Most teams try to avoid conflict, yet can't stop focusing on the negative. Healthy teams do the opposite.

“Morale is at an all-time low.” “Everyone feels overworked, understaffed, and undervalued.” “We lose staff faster than we can hire them.” “The atmosphere is negative, and everyone is irritable and quick to snap.” “Dread is palpable at the beginning of every workday.”
This is how one physician leader described his practice environment to me. I had been invited to speak to his team members about well-being, and when I asked them how they were doing, they admitted to feeling “beat up,” “in a rut,” “boxed in,” and “not supported.” They shared that they felt more pressure than ever to deliver better outcomes with fewer people and fewer resources. Everyone I spoke with was negative, some were cynical, and others were clearly burned out. Many viewed their only option as leaving.
The team had multiple sources of conflict and negativity, but chief among them was a chronic barrage of mandated, top-down, unfunded initiatives, which left everyone feeling overwhelmed, demotivated, and demoralized.
Perhaps you can relate to this team's story, or perhaps you have a healthy team and want to keep it that way. This article will outline why a healthy team matters and share two habits that can promote team well-being: managing conflict and practicing gratitude.
KEY POINTS
- The health of a team affects not only the individuals on the team but also the practice's performance.
- Being able to address conflicts openly but respectfully is key to a team's progression, and it requires a foundation of trust.
- Gratitude is important to team wellness, because team members who feel appreciated and recognized will extend those feelings to others, creating a positive cycle.
THE IMPORTANCE OF A HEALTHY TEAM AND A SKILLED LEADER
Health care is a science, an art, and an interdisciplinary team activity. A healthy team is a high-performing team, leading to better patient outcomes, reduced costs to the health care system, and improved well-being of health care providers.1–6 Traditionally, medical care was delivered exclusively by physicians. But excessive workloads and limited workforce now demand team-based care models in which health professionals work together at the top of their licenses.
Doctors who serve as team leaders require new skills to support not only the health and well-being of patients but also of their team members.7 The best team leaders are “multipliers” who amplify the strengths, skills, and voices of others, as opposed to “diminishers” who drain capability and intelligence from their teams.8 Leaders who possess this quality don't need to accomplish everything themselves or be experts in every area. They support the strengths and welcome the diversity of their members, recognizing that group contribution is greater than the sum of individual contributions. Diverse teams offer rich perspectives not possible from single voices. This diversity includes not only age, gender, ethnicity, race, etc., but also profession and discipline. Interdisciplinary and interprofessional teams demonstrate better patient outcomes.9 But with diversity comes the potential for differences of opinion and conflict.
CONFLICT IS NATURAL; RESOLVING IT REQUIRES TRUST
Highly productive teams take time to develop, and their progress is not always linear. Leaders who understand team dynamics prepare teams to manage differences throughout their development. Within the Tuckman stages of group development, conflict is a critical component of the “storming” phase that occurs during a team's progression from “forming” to “adjourning.”
The Five Behaviors model for team cohesion, introduced by Patrick Lencioni,10 also emphasizes the importance of conflict. Lencioni suggests that high-performing teams must exhibit five key behaviors: trust, conflict, commitment, accountability, and results. A team's progression to commitment, accountability, and results depends on a solid foundation of trust and expression of disagreement. Healthy disagreement leads to finding common ground. When voices are suppressed, teams don't perform optimally.
Healthy teams circle back to storming at pivotal points in decision-making and during periods of high stress. Teams that have the opportunity to express negative feelings respectfully move forward, whereas teams that lack the opportunity for forthright conversation stagnate. Silence does not imply consent. It can be an ominous sign of dissent, disengagement, hopelessness, and distrust, all of which limit well-being and contribute to burnout. But teams under chronic stress that have trust can effectively manage conflict and be high-performing.
THE NATURAL PROGRESSION OF A TEAM
Teams progress through five stages, from “forming” to “adjourning.” In the “storming” stage, conflict is a critical component.1
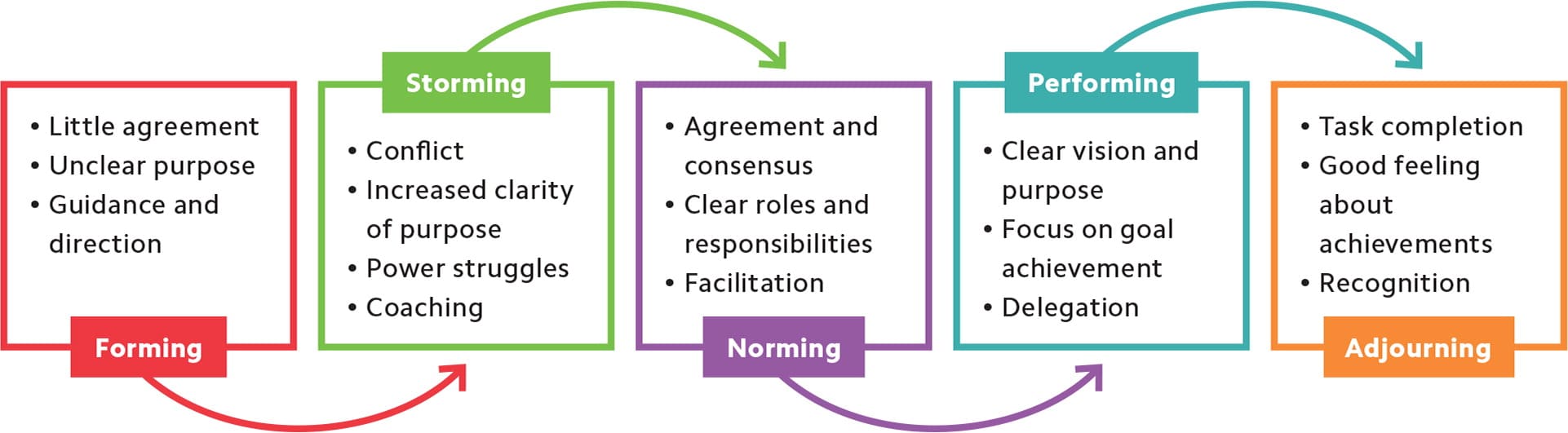
1. Tuckman BW, Jensen MAC. Stages of small-group development revisited. Group & Organization Studies. 1977;2(4):419–427.
PRACTICING TEAM APPRECIATION AND GRATITUDE
Appreciation has been shown to promote physical, social, emotional, and mental health and happiness, with lasting benefits that extend beyond the grateful individuals to those on their teams. Regularly practiced gratitude reduces levels of stress hormones, inflammatory responses, illness, anxiety, and depression, and increases sleep, exercise, dopamine, and immune response. It also boosts self-esteem, energy, enthusiasm, optimism, overall satisfaction with life, and the ability to cope with stress and achieve personal goals.11–14
Incorporating appreciation as a daily practice reminds us to focus on what matters and not take for granted the gifts we have been given. Practicing gratitude need not be complex. It can be as simple as saying “thank you” to a staff member or colleague, or using appreciative inquiry (AI) to emphasize the good in our lives, particularly when perceptions turn bad. AI is defined as the “search for the best in people, their organizations, and the relevant world around them.”15 Engaging in simple AI exercises with purposeful attention to “blessings” as opposed to “burdens” provides individual and interpersonal benefits.16,17
When a team is negative, refocusing members on “what is going well” can benefit all. Appreciation in the workplace not only adds to individual well-being but also strengthens a culture of well-being. When individuals feel appreciated and recognized, their generosity grows and seeps into the environment. Gratitude activates a positive cycle that expands beyond self-care to benefit others.
The benefits of gratitude exercises are long-lasting. Participants in a simple gratitude letter-writing intervention showed both behavioral increases in gratitude and significantly greater neural modulation in the medial prefrontal cortex, with effects present three months later.18 Similar simple exercises performed by health professionals experiencing burnout demonstrated benefits that lasted more than a year.19
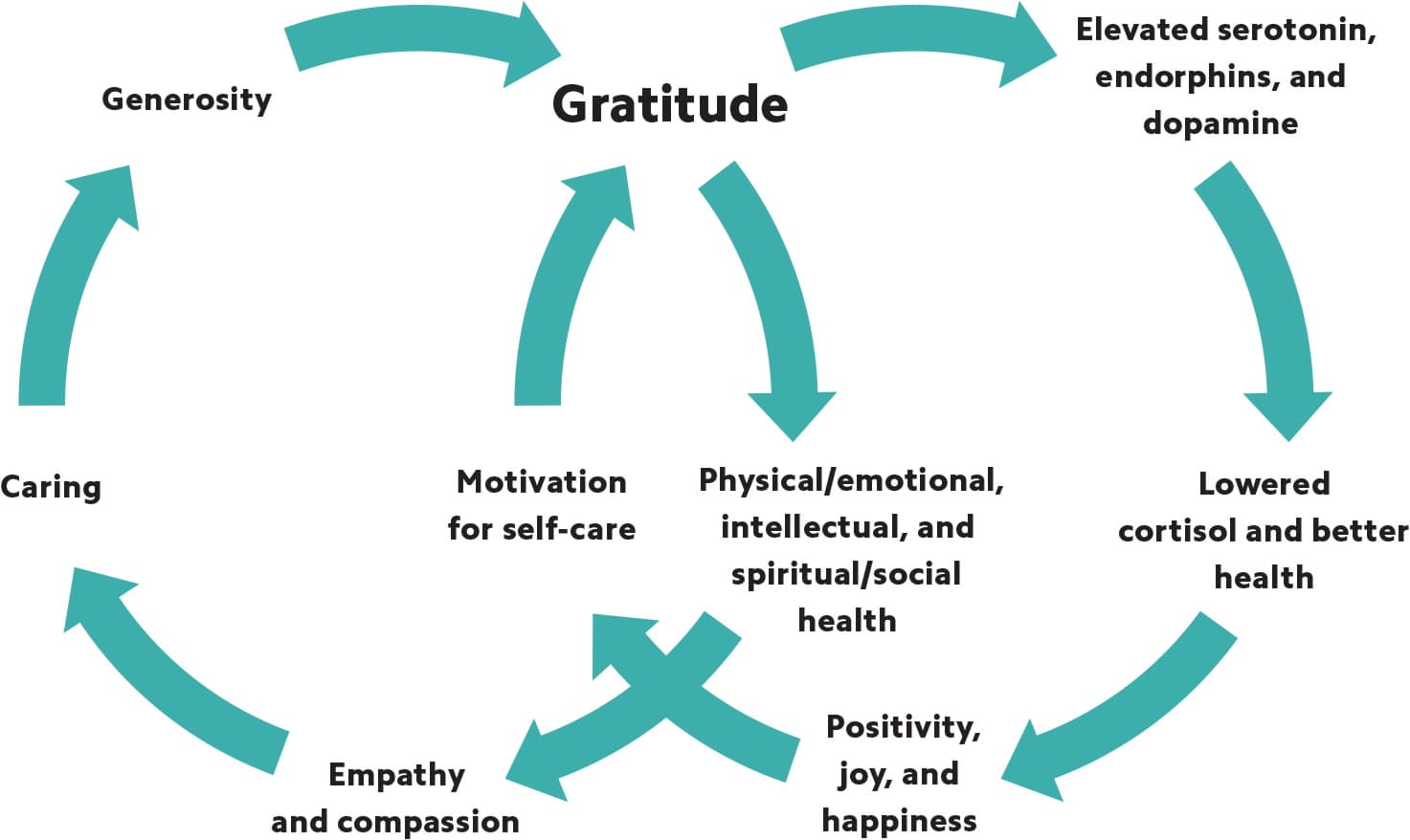
POSITIVE GRATITUDE CYCLE
Gratitude activates a positive cycle, beginning with physical benefits that lead not only to motivation for self-care but also caring for others.
RETREATING TO MOVE A TEAM FORWARD
As teams work to establish the habits of managing conflict and practicing gratitude, a retreat can be enormously helpful. Retreat planning should follow the “Five Ps.”
Purpose: Articulate the vision for the team (e.g., “healthy individuals contributing to a healthy team”) and then lay out the goals for the retreat, such as to uncover factors that uniquely contribute to team dissatisfaction, to reframe the team in a positive manner, and to empower team members to lead change.
People: Decide who should attend (e.g., the full team or a smaller subset), and then recruit a small group of volunteers for planning. For an off-site, full-day retreat, planning can take several months because you'll need to clear schedules and ensure clinical coverage as well as funding.
Policies: Draft basic ground rules to assure professionalism and respectful discussion as well as attendance. It's also helpful to have guidelines on unplugging so that everyone is engaged, not distracted.
Process: Identify activities that will help you meet your goals. One helpful exercise is creating a fishbone diagram in which the group breaks into teams and identifies factors that limit their overall well-being. This may include individual factors (thoughts and feelings, personality characteristics, and behaviors) as well as institutional factors (culture, programs/processes, and policies). Capture responses on flip charts, post them around the room, and share them out loud. Another helpful exercise is a SWOT analysis, which involves identifying individual and collective strengths (What do we do well as a team in caring for ourselves and each other?), weaknesses (What could we do better to understand and support one another as a team?), opportunities (What resources are available to support us?), and threats (What must we be aware of that can negatively impact or limit our team's well-being?).
Products: One key product of a retreat is that the team feels heard and appreciated. Additionally, the team utilizes the results of the above exercises to form a team health improvement plan. The Personal Health Improvement Plan tool (also available at http://www.MyPHIT.org with daily reminders) can be adapted for team use. This plan drives specific goals and actions the team will take to address specific concerns. Here are just a few ideas — some simple, some complex:
- Implement a new workflow to address a key source of team frustration or inefficiency,
- Get leadership buy-in and pilot an innovation project of the team's choosing,
- Allow work-from-home days for non-clinical work,
- Have a “moment of gratitude” at the beginning of staff meetings,
- Create an appreciation board in the clinic with notes from grateful colleagues and patients,
- Use team huddles to check in on each other's successes and challenges,
- Dedicate time and resources to wellness each week — “Wellness Wednesdays” or “Free-time Fridays,”
- Designate quiet space and time for team members to enjoy breaks,
- Tag team lunches, providing daily cross-coverage so that everyone has the freedom to go out for lunch if they choose.
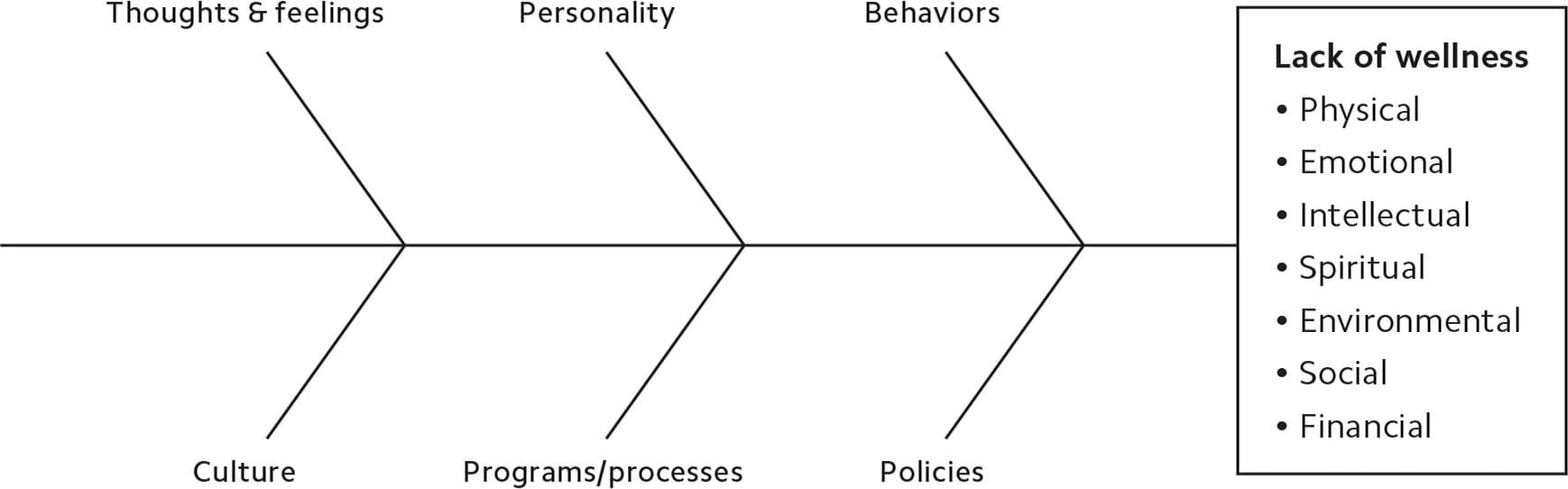
USING A FISHBONE ANALYSIS WITH YOUR TEAM
A fishbone (or cause and effect) diagram, can help your team answer the question “What factors are causing a lack of wellness within our team?” Simply brainstorm as a group and list the root causes on the appropriate section of the diagram. For example, you might note under culture a “fear of making mistakes,” or under behaviors “skipping lunch.”
MAKING WELLNESS A TEAM PRIORITY
The negative team scenario I described at the outset actually has a positive ending. The physician leader recognized the team's well-being was in jeopardy and began working on building trust, managing conflict, and practicing appreciation and gratitude. During an all-day retreat, the team members expressed their concerns, identified solutions, and formed a plan. When I checked in with the physician leader a few months ago, in the midst of the COVID-19 pandemic, he said his team was still thriving despite all the changes and challenges.
While it may not be feasible right now to close down your clinic for an all-day retreat, or go offsite, setting aside time on a regular basis for team well-being sends a powerful message to team members that their wellness (and your own) is a priority. As you consistently apply the habits of a healthy team, you will not only achieve a healthier team but a more successful practice.
SERIES OVERVIEW

In this or previous issues:
- Creating your personal wellness plan (January/February 2020).
- Self-care through mindfulness and strategies for promoting physical health (March/April 2020).
- Family well-being through social connectivity and time management (May/June 2020).
- Team well-being through conflict resolution and promotion of gratitude in the workplace (this article).
In upcoming issues:
- Organizational well-being through prioritizing purpose and creating resilient leaders.
- Community well-being through cognitive reframing and building emotional intelligence.

