
Am Fam Physician. 2022;105(1):77-78
Author disclosure: No relevant financial relationships.
A 64-year-old man presented with a 10-year history of severe scrotal swelling. The swelling fluctuated in size but was enlarging. The area was tender to touch but otherwise not painful. He reported no hematuria, voiding difficulties, or urinary frequency or retention. He was unable to obtain an erection.
On physical examination, his vital signs were normal. His abdomen was soft, with normal bowel sounds. There was no hepatosplenomegaly or abdominal tenderness, including no costovertebral angle tenderness. Slight suprapubic swelling was detected.
Genital examination revealed a volleyball-sized scrotal swelling that engulfed the penis (Figure 1). The left testicle was displaced, and the right testicular anatomy was distorted, with the testicle possibly located in the inguinal canal. The scrotal skin was tender, thickened, and hyperpigmented.
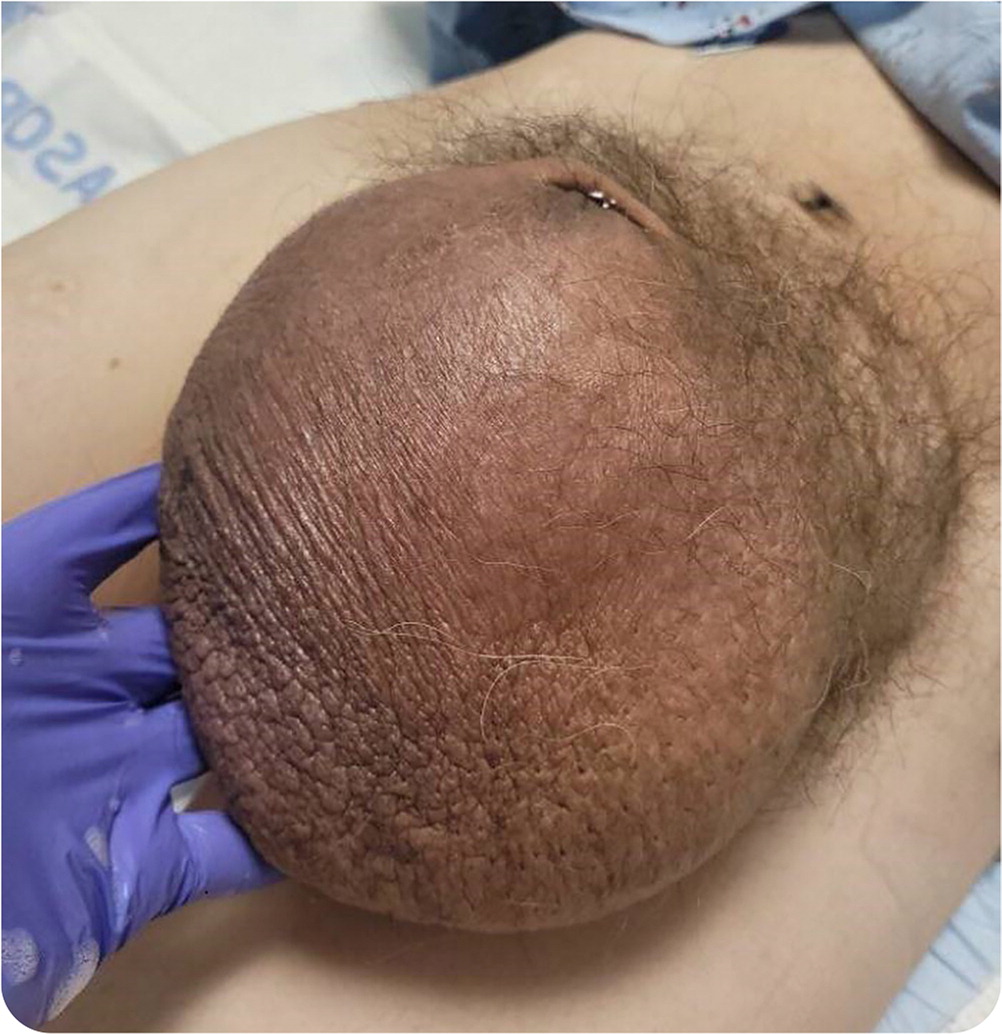
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Femoral artery aneurysm.
B. Hydrocele.
C. Inguinal hernia.
D. Testicular torsion.
E. Varicocele.
Discussion
The answer is C: inguinal hernia. Inguinal hernias are protrusions of the abdominal contents into the inguinal canal via an abdominal wall defect. Inguinal hernias are commonly direct or indirect. A direct inguinal hernia projects through the deep inguinal ring, medial to the inferior epigastric vessels through the posterior wall. Indirect inguinal hernias project through the internal inguinal ring, lateral to the inferior epigastric vessels, with potential descent into the inguinal canal. Direct hernias typically develop in adulthood and are more likely to recur than indirect hernias.1,2
Although imaging is not needed to diagnose most inguinal hernias, ultrasonography can distinguish hernias from other causes of groin pain. Inguinal hernias, especially indirect types, are often asymptomatic. Both types may cause bulging, localized fullness, or heaviness in the groin that increases over time. These hernias may be reducible and decrease when supine. Associated symptoms can include a burning or dull aching sensation and increased pain with Valsalva maneuvers (coughing, straining, lifting). Severe acute pain suggests an incarcerated hernia.
A true femoral artery aneurysm involves all three layers (intima, media, and adventitia) and is often associated with other peripheral aneurysms and arteriosclerotic conditions. In contrast, a pseudoaneurysm consists of an outpouching of one or two layers of the vessel wall. Femoral artery aneurysms often present as asymptomatic leg or groin swelling but may cause tenderness, pain, a pulsatile mass, or ecchymosis. Possible complications include expansion, rupture, embolization, extravasation with arterial wall compression, and ischemia.3
A hydrocele is a collection of fluid in the space surrounding the testicle between the layers of the tunica vaginalis.4 It may be communicating (patent processus vaginalis with free flow of fluid) or noncommunicating (usually scrotal and may extend to the external inguinal ring).1 Hydroceles present as painless scrotal swellings anterior to the testicle and cord that enlarge and become increasingly tense during the day. Scrotal swelling is not reducible. Fluid is present on transillumination. Hydroceles are common in infants and children.
Testicular torsion occurs when the testicle rotates and twists on the spermatic cord, potentially obstructing testicular blood flow.5 Torsion presents as sudden, severe, unilateral scrotal pain or as vague abdominal or inguinal pain that gradually radiates to the scrotum. The scrotum may appear erythematous, swollen, and discolored. Associated nausea and vomiting can occur. The twisting of the spermatic cord can cause the testicle to become high riding within the scrotum and can lead to reduction or elimination of the cremasteric reflex. Prehn sign is used to differentiate bacterial epididymitis and testicular torsion (scrotal elevation relieves pain in epididymitis but not torsion). Testicular torsion is most common in newborns and teenagers.
A varicocele is abnormal dilation and enlargement of the scrotal venous pampiniform plexus, which drains blood from each testicle.6 Varicoceles can be asymptomatic or present as a mild dull, achy pain or heaviness in the scrotum that worsens with standing, vigorous exercise, or Valsalva maneuvers. They may be described as soft lumps above the testicle (bag of worms), usually on the left side of the scrotum. Varicoceles may be the result of trauma but are often found during routine examinations or evaluations for infertility.
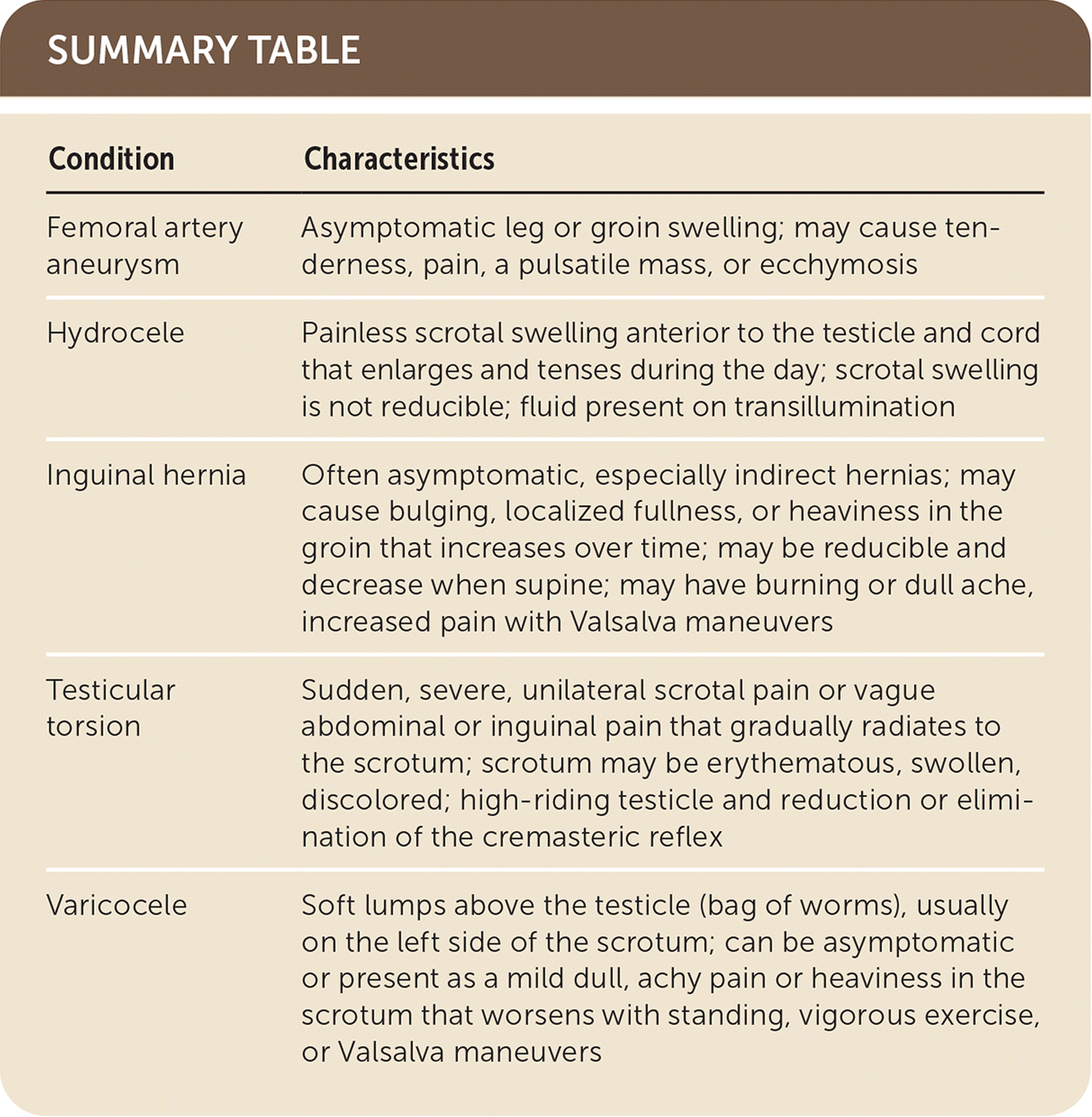
| Condition | Characteristics |
|---|---|
| Femoral artery aneurysm | Asymptomatic leg or groin swelling; may cause tenderness, pain, a pulsatile mass, or ecchymosis |
| Hydrocele | Painless scrotal swelling anterior to the testicle and cord that enlarges and tenses during the day; scrotal swelling is not reducible; fluid present on transillumination |
| Inguinal hernia | Often asymptomatic, especially indirect hernias; may cause bulging, localized fullness, or heaviness in the groin that increases over time; may be reducible and decrease when supine; may have burning or dull ache, increased pain with Valsalva maneuvers |
| Testicular torsion | Sudden, severe, unilateral scrotal pain or vague abdominal or inguinal pain that gradually radiates to the scrotum; scrotum may be erythematous, swollen, discolored; high-riding testicle and reduction or elimination of the cremasteric reflex |
| Varicocele | Soft lumps above the testicle (bag of worms), usually on the left side of the scrotum; can be asymptomatic or present as a mild dull, achy pain or heaviness in the scrotum that worsens with standing, vigorous exercise, or Valsalva maneuvers |
