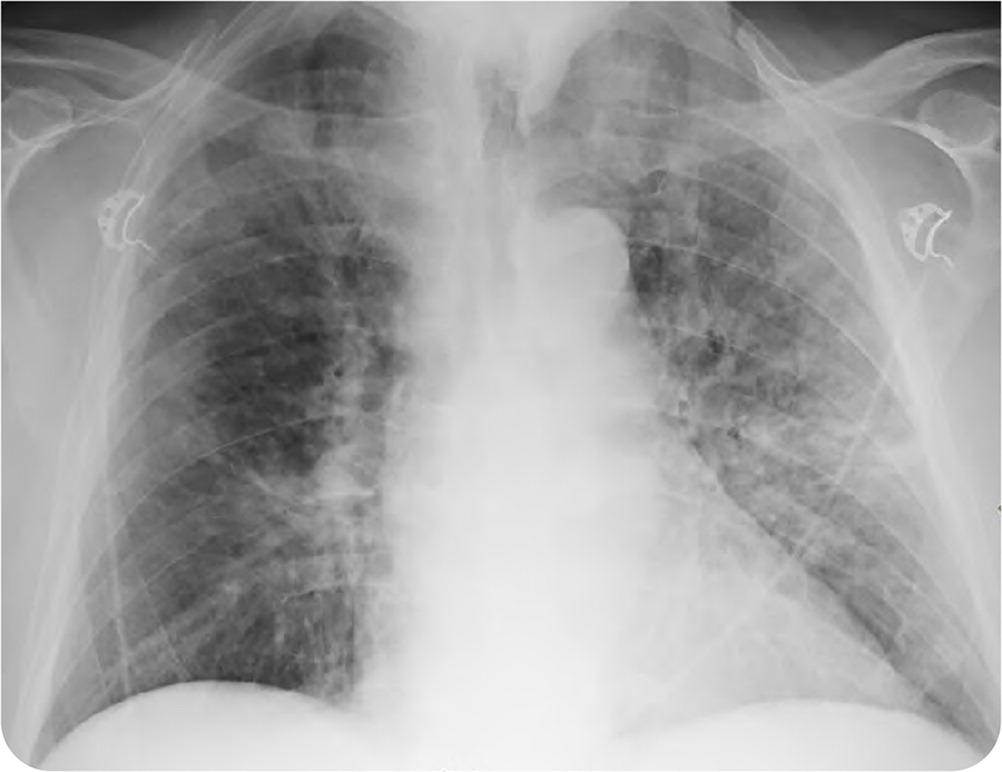
Question
Based on the patient's history, physical examination, laboratory, and imaging findings, which one of the following is the most likely diagnosis?
A. Aspiration pneumonia.
B. Congestive heart failure.
C. COVID-19 interstitial pneumonia.
D. Mycoplasma pneumonia.
Discussion
The answer is C: COVID-19 interstitial pneumonia, a novel acute respiratory illness caused by SARS-CoV-2 infection. Many patients with acute COVID-19 present with respiratory symptoms, including dry cough, shortness of breath, tachypnea, and hypoxemia. Pneumonia and acute respiratory failure can develop in the 5% to 10% of patients with severe disease.1 Patients with COVID-19 typically follow a biphasic disease course, with a milder initial presentation that is followed by clinical deterioration about seven to 10 days after the onset of symptoms.1 Imaging findings include bilateral ground-glass opacities, and subsegmental and lobar areas of consolidation.2
The patient's nasal swab test was positive for COVID-19 at the urgent care clinic three days before the patient presented to the emergency department. Polymerase chain reaction testing is most useful for the initial diagnosis of COVID-19. Treatment is generally supportive with oxygen, antiviral therapy, and intravenous fluids. Patients who require mechanical ventilation and dialysis have a much poorer prognosis. Bacterial pneumonia typically presents with a focal or lobar consolidation on chest radiography. Other viral causes of pneumonia can present with similar interstitial infiltrates, which makes polymerase chain reaction testing for common viruses, such as influenza A and B, important when diagnosing COVID-19.
Aspiration pneumonia is caused by the inhalation of foreign particles into the lungs. Certain populations are at greater risk of this disease, including older people and those with dysphagia or impaired neurologic status (e.g., due to stroke or alcohol or drug use). Radiographs show opacification of the posterior segment of the upper lobes and the superior segment of the lower lobes. Because of the more obtusely angled right bronchus, the right lower lobe is most often involved with aspiration, but the position of the patient during the aspiration event leads to bilateral involvement in 50% of cases.3 The low specificity of diagnostic radiography in aspiration pneumonia can be improved with computed tomography.3
Mycoplasma pneumonia typically presents with mild symptoms, including fever, cough, wheezing, and dyspnea. Chest radiography may show airspace opacities, reticular opacities, and bronchial thickening. Computed tomography findings are similar to radiography, but in more detail, and can include interstitial thickening and centrilobular nodules.5
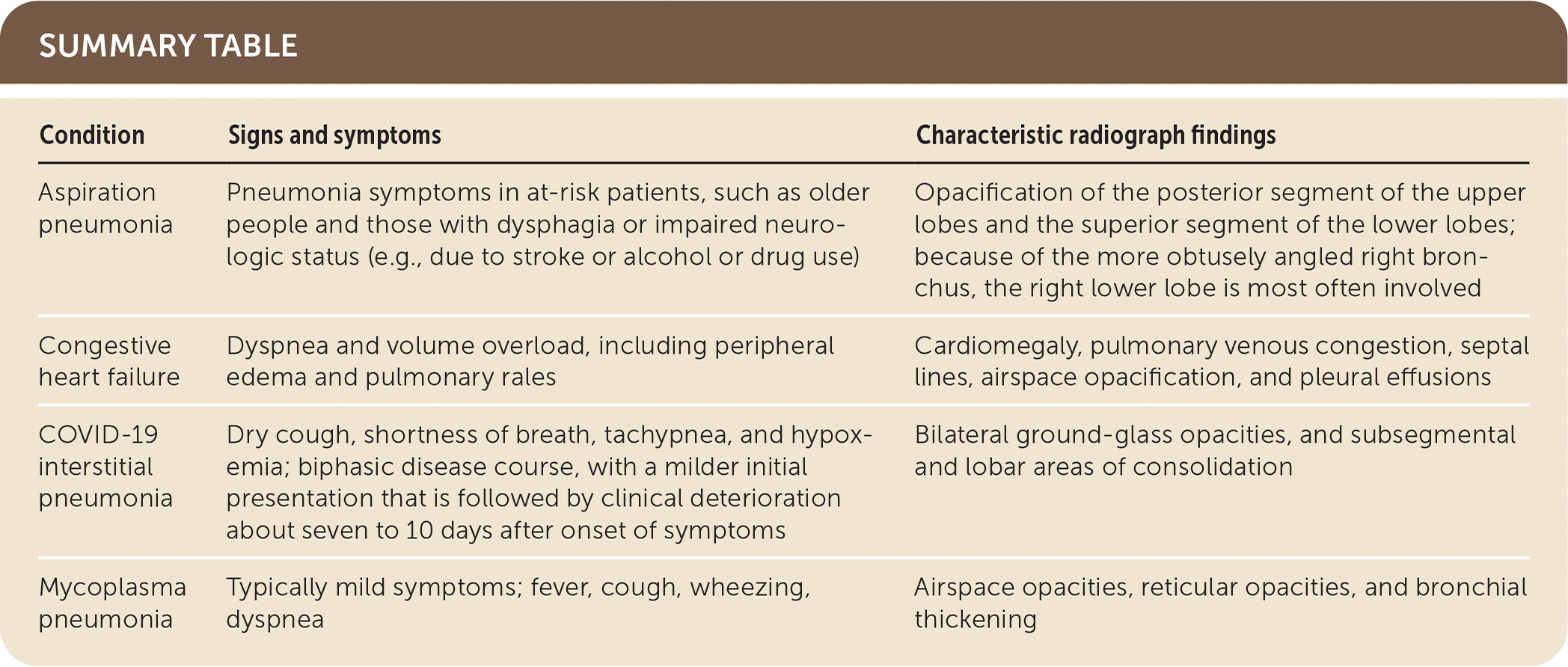
| Condition | Signs and symptoms | Characteristic radiograph findings |
|---|---|---|
| Aspiration pneumonia | Pneumonia symptoms in at-risk patients, such as older people and those with dysphagia or impaired neurologic status (e.g., due to stroke or alcohol or drug use) | Opacification of the posterior segment of the upper lobes and the superior segment of the lower lobes; because of the more obtusely angled right bronchus, the right lower lobe is most often involved |
| Congestive heart failure | Dyspnea and volume overload, including peripheral edema and pulmonary rales | Cardiomegaly, pulmonary venous congestion, septal lines, airspace opacification, and pleural effusions |
| COVID-19 interstitial pneumonia | Dry cough, shortness of breath, tachypnea, and hypoxemia; biphasic disease course, with a milder initial presentation that is followed by clinical deterioration about seven to 10 days after onset of symptoms | Bilateral ground-glass opacities, and subsegmental and lobar areas of consolidation |
| Mycoplasma pneumonia | Typically mild symptoms; fever, cough, wheezing, dyspnea | Airspace opacities, reticular opacities, and bronchial thickening |
