
Fam Pract Manag. 2019;26(5):32
Author disclosure: no relevant financial affiliations disclosed.
“ESTABLISHED” VS. “NEW” PATIENT CODES
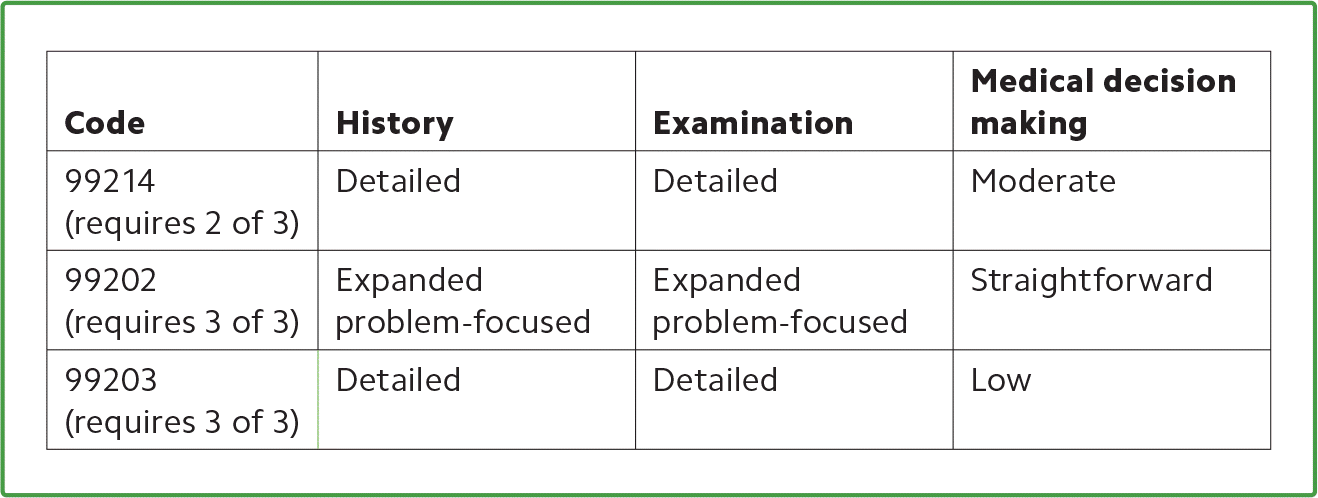
| Code | History | Examination | Medical decision making |
|---|---|---|---|
| 99214 (requires 2 of 3) | Detailed | Detailed | Moderate |
| 99202 (requires 3 of 3) | Expanded problem-focused | Expanded problem-focused | Straightforward |
| 99203 (requires 3 of 3) | Detailed | Detailed | Low |
