
Am Fam Physician. 2021;104(1):83-84
Author disclosure: No relevant financial affiliations.
A 63-year-old patient with multiple chronic medical conditions was admitted to the hospital for nonpurulent cellulitis at the base of the neck. The diagnostic workup revealed methicillin-resistant Staphylococcus aureus (MRSA) bacteremia and a urinary tract infection. Chest radiography and transthoracic echocardiography were unremarkable.
After five days of appropriate culture-guided intravenous antibiotics, the patient's inflammatory markers remained elevated, and blood cultures continued to grow MRSA. Skin examination revealed lesions on the soles of the feet (Figure 1).
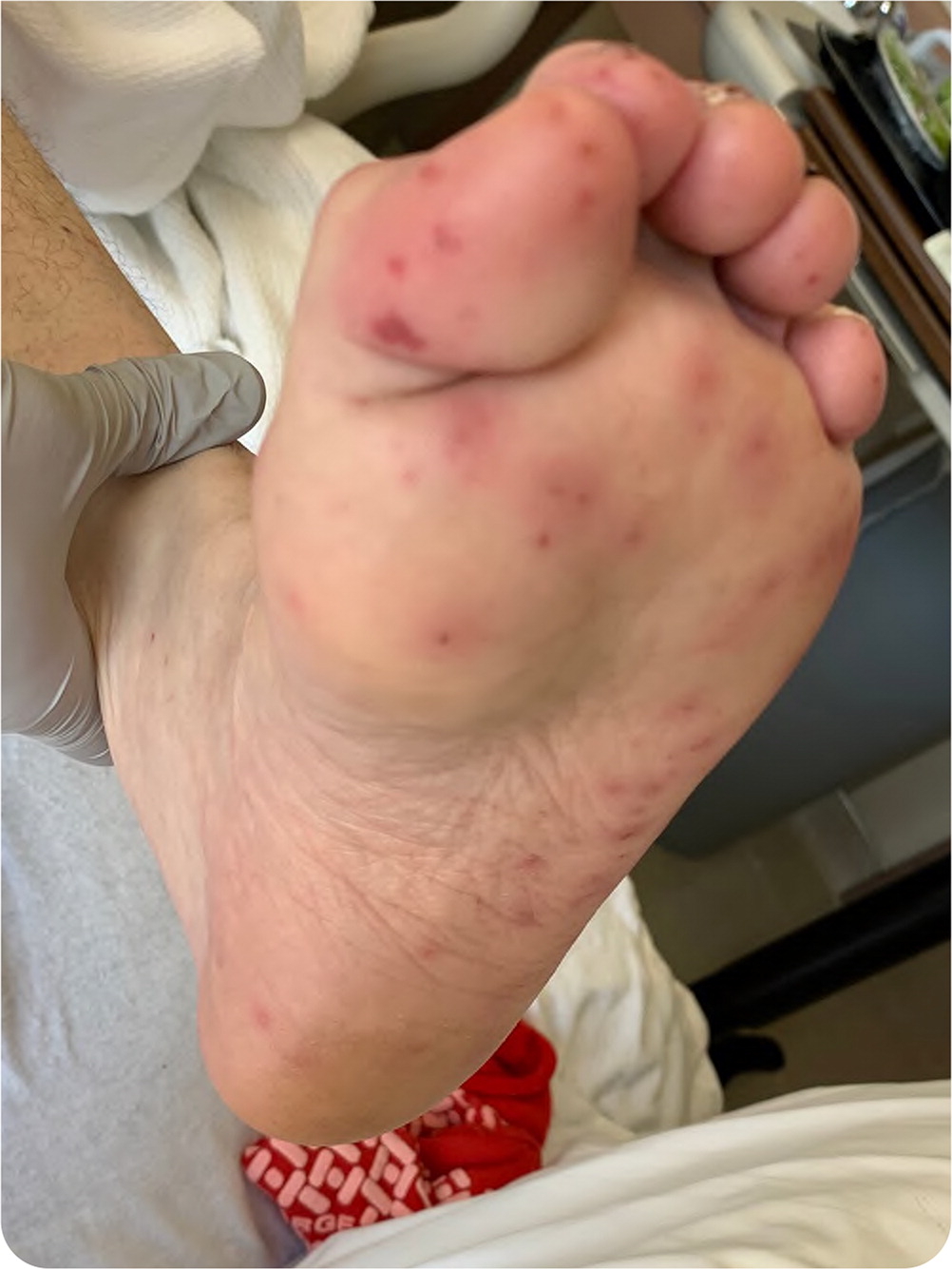
Question
Based on the patient's history and physical examination findings, which one of the following is the best next step?
A. Biopsy of foot lesions.
B. Referral for cardiothoracic surgery.
C. Repeat transthoracic echocardiography.
D. Rickettsia serology.
E. Transesophageal echocardiography.
Discussion
The answer is E: transesophageal echocardiography. Figure 1 shows Janeway lesions caused by septic microthrombi, which are highly suggestive of infective endocarditis. When there is low suspicion for endocarditis, the American Heart Association recommends beginning with transthoracic echocardiography.1 If concerning features are found or suspicion for infective endocarditis increases, a transesophageal echocardiography should be performed. Transesophageal echocardiography detects evidence of infective endocarditis in 19% of patients with negative findings on transthoracic echocardiography and allows for further characterization of valvular disease and evaluation for surgical management.2
Suspicion for infective endocarditis is initially evaluated using modified Duke criteria (Table 1).2 Infective endocarditis can be definitively diagnosed if the patient has two major criteria, one major and three minor criteria, or five minor criteria. Infective endocarditis is possible in those with one major and one minor criteria or three minor criteria. A definite diagnosis according to modified Duke criteria has a sensitivity of 80%.2 A nondiagnosis has a negative predictive value of more than 92%.2 This patient had one major and one minor criteria initially, developing a second minor criterion with the septic emboli. The patient underwent a transesophageal echocardiography, which revealed endocardial involvement. This provided the two major criteria needed for a definitive diagnosis.

| Major criteria |
| Two positive blood cultures for organisms known to commonly cause infective endocarditis |
| Single culture positive for Coxiella burnetii |
| Endocardial involvement |
| Minor criteria |
| Predisposing heart condition or injection drug use |
| Fever |
| Vascular phenomenon |
| Immunologic phenomenon |
| Positive blood culture findings that do not meet major criteria |
Biopsy of the lesions would show septic microthrombi that could be cultured for the causative microorganism. However, biopsy findings would not contribute to the diagnosis of infective endocarditis using Duke criteria.
Repeat transthoracic echocardiography is inappropriate because it was previously negative and would be unlikely to yield additional information.
This patient requires a definite diagnosis of endocarditis and further characterization of valvular disease before referral for surgical management. Indications for valve repair or replacement include heart failure, heart block, recurrent emboli, larger vegetations (greater than 10 mm), and persistent bacteremia.7
Rocky Mountain spotted fever, caused by Rickettsia rickettsii infection, can lead to a high fever and a rash on the soles, similar to this patient's presentation. However, this diagnosis was less likely because of the MRSA bacteremia. Rocky Mountain spotted fever is commonly associated with a tick bite and is more prevalent in the southeastern United States.
The opinions and assertions contained herein are the private views of the authors and are not to be construed as official or as reflecting the views of the U.S. Army Medical Department or the U.S. Army at large.
