
Successful reporting begins with preparation.
Fam Pract Manag. 2010;17(1):24-26
Sally Roland is a compliance coordinator for the Methodist Physicians Clinic in Omaha, Neb. Author disclosure: nothing to disclose.
Fifty-five percent of physicians and other eligible health care providers who submitted data for the Centers for Medicare & Medicaid Services (CMS) Physician Quality Reporting Initiative (PQRI) in 2008 received their incentive payments. This was only slightly higher than the percentage paid in 2007. Participation grew in 2008, but the fact that nearly half of those who reported quality data did not earn an incentive payment is evidence of the frustration and difficulty that many physicians have experienced with the program. Our practice has participated in PQRI every year and achieved great results. This article will describe how we did it, and what you can do to make your practice's reporting a success.
Our venture
Our multispecialty group, Methodist Physicians Clinic Inc., comprises 140 physicians and 40 midlevel providers. Under the leadership of David Filipi, MD, then vice president of medical affairs, our clinic geared up to participate in the PQRI program beginning on July 1, 2007. Our goal was, and continues to be, to provide the highest level of care for our patients and their families. Participating in the PQRI program offered us an opportunity to measure our success in this endeavor.
Most of our physicians participated in the program. Those who chose not to concluded that none of the PQRI quality measures could be readily applied to their specialty. Family physicians in our group reported on the diabetes mellitus measures. (For a list of the PQRI measures and other information about the program, go to http://www.cms.hhs.gov/PQRI/02_Spotlight.asp.)
Physicians who successfully participated in the PQRI program in 2007 and 2008 were eligible to earn a bonus equal to 1.5 percent of their total Medicare allowed charges for the year. (The incentive payment was raised to 2 percent in 2009.) It is important to estimate potential costs and bonuses before making a decision about whether to take part in the program. We estimated our costs to be approximately $4 per patient encounter (based on physicians' time and materials; administrative expenses were not included) and concluded that our participation would be worthwhile.
How we reported the data
We knew creating an efficient administrative process would be critical to our success. Our clinic held brainstorming sessions to decide how to most effectively collect and report the PQRI data without overburdening the physicians. We learned quickly how important it is to involve the coding and billing staff, who were instrumental in helping develop a clearly defined process for reporting the data. Ultimately we decided to design data collection stickers to help us capture the clinical information required for each particular measure (for example, see the diabetes measure sticker below).
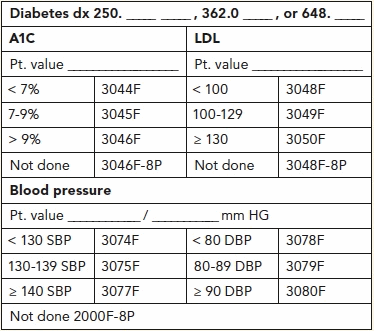
We distributed instructions to all staff that explained how we would incorporate the stickers into our clinical and billing processes. The system works like this for the PQRI diabetes measures: If the patient has an established diagnosis of diabetes, the ancillary staff places the diabetes sticker on the superbill before the physician sees the patient. An ancillary staff member collects the chart and superbill after the visit and records the required data (A1C, LDL and blood pressure) on the PQRI sticker. If there is no indication in the documentation that the physician addressed the patient's diabetes during the visit, the staff member can ignore the sticker. When a patient is first diagnosed with diabetes, the physician may cue the staff member verbally that a new diabetes diagnosis has been made, or the staff member may see the diabetes diagnosis code when reviewing the superbill. In either case, the staff member then attaches the PQRI sticker to the superbill, records the appropriate data and forwards the superbill to the coding staff for data entry.
The coding staff then converts the clinical data from the sticker into the CPT Category II codes (or “quality codes”) for PQRI reporting. To do this, they simply circle the appropriate code that correlates to the data provided by the clinical staff. If you look at the above label, for example, you can see that if the patient's A1C was 7.9 percent, the coder would circle code 3045F. If the LDL value was 142, the coder would circle 3050F. If the patient's blood pressure was 120/86, the coder would circle 3074F for the systolic blood pressure and 3079F for the diastolic blood pressure.
If the clinical staff forgets to attach the appropriate sticker to the superbill, the coding staff does it. This is time consuming, as the coder then has to go into the patient's record to look up the clinical data required.
The billing department developed their own system for ensuring that the necessary PQRI reporting codes are included in claims. They added a step that allows for review of electronic claims before they are submitted to payers.
Tips for reporting
Many providers did not qualify for the PQRI incentive payment because they missed one or more required elements on their claims. Because there is no opportunity to revise and resubmit a claim and because you must report on 80 percent of eligible patients to earn the incentive payment, it is crucial that claims be correct before submission. Based on our experience, here are our tips for successful reporting:
1. Prepare. Refer to the list of PQRI measures (there are 179 measures for 2010) published by CMS and identify those that you can report on. You must report on at least three measures to be eligible for the incentive payment. Estimate the financial impact that the program would have on your practice as well as the potential for increased quality of care and its impact on your patients. If necessary, present this information to physicians and clinical staff to gain their support and involvement. Early on, enlist the support and commitment of the administrative, coding and billing staff.
2. Select measures. Choose the measures you will report on. They should reflect data you are already tracking in the process of managing a patient's chronic health condition or other diagnosis. For a patient with diabetes, for example, you would report on measures for blood pressure, lipid management and A1C.
3. Collect data. Collect the necessary PQRI data as patients receive care using a system that makes it easy to capture the CPT Category II code at the time of service. It is most efficient to collect the data while the provider's staff has the information readily available.
4. Report data. Be sure to include all elements required for reporting on the selected measures. Submit the CPT Category II code, along with the CPT and ICD-9 codes that are required, for the PQRI measures you are reporting on. Report all required data elements on the same claim as the charges for services submitted to CMS. Verify that a national provider identifier number is correctly reported on all claims.
5. Monitor. Run internal reports to ensure that PQRI data is being reported for at least 80 percent of all Medicare patients with the condition you're reporting on. Running reports to track the accuracy and volume of claims and analyzing this data regularly will help your practice identify process improvements and prepare for the next reporting year.
A BRIEF HISTORY OF PQRI
The Physician Quality Reporting Initiative sprouted from the roots of the 2006 Tax Relief and Health Care Act. This act required the establishment of a physician quality reporting system, including an incentive payment for eligible professionals who satisfactorily reported data on specific quality measures for services covered by the Center for Medicare & Medicaid Services (CMS). PQRI officially launched on July 1, 2007.
Participation in the PQRI program is currently voluntary, but many believe that PQRI is a precursor to a mandatory pay-for-performance program. Because of its voluntary nature, CMS established a financial incentive for reporting data. Participants who successfully report can now earn a bonus payment of 2 percent of the total allowed charges for covered services provided to Medicare fee-for-service patients.
Enjoying the fruits of our labor
Eighty-four percent of our family physicians (38 out of 45) qualified for the PQRI incentive payment in 2008, earning a total of $45,851 through the program. The bonuses averaged just over $1,000 each and ranged from $94 to $2,707.
More important, we are very proud of the quality of care we provide to our patients. Our family physicians have much better control of their diabetic patients' A1Cs, lipids and blood pressures when compared with family physicians nationally. According to CMS data, nearly 61 percent of our patients with diabetes reached A1C, lipid and blood pressure levels that put them in the top quartile of all patients for whom these measures were reported.
We strongly encourage you to take part in this year's PQRI process. The reporting period for 2010 runs from Jan. 1 to Dec. 31. If you would like to participate, there's no signup or registration required. We wish you good luck and successful reporting.
