Taking steps to recognize and correct unconscious assumptions toward groups can promote health equity.

Jamie is a 38-year-old woman and the attending physician on a busy inpatient teaching service. On rounds, she notices several patients tending to look at the male medical student when asking a question and seeming to disregard her. Alex is a 55-year-old black man who has a history of diabetic polyneuropathy with significant neuropathic pain. His last A1C was 7.8. He reports worsening lower extremity pain and is frustrated that, despite his bringing this up repeatedly to different clinicians, no one has addressed it. Alex has been on gabapentin 100 mg before bed for 18 months without change, and his physicians haven't increased or changed his medication to help with pain relief.
Alisha is a 27-year-old Asian family medicine resident who overhears labor and delivery nurses and the attending complain that Indian women are resistant to cervical exams.
These scenarios reflect the unconscious assumptions that pervade our everyday lives, not only as practicing clinicians but also as private citizens. Some of Jamie's patients assume the male member of the team is the attending physician. Alex's physicians perceive him to be a “drug-seeking” patient and miss opportunities to improve his care. Alisha is exposed to stereotypes about a particular ethnic group.
Although assumptions like these may not be directly ill-intentioned, they can have serious consequences. In medical practice, these unconscious beliefs and stereotypes influence medical decision-making. In the classic Institute of Medicine report “Unequal Treatment: Confronting Racial and Ethnic Disparities in Health Care,” the authors concluded that “bias, stereotyping, and clinical uncertainty on the part of health care providers may contribute to racial and ethnic disparities in health care” often despite providers' best intentions.1 For example, studies show that discrimination and bias at both the individual and institutional levels contribute to shocking disparities for African-American patients in terms of receiving certain procedures less often or experiencing much higher infant mortality rates when compared with non-Hispanic whites.2,3 As racial and ethnic diversity increases across our nation, it is imperative that we as physicians intentionally confront and find ways to mitigate our biases.
KEY POINTS
- Implicit bias is the unconscious collection of stereotypes and attitudes that we develop toward certain groups of people, which can affect our patient relationships and care decisions.
- You can overcome implicit bias by first discovering your blind spots and then actively working to dismiss stereotypes and attitudes that affect your interactions.
- While individual action is helpful, organizations and institutions must also work to eliminate systemic problems.
DEFINING AND REDUCING IMPLICIT BIAS
For the last 30 years, science has demonstrated that automatic cognitive processes shape human behavior, beliefs, and attitudes. Implicit or unconscious bias derives from our ability to rapidly find patterns in small bits of information. Some of these patterns emerge from positive or negative attitudes and stereotypes that we develop about certain groups of people and form outside our own consciousness from a very young age. Although such cognitive processes help us efficiently sort and filter our perceptions, these reflexive biases also promote inconsistent decision making and, at worst, systematic errors in judgment.
Cognitive processes lead us to associate unconscious attributes with social identities. The literature explores how this influences our views on race, ethnicity, age, gender, sexual orientation, and weight, and studies show many people are biased in favor of people who are white, young, male, heterosexual, and thin.4 Unconsciously, we not only learn to associate certain attributes with certain social groupings (e.g., men with strength, women with nurturing) but also develop preferential ranking of such groups (e.g., preference for whites over blacks). This unconscious grouping and ranking takes root early in development and is shaped by many outside factors such as media messages, institutional policies, and family beliefs. Studies show that health care professionals have the same level of implicit bias as the general population and that higher levels are associated with lower quality care.5 Providers with higher levels of bias are more likely to demonstrate unequal treatment recommendations, disparities in pain management, and even lack of empathy toward minority patients.6 In addition, stressful, time-pressured, and overloaded clinical practices can actually exacerbate unconscious negative attitudes. Although the potential impact of our biases can feel overwhelming, research demonstrates that these biases are malleable and can be overcome by conscious mitigation strategies.7
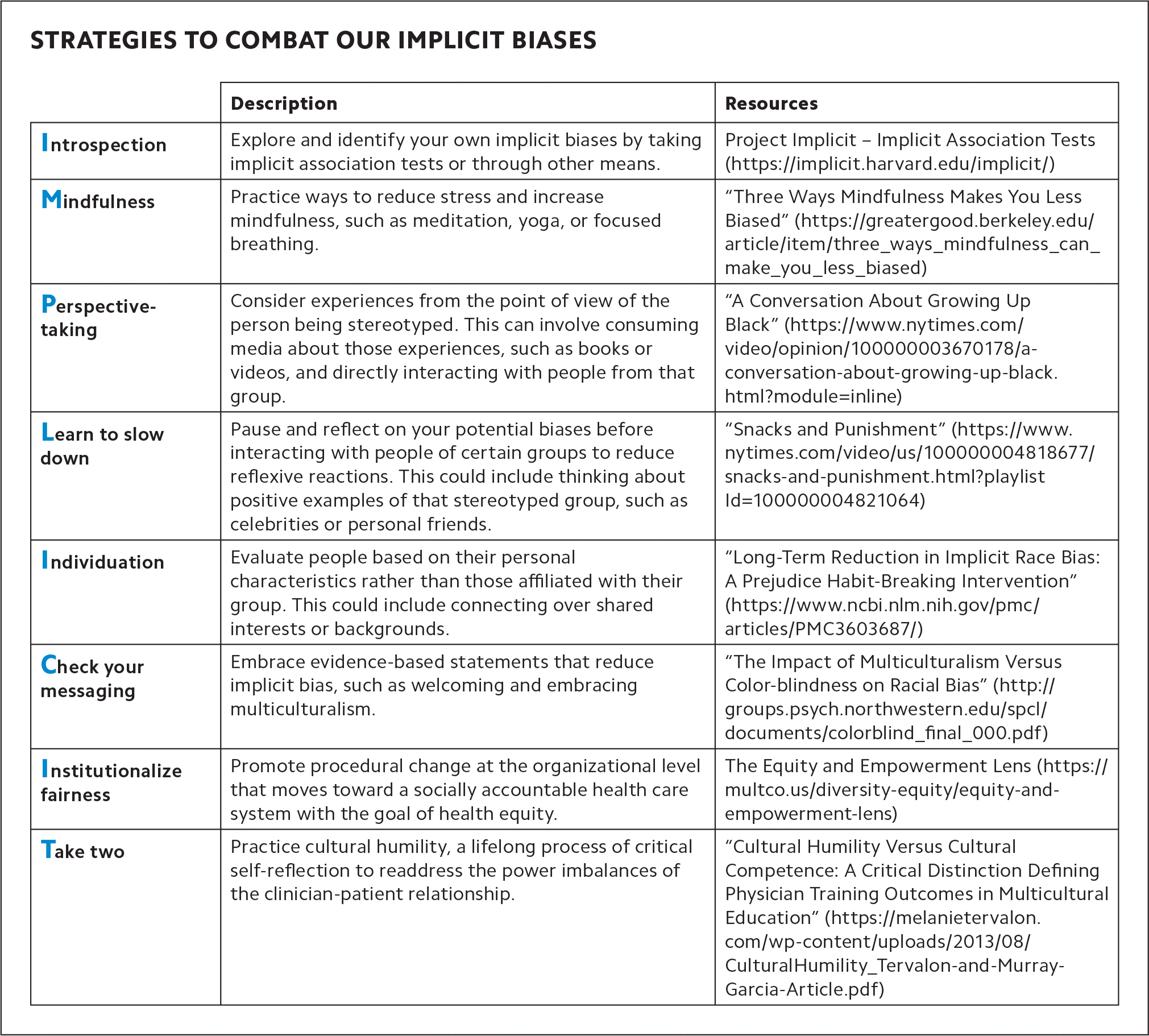
We recommend three overarching strategies to mitigate implicit bias – educate, expose, and approach – which we will discuss in greater detail. We have further broken down these strategies into eight evidence-based tactics you can incorporate into any quality improvement project, diagnostic dilemma, or new patient encounter. Together, these eight tactics spell out the mnemonic IMPLICIT. (See “Strategies to combat our implicit biases.”)
STRATEGIES TO COMBAT OUR IMPLICIT BIASES
| Description | Resources | |
|---|---|---|
| Introspection | Explore and identify your own implicit biases by taking implicit association tests or through other means. | Project Implicit – Implicit Association Tests |
| Mindfulness | Practice ways to reduce stress and increase mindfulness, such as meditation, yoga, or focused breathing. | “Three Ways Mindfulness Makes You Less Biased” |
| Perspective-taking | Consider experiences from the point of view of the person being stereotyped. This can involve consuming media about those experiences, such as books or videos, and directly interacting with people from that group. | “A Conversation About Growing Up Black” |
| Learn to slow down | Pause and reflect on your potential biases before interacting with people of certain groups to reduce reflexive reactions. This could include thinking about positive examples of that stereotyped group, such as celebrities or personal friends. | “Snacks and Punishment” |
| Individuation | Evaluate people based on their personal characteristics rather than those affiliated with their group. This could include connecting over shared interests or backgrounds. | “Long-Term Reduction in Implicit Race Bias: A Prejudice Habit-Breaking Intervention” |
| Check your messaging | Embrace evidence-based statements that reduce implicit bias, such as welcoming and embracing multiculturalism. | “The Impact of Multiculturalism Versus Color-blindness on Racial Bias” |
| Institutionalize fairness | Promote procedural change at the organizational level that moves toward a socially accountable health care system with the goal of health equity. | The Equity and Empowerment Lens |
| Take two | Practice cultural humility, a lifelong process of critical self-reflection to readdress the power imbalances of the clinician-patient relationship. | “Cultural Humility Versus Cultural Competence: A Critical Distinction Defining Physician Training Outcomes in Multicultural Education” |
EDUCATE
When we fail to learn about our blind spots, we miss opportunities to avoid harm. Educating ourselves about the reflexive cognitive processes that unconsciously affect our clinical decisions is the first step. The following tactics can help:
Introspection. It is not enough to just acknowledge that implicit bias exists. As clinicians, we must directly confront and explore our own personal implicit biases. As the writer Anais Nin is often credited with saying, “We don't see things as they are, we see them as we are.” To shed light on your potential blind spots and unconscious “sorting protocols,” we encourage you to take one or more implicit association tests. Discovering a moderate to strong bias in favor of or against certain social identities can help you begin this critical step in self exploration and understanding.8 You can also complete this activity with your clinic staff and fellow physicians to uncover implicit biases as a group and set the stage for addressing them. For instance, many of us may be surprised to learn after taking an implicit association test that we follow the typical bias of associating males with science — an awareness that may explain why the patient in our first case example addressed questions to the male medical student instead of the female attending.
Mindfulness.It should come as no surprise that we are more likely to use cognitive shortcuts inappropriately when we are under pressure. Evidence suggests that increasing mindfulness improves our coping ability and modifies biological reactions that influence attention, emotional regulation, and habit formation.9 There are many ways to increase mindfulness, including meditation, yoga, or listening to inspirational texts. In one study, individuals who listened to a 10-minute meditative audiotape that focused them and made them more aware of their sensations and thoughts in a nonjudgmental way caused them to rely less on instinct and show less implicit bias against black people and the aged.10
EXPOSE
It is also helpful to expose ourselves to counter-stereotypes and to focus on the unique individuals we interact with. Similarity bias is the tendency to favor ourselves and those like us. When our brains label someone as being within our same group, we empathize better and use our actions, words, and body language to signal this relatedness. Experience bias can lead us to overestimate how much others see things the same way we do, to believe that we are less vulnerable to bias than others, and to assume that our intentions are clear and obvious to others. Gaining exposure to other groups and ways of thinking can mitigate both of these types of bias. The following tactics can help:
Perspective-taking. This tactic involves taking the first-person perspective of a member of a stereotyped group, which can increase psychological closeness to that group.8 Reading novels, watching documentaries, and listening to podcasts are accessible ways to reach beyond our comfort zone. To authentically perceive another person's perspective, however, you should engage in positive interactions with stereotyped group members in real life. Increased face-to-face contact with people who seem different from you on the surface undermines implicit bias.
Learn to slow down. To recognize our reflexive biases, we must pause and think. For example, the next time you interact with someone in a stereotyped group or observe societal stereotyping, such as through the media, recognize what responses are based on stereotypes, label those responses as stereotypical, and reflect on why the responses occurred. You might then consider how the biased response could be avoided in the future and replace it with an unbiased response. The physician treating Alex in the introduction could use this technique by slowing down and reassessing his medical care. By acknowledging the potential for bias, the physician may recognize that safe options remain for managing Alex's neuropathic pain.
Additionally, research strongly supports the use of counter-stereotypic imaging to replace automatic responses.11 For example, when seeking to contradict a prevailing stereotype, substitute highly defined images, which can be abstract (e.g., modern Native Americans), famous (e.g., minority celebrities like Oprah Winfrey or Lin-Manuel Miranda), or personal (e.g., your child's teacher). As positive exemplars become more salient in your mind, they become cognitively accessible and challenge your stereotypic biases.
Individuation. This tactic relies on gathering specific information about the person interacting with you to prevent group-based stereotypic inferences. Family physicians are trained to build and maintain relationships with each individual patient under their care. Our own social identities intersect with multiple social groupings, for example, related to sexual orientation, ethnicity, and gender. Within these multiplicities, we can find shared identities that bring us closer to people, including shared experiences (e.g., parenting), common interests (e.g., sports teams), or mutual purpose (e.g., surviving cancer). Individuation could have helped the health care workers in Alisha's labor and delivery unit to avoid making judgments based on stereotypes. We can use this tactic to help inform clinical decisions by using what we know about a person's specific, individual, and unique attributes.11
APPROACH
Like any habit, it is difficult to change biased behaviors with a “one shot” educational approach or awareness campaign. Taking a systematic approach at both the individual and institutional levels, and incorporating a continuous process of improvement, practice, and reflection, is critical to improving health equity.
Check your messaging. Using very specific messages designed to create a more inclusive environment and mitigate implicit bias can make a real difference. As opposed to claiming “we don't see color” or using other colorblind messaging, statements that welcome and embrace multiculturalism can have more success at decreasing racial bias.
Institutionalize fairness. Organizations have a responsibility to support a culture of diversity and inclusion because individual action is not enough to deconstruct systemic inequities. To overcome implicit bias throughout an organization, consider implementing an equity lens – a checklist that helps you consider your blind spots and biases and assures that great ideas and interventions are not only effective but also equitable (an example is included in the table above). Another example would be to find opportunities to display images in your clinic's waiting room that counter stereotypes. You could also survey your institution to make sure it is embracing multicultural (and not colorblind) messaging.
Take two. Resisting implicit bias is lifelong work. The strategies introduced here require constant revision and reflection as you work toward cultural humility. Examining your own assumptions is just a starting point. Talking about implicit bias can trigger conflict, doubt, fear, and defensiveness. It can feel threatening to acknowledge that you participate in and benefit from systems that work better for some than others. This kind of work can mean taking a close look at the relationships you have and the institutions of which you are a part.
MOVING FORWARD
Education, exposure, and a systematic approach to understanding implicit bias may bring us closer to our aspirational goal to care for all our patients in the best possible way and move us toward a path of achieving health equity throughout the communities we serve. The mnemonic IMPLICIT can help us to remember the eight tactics we all need to practice. While disparities in social determinants of health are often beyond the control of an individual physician, we can still lead the fight for health equity for our own patients, both from within and outside the walls of health care. With our specialty-defining goal of getting to know each patient as a unique individual in the context of his or her community, family physicians are well suited to lead inclusively by being humble, respecting the dignity of each person, and expressing appreciation for how hard everyone works to overcome bias.

