Caring for the whole family is a defining aspect of family medicine, yet many physicians have stopped seeing young patients. Here's why and how to welcome them back.
Related articles from American Family Physician: "Health Maintenance in School-Aged Children: Part I. History, Physical Examination, Screening, and Immunizations" and "Part II. Counseling Recommendations."

Caring for infants, children, and teens can be one of the major joys of being a family physician. It helps fulfill our mission to maintain our patients' health through every age and stage of their lives. But a recent study found that family physicians increasingly are no longer seeing children in their practices.1 The proportion of family physicians providing care to children fell from 78 percent in 2000 to 68 percent in 2009.2 Of course, this is not a uniform trend. The care of children by family physicians is more prevalent in rural areas and in communities with fewer pediatricians.2 The message is clear, however: Caring for children is no longer assumed to be an integral part of a family physician's scope of practice.
Several likely factors are fueling this narrowing of family physicians' scope. As more physicians work for hospitals or other large health care organizations, they may find employers attempting to streamline care into silos, leading family physicians to focus exclusively on adult patients. Emerging risk-sharing and pay-for-performance models that provide enhanced payments for complex care may lead some family physicians to undervalue caring for young patients. Some may also perceive the financial challenges and clinical demands of caring for young patients to be discouraging. For instance, a commonly mentioned barrier is the cost and administrative hassle of providing childhood vaccines. Lastly, in some regions with a high number of pediatricians, competition for young patients is stiff.
So should we accept the erosion of a defining aspect of family medicine and surrender all of our young patients to pediatricians? Not at all. We should actively embrace the whole family focus of our training and, where possible, reintroduce children to our offices. This article will explain why caring for children can be important to your practice and your community and how to expand this care.
KEY POINTS
- Caring for children is a key part of family medicine, but the changing health care landscape has led many family physicians to either give up on pediatrics or reduce the number of young patients they see in their practices.
- Family physicians should restore this aspect of their practices to maintain comprehensive family care, keep their practice panels mixed in age, and help young patients more smoothly transition into adult care.
- Practices must be welcoming to young patients and their families in terms of the physical environment, the appointment types and clinical services offered, and the training maintained.
- Young patients do not typically generate the same level of revenue as older patients, but pediatric care can still make financial sense for a practice.
WHY TREAT YOUNG PATIENTS?
The satisfaction that comes from taking care of children shouldn't be underestimated in a time of increasing physician burnout. Our practice opened 22 years ago offering full-spectrum care. A dozen years later, as advocating for obstetrical (OB) privileges became more difficult, we ceased practicing OB and other inpatient care. We subsequently realized our practice demographics would rapidly change if we didn't continue to attract and retain young families with children. We were aware that practice panels tend to age as physicians do, and we wanted to maintain a mix of patients, health conditions, and acuities to keep our practice schedules varied and interesting. Interspersing quick children's sick visits with more involved chronic care adult encounters makes for a true family medicine experience. Treating kids is both fun and uniquely rewarding. Children change rapidly, and our counseling and care have significant impact.
Another reason family physicians should treat children is that our breadth of knowledge amplifies pediatric care. For example, children with prediabetes or asthma can benefit from the years of experience family physicians have managing those conditions in adults. Likewise, if a young patient has a rare disease or condition and needs to receive care from a tertiary center, we can coordinate care with those consultants as effectively as we do for our adult patients in similar circumstances. We also understand the problems that develop when pediatric and adult care are disconnected. We see these firsthand, despite attempts by many specialty organizations to encourage transition plans.3 For instance, more than once, I [Dr. Reddy] have had young adult patients casually mention that they had leukemia in childhood, which was not disclosed in history or intake forms. We know that patients in remission from childhood cancer benefit more if their surveillance plans carry through to adulthood.4 Yet, I am astonished by how easily this information can be missed, requiring a search to find records and initiate appropriate care.
Caring for children isn't just beneficial for the young patient. Treating the family as a whole allows us to make recommendations to our patients that pediatricians just wouldn't be in a position to offer. Let's say the patient is a woman in her 60s with uncontrolled diabetes and a poor diet. She's the main cook in her household, and her daughter, who is recently divorced, has moved back into the home with her three young children. The patient may say she's too busy caring for her grandchildren to eat well. But in motivating her to change her behavior, we can explain that paying greater attention to her own diet and providing healthier choices for her grandchildren will be an important way to care for them. We may have lost that perspective if we only saw the adult or the children. As family physicians, we can see all of the ill members together, we can care for both the newborn and the breastfeeding mother with postpartum depression, and we can understand the teenager's mood disorder because we know the parents have been dealing with severe stressors even if the teen doesn't disclose this.
Finally, we can make the young patient's transition from pediatric to adult care much smoother. In their late teens and early 20s, young adults face many medical and personal risks, including risks to their mental and sexual health. But many of them do not have a regular physician or other clinician to come to in a crisis. By continuing to see young adults after they turn 18, we provide continuity of care and avoid the problems that arise when patients age out of their pediatric practices and suddenly find themselves without a regular doctor.3 We are especially well suited to lay the groundwork for self-care and good habits in college because we deeply understand our patients' social and emotional context by the time they start to become independent adults. They are much more likely to reach out to us when they need assistance if we have been seeing them since childhood and have earned their trust by providing compassionate and, when needed, confidential care over the years. (See “Protecting Adolescent Patient Privacy: Four Key Questions,” FPM, January/February 2019.)
HOW TO PROVIDE CARE TO MORE CHILDREN
Adding to or expanding your practice's offerings requires the same steps: determining if there is a market for the service, assessing your professional capability and physical space, and evaluating how best to attract patients.
Measure the market. The first, and biggest, consideration is whether caring for more children makes sense for your practice. If you live or work in a community with fewer children or the market is already saturated with pediatricians, this might not be the best strategy. Likewise, if you are employed in a large organization that regularly funnels young patients to its pediatricians, changing that approach will not be easy. On the other hand, if you are located in a growing community with lots of young families or an area under-represented by pediatricians, this may be an excellent way to grow your practice. You could benefit further — or persuade your organization to give it a chance — if you have competitive advantages, such as enhanced language capabilities (everyone in our practice speaks Spanish), educational programs (we offer a child literacy program called Reach Out and Read5), or the ability to perform procedures (we offer outpatient birth control implants and IUDs as well as dermatologic surgery).
Get needed training. Family physicians are trained to handle a wide range of health issues, but there may be conditions specific to the care of children that you have lost familiarity with — think Kawasaki disease — or new approaches regarding patients' developmental issues. You can obtain updated pediatric continuing medical education through national conferences, such as those offered by the American Academy of Family Physicians, or online learning opportunities. You can also consult with other physicians in your community to take a team approach, just as you may do with some adult chronic conditions. For example, most community pediatricians rely on psychiatrists and other behavioral health specialists for the initial diagnosis of conditions such as autism and attention-deficit/hyperactivity disorder.
Create a kid-friendly space. Your office was likely designed with adult patients in mind, so some physical changes may be necessary. Your space should be welcoming to young patients, both to reduce the fear they may have of going to the doctor and to communicate to their parents or guardians that caring for children is an integral part of your practice. This preparation begins in the waiting room. In my [Dr. Reddy's] practice, we try to provide a print-rich and engaging space for all visitors by leaving our reception area screen-free and soothing. We have a fish tank and offer books and magazines of interest to all ages, including children. You could designate a special area for children, which could feature books, toys, furniture, art, and other decor chosen with children in mind. Our exam rooms are also kid-friendly. Instead of the usual collection of medical diagrams and charts, we feature large laminated “Where's Waldo?” posters that regularly get positive comments from children and adults. (This was my [Dr. Reddy's] teenage daughter's idea.) We also give out stickers at visits and books at well-child checks to children from 6 months to 5 years old.
Establish your competitive advantage. Consider offering special appointment slots that line up with the needs of parents, such as early in the morning or after school. To differentiate ourselves from local pediatricians, we have researched and adopted Canadian and European techniques to address fear of injections, such as managing expectations of pain honestly and providing topical numbing agents.6
Get the word out. The efforts above communicate to parents in your practice that you see children as important patients. But communicating that fact to the community at large is also necessary. Marketing that highlights your skills to care for the entire family is helpful and can include local advertising or posting signs outside your office and in your reception area that explain you treat children. Offering to give talks at hospitals, adult education centers, or schools on concussion care, nutrition, or other topics can generate very fruitful word of mouth referrals and has been a great practice builder for us. Also, be aware that in many markets if parents search for a physician for their child through their insurer's network listing, they may not find you unless they specifically look for “family physicians.” It may help to ask your plans to include you on their list of pediatric care options.
Ask for referrals. Seeking referrals from internists and obstetricians is also productive. Speak with OB groups or departments, as well as their nursing staffs, and let them know you do see children so they can give your name to new parents.
FINANCIAL CONSIDERATIONS AND POSSIBLE OBSTACLES
Besides institutional and market competition issues, there are coding and reimbursement challenges you may need to address to expand your care of children.
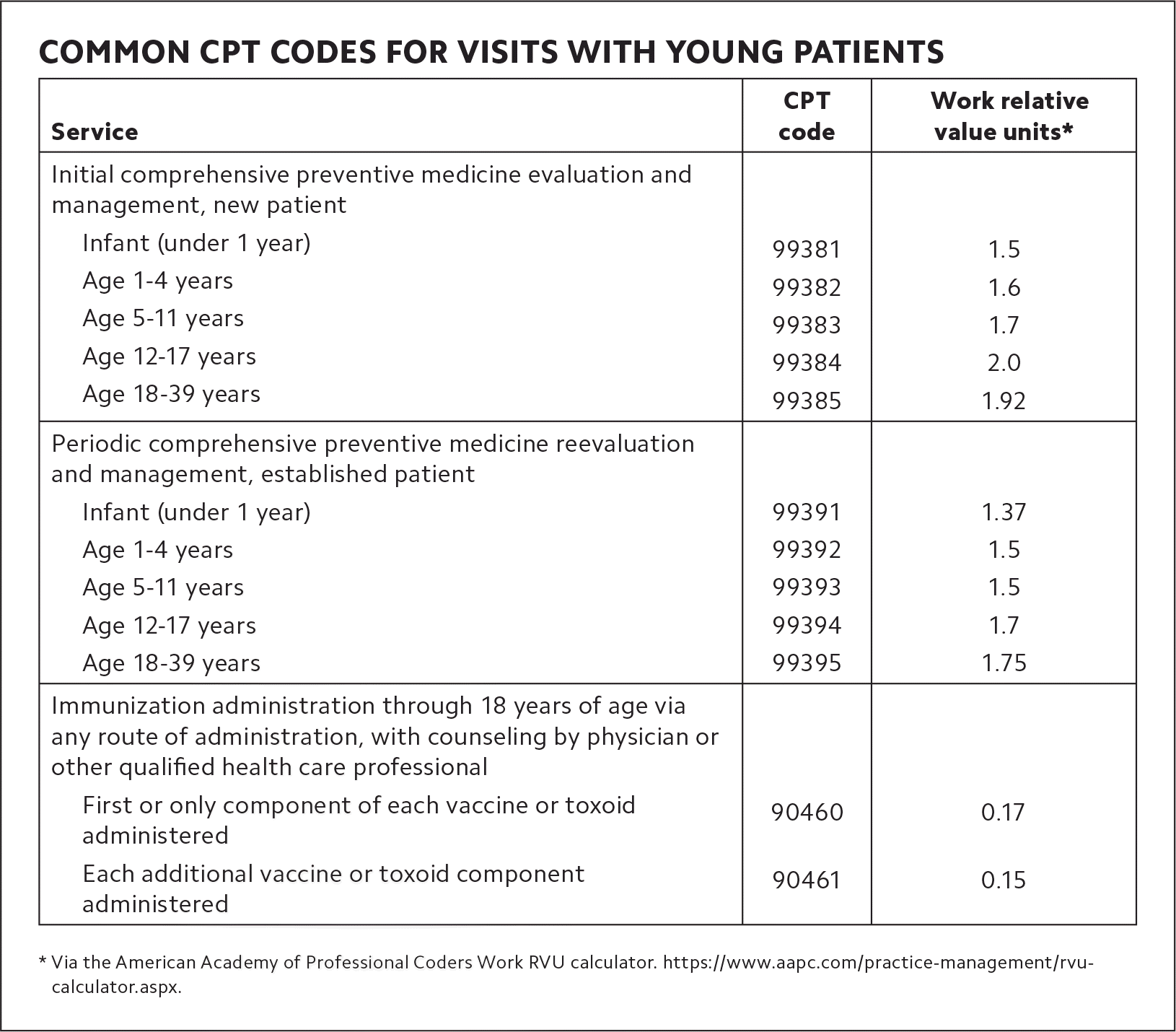
Generating revenue will often require familiarity with new codes. (See “Common CPT codes for visits with young patients.”) Physicians who have primarily cared for older patients may be focused on Current Procedural Terminology (CPT) codes and Hierarchical Condition Category (HCC) codes designed to reward higher patient complexity. In addition, physicians may be focused on billing for Medicare annual wellness visits or transitional care management services. This is especially true in employment situations where physician compensation is tied to productivity, quality measures, and HCC bonuses.
COMMON CPT CODES FOR VISITS WITH YOUNG PATIENTS
| Service | CPT code | Work relative value units* |
|---|---|---|
| Initial comprehensive preventive medicine evaluation and management, new patient | ||
| Infant (under 1 year) | 99381 | 1.5 |
| Age 1–4 years | 99382 | 1.6 |
| Age 5–11 years | 99383 | 1.7 |
| Age 12–17 years | 99384 | 2.0 |
| Age 18–39 years | 99385 | 1.92 |
| Periodic comprehensive preventive medicine reevaluation and management, established patient | ||
| Infant (under 1 year) | 99391 | 1.37 |
| Age 1–4 years | 99392 | 1.5 |
| Age 5–11 years | 99393 | 1.5 |
| Age 12–17 years | 99394 | 1.7 |
| Age 18–39 years | 99395 | 1.75 |
| Immunization administration through 18 years of age via any route of administration, with counseling by physician or other qualified health care professional | ||
| First or only component of each vaccine or toxoid administered | 90460 | 0.17 |
| Each additional vaccine or toxoid component administered | 90461 | 0.15 |
*Via the American Academy of Professional Coders Work RVU calculator.
Visits involving young patients are often of lower acuity. However, they are generally short enough that you can schedule more of them. By making sure you capture all the appropriate codes for the work you do, you can optimize reimbursement. For instance, if you administer questionnaires at physicals to screen for autism or other developmental problems in infants and young children or for mood disorders and substance use in older children and teens (such as the adolescent version of the Patient Health Questionnaire-9 and the CRAFFT Screening Test for substance abuse), insurers will generally reimburse you for that. If you accept Medicaid, your local health department can advise what types of screening instruments are necessary, including any specific to your area such as lead exposure screening. Be sure to check with your payers to learn what screening services they cover.
Also, don't forget to use time-based coding to be fairly paid for the counseling you provide around development, nutrition, and mood and behavioral issues. We devote a fair amount of time to counseling, and it's not unusual for us to code E/M office visits at a higher level based on appropriate time spent.
Coding and billing for child and adolescent vaccinations is another area of potential revenue. A well-child visit that includes counseling for vaccines and vaccine provision is generally well reimbursed in our market. A well-child visit that includes a preventive medical service, a screening test of visual acuity, and a pure tone audiometry test generates between $126 and $206 in reimbursement, depending on the insurer. One that includes counseling for and administering three common childhood vaccines (human papillomavirus; meningococcal polysaccharide; and tetanus toxoid, reduced diphtheria toxoid, and acellular pertussis) ranges between $122 and $510 in our market.
You will need to become familiar with the childhood immunization schedules and vaccination combinations. You'll also need to order, stock, and track a larger supply of vaccines, which could include additional refrigeration and inventory control measures. Local health departments and online references such as Immunize.org can help you navigate this process. The AAFP provides annual laminated vaccine schedules, and medical assistants can help keep track of patients' vaccinations and identify the best combinations to minimize doses, reducing the burden on physicians.
Working with vaccine purchasing groups can lead to significant savings, and we have found that appealing vaccine reimbursements that are less than the purchase price often results in the insurer paying the difference. Starting a vaccine program for children may also demystify the process and allow you to more consistently provide vaccines for your older patients. (For more on implementing vaccinations in your practice, see “Immunizations: How to Protect Patients and the Bottom Line,” FPM, March/April 2015.)
ACHIEVING THE VISION
Caring for children is an integral part of the vision of family medicine. Continuing to provide that care can give you more career satisfaction, generate greater recognition of the value of family medicine, and ensure better health care and closer relationships with your patients.

