
Am Fam Physician. 2021;103(11):672-679
Related editorial: Promoting Safety in Community-Based Birth Settings
Patient information: See related handout on having a baby outside of a hospital, written by the authors of this article.
Author disclosure: No relevant financial affiliations.
Since the 1970s, most births in the United States have been planned to occur in a hospital. However, a small percentage of Americans choose to give birth outside of a hospital. The number of out-of-hospital births has increased, with one in every 61 U.S. births (1.64%) occurring out of the hospital in 2018. Out-of-hospital (or community) birth can be planned or unplanned. Of those that are planned, most occur at home and are assisted by midwives. Patients who choose a planned community birth do so for multiple reasons. International observational studies that demonstrate comparable outcomes between planned out-of-hospital and planned hospital birth may not be generalizable to the United States. Most U.S. studies have found statistically significant increases in perinatal mortality and neonatal morbidity for home birth compared with hospital birth. Conversely, planned community birth is associated with decreased odds of obstetric interventions, including cesarean delivery. Perinatal outcomes for community birth may be improved with appropriate selection of low-risk, vertex, singleton, term pregnancies in patients who have not had a previous cesarean delivery. A qualified, licensed maternal and newborn health professional who is integrated into a maternity health care system should attend all planned community births. Family physicians are uniquely poised to provide counseling to patients and their families about the risks and benefits associated with community birth, and they may be the first physicians to evaluate and treat newborns delivered outside of a hospital.
Although uncommon, planned out-of-hospital births are becoming increasingly popular in the United States. From 2004 to 2017, the number of out-of-hospital births in the United States increased by 75%.1 In 2018, out-of-hospital births represented 1.64% of all births, which translates to one in every 61 newborns being delivered in a location other than a hospital.2 Although small in magnitude, this is a reversal of the trend that occurred during the 20th century in which the frequency of hospital births rose from 37% in 1935 to more than 99% by 1970, where it remained essentially unchanged until 2004.3
Out-of-hospital birth, often referred to as community birth, can be planned or unplanned. Of those that are planned, the most commonly chosen location is the home; 62% of out-of-hospital births were at home in 2018.1,2 Deliveries at free-standing birth centers have also increased and made up roughly one-third of community births in 2018.2 Most maternal and newborn health professionals who attend planned out-of-hospital births in the United States are midwives.2,4 In 2018, only 4.2% of out-of-hospital births were attended by physicians.2
Given their unique role spanning care provided by midwives, obstetricians, and pediatricians, family physicians can provide trusted guidance to patients and families who express an interest in out-of-hospital birth.
Patient Selection
Patients inquiring about community birth should be counseled that an appropriate candidate should have a low-risk pregnancy (Table 15–8) that is at term with a single fetus in vertex presentation and should have no previous cesarean delivery.9 Planned hospital birth is strongly recommended for patients with conditions that increase the risk of maternal or neonatal adverse outcomes, including nulliparity and gestational age of 41 weeks or more4,10,11 (Table 29,12–14). Planned community birth should be attempted only in the presence of a maternal and newborn health professional who meets or exceeds the International Confederation of Midwives Global Standards for Midwifery Education, working within an integrated, regulated maternity care system with the ability to consult and transfer to a higher level of care in a timely manner if necessary.9,13–16

| American College of Obstetricians and Gynecologists Low risk: A clinical scenario lacking clear demonstrable benefit for medical intervention. What constitutes low risk will vary depending on individual circumstances and the proposed intervention.5 |
| Eunice Kennedy Shriver National Institute of Child Health and Human Development Low risk: No maternal or fetal indication for delivery before 40 5/7 weeks.6 High risk: The mother, fetus, or both are at higher risk for health problems during pregnancy or labor vs. a typical pregnancy.7 |
| Society for Maternal-Fetal Medicine Low risk: All term, singleton, vertex, live birth deliveries without previous cesarean delivery or high-risk diagnoses.8 |

| Preexisting medical conditions Any significant medical condition that could impact childbirth, including: Asthma requiring hospitalization Bleeding disorder Confirmed cardiac disease Diabetes mellitus Hepatic disease Hypertensive disorders Hyperthyroidism Orthopedic condition limiting vaginal delivery Renal disease Seizure disorder Systemic lupus erythematosus Thromboembolic disorder Evidence of active infection with hepatitis, HIV, herpes simplex virus, syphilis, or tuberculosis Maternal age of 35 years or older Psychiatric conditions requiring inpatient care Substance abuse or dependence Previous obstetric conditions Cesarean delivery or uterine surgery Intrauterine fetal death or stillbirth Postpartum hemorrhage Preeclampsia with preterm birth or eclampsia Retained placenta requiring manual removal Shoulder dystocia Current obstetric conditions Any condition necessitating pharmacologic induction of labor Evidence of fetal congenital anomaly Gestational age of 41 weeks or more Gestational diabetes Gestational hypertension Intrauterine growth restriction Malpresentation Multiple gestation Oligohydramnios Placenta accreta, increta, or percreta Placenta previa Placental abruption Polyhydramnios Preeclampsia Prepregnancy body mass index greater than 35 kg per m2 Preterm labor Prolonged rupture of membranes without active labor Rh isoimmunization Significant anemia |
Issues of Safety
Establishing the safety of community birth is difficult primarily because the concept of safety in relation to birth setting is variable depending on the perception of risk by patients, their families, and the various maternal and newborn health professionals. This is reflected by the differences in position statements regarding the best practices for place of birth for low-risk pregnancies among the organizations that represent maternal and newborn health professionals (Table 39,13–15,17,18). Choice of birth setting may be influenced by health, pregnancy status, family needs, and religious or cultural values. Patients may perceive that, compared with hospital birth, out-of-hospital birth is safer for any of the reasons listed in Table 4.19–24 Furthermore, several studies substantiate comparable outcomes for out-of-hospital birth in low-risk pregnancies attended by midwives.4,12,25–27

| American Academy of Pediatrics13 Hospitals and accredited birth centers are safest for birth in the United States Planned home birth not recommended; however, the organization recognizes that patients may choose home birth At least two medical attendants should be present, with one whose primary responsibility is care of the newborn American College of Nurse-Midwives14,15 Safety of birth in any setting is a primary concern Midwives who provide care independently in the home for healthy patients during pregnancy, labor, and birth should do so within parameters of setting-specific clinical practice guidelines Safety of home birth is optimized by: Assessing appropriateness of the patient and family for planned home birth Attendance by a qualified maternal and newborn health professional Practice within integrated systems that support collaborative care American College of Obstetricians and Gynecologists9 Hospitals and accredited birth centers are safest for birth Each patient has the right to make a medically informed decision about delivery Patients inquiring about planned home birth should be informed of the risks and benefits, including: Planned home birth is associated with more than two-fold increased risk of perinatal death (one to two per 1,000 births) and threefold increased risk of neonatal seizures or serious neurologic dysfunction (0.4 to 0.6 per 1,000 births) compared with hospital births Planned home birth is associated with fewer maternal interventions than planned hospital birth Factors critical to reducing perinatal mortality include: Access to consultation Access to safe and timely transport to nearby hospitals Appropriate selection of candidates for home birth Availability of a physician, certified nurse midwife, certified midwife, or midwife whose education and licensure meet International Confederation of Midwives Global Standards for Midwifery Education, practicing obstetrics within an integrated and regulated health system Absolute contraindications to home birth include: Fetal malpresentation Multiple gestation Previous cesarean delivery Association of Women's Health, Obstetric and Neonatal Nurses17 Patients have the right to choose and have access to the full range of maternal newborn health professionals and settings for pregnancy and birth, including hospital, freestanding birth center, or home Clinicians should respect a patient's choice of birth setting and birth attendant Midwives Alliance of North America18 Home birth is safe for healthy patients with a skilled midwife present and timely access to medical care when needed Each birth setting carries a particular set of risks and benefits Each patient must evaluate and decide which set of risks and benefits is most acceptable and in keeping with belief system and family's best interests “There is no significant statistical difference in outcome in terms of maternal or perinatal mortality between hospital and out-of-hospital birth; however, there is increased morbidity in the hospital.” |

| Avoidance of unnecessary interventions |
| Better outcomes |
| Better personal relationship with delivering individual |
| Desire to not repeat previous negative experience |
| Empowering |
| Freedom to eat and drink ad lib |
| Freedom to move around |
| Greater comfort |
| Innate trust in the birthing process |
| Limit medicalization of and interference with birthing process |
| Maintain autonomy and control |
| Mistrust of conventional medicine |
| Negative feelings associated with doctors or hospitals |
| No access or limited access to maternity care |
| Only option available for vaginal birth after cesarean delivery |
| Optimal environment to promote physiologic birth |
| Peaceful, calming environment |
| Safer environment |
| Undisturbed birth experience |
Hospital-based maternity care is often criticized for its high reliance on technology and the medicalization of birth. Patients who choose community birth cite the desire to avoid unnecessary interventions as one of the reasons that they perceive out-of-hospital birth to be safer than planned hospital birth.19 The American College of Obstetricians and Gynecologists (ACOG) acknowledges that “many common obstetric practices are of limited or uncertain benefit for low-risk women in spontaneous labor.”5 The high rates of cesarean delivery in U.S. hospitals are also concerning.19–21,23,24 In contrast, the paradigm for care in midwifery is based on the premise that minimal or no intervention facilitates a patient's natural ability to deliver vaginally.28
Compared with planned hospital birth, community birth in the United States is associated with an increased risk of neonatal death, neonatal seizures, and low Apgar scores.3,10,29,30 Although the absolute difference in risk is small, with an excess of about one death per 1,000 planned out-of-hospital deliveries, these events are catastrophic. Conversely, planned community birth is associated with decreased odds of obstetric interventions, increased odds of unassisted vaginal births, and lower cesarean delivery rates.9,25,29,31–35
Public health issues can influence the safety assessment of various birth settings. During pandemics, such as COVID-19, more patients may consider alternatives to hospital birth.36 Reasons include the desire to limit potential exposure to disease, concern for lack of available resources as hospitals plan for overwhelming numbers of sick patients, or fear of giving birth alone because of hospital restrictions limiting the presence of family or support.37 ACOG, the American Academy of Family Physicians, the American College of Nurse-Midwives, and the Society for Maternal-Fetal Medicine released a joint statement in March 2020 (available at https://s3.amazonaws.com/cdn.smfm.org/media/2279/homebirth.pdf) on the care of pregnant patients during a pandemic, reassuring the public that hospitals and licensed, accredited birth centers remain safe places to give birth.
Geographic access issues can also impact perceived safety. As of 2018, more than 1,000 U.S. counties with more than 5 million people have no obstetric physicians or hospitals.38 In counties that have lost hospital-based obstetric services, the frequency of out-of-hospital birth has increased.39 People who reside in these “maternity care deserts” may have no choice, or they may choose community birth to avoid long commutes, scheduled deliveries, and separation from family or other support during delivery.
Patients with higher risk pregnancies who strongly desire vaginal birth may be willing to accept the risks associated with out-of-hospital birth rather than choose a planned hospital birth with a higher probability of a cesarean delivery. ACOG considers fetal malpresentation, multiple gestation, and previous cesarean delivery to be absolute contraindications to home birth.9 Neonatal death has been reported to be as high as one in 78 for breech home deliveries. Among newborns delivered via vaginal birth after cesarean (VBAC), those born at home are eight times more likely to have seizures than those born in the hospital.10,40 In nulliparous patients and those at 41 weeks' or more gestation, home birth is associated with higher risk of neonatal mortality compared with planned hospital birth.10,30
As many as one-third of midwife-attended home births have conditions that are not considered low risk according to ACOG and the American Academy of Pediatrics.41 For instance, patients who desire a trial of labor after cesarean (TOLAC) often have limited availability of hospitals or physicians willing to support this option. A 2012 survey of California hospitals found that 43% did not allow TOLAC, and those that did had few physicians willing to manage a patient who wants a TOLAC.42 Fewer than one in 10 patients with a previous cesarean birth will deliver vaginally.40 Most of these occur in a hospital; however, from 2007 to 2010 the proportion of out-of-hospital VBAC births increased from 1.78% to 2.45%.40
Studies of Community Birth
Comparing neonatal or maternal outcomes by birth setting is challenging. A Cochrane review identified only one randomized controlled trial of planned home birth, which enrolled just 11 participants and was too small to provide meaningful conclusions.16 To date, nearly all studies have been observational and have focused primarily on perinatal or neonatal morbidity and mortality 3,4,10–12,29,30,40,41,43,44 (eTable A). Maternal mortality is uncommon, and no U.S. studies have been able to evaluate differences in relation to birth setting. Several international studies have reported no significant differences in outcomes in planned out-of-hospital birth for low-risk patients attended by midwives compared with planned hospital birth.11,32,33,45–47 However, the data for these studies come from countries that have specific eligibility criteria for home birth as well as consistent standards for midwifery practice, neither of which exists in the United States. Consequently, these findings may not be generalizable to the U.S. population.
| Author (year) | Data source and outcome measures | Study size | Key findings | Conclusion |
|---|---|---|---|---|
| Bachilova (2018)A1 | Vital statistics 2011 to 2013 Identification of risk factors associated with neonatal death in planned home births | 71,704 planned and delivered home births | Early neonatal deaths were higher in nulliparous births (OR = 2.71), previous cesarean delivery (OR = 2.62), malpresentation (OR = 4.27), plural births (OR = 9.79), preterm births (OR = 4.68), and gestational age of 41 weeks or more (OR = 1.76) | Nulliparity, a previous cesarean delivery, nonvertex presentation, multifetal gestation, preterm birth, and birth at 41 weeks' or more gestation are risk factors for early neonatal death in planned home birth |
| Cheng (2013)A2 | Vital statistics 2008 Outcomes associated with planned home births compared with hospital births | 2,081,753 births, of which 12,039 were planned home births | AORs for five-minute Apgar score less than 4 and neonatal seizures for planned home vs. hospital birth were 1.87 and 3.08, respectively Patients with planned home births had fewer interventions | Planned home birth is associated with increased neonatal complications but fewer obstetric interventions |
| Cheyney (2014)A3 | Birth registry 2004 to 2009 Descriptive statistics for outcomes of planned home birth | 16,924 planned home births recorded in a voluntary, self-reported data set | Intrapartum plus neonatal death rate was 2.06 per 1,000 planned home births Breech presentation, nulliparity, and previous cesarean delivery conferred increased risk | Low-risk patients planning home births experience high rates of physiologic birth and low rates of intervention |
| Grünebaum (2013)A4 | Vital statistics 2007 to 2010 Five-minute Apgar score of 0 Neonatal seizures or serious neurologic dysfunction | 12,891,274 hospital physician deliveries 1,118,578 hospital midwife deliveries 42,216 freestanding birth center deliveries 67,429 home birth midwife deliveries | Home births and birth center births attended by midwives had higher risk of five-minute Apgar score of 0, neonatal seizures, or serious neurologic dysfunction than hospital births attended by physicians or midwives | Increased risk of five-minute Apgar score of 0 and neonatal seizures or serious neurologic dysfunction in out-of-hospital births should be disclosed to patients who express interest in out-of-hospital birth |
| Grünebaum (2014)A5 | Vital statistics 2006 to 2009 Neonatal mortality in relation to birth setting and birth attendant | 12,709,881 hospital physician deliveries 1,096,555 hospital midwife deliveries 39,523 freestanding birth center deliveries 61,993 home birth midwife deliveries | Home birth midwife deliveries had higher neonatal mortality than hospital midwife deliveries (relative risk = 3.87); the excess total neonatal mortality for home birth midwife deliveries was 0.932 per 1,000 births | Increase in total neonatal mortality for home births and even higher risks for patients at 41 weeks' or more gestation and patients having a first birth |
| Grünebaum (2015)A6 | Vital statistics 2010 to 2012 Analysis of the perinatal risks of midwife-attended planned home births | 56,140 midwife-attended planned home births 34.4% by certified nurse midwife 65.7% by “other midwife” | Midwife-attended planned home births had the following risk factors: 0.74% breech 0.64% twin gestation 4.4% previous cesarean delivery 28.19% gestational age of 41 weeks or more | At least 30% of midwife-attended planned home births are not low-risk pregnancies, according to American College of Obstetricians and Gynecologists recommendations |
| Grünebaum (2017)A7 | Vital statistics 2009 to 2013 Neonatal death for certified nurse midwife hospital deliveries, physician hospital deliveries, and planned home birth deliveries to identify risk factors for planned home birth | 11,779,659 hospital physician deliveries 1,077,197 hospital certified nurse midwife deliveries 96,815 planned home births | Overall risk of neonatal death was higher in planned home births compared with hospital births by physicians or certified nurse midwives Neonatal mortality rates were increased in planned home births with the following risk factors: Breech Nulliparous patients Previous cesarean delivery Gestational age of 41 weeks or more | Two additional risk factors (first-time births and gestational age of 41 weeks or more) should be added to the list of absolute contraindications to planned home birth |
| Malloy (2010)A8 | Vital statistics 2000 to 2004 Neonatal mortality | 1,237,129 hospital certified nurse midwife deliveries 17,389 hospital “other midwife” deliveries 13,529 home certified nurse midwife deliveries 42,375 home “other midwife” deliveries 25,319 birth center certified nurse midwife deliveries | AOR for neonatal mortality for home certified nurse midwife vs. hospital certified nurse midwife deliveries was 2.02 AOR for neonatal mortality for home “other midwife” vs. hospital certified nurse midwife deliveries was 3.63 | Deliveries at home attended by certified nurse midwives and “other midwives” are associated with higher risks of mortality than hospital-attended certified nurse midwife deliveries |
| Snowden (2015)A9 | Vital statistics (state of Oregon) 2012 to 2013 Perinatal morbidity and mortality, maternal morbidity, and obstetric procedures | 75,923 planned hospital births 3,203 planned out-of-hospital births 601 planned out-of-hospital births that occurred in hospital after transfer | Planned out-of-hospital birth was associated with increased odds of perinatal death (AOR = 2.43) and neonatal death (AOR = 2.87) compared with planned hospital birth Planned out-of-hospital birth was associated with decreased odds of cesarean delivery (AOR = 0.18) and increased odds of unassisted vaginal delivery (AOR = 5.63) | Rates of obstetric interventions are lower but risks of perinatal death and other adverse neonatal outcomes are higher in planned out-of-hospital birth compared with planned hospital birth; however, the absolute risk of death is low in both settings |
| Stapleton (2013)A10 | American Association of Birth Centers birth registry 2007 to 2010 Descriptive statistics of patients planning birth center birth | 79 birth centers in 33 states 15,574 patients with planned birth center birth at onset of labor | 93% of patients had spontaneous vaginal delivery Transfer rates were 12.4% intrapartum, 2.4% postpartum, and 2.6% neonatal Cesarean delivery rate was 6% | Study demonstrates low rates of obstetric interventions at birth center deliveries |
| Tilden (2017)A11 | Vital statistics 2007 to 2010 Neonatal outcomes of VBAC deliveries in relation to birth setting | 106,823 hospital VBAC births 3,147 out-of-hospital VBAC births | Compared with hospital VBAC, out-of-hospital VBAC neonates had increased odds of seizures (AOR = 8.53) and five-minute Apgar score less than 4 (AOR = 1.77) | Adverse outcomes are more common for neonates born by VBAC outside of a hospital |
Community Birth Planning
Although ACOG and the American Academy of Pediatrics advise that hospitals and accredited birth centers are the safest location for birth, most planned community births occur at home and are attended by a midwife.2,9,13 Among patients who plan a home birth, a small number choose unassisted childbirth (also called freebirth) because they believe that childbirth is inherently safe and that unacceptable risks are associated with professional support; however, perinatal mortality is increased and maternal mortality has been reported to be 90 times higher in U.S. patients without obstetric care.48,49 The World Health Organization advocates for the presence of a maternal and newborn health professional at all deliveries, including uncomplicated childbirth, to identify and refer mothers and newborns who experience unanticipated complications.50 Unassisted childbirth should be strongly discouraged.49
MIDWIVES
The United States has three different professional credentials for midwives with differing levels of education and training, as well as variable practice conditions and standards of care51 (eTable B). Certified nurse midwives and certified midwives receive formal education in university-based systems. Certified nurse midwives are trained in nursing and midwifery, whereas certified midwives and certified professional midwives are known as direct-entry midwives because they are not required to have a nursing education as part of their training. Notably, direct-entry midwives are not licensed in all states. Certified professional midwives represent the majority of direct-entry midwives and may take different pathways to certification, with most graduating from an accredited program (36.9%) or completing a portfolio evaluation process (48.5%).52

| American Association of Birth Centers (AABC; https://www.birthcenters.org) Multidisciplinary membership organization that promotes and supports birth centers as safe environments for minimal-intervention birth Scope of practice Birth center provides a mother-centered range of services to meet the physical, emotional, socioeconomic, informational, and medical needs of the client as listed in the AABC Standards for Birth Centers Freestanding birth center is a distinct and separate space (not a hospital) for childbirth where the care provided is defined by the principles of midwifery AABC Standards for Birth Centers set national standards to assess the quality of services provided to childbearing families in birth centers American College of Nurse-Midwives (ACNM; https://www.midwife.org) Professional association that represents certified nurse midwives and certified midwives Scope of practice: provide primary care, gynecologic, and family planning services for patients from adolescence to beyond menopause, including: Care during pregnancy, childbirth, and postpartum period Care of normal newborn during the first 28 days of life Preconception care Practice in a variety of settings, including: Ambulatory care clinics Birth centers Homes Hospitals Private offices Public health systems Must meet the Core Competencies for Basic Midwifery Practice and must practice in accordance with the Standards for the Practice of Midwifery as defined by the ACNM Midwives Alliance of North America (MANA; https://www.mana.org) Professional midwifery organization that is inclusive of all midwives regardless of educational route to midwifery Scope of practice MANA Core Competencies establish the essential knowledge, clinical skills, and critical thinking necessary for entry-level practice for direct-entry midwifery Midwife may practice in any setting, including home, community, hospital, or clinic Each midwife will develop practice guidelines for their services that are in agreement with the MANA Standards and Qualifications for the Art and Practice of Midwifery, the MANA Statement of Values and Ethics, and the MANA Core Competencies for Midwifery Practice National Association of Certified Professional Midwives (NACPM; https://www.nacpm.org) Membership organization representing certified professional midwives Scope of practice Members are trained to recognize abnormal or dangerous conditions needing expert help outside their scope Members have a plan for consultation and referral, and provide emergency care for mothers and babies until additional assistance is available Offer care, education, counseling, and support to patients and their families throughout pregnancy, birth, and the postpartum period Members practice primarily in out-of-hospital settings NACPM Standards of Practice provide a tool for measuring actual practice and appropriate use of the body of knowledge of midwifery North American Registry of Midwives (NARM; http://www.narm.org) Mission is to provide and maintain an evaluation process for multiple routes of midwifery education and training and to identify best practices to set the standards for the certified professional midwife credential Scope of practice Derived from the NARM Job Analysis, state laws and regulations, and individual practice guidelines developed by each midwife according to their skills and knowledge Certified professional midwives work with their clients to: Monitor the pregnancy, labor, birth, and newborn and postpartum periods Promote a healthy pregnancy Provide education for informed decision-making Recommend appropriate management in collaboration with other health care professionals when necessary if complications arise Most certified professional midwives work in private homes or birth centers NARM does not set protocols for all certified professional midwives to follow but requires that they develop their own practice guidelines based on standards, values, and ethics held by the midwife |
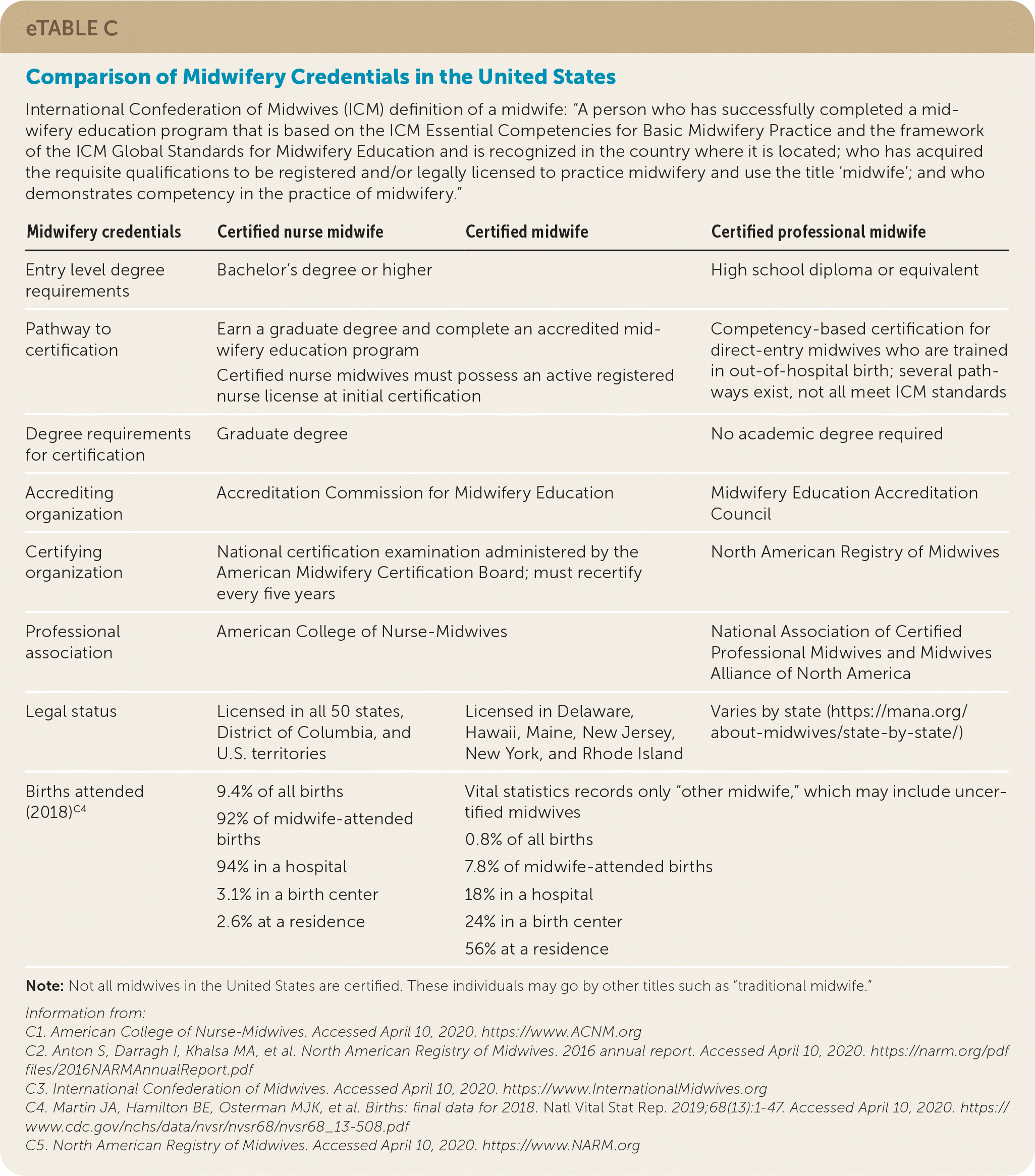
The regulation and licensure of midwives vary by state, with some states prohibiting certain types of midwives from participation in planned home birth.53 There are also “traditional” midwives who may or may not be certified or licensed. In the interest of public health and safety, the American College of Nurse-Midwives states that any person who wants to become a midwife in the United States should meet, at minimum, the International Confederation of Midwives International Definition of the Midwife and the Global Standards for Midwifery Education.54 Not all pathways to midwifery in the United States are accredited and, thus, not all meet International Confederation of Midwives standards52,55 (eTable C).
| Midwifery credentials | Certified nurse midwife | Certified midwife | Certified professional midwife | |
|---|---|---|---|---|
| Entry level degree requirements | Bachelor's degree or higher | High school diploma or equivalent | ||
| Pathway to certification | Earn a graduate degree and complete an accredited midwifery education program Certified nurse midwives must possess an active registered nurse license at initial certification | Competency-based certification for direct-entry midwives who are trained in out-of-hospital birth; several pathways exist, not all meet ICM standards | ||
| Degree requirements for certification | Graduate degree | No academic degree required | ||
| Accrediting organization | Accreditation Commission for Midwifery Education | Midwifery Education Accreditation Council | ||
| Certifying organization | National certification examination administered by the American Midwifery Certification Board; must recertify every five years | North American Registry of Midwives | ||
| Professional association | American College of Nurse-Midwives | National Association of Certified Professional Midwives and Midwives Alliance of North America | ||
| Legal status | Licensed in all 50 states, District of Columbia, and U.S. territories | Licensed in Delaware, Hawaii, Maine, New Jersey, New York, and Rhode Island | Varies by state (https://mana.org/about-midwives/state-by-state/) | |
| Births attended (2018)C4 | 9.4% of all births 92% of midwife-attended births 94% in a hospital 3.1% in a birth center 2.6% at a residence | Vital statistics records only “other midwife,” which may include uncertified midwives 0.8% of all births 7.8% of midwife-attended births 18% in a hospital 24% in a birth center 56% at a residence | ||
BIRTH CENTERS
Birth centers are facilities where low-risk patients with uncomplicated pregnancies can deliver in a home-like environment attended by midwives. Currently, there are fewer than 400 known birth centers licensed in 42 states.31 Of these, 119 freestanding birth centers are accredited according to national standards established by the American Association of Birth Centers. Accredited birth centers conduct ongoing assessment to ensure pregnant patients meet specified eligibility criteria.56 ACOG recognizes accredited birth centers as part of an integrated maternity health system in which consultation and referral for patients or newborns who exceed the birth center scope of practice can take place.57
Transfer to Hospital Care
Transfer to hospital care may be indicated in planned out-of-hospital birth for a variety of reasons (Table 54,12,13,45,58); up to one-third of nulliparous patients require transfer to a hospital.45,58 Patients who are transferred are more likely to have medical or obstetric risk factors.29 Long distances, delays in decision to transfer, or difficulty arranging transfer because of a lack of integration may lead to worse outcomes. Consequently, community birth plans should include contingencies for urgent and nonurgent transport to a nearby hospital with prearranged agreements for obstetric and neonatal care.9,13–15

| During labor Maternal Cord prolapse Hemorrhage Malpresentation Maternal exhaustion Prolonged rupture of membranes without active labor Request for pain control Slow progress of labor Suspected intra-amniotic infection Fetal Fetal demise Fetal distress Gestational age < 37 weeks After delivery Maternal Lacerations requiring repair by an obstetrician Postpartum hemorrhage Retained placenta Newborn Congenital malformation Hyperbilirubinemia Hypoglycemia Low Apgar score Poor feeding Respiratory distress Suspected sepsis |
Newborn Care
A qualified clinician whose primary responsibility is care of the newborn should be present at all community births. The attendant should have the proper equipment for resuscitation according to current Neonatal Resuscitation Program protocols and should ensure that American Academy of Pediatrics Guidelines for Perinatal Care are followed.13 A detailed record of the patient's prenatal care and delivery, as well as care provided to the newborn, should accompany the newborn to the initial evaluation within the first 24 hours of life. Clinicians should review pertinent maternal laboratory and study results. Newborn tests, medications, and vaccinations must be reviewed and completed as necessary (Table 613). Regardless of personal beliefs, family physicians should remain nonjudgmental about parental choice of birth location while maintaining their role as an advocate for the child.

| Before delivery Ensure availability of appropriate transport to medical facility Ensure availability of proper resuscitation equipment Ensure presence of separate health care professional qualified in neonatal resuscitation whose primary responsibility is care of the newborn Validate communication and coordination with nearby medical facility At delivery Assign Apgar scores Provide warmth and appropriate resuscitation measures Subsequent care Arrange follow-up with clinician experienced in the care of children Assess risk of group B streptococcal disease Assess risk of hypoglycemia Complete physical examination Congenital heart disease screening Eye prophylaxis for gonococcal ophthalmia neonatorum Hearing screening Hepatitis B vaccination Record vital signs and measurements Screening for hyperbilirubinemia Universal newborn screening Vitamin K administration |
Ethical Implications
The selection of birth setting involves an exchange of risks. Community birth is associated with decreased obstetric interventions and lower cesarean delivery rates, which are consistent with outcomes for low-risk pregnancies managed by hospital-based midwives.28,59 On the other hand, community birth has a higher risk of neonatal morbidity and mortality. This is especially true for patients who are not considered low risk, which may be almost one-third of those who plan a home birth.41 Family physicians have an obligation to respect patient autonomy while adhering to the principles of beneficence and nonmaleficence.60 In such situations, dialogue with the patient and directive counseling rather than confrontation may provide essential information about the risks and benefits associated with hospital and out-of-hospital birth, proper patient selection, choice of attendant, and contingency planning.
Data Sources: A PubMed search was completed in Clinical Queries using the key terms home birth, birth center, out-of-hospital birth, midwife, maternal outcome, and perinatal outcome. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. Also searched were the Cochrane database and Ovid. Search dates: December 27, 2019, and March 4, 2021.
The views expressed in this article are those of the authors and do not reflect the official policy or position of the Department of the Army, the Department of the Navy, the Uniformed Services University of the Health Sciences, the Department of Defense, or the U.S. government.
